Who Benefits as Insurers Automate Claim Denials?
Analysis reveals 11 key thematic connections.
Key Findings
Insurer Operational Amplification
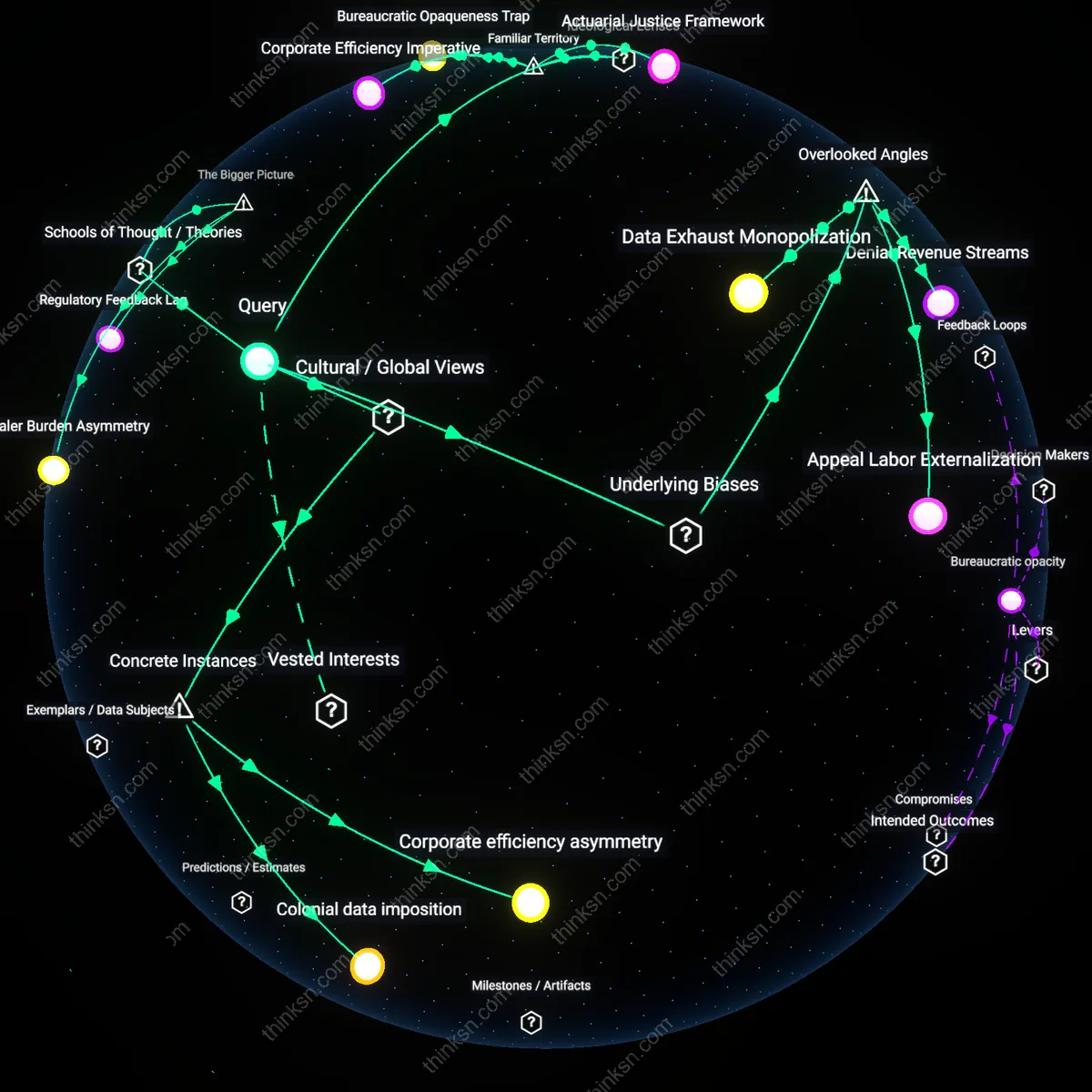
Insurers benefit most from automated claim processing because it systematically reduces labor-intensive validation and accelerates denial workflows, enabling faster case throughput and lower cost per claim. This efficiency is driven by proprietary algorithms trained on historical claims data, which reinforce existing underwriting biases and create feedback loops that disproportionately flag edge cases—like those from marginalized demographics—for denial. The non-obvious systemic consequence is that automation does not merely speed up decisions but actively reshapes the boundary of what counts as a 'valid' claim, embedding risk aversion into technical infrastructure. What makes this dynamic hold is the alignment between corporate cost-minimization pressures and the scalability of machine learning systems in regulatory environments that permit opaque adjudication protocols.
Appealer Burden Asymmetry
Individuals appealing denials are structurally disadvantaged because automated systems generate denials through opaque, data-driven logic that is not mirrored in the appeal process, which remains manual and resource-intensive. Insurers deploy automation to produce standardized, rapid rejections while forcing appellants to navigate fragmented human review channels that lack access to the same algorithmic logic—creating a power imbalance in evidentiary control. This asymmetry is sustained by legal and regulatory frameworks that treat algorithms as trade secrets, thereby legitimizing information hoarding. The underappreciated consequence is that the system incentivizes abandoning appeals altogether, not due to lack of merit but due to procedural friction engineered by mismatched scales of automation and recourse.
Regulatory Feedback Lag
Regulatory agencies benefit indirectly from automated claim processing by inheriting the appearance of systemic efficiency, which defers political pressure for reform despite growing discrepancies between automated denials and consumer harm. As insurers report faster processing times and lower error rates—metrics optimized for automation—regulators use these indicators as proxies for fairness, even when appeal success rates reveal systematic errors. This creates a feedback lag where policy responses trail behind technological entrenchment, allowing adverse selection mechanisms to solidify under the guise of innovation. The key dynamic is the substitution of procedural speed for justice outcomes in regulatory assessment, which rewards performative compliance over substantive accountability.
Corporate Efficiency Imperative
Insurance corporations benefit most from automated claim processing because it reduces labor costs and accelerates adjudication through algorithmic triage of standardized claims, primarily at the expense of nuanced human review. This system functions by encoding predefined eligibility criteria into machine-readable rules, enabling firms like UnitedHealth or State Farm to process claims at scale with minimal oversight, thereby increasing profit margins and shareholder value. What is underappreciated in public discourse—where automation is often framed as neutral or universally convenient—is how this efficiency is selectively optimized for corporate cost structures, not consumer fairness, especially when appeals require evidence outside algorithmic parameters.
Bureaucratic Opaqueness Trap
Individuals appealing denied claims are harmed by automated processing because the logic of denial becomes embedded in black-box systems that obscure accountability and resist contestation. When a claim is denied by an algorithm used by insurers such as Aetna or Geico, the individual must navigate a rigid, multi-tiered appeals process designed for compliance rather than redress, often without access to the specific code or data weightings that determined the outcome. While the public assumes automation brings transparency and speed, the non-obvious reality is that it often intensifies bureaucratic inaccessibility, turning appeals into procedural labyrinths where the lack of human agency at decision points eliminates negotiation and empathy.
Actuarial Justice Framework
Actuarial logic benefits from automated claim processing by reinforcing risk-based stratification as the moral and operational core of insurance, where fairness is defined by statistical consistency rather than individual circumstance. Under this framework—embraced across liberal and conservative ideologies alike—automation validates decisions that align with population-level data, penalizing outliers whose conditions or claims deviate from modeled norms. The unacknowledged consequence, despite widespread belief in technology’s impartiality, is the quiet displacement of ethical judgment with predictive conformity, positioning algorithmic denial not as error but as systemic fidelity to risk pools.
Corporate efficiency asymmetry
In India, the 2021 rollout of automated claim processing by the Insurance Regulatory and Development Authority (IRDAI) disproportionately reduced processing times for urban, digitally literate policyholders, while rural claimants in Odisha’s tribal districts faced higher denial rates due to misaligned biometric data and poor documentation infrastructure, revealing that automation amplifies structural disparities despite universal design claims. The system benefits insurers by reducing labor costs and claim durations, but appeals become functionally inaccessible for those without digital intermediaries, making reversals rare; this exposes how 'neutral' automation privileges those already integrated into formal bureaucratic systems. The non-obvious insight is that automation’s efficiency gains are not uniformly distributed but are structurally biased toward those who mirror urban, Western data norms.
Colonial data imposition
When Kenya’s Jubilee Insurance deployed AI-driven claim assessment in 2020, Maasai pastoralists in Kajiado County experienced systemic denial due to automated land-title verification systems requiring fixed geographic coordinates—contradicting customary oral tenure recognized under Kenyan law but invisible to Western-coded algorithms. The appeals process, designed for document-based disputes, failed to accommodate oral testimony, rendering traditional dispute resolution mechanisms invisible; this reflects a deeper imposition of colonial cartographic rationality through digital systems. The underappreciated reality is that automation does not merely accelerate claims—it enforces a model of property and identity that erases indigeneity by design.
Denial Revenue Streams
Insurers benefit from automated claim processing by retaining deniable claims in circulation longer, increasing premium volume before adjudication, because actuarial models reward holding capital from initially denied claims that appeal slowly. This mechanism operates through the time-value of premiums and reinsurance treaties that incentivize deferral of final settlement, a dynamic rarely acknowledged in discourse that assumes automation only speeds accurate outcomes. The non-obvious impact is that individuals appealing denials effectively subsidize insurer liquidity by prolonging their own claim status in a liminal, statistics-friendly but human-costly state.
Appeal Labor Externalization
Third-party medical review firms benefit from automated claim processing by becoming the de facto arbiters of medical necessity during appeals, because insurers outsource clinical justification to entities paid per evaluation with embedded incentives to align with denial frameworks. This system functions through contracted networks that standardize 'peer-reviewed' criteria in ways opaque to patients, shifting burden onto individuals to refute algorithmically-preferenced determinations. The overlooked reality is that appeal success often depends less on clinical truth than on navigating a secondary bureaucracy whose profitability depends on sustained dispute volume.
Data Exhaust Monopolization
Insurtech platforms benefit from automated claim processing by aggregating structured denial and appeal patterns into proprietary datasets that refine risk segmentation beyond actuarial basics, because every appeal generates behavioral metadata on persistence, comorbidity articulation, and provider alignment. This operates through back-end data pipelines that convert patient struggle into training inputs for future underwriting algorithms, a feedback loop invisible to individuals contesting decisions. The unacknowledged consequence is that each appeal denial appeal strengthens the system's capacity to identify and preemptively exclude 'high-effort claimants' in downstream products.