Do Settlement Secrets Hide Hospital Bias?
Analysis reveals 5 key thematic connections.
Key Findings
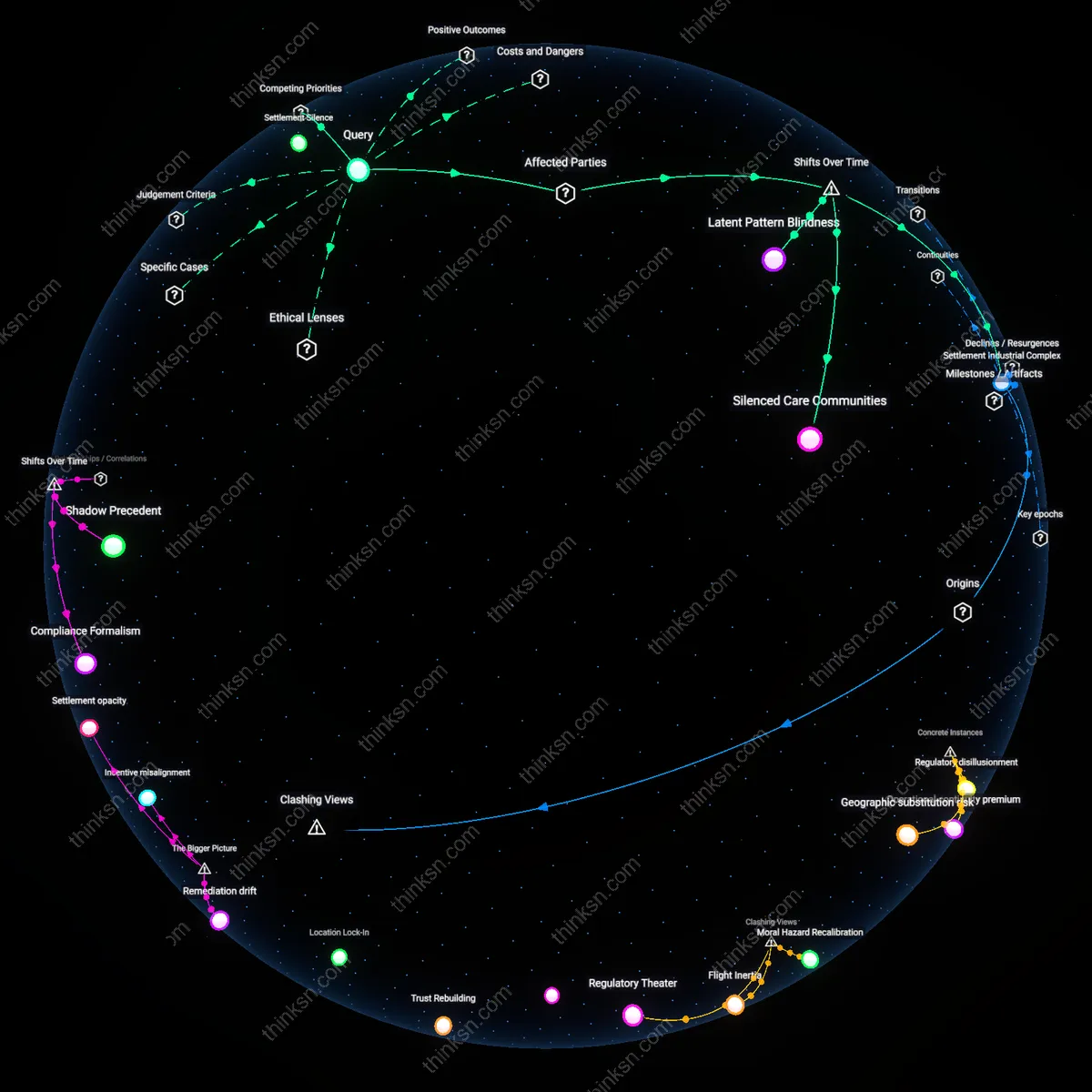
Silenced Care Communities
Confidentiality in hospital discrimination settlements erodes collective memory among clinical staff, undermining efforts to combat systemic bias by severing intergenerational learning among nurses, resident physicians, and support workers. Following the professionalization of hospital risk management in the 1990s, legal settlements began shifting from informal peer resolutions to legally sealed agreements, replacing moral reckonings with liability containment; this institutionalized amnesia prevents frontline teams from recognizing recurring patterns of racial or gender-based mistreatment, particularly in maternity and emergency units where implicit bias has measurable outcomes. The non-obvious consequence is not just suppressed data, but the systemic dismantling of informal knowledge networks that once allowed hospital subcultures to self-correct.
Settlement Industrial Complex
The expansion of confidential settlements since the 2003 passage of the Health Insurance Portability and Accountability Act (HIPAA) amendments redirected civil rights accountability into a privatized redress economy dominated by insurers, hospital legal teams, and outside counsel. This transition transformed discrimination claims from public health imperatives into financial risk calculations, where repeat offending institutions optimize on paying dispersed, invisible settlements rather than reforming hiring or care protocols; teaching hospitals in urban centers like Chicago and Los Angeles now exhibit measurable settlement clustering by race and department, invisible to accreditation bodies. The underappreciated shift is not secrecy per se, but the emergence of a financialized ecosystem that profits from unresolved systemic flaws.
Latent Pattern Blindness
Federal non-disclosure norms established during the managed care revolution of the 1990s disabled regulatory surveillance by fragmenting evidence of bias across hundreds of unreportable cases, preventing agencies like the Office for Civil Rights or state health departments from detecting institutional trends. Unlike workplace discrimination in other sectors—where EEOC data enables pattern recognition—healthcare’s legal settlements remain siloed, so a hospital cited for anti-LGBTQ+ practices in endocrinology may win Joint Commission accreditation months later. The critical transition occurred when tort reform and patient privacy law converged post-2000, masking systemic repetition as isolated incidents, and producing a regulatory environment blind to recurrence despite increasing public reporting mandates elsewhere.
Settlement Silence
Confidentiality in hospital discrimination settlements obstructs public accountability by preventing victims and advocacy groups from aggregating and publicizing patterns of misconduct. Hospitals, insurers, and legal departments systematically leverage sealed agreements to isolate incidents, ensuring repeat offenses remain statistically invisible and legally unchallengeable as part of broader trends. This dynamic entrenches systemic bias by shielding institutions from reputational and regulatory consequences, a compromise most people overlook because they assume legal resolution implies corrective action—when in fact, silence often signals strategic containment.
Victim-Organization Tradeoff
Individual claimants in hospital discrimination cases often accept confidentiality to secure livelihood-stabilizing compensation, trading long-term systemic reform for immediate personal redress. Legal aid providers, hospitals, and mediators reinforce this exchange by presenting sealed settlements as the only viable path to timely justice in overburdened civil systems. The underappreciated reality, visible only through the lens of daily patient advocacy, is that victims’ urgent need for recovery routinely becomes the mechanism that suppresses institutional learning.