Corporate Hospital Consolidation: When Risks Outweigh Benefits?
Analysis reveals 5 key thematic connections.
Key Findings
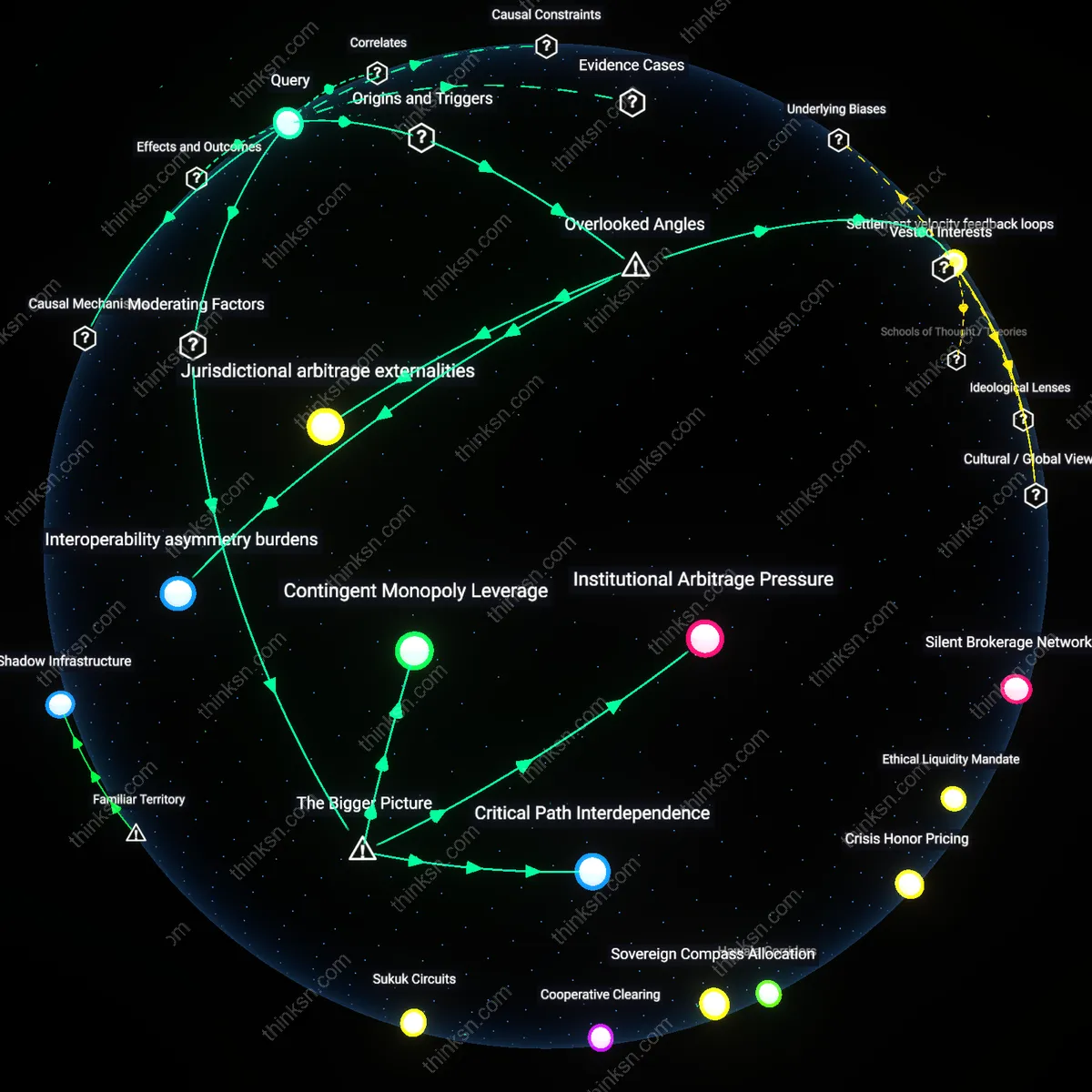
Regulatory Arbitrage Momentum
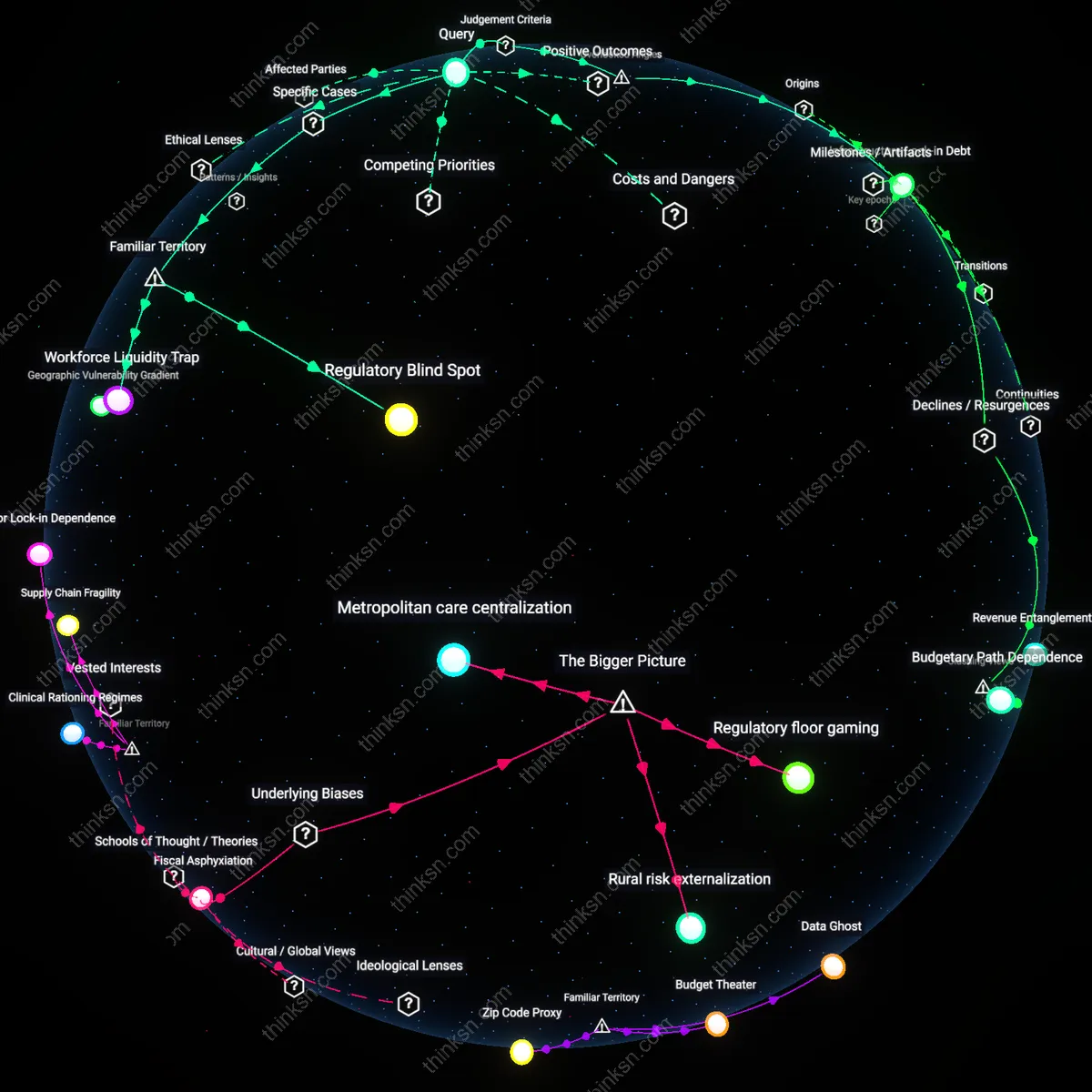
Hospital consolidation becomes systemically riskier than its efficiencies when state-level certificate-of-need laws are selectively weakened to attract corporate investment, thereby enabling national chains to exploit regulatory gaps while offloading uncompensated care onto isolated public hospitals. This shift creates a momentum-driven race to deregulate, where states compete to become hospitable to consolidated systems not by improving care but by absorbing externalities—eroding regional redundancy and mutual aid capacity. The non-obvious mechanism is not market concentration per se, but how fiscal incentives for state regulators generate self-reinforcing momentum in lowering oversight, privileging entry by systems designed to extract rather than sustain. This reframes systemic risk as politically subsidized erosion of care backstops, not mere price inflation.
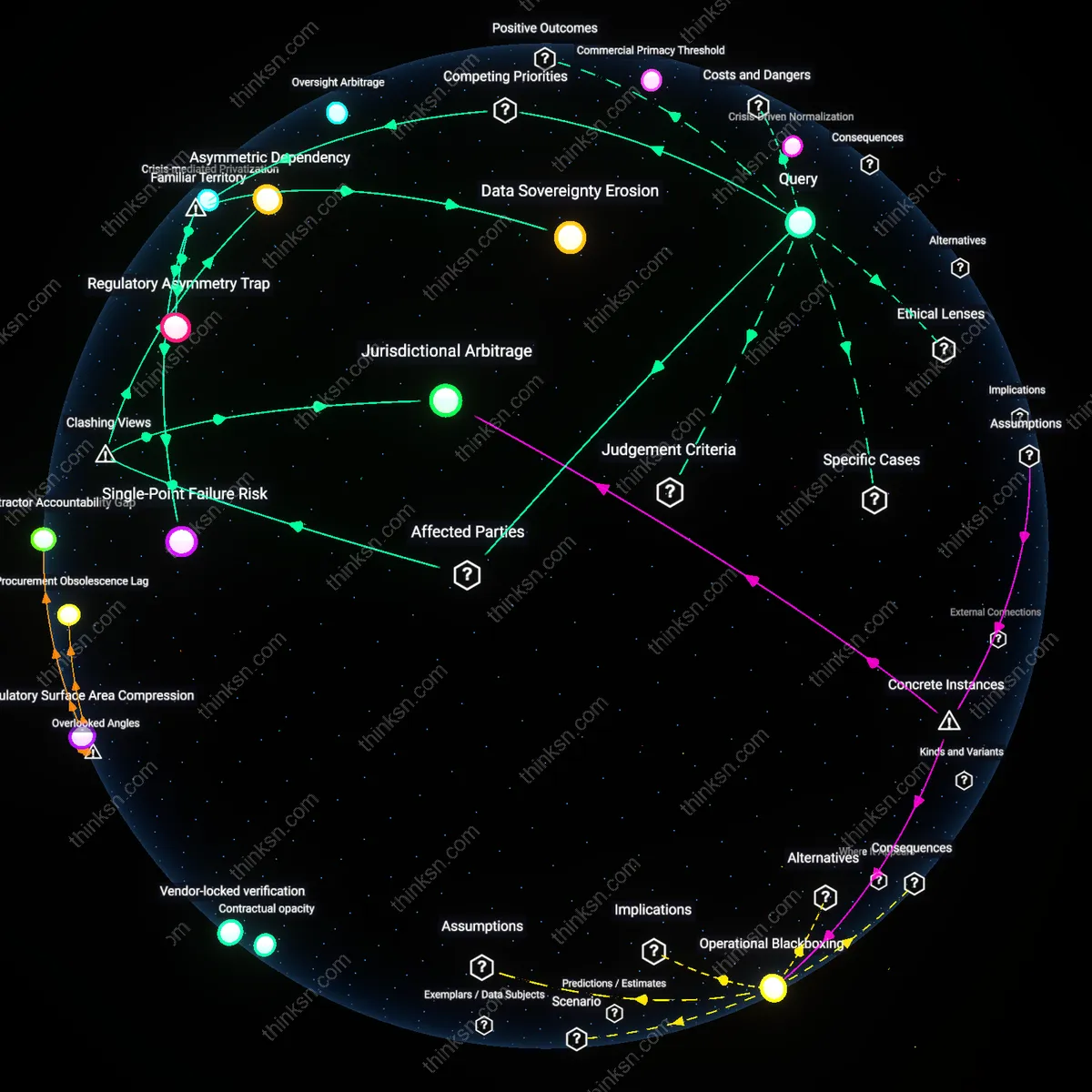
Infrastructure Lock-in Debt
The tipping point occurs when consolidated systems commit to proprietary digital infrastructure—such as unified EHR platforms or robotic surgery fleets—across acquired hospitals, generating irreversible capital outlays that force continued operation even as demographic demand shifts, especially in aging Appalachia or post-industrial Midwest towns. These sunk-cost systems cannot downsize or pivot because divestiture would trigger massive debt defaults, binding communities to underused, overstaffed facilities that drain public health budgets. The hidden dependency is not on patient volume but on financial covenants tied to technology leases, making closure politically and contractually impossible even when medically inefficient—transforming fixed assets into structural liabilities that pre-empt future care design.
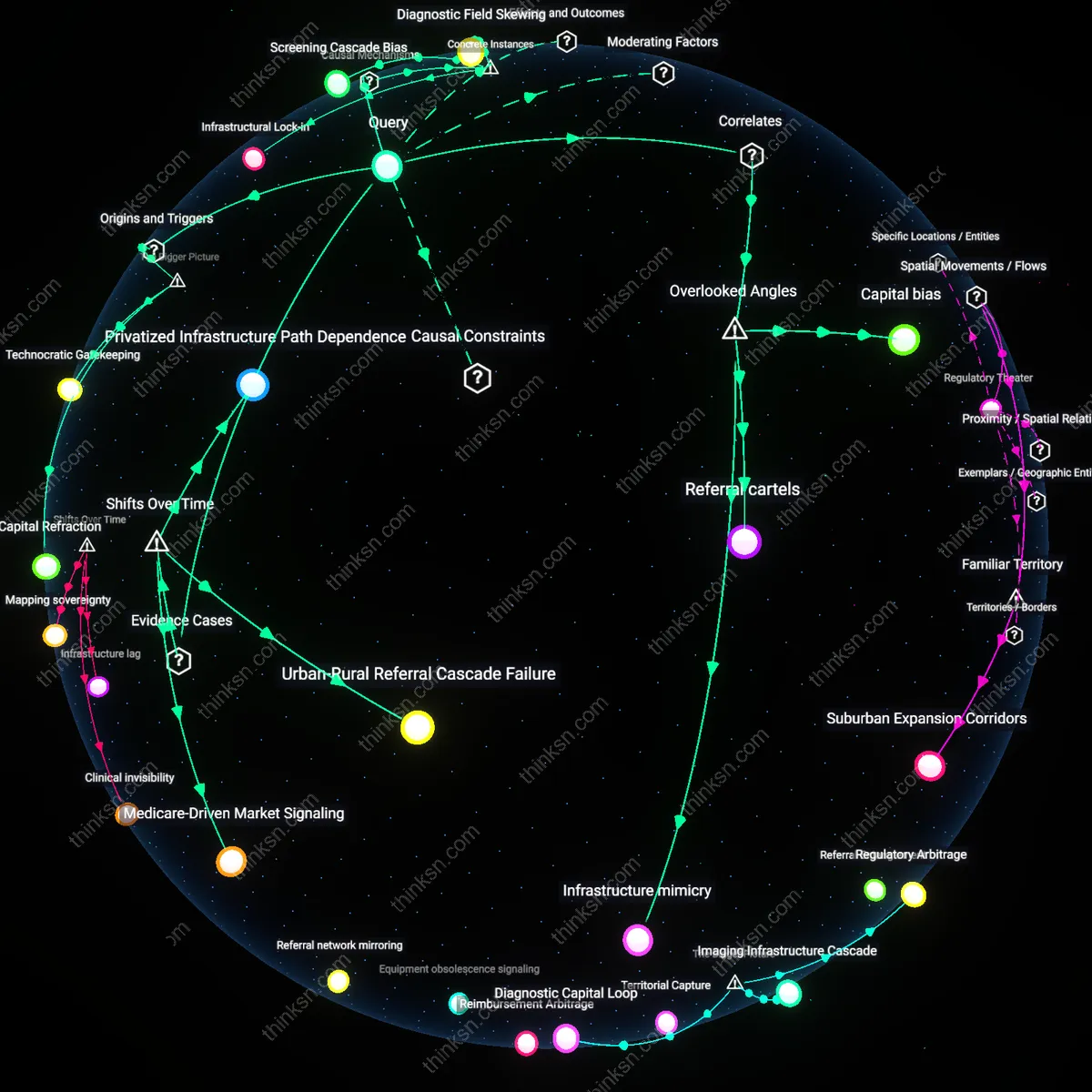
Supply Chain Monopoly
When a single corporate operator like CommonSpirit Health controls hundreds of hospitals across multiple states, it standardizes procurement through centralized vendors, creating reliance on a handful of suppliers for critical goods; this concentration means a disruption at one distribution hub—such as during the 2021 Texas winter storm that shuttered a major medical supply warehouse—can cascade into shortages across unaffiliated regional systems that depend on the same narrow supply chain. Most people associate hospital consolidation with local closures or pricing power, not with system-wide fragility baked into logistics networks, but the real risk emerges when corporate scale unintentionally creates single points of failure in sourcing and distribution.
Regulatory Blind Spot
When HCA Healthcare expands into new markets through acquisition, it leverages its national footprint to negotiate uniform terms with state regulators and Medicare administrators, effectively setting default standards that smaller systems must follow; this creates a feedback loop where regulators begin to design oversight frameworks around the practices of dominant operators, assuming their protocols are representative when they may instead reflect outlier efficiencies. The public tends to focus on how big hospital chains influence prices or care quality, but what goes unnoticed is how their size distorts the regulatory imagination—making it harder to detect or enforce alternatives that don’t fit the corporate model.
Workforce Liquidity Trap
In regions like rural Tennessee, where Ascension and HCA dominate nearly all acute care positions, nurses and technicians face a job market in which competing employers are not independent entities but divisions of the same parent corporations, leading to synchronized wage-setting and staffing policies; this eliminates meaningful labor mobility despite apparent competition, intensifying burnout during crises like the COVID-19 surge when workers couldn’t ‘vote with their feet’ by switching employers. While most assume consolidation only affects administrative overhead or billing, the deeper issue is how it freezes human capital in place—transforming geographic labor markets into internal talent silos that can’t adapt to systemic stress.