Should I Trust My Gut Over Joint Replacement Stats?
Analysis reveals 8 key thematic connections.
Key Findings
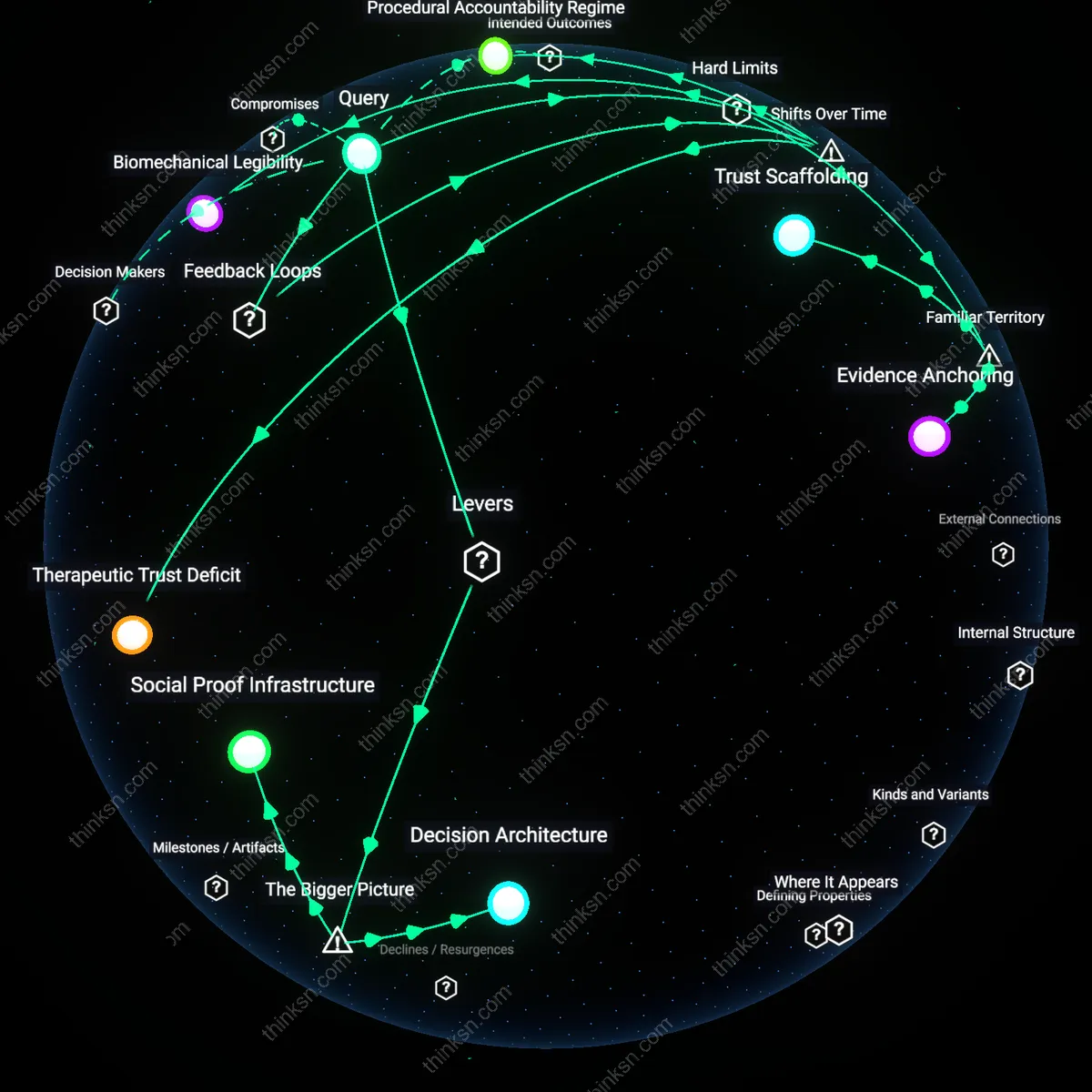
Trust Scaffolding
A shared decision-making protocol between orthopedic surgeons and primary care providers can align the patient’s lived experience with clinical data by contextualizing statistical benefits within personal risk narratives. This mechanism operates through coordinated pre-operative counseling sessions where probabilistic outcomes are translated into everyday consequences—such as mobility, pain levels, and independence—using visual aids and patient-specific baselines. The involvement of trusted primary care clinicians, whose relationships predate the surgical recommendation, counters the alienation many patients feel when confronted with impersonal success rates, making the unfamiliar recommendation feel continuous with prior care. Although shared decision-making is widely endorsed, its function here as a structural bridge—rather than a procedural box-checking exercise—is underappreciated in routine orthopedic practice, where scheduling silos often segregate specialties.
Evidence Anchoring
Selective presentation of longitudinal patient-reported outcome measures (PROMs) from demographically matched cohorts creates a relatable evidentiary framework that reduces the psychological distance between abstract survival statistics and personal consequence. This works through electronic health record-integrated dashboards in outpatient clinics that display real-world trajectories—like ‘patients in their 70s from this region who delayed versus pursued replacement’—thereby embedding statistical superiority within familiar life patterns. The mechanism leverages social proof without generalization, exploiting the high-recall association between peer experience and medical credibility. What’s rarely acknowledged is how deeply outcome statistics are discounted when stripped of narrative continuity, even when patients rationally accept their validity.
Effort Calibration
Rehabilitation milestone modeling—co-developed by physical therapists and patients before surgery—translates the statistical probability of functional improvement into a tangible sequence of effort-bound achievements, replacing abstract success metrics with concrete proximal goals. This process functions by mapping clinical outcomes (e.g., 90% pain reduction at 6 months) onto incremental, observable tasks such as stair navigation or unassisted transfers, tracked through wearable-informed logs reviewed weekly. The framework respects hard limits of insurance-covered therapy sessions and outpatient access by front-loading patient agency in goal setting, transforming reluctance from resistance to pacing. While rehabilitation is presumed to follow surgery, its preemptive structuring as a joint author of expected benefit reframes compliance as co-ownership, a shift rarely codified in preoperative workflows despite its intuitive resonance with patient autonomy.
Decision Architecture
Standardizing preoperative decision aids in orthopedic care pathways compels clinicians to structure patient discussions around probabilistic outcomes, converting abstract statistics into tangible trade-offs. Health systems like Kaiser Permanente have implemented mandatory decision support tools for joint replacement, leveraging clinical workflows to embed evidence-based narratives directly into the physician-patient encounter—this shifts decision-making from emotional impulse to deliberative comparison, operationalized through the routinization of choice. The non-obvious force here is not patient education per se, but the procedural requirement of engagement, which transforms statistical evidence into a systemic input rather than an optional add-on.
Social Proof Infrastructure
Integrating peer patient outcome data into preoperative counseling through digital platforms generates socially grounded validation of statistical benefits, making population-level evidence feel personally relevant. At institutions like the Mayo Clinic, secure patient networks now allow individuals considering joint replacement to view anonymized recovery trajectories and functional improvements of prior patients with similar profiles—this reframes reluctance by situating risk perception within observable peer experience. The breakthrough is that statistical credibility is not overcome cognitively but displaced socially, where trust in shared experience becomes the medium through which impersonal data achieves persuasive power.
Therapeutic Trust Deficit
A personalized risk communication protocol embedded in orthopedic clinics after the 2010s evidentiary shift toward value-based care converts statistical evidence into longitudinal trust-building, countering patient reluctance not by overriding intuition but by aligning it with iterative clinical feedback. This mechanism operates through recurring shared decision-making encounters where statistical trends are reinterpreted as individual trajectories, involving primary care physicians, surgeons, and digital health tools that log symptom progression—transforming population-level data into a patient-specific narrative arc. The non-obvious element is that statistical persuasion fails unless it is temporally mirrored in the patient’s experience; only when evidence evolves *with* the patient does it gain adherence, revealing that the post-2010 data-intensive turn in orthopedics exposed a *therapeutic trust deficit*—a gap not in knowledge, but in the pacing of trust formation across time.
Biomechanical Legibility
The integration of motion-analysis imaging into preoperative assessment since the 2010s reframes joint replacement from an actuarial recommendation into a visibly imperative by making functional decline biomechanically legible, thereby stabilizing patient acceptance despite initial reluctance. Radiologists, physical therapists, and surgeons now co-produce dynamic gait visualizations that depict joint deterioration as a visible trajectory, altering patient perception not through abstract survival statistics but through embodied recognition of instability—a reinforcing loop where imaging validates clinical advice, which prompts further testing, deepening commitment to intervention. The underappreciated shift is that prior to widespread gait labs in orthopedic centers (c. 2012–2015), joint failure was inferred from pain reports; now, its progression is seen, producing *biomechanical legibility* as the residual condition that makes statistical benefits personally undeniable.
Procedural Accountability Regime
The post-2005 expansion of national joint registries in Sweden, the UK, and eventually the US created a feedback loop in which surgeon performance and implant longevity became publicly traceable, shifting patient reluctance from resistance to statistical skepticism toward demand for procedural accountability. As revision rates and implant-specific outcomes circulated not as abstract averages but as surgeon- and hospital-branded metrics, patients began to condition consent on transparency, transforming intuitive doubt into a systematic lever for quality improvement. This marks a break from the pre-registry era (before ~2003), when outcomes were invisible and statistics felt impersonal; now, persistent reluctance has been recast into a stabilizing force—*procedural accountability regime*—where mistrust fuels data scrutiny rather than avoidance.