Do Generic Denial Letters Undermine State Appeal Rights?
Analysis reveals 6 key thematic connections.
Key Findings
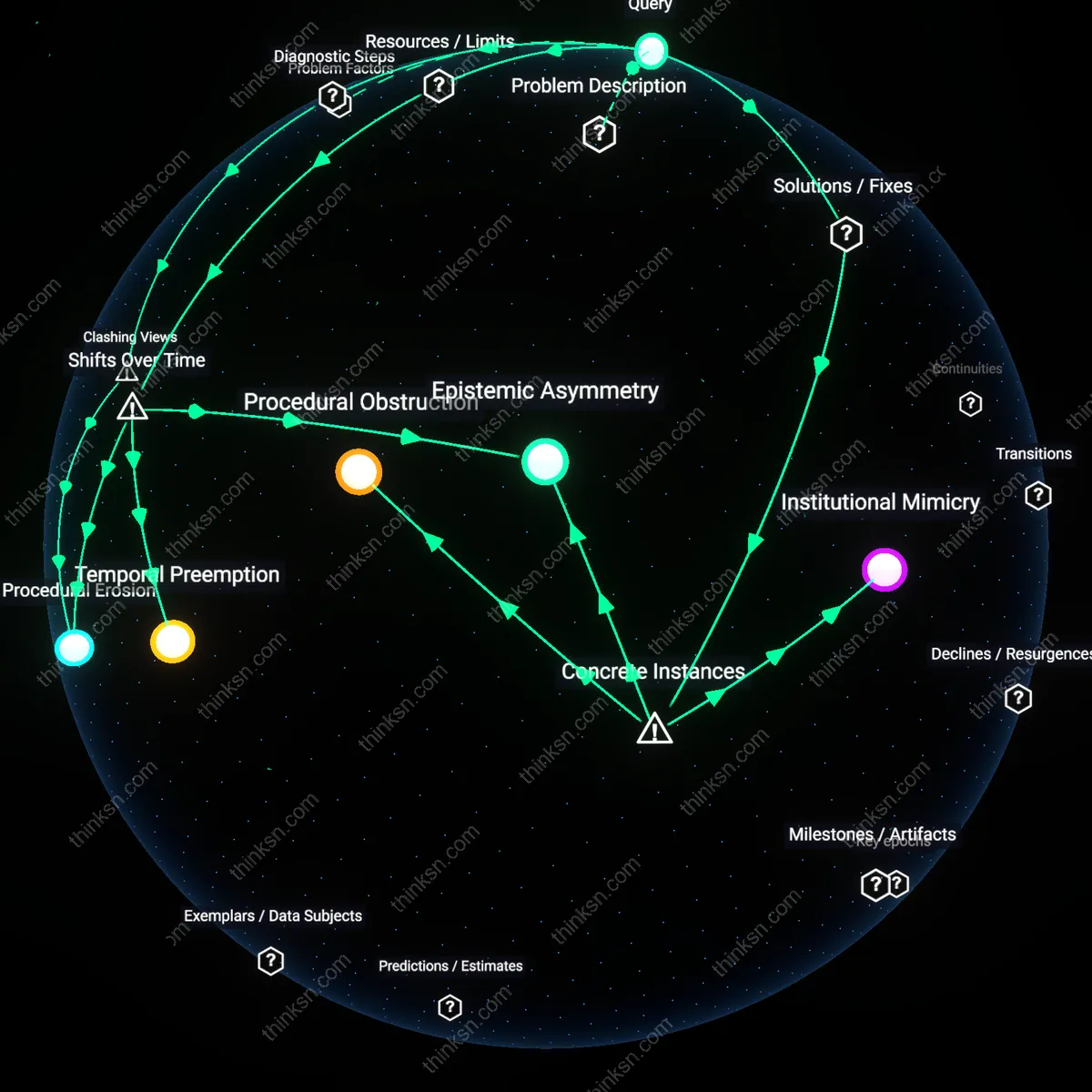
Procedural Erosion
Insurers' use of generic denial letters systematically undermines state-guaranteed appeal rights by substituting placeholder reasoning for individualized clinical judgment, thus shifting the burden of proof onto patients who must now disprove vague assertions they cannot meaningfully challenge. This mechanism operates through the administrative adjudication systems of state Medicaid programs and private plans under state regulation, where appeal bodies rely on the appearance of due process even when denials lack clinical specificity. The non-obvious consequence is not outright denial of appeals but the degradation of their functional utility—patients may appeal, but without access to the actual rationale, the process becomes a ritualized compliance rather than a corrective mechanism, contradicting the intuitive belief that procedural availability ensures equitable redress.
Regulatory Inertness
State regulatory agencies fail to enforce statutory appeal rights because they treat insurers' form letters as compliant documentation, mistaking administrative regularity for clinical justification, thus allowing the mechanical reproduction of denials to simulate adherence to law without substantive review. This dynamic functions through insurance departments’ reliance on process audits rather than clinical validation, where the presence of a denial letter—regardless of content—satisfies oversight requirements. The underappreciated reality is that regulatory compliance has been redefined as box-checking, permitting insurers to exploit the deference granted to ‘clinical judgment’ while submitting text that cites no diagnostic criteria, thereby hollowing out the appeal right from within the very systems meant to protect it.
Procedural Obstruction
In the 2022 California Department of Managed Health Care enforcement action against UnitedHealthcare, the insurer was found to have systematically reused form denial letters that omitted patient-specific clinical rationale, thereby rendering appeals functionally incoherent even as the state guaranteed timely review; this practice exploited the gap between procedural compliance and substantive accountability, where the insurer met the letter of appeal processing rules while undermining their purpose through information asymmetry; the non-obvious insight is that standardization—often a hallmark of efficiency—can become a weapon of administrative burden when decoupled from clinical specificity.
Epistemic Asymmetry
Following the 2018 Maine Medicaid appeals backlog crisis, patient advocates demonstrated that insurers' use of generic denials forced appeal officers to reverse decisions not because the original medical need was clarified, but because insurers failed to produce any individualized justification during review—a structural flaw where the burden of proof inverted; clinicians had to prove medical necessity without access to the insurer’s undisclosed criteria, while denials cited no clinical guidelines or patient-specific data; this reveals that appeal rights collapse not when rules are broken, but when the evidentiary foundation for contesting decisions is never formed in the first place.
Institutional Mimicry
After a 2020 class action in Oregon exposed PacificSource’s use of denial templates copied across unrelated medical conditions—including behavioral health and cardiac surgery—the court found that the insurer treated clinical review as a post hoc formality rather than a precondition for denial, signaling that the appeals process was designed to mimic fairness rather than produce it; the template reuse demonstrated that the insurer prioritized legal defensibility over clinical coherence, creating an appearance of review while insulating decisions from genuine scrutiny; the underappreciated mechanism here is that institutional legitimacy can be simulated through paperwork rituals that hollow out mandated rights.
Temporal Preemption
Insurers' generic denials now function as anticipatory closures that exploit the finite duration of treatment windows, a tactic that intensified after Medicaid managed care expansion in the 2000s transferred risk to private plans operating under strict cost timelines. By issuing broad, non-specific rejections during the initial claim phase, insurers compress the time available for meaningful appeal—particularly in mental health and pediatric chronic care, where treatment delays of even weeks can invalidate clinical utility—effectively nullifying retroactive wins. This shift from appeal-as-redress to appeal-as-formality exposes how administrative time has become a strategic resource, weaponized to render appeal rights moot through delay disguised as due process.