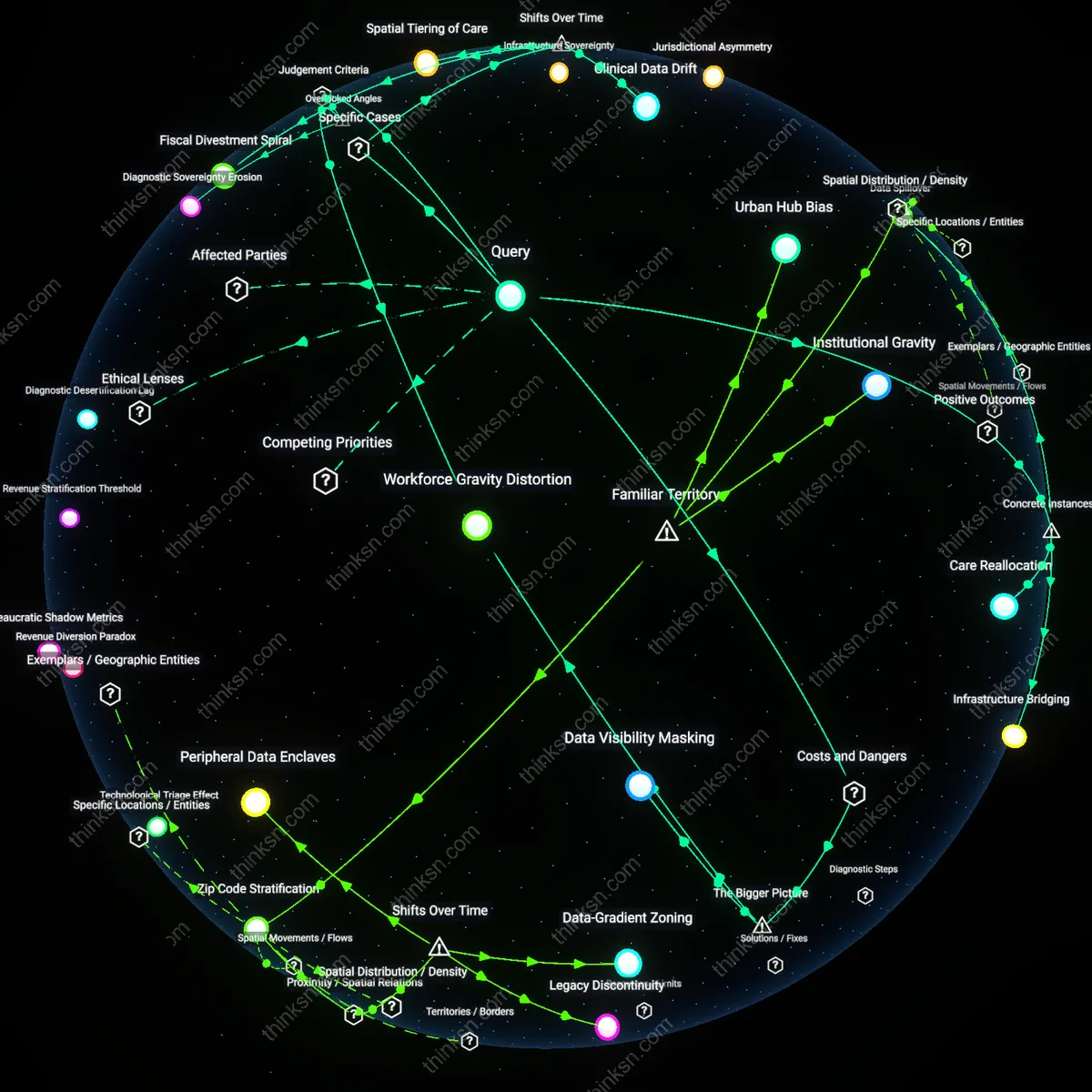
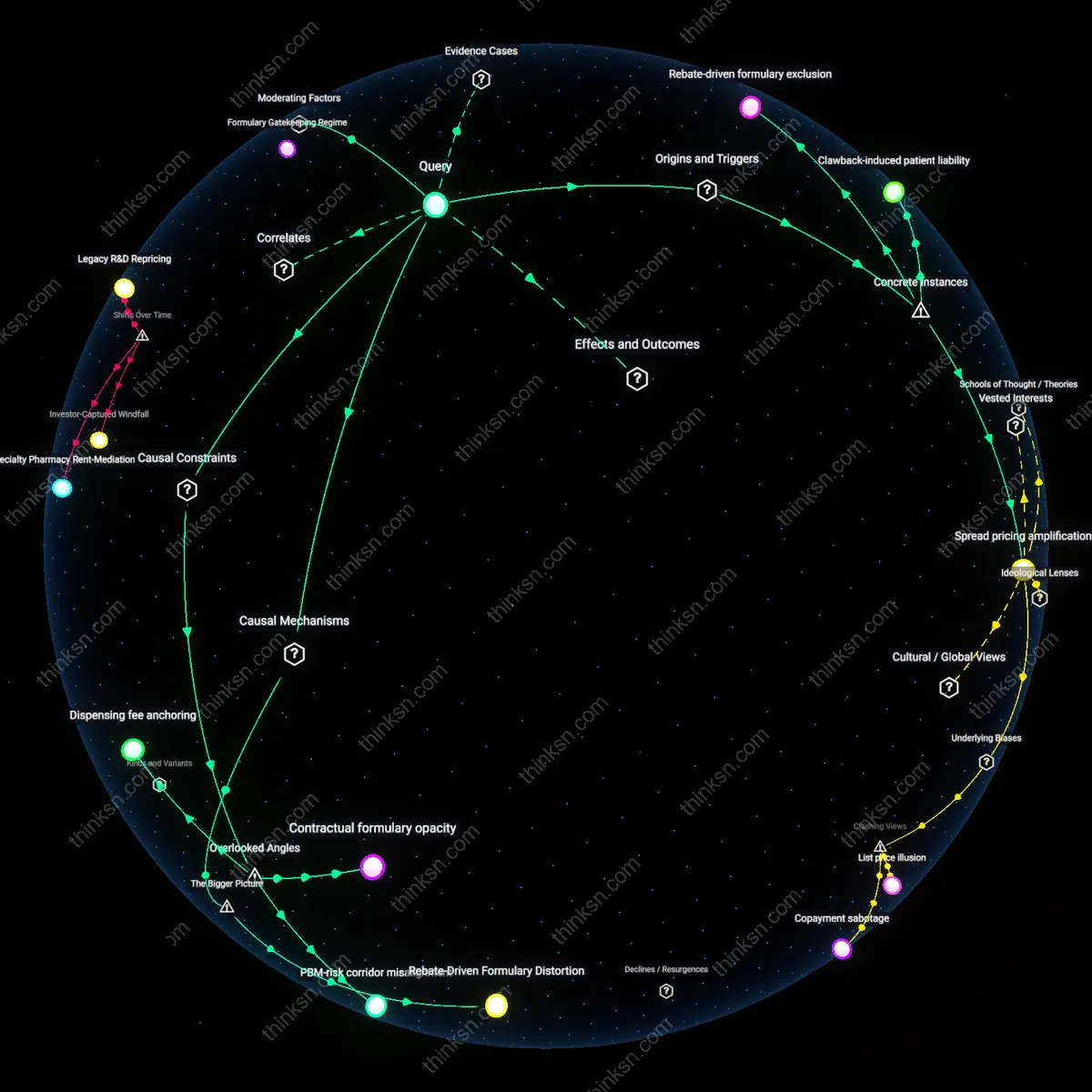
Do New Diabetes Drugs Work for Low-Income Patients?
Analysis reveals 10 key thematic connections.
Key Findings
Regulatory Inertia
Clinical trial homogeneity enables regulatory approval based on narrow efficacy data, which then locks in prescribing standards that ignore low-income populations’ metabolic diversity. Regulatory bodies like the FDA legitimize drug indications using trial results from predominantly white, insured cohorts, making it bureaucratically simpler to maintain these guidelines than to adapt them for underrepresented groups, even when post-market evidence shows differential responses. This creates a self-reinforcing cycle where real-world ineffectiveness in low-income communities is dismissed as non-compliance rather than a mismatch in biological or environmental response, obscuring systemic gaps in drug applicability. The non-obvious insight is that regulation—not just access or awareness—acts as a hidden gatekeeper that naturalizes trial biases.
Commercial Disregard
Pharmaceutical companies deprioritize real-world validation in low-income settings because post-approval studies in these populations do not enhance revenue under current reimbursement models. Once a drug is approved and marketed to insured populations, there is minimal financial incentive to fund research in safety-net clinics where formulary decisions are price-sensitive and innovation uptake is slow. As a result, clinicians in community health centers lack locally relevant evidence to justify prescribing newer, costlier diabetes drugs, not due to ignorance but because the evidentiary standard is commercially mediated. This reframes the knowledge gap not as a scientific shortfall but as a deliberate market-driven omission.
Therapeutic Alienation
Low-income patients often reject new diabetes drugs not due to access alone but because clinical trial designs ignore the lived conditions—such as food insecurity or shift labor—that shape medication adherence and glucose patterns. When trials assume regular meal timing and stable routines, the resulting dosing regimens feel alien or unworkable in precarious daily environments, leading to distrust in both the drug and the prescriber. This mismatch produces therapeutic alienation, where medical authority is undermined not by misinformation but by the experiential irrelevance of evidence-based protocols. The dissonance reveals that clinical validity is not just biological but also sociotemporally embedded.
Distributional friction
Clinical trial participant mismatch reduces trust among low-income community pharmacists, who then hesitate to recommend new diabetes drugs, slowing diffusion even when prescribed. Local pharmacy gatekeepers—especially independent or clinic-affiliated dispensers in underserved urban areas—rely on experiential familiarity and peer consensus when advising patients; when trial populations lack demographic resonance with their patient base, pharmacists perceive the evidence as less generalizable and are more likely to default to older, familiar medications. This dynamic is rarely captured in health policy models, which assume passive transmission from prescriber to dispenser to patient, but the pharmacist’s epistemic caution acts as a hidden checkpoint that can decelerate adoption, particularly for drugs with narrow therapeutic indices or complex dosing. The overlooked role of frontline pharmacy judgment introduces distributional friction—a non-market, non-regulatory delay mechanism rooted in perceived evidentiary adequacy at the point of care delivery.
Infrastructure legibility
New diabetes drugs optimized in trial settings dominated by high-income, well-resourced clinics fail to align with the diagnostic rhythms of safety-net clinics, making them harder to integrate into routine workflows. In low-income communities, primary care visits are often brief, triage-driven, and lack consistent HbA1c or continuous glucose monitoring follow-up, so therapies requiring precise glycemic baselines or titration schedules become de facto incompatible with the tempo and data availability of actual practice. Unlike typical analyses that focus on cost or patient adherence, this mismatch reveals how drug usability is co-determined by the legibility of the care infrastructure—the extent to which a treatment can be parsed, tracked, and managed within existing clinical information flows. When new drugs demand a level of monitoring precision that the system cannot routinely produce, their clinical logic becomes opaque, reducing effective utilization regardless of approval status or insurance coverage.
Access Inertia
Clinical trial demographics dominated by insured, urban populations create regulatory approval pathways that assume patient access through specialty clinics, which directly limits real-world adoption in low-income communities reliant on understaffed public health centers. This mechanism operates through FDA reliance on homogenous efficacy data, causing formulary committees in safety-net hospitals to delay or reject new diabetes drug contracts due to unproven performance in their actual patient mix. What’s underappreciated is that even when low-income clinics want to adopt new therapies, procurement systems are structurally calibrated to trial-derived prescribing norms that don’t reflect their patients’ comorbidities or care continuity.
Trust Deficit
When clinical trials enroll few participants who look like or live like low-income patients, community members interpret new diabetes drugs as 'not meant for us,' which directly reduces adherence and early uptake even when drugs are available. This belief spreads through word-of-mouth networks in neighborhoods with historical memories of medical exploitation, where the visible absence of people like oneself in drug development becomes a proxy for corporate indifference. The non-obvious insight is that familiarity with the medical system doesn’t necessarily build trust—instead, repeated exposure to exclusionary trial designs reinforces the perception that innovation bypasses their needs altogether.
Prescribing Lag
Primary care providers in federally qualified health centers delay writing prescriptions for newly approved diabetes drugs because trial results lack data on patients with erratic follow-up or food insecurity, which directly causes hesitation when treating low-income populations with complex social risk factors. This dynamic flows through clinical decision support systems that flag new medications as 'high-risk' without real-world effectiveness studies in safety-net settings, making physicians default to older, less effective regimens. What’s rarely acknowledged is that provider caution isn’t due to resistance to change but stems from ethical concerns about applying population-level data to individuals whose lived conditions were never tested.
Regulatory feedback loop
Clinical trial demographic homogeneity disables post-market surveillance systems from detecting differential drug efficacy in low-income populations, because regulatory approval processes reward speed and statistical significance over population representativeness, embedding a systemic preference for homogeneity that persists into real-world prescribing patterns. This occurs because pharmaceutical developers optimize trials for FDA endpoints using insured, English-speaking, urban-suburban recruits—often excluding Medicaid enrollees or non-English speakers—which creates a regulatory feedback loop where drugs are approved without data on real-world social variability. The non-obvious consequence is that post-approval pharmacovigilance systems fail to correct for initial gaps, not due to inadequate monitoring, but because downstream data is interpreted through clinical trial baselines that never included the physiologically distinct metabolic profiles shaped by poverty-driven comorbidities like food insecurity or chronic stress.
Formulary gatekeeping
Public health formularies in low-income communities adopt new diabetes drugs only after prolonged cost-effectiveness reviews, but these evaluations rely on trial-derived models that misestimate real-world adherence and complications, producing a formulary gatekeeping effect that delays access precisely where metabolic outcomes are worst. This bottleneck exists because Medicaid Managed Care Organizations and state pharmacy boards use clinical trial hazard ratios—generated in healthier, more adherent populations—to project long-term savings, failing to account for higher rates of insulin resistance, polypharmacy, or erratic care access in low-income settings. The underappreciated dynamic is that these agencies, under fiscal pressure, treat trial data as universally generalizable, thereby mistaking statistical validity for social validity, and reinforcing a cycle where drugs proven in affluent cohorts are deemed 'not cost-effective' for poorer ones due to misrepresented failure rates.