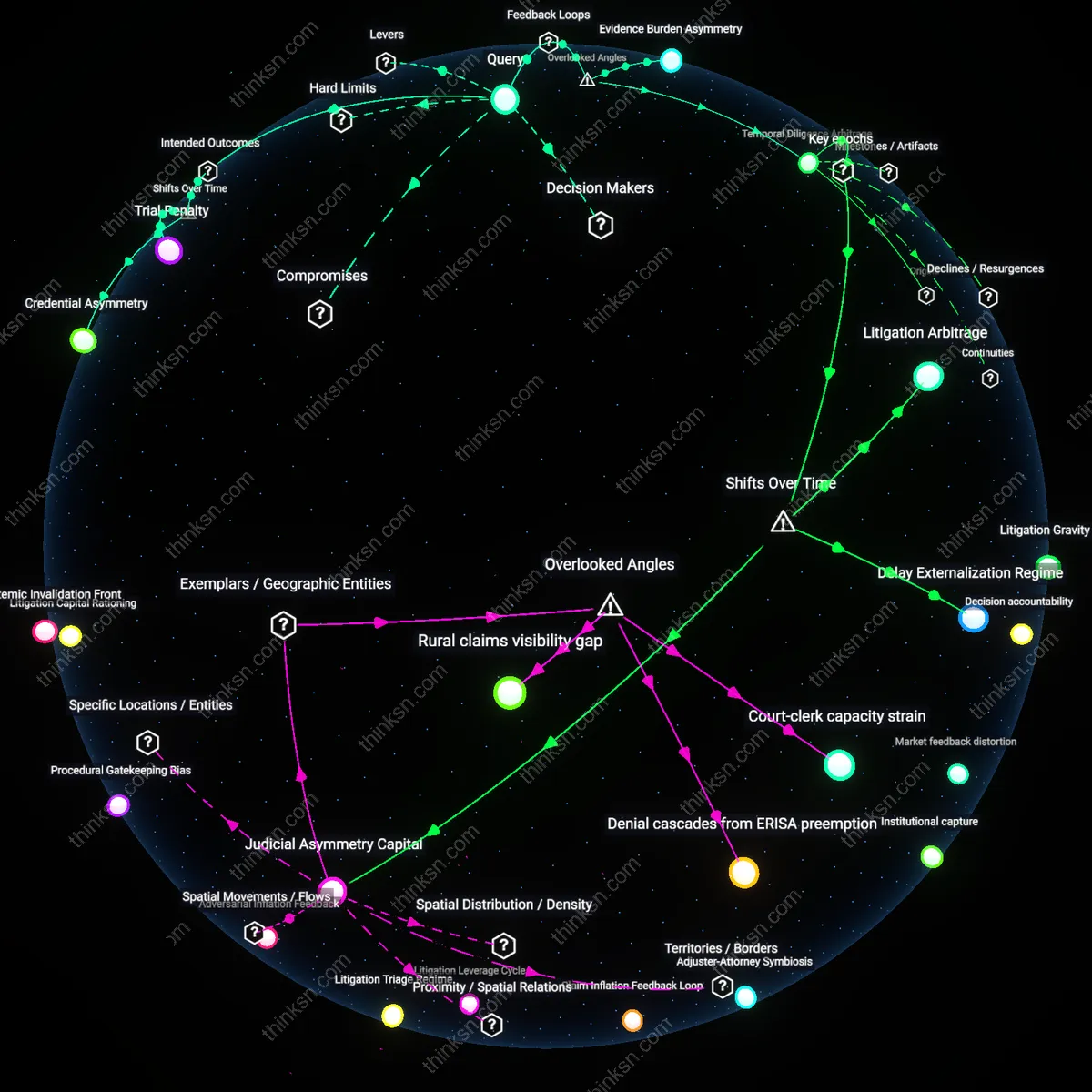
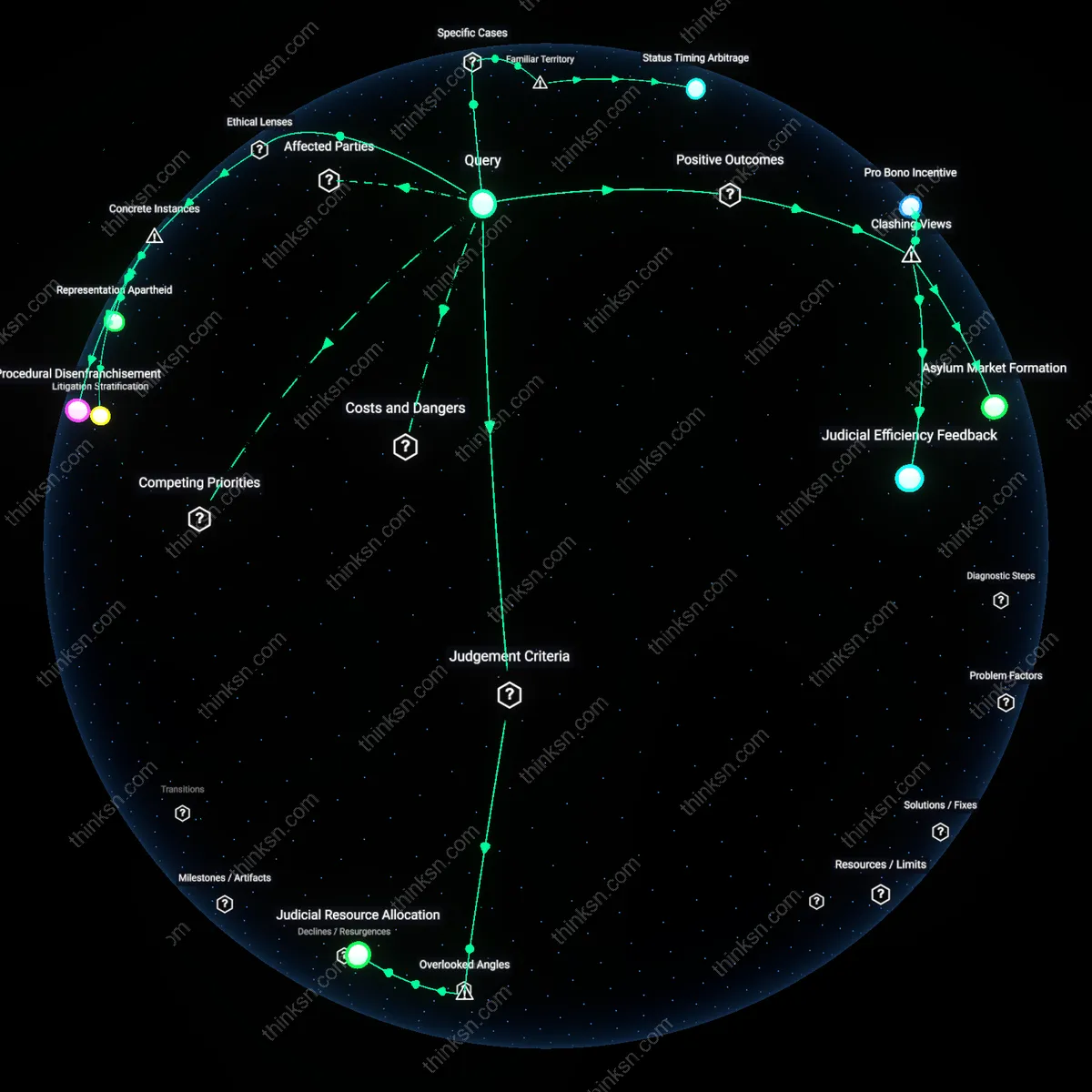
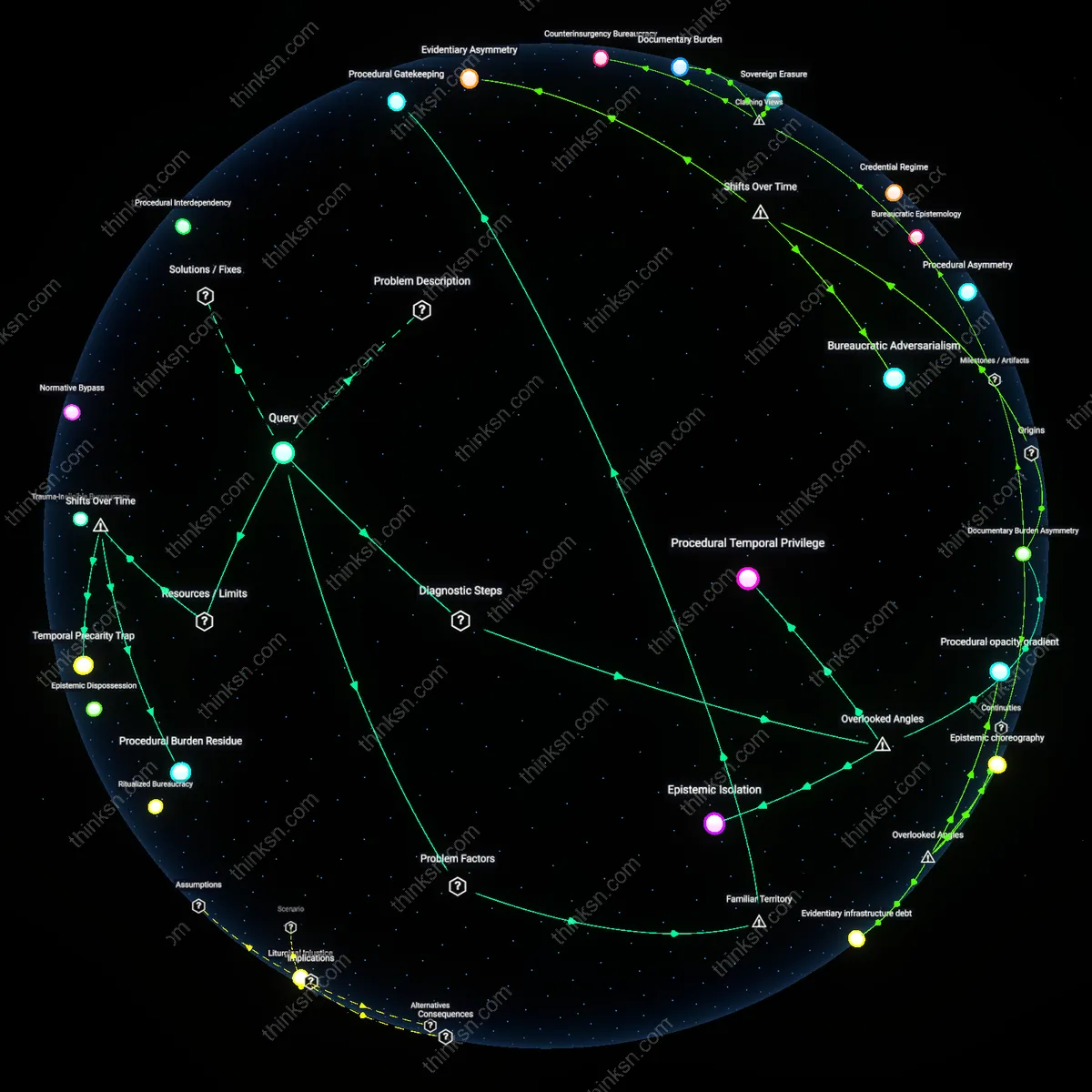
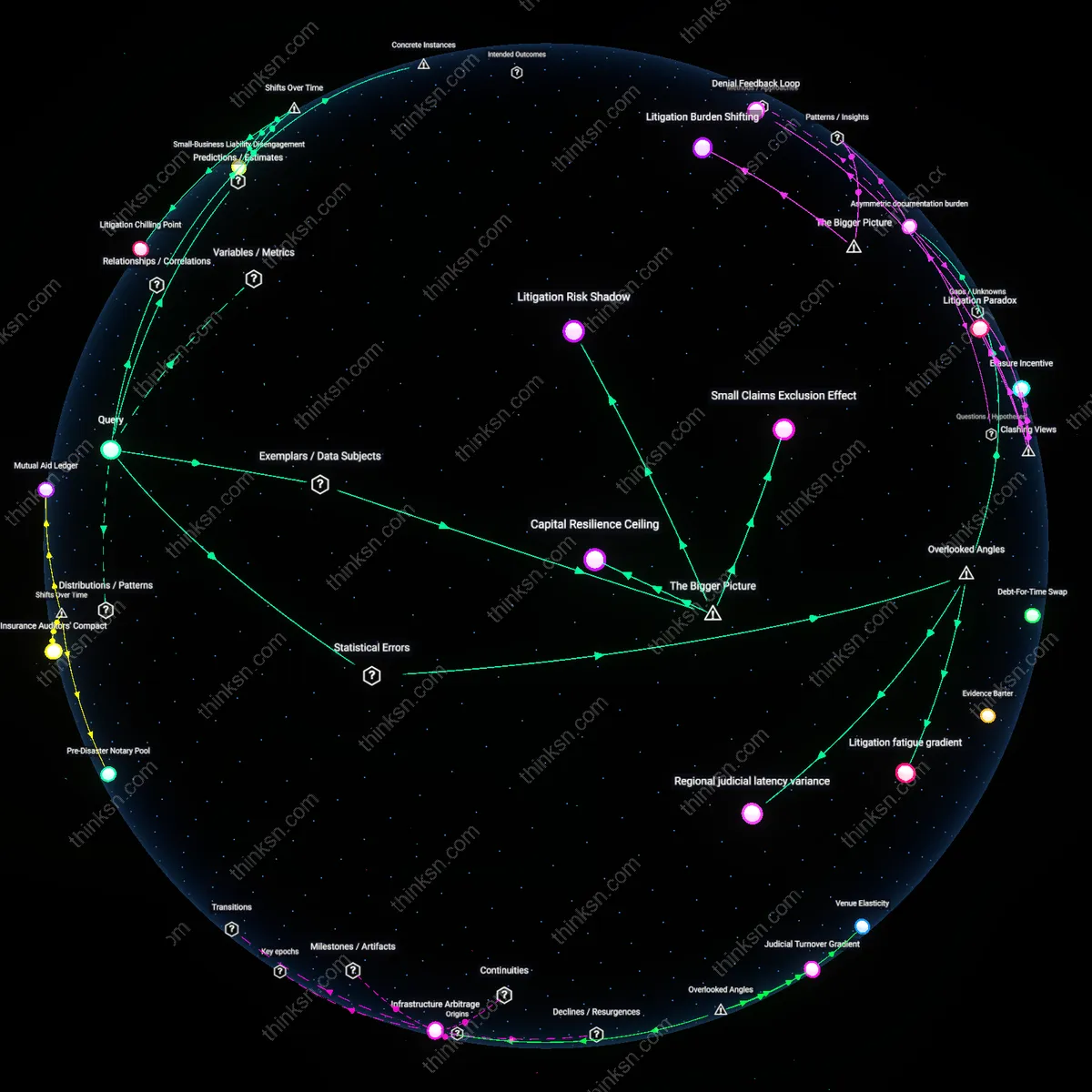
How Legal Counsel Disparities Skew Insurance Denial Outcomes?
Analysis reveals 6 key thematic connections.
Key Findings
Procedural Trauma Fatigue
Defendants in insurance denial lawsuits who face repeated procedural setbacks due to underresourced counsel are more likely to abandon litigation, reinforcing systemic inequity through attrition rather than merit. Each missed deadline or defaulted hearing—often stemming from overloaded public defenders or legal aid clinics—triggers a cascade of adverse consequences, including case dismissal and precedent erosion, which in turn reduces future legal capacity as funders observe low win rates. This feedback loop is non-obvious because most analyses focus on trial outcomes rather than cumulative procedural endurance, yet it determines who can remain in the system long enough to win. The mechanism operates through courts’ unflagging procedural neutrality, which becomes de facto bias when access to compliance resources is unequal.
Evidence Burden Asymmetry
Insurers systematically shift evidentiary burdens onto underrepresented policyholders in bad-faith denial cases by requiring granular documentation of unmet health needs, a dynamic hidden within evidentiary standards rather than courtroom power. Because well-resourced plaintiffs can muster retrospective medical records, expert affidavits, and treatment timelines—resources often unavailable to low-income claimants—courts implicitly validate denials not because they are legally correct, but because challenges cannot meet proceduralized proof thresholds. This overlooked mechanism stabilizes inequity by making the legal system’s legitimacy dependent on archivable suffering, a condition rarely recognized since evidentiary rules are assumed neutral. The reinforcing loop emerges when precedent built on incomplete records further narrows acceptable evidence, raising the bar for future claimants.
Temporal Diligence Arbitrage
Well-represented insurers exploit time-intensive motion practice to deplete the attention budgets of self-represent participans, creating a feedback loop where delay becomes a structural advantage. In states like Florida and Texas, where civil litigation timelines allow unlimited pre-trial motions, insurance firms with in-house legal teams file dilatory but technically valid challenges—such as discovery disputes over medical billing codes—knowing their opponents lack capacity to respond within required windows. This dynamic is overlooked because legal equity debates focus on access to lawyers, not access to sustained temporal engagement, yet it determines whether a case survives its first year. As unrepresented litigants fall behind, courts default to administrative rulings that favor the punctual, cementing a system where timeliness, not truth, determines justice.
Trial Penalty
Unequal access to counsel increases the rate at which claimants accept unfavorable settlements in insurance denial cases because delays in legal representation force time-constrained plaintiffs—especially low-income workers—into risk-averse decisions long before trial; this mechanism emerged prominently after the 1970s expansion of private health insurance and the simultaneous defunding of public interest law firms, which turned pretrial procedural delays into structural leverage for insurers, revealing how procedural timelines covertly penalize unrepresented litigants even when merits are strong.
Credential Asymmetry
The professionalization of medical underwriting from the 1990s onward elevated insurer reliance on clinically formatted documentation, which attorneys are uniquely trained to challenge through discovery and expert rebuttals, thereby widening outcome disparities between represented and unrepresented plaintiffs during administrative appeals; this shift entrenched legal expertise as a gatekeeper to medical credibility, exposing how insurance adjudication evolved from contract disputes into hybrid legal-clinical evaluations where representation determines epistemic legitimacy.
Funding Arbitrage
After the 2008 recession, state-level cuts to civil legal aid coincided with the rise of litigation financing for plaintiff law firms specializing in insurance appeals, creating a bifurcated system where access to representation increasingly depends on the perceived profitability of a case rather than the severity of harm, which has redirected advocacy toward higher-benefit claims and away from chronically ill, low-income patients, revealing how financialization of legal risk has replaced needs-based access with market-driven triage.