Do Patent Extensions Protect Investment or Prolong Pain for Patients?
Analysis reveals 8 key thematic connections.
Key Findings
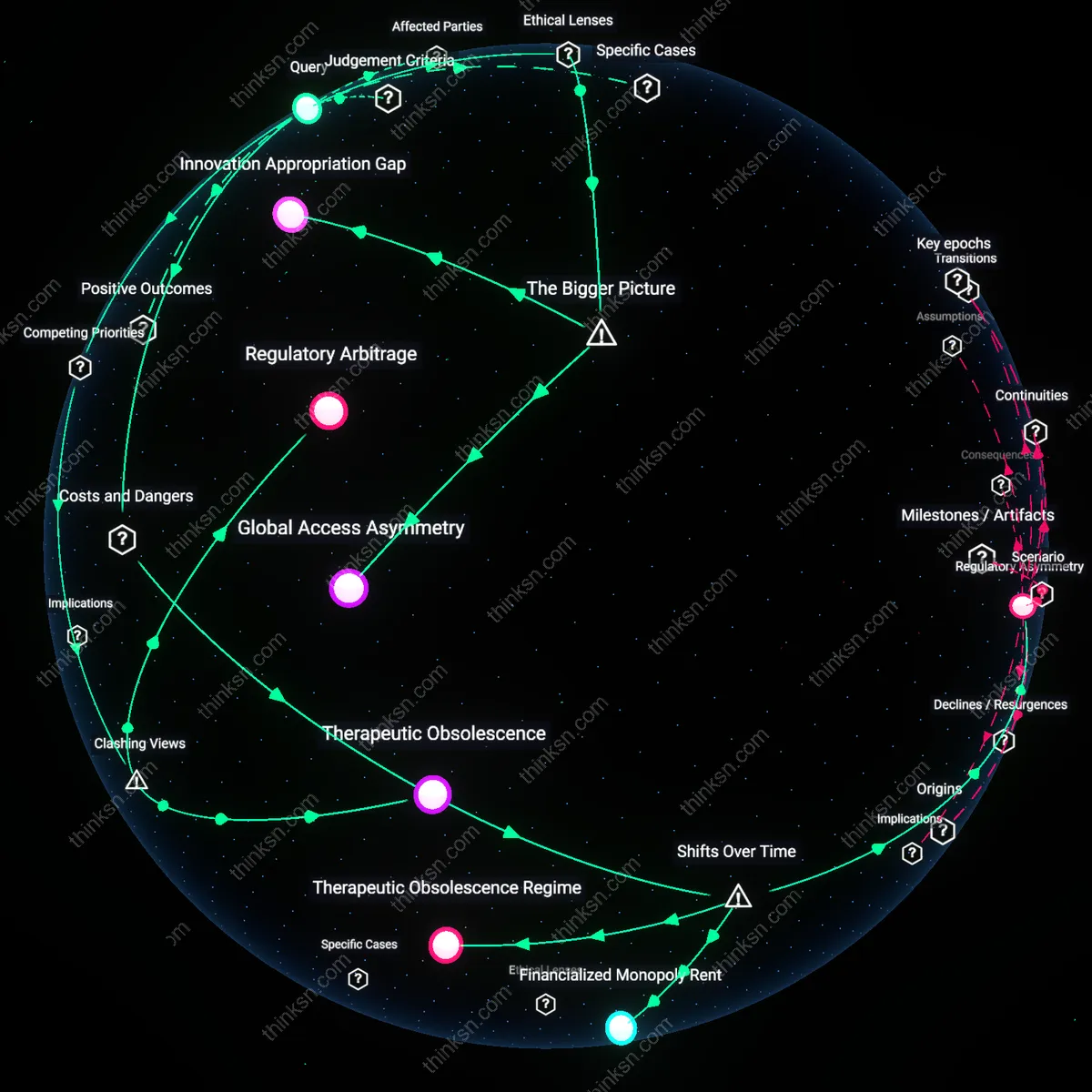
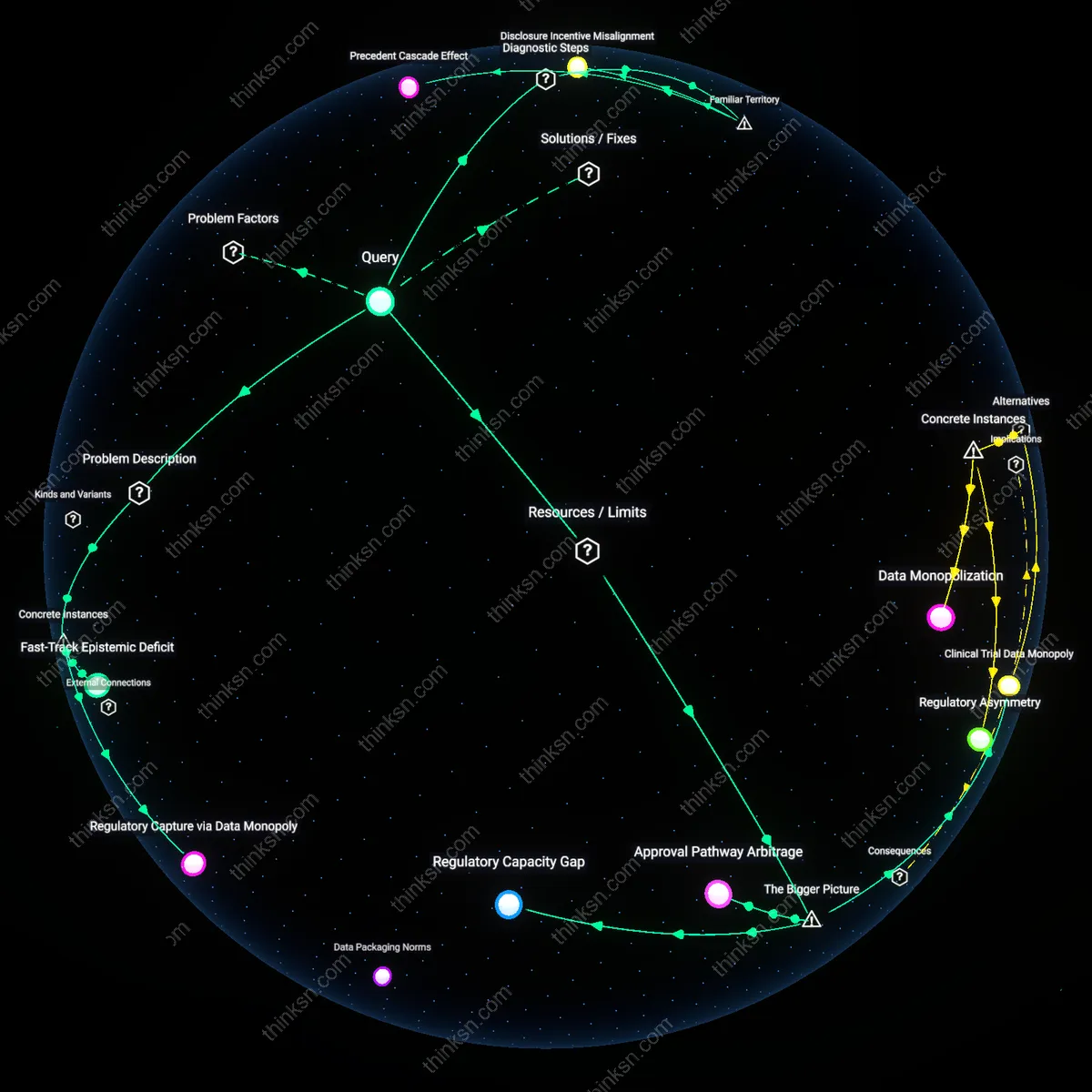
Regulatory Asymmetry
Patent extensions became a structural subsidy after the 1984 Hatch-Waxman Act, which balanced generic market entry with added exclusivity, thereby embedding prolonged pricing power into regulatory design. The mechanism—linking FDA approval timelines to patent terms—allowed originator firms to convert bureaucratic delays into extended market protection, shifting risk from investors to public payers. This recalibration transformed temporary intellectual property into a permanent cost transfer, naturalizing what was meant to be an exception. The non-obvious consequence is that policy meant to accelerate generic competition instead institutionalized delays by rewarding large firms capable of navigating complex regulatory pathways.
Financialized Monopoly Rent
The justification of patent extensions shifted in the 1990s as biotech firms reframed R&D costs through Wall Street valuation models, making extended revenue streams a prerequisite for investor confidence. By anchoring drug development legitimacy to future earnings projections—rather than actual outlays—firms leveraged time itself as a financial asset, divorcing exclusivity from innovation effort. This pivot turned patent duration into a speculative instrument, where extensions secured not just cost recovery but outsized returns essential to stock performance. The unappreciated dynamic is that monopolistic pricing became a feature of capital markets, not just pharmaceuticals, normalizing patient access restrictions as systemic financial infrastructure.
Therapeutic Obsolescence Regime
From the 2000s onward, patent extensions have been systematically justified by incremental modifications to existing drugs—such as dosage forms or combination therapies—marking a shift from novel molecule investment to lifecycle management strategies. Firms like those producing extended-release opioids or next-gen statins exploited regulatory incentives for 'improvements' to reset exclusivity clocks, despite marginal clinical benefit. This trajectory reveals that extensions no longer protect foundational innovation but instead delay therapeutic stagnation by suppressing competition to aging products. The underrecognized outcome is a self-perpetuating system in which drug development prioritizes temporal dominance over medical advancement, corroding therapeutic progress itself.
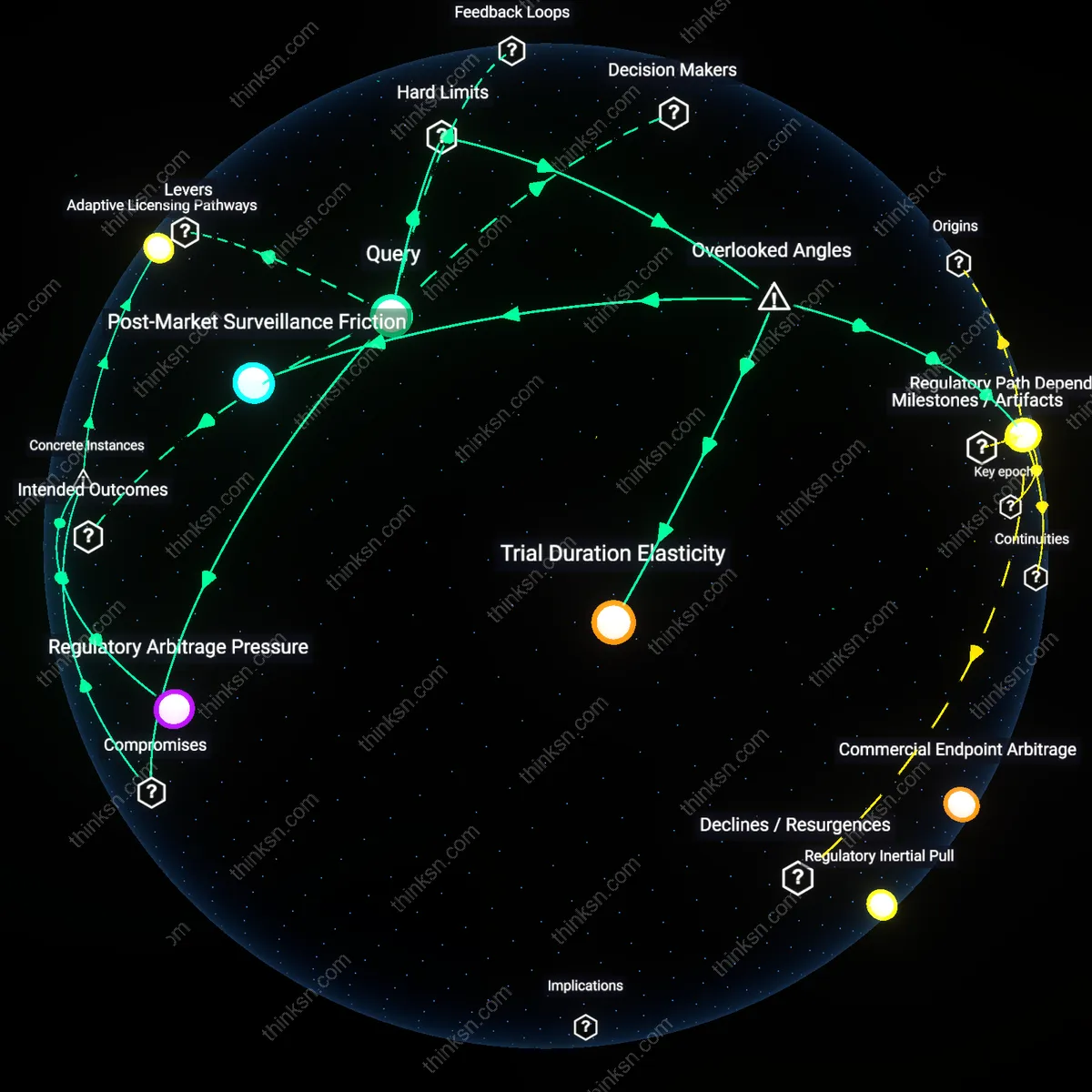
Regulatory Arbitrage
Patent extensions are less about rewarding innovation and more about enabling pharmaceutical firms to exploit jurisdictional misalignments in regulatory review timelines. Companies strategically file for extended protection in markets where health technology assessment bodies lack authority to challenge patent validity, turning the gap between clinical approval and market competition into a revenue extraction window. This mechanism reveals that the core conflict is not between innovation and access but between synchronized global health governance and fragmented national regulatory regimes—an underappreciated dynamic where legal compliance masks rent-seeking. The dissonance lies in reframing extensions not as a compromise but as an exploit of systemic miscoordination.
Therapeutic Obsolescence
Patent extensions are justified within the drug development ecosystem precisely because they accelerate the planned redundancy of older treatments, not because they sustain valuable ones. When a company extends the exclusivity of a marginally improved successor drug, it suppresses both generics and clinically adequate predecessors, forcing uptake of newer agents even when population health outcomes do not improve. This dynamic operates through formulary capture in public and private insurers, where rebate-driven contracts make extended monopolies more fiscally rational than competitive pricing. The non-obvious insight is that extensions are not protecting investment but engineering demand displacement—a challenge to the narrative that time-limited returns are necessary for medical progress.
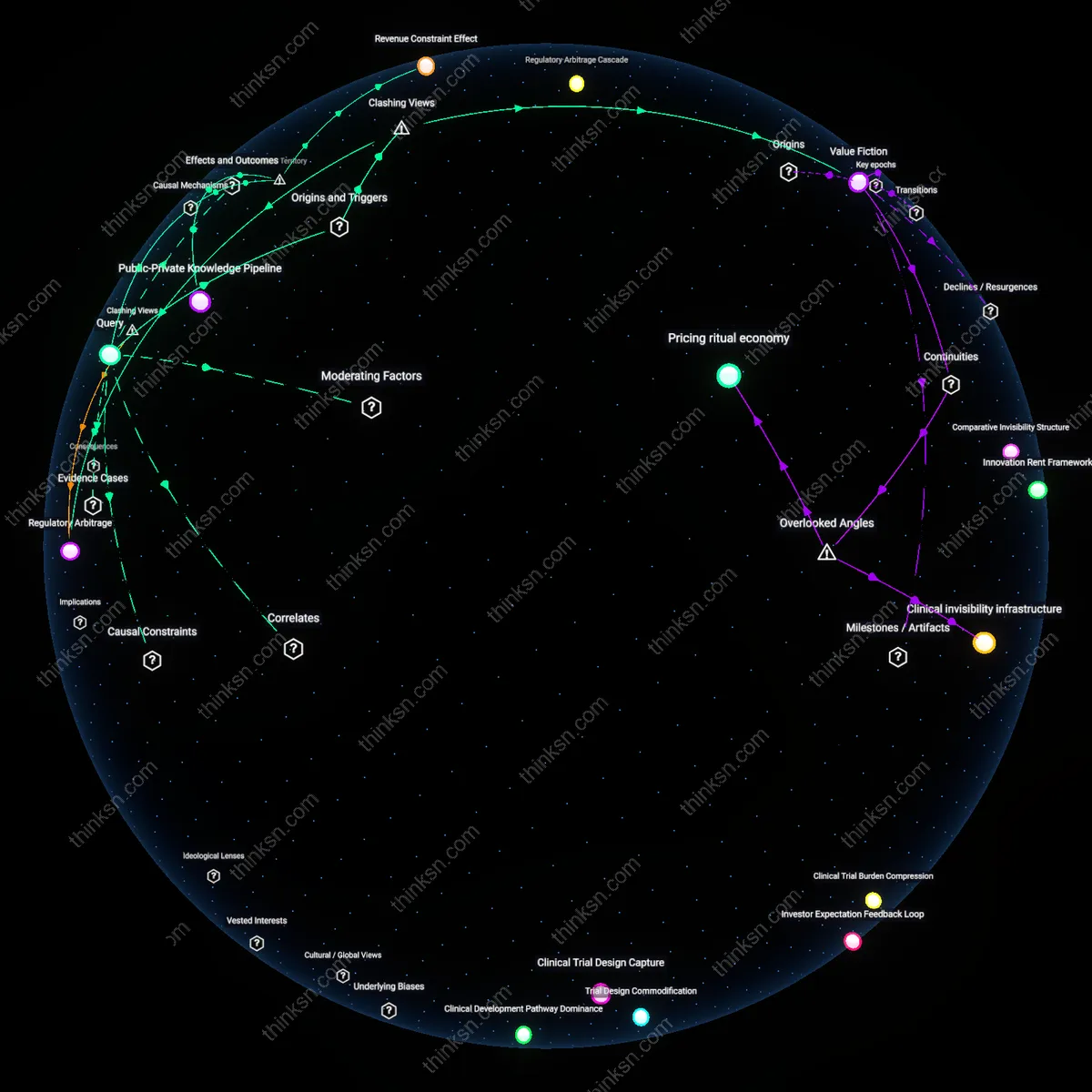
Price Epistemic Asymmetry
Patent extensions persist because manufacturers control the informational infrastructure that determines what counts as a 'fair' return on R&D, shifting the balance from observable production costs to modeled financial risk. By embedding proprietary cost-of-capital estimates and undisclosed clinical trial expenditures into regulatory negotiations, firms make the justification for extensions appear evidence-based while insulating assumptions from scrutiny. This operates through closed-door pricing dossiers submitted to agencies like NICE or ICER, where methodological opacity prevents independent validation. The friction arises when transparency is framed as compromising commercial sensitivity rather than enabling democratic accountability—exposing that the trade-off is not between innovation and access but between proprietary knowledge and public reason.
Global Access Asymmetry
Patent extensions can be ethically defended within Rawlsian liberal egalitarianism when framed as generating cross-border redistributive capacity, as excess profits from high-income markets like Germany or Canada fund differential pricing and generic licensing in low-income regions such as sub-Saharan Africa through mechanisms like the Medicines Patent Pool. The causal link depends on transnational pharmaceutical firms acting as conduit institutions that convert time-bound monopolies in the Global North into subsidized access programs in the Global South, enabled by international health governance norms and WTO/TRIPS flexibilities. Without this asymmetric surplus extraction, there would be fewer resources and less institutional will to scale treatments like antiretrovirals in resource-poor settings. The underappreciated dynamic is that local price gouging in wealthy countries is functionally subsidizing global health equity, making extensions a hidden fiscal engine for humanitarian distribution.
Innovation Appropriation Gap
Patent extensions are systemically necessary within Schumpeterian innovation economics because the lag between clinical breakthroughs and their generalizable application creates a window where follow-on competitors can free-ride on pioneer firms’ de-risked pathways, as seen in the rapid biosimilar entries post-2015 in monoclonal antibody markets. This gap emerges when regulatory blueprints—such as established dosing regimens, biomarker endpoints, or safety profiles—become public knowledge through the original approval process, allowing competitors to bypass costly exploratory phases. Extensions function not as pure profit protection but as compensation for this involuntary knowledge spillover, preserving the lead innovator’s ability to recoup investments before genericization accelerates. The overlooked reality is that stronger public science enables faster imitation, so exclusivity lengthening is a corrective mechanism to maintain innovation incentives in an era of open discovery.