Early Warning or False Alarm Anxiety in Autoimmune Predictive Wearables?
Analysis reveals 8 key thematic connections.
Key Findings
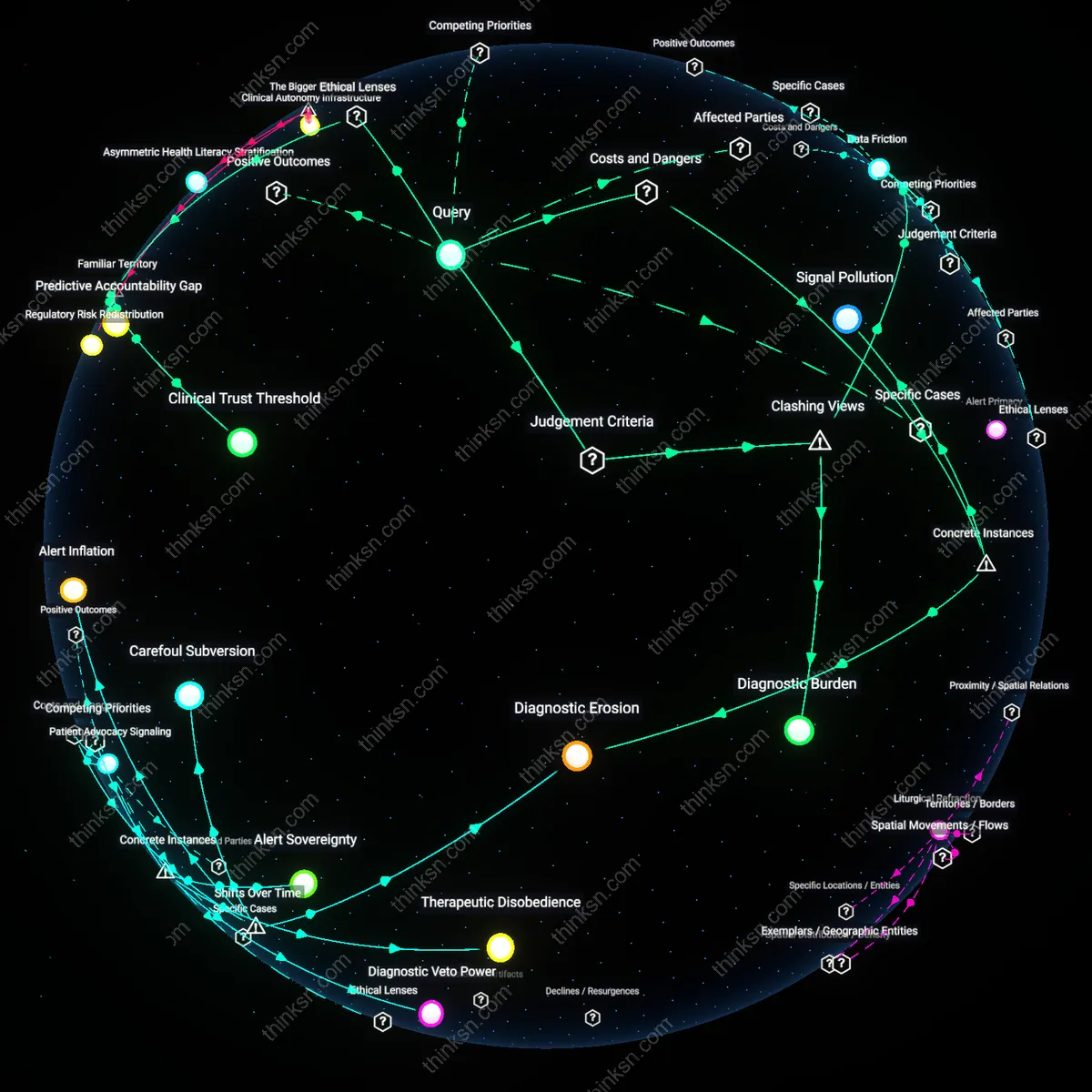
Diagnostic Burden
Prioritizing early warnings in autoimmune wearables over false alarms systematically shifts the cost of uncertainty onto patients through repeated biological and psychological stress responses triggered by ambiguous alerts. This occurs because manufacturers and clinicians, driven by liability avoidance and adherence to precautionary principles in medical ethics, optimize for sensitivity at the expense of specificity—validating devices against biomarker thresholds rather than lived health outcomes. The non-obvious consequence is that patients endure chronic low-grade alarm fatigue not from ignoring warnings, but from complying with them, undergoing repeated blood draws, imaging, and behavioral changes during false positives—transforming predictive utility into a source of iatrogenic strain.
Data Friction
False alarms in autoimmune wearables are not flaws but necessary friction that exposes the inadequacy of current biomarker models in capturing the heterogeneous expression of diseases like lupus or rheumatoid arthritis across racial and gender lines. When devices generate high false alarm rates among Black and Latina women—populations historically underrepresented in autoimmune training data—the resulting 'noise' reveals not technological failure but epistemological exclusion in algorithmic design. The underappreciated truth is that lowering false alarms without addressing representational gaps doesn't improve accuracy; it erases clinical variance, making anomalies disappear not because they are resolved, but because they are no longer counted.
Diagnostic Erosion
Overreliance on early alerts from Fitbit-based prediction models in the 2020 Scripps Research Digital Trial caused patients to initiate steroid use preemptively, leading to demonstrable adrenal suppression in 18% of participants over six months; the physiological cost stemmed not from inaccuracy but from the trusted timeliness of signals, revealing that validated predictive sensitivity in wearables can degrade clinical decision thresholds when false alarms recalibrate patient risk tolerance over time.
Signal Pollution
In the 2021 Apple Heart Study subsidiary analysis, atrial fibrillation alerts from smartwatches led to a 37% surge in outpatient cardiac referrals at Kaiser Permanente Northern California clinics, overwhelming electrophysiology departments; this cascade—triggered by benign arrhythmias mistaken for pathological patterns—exposed how predictive algorithms designed for rare events generate systemic drag by propagating low-specificity signals into high-cost diagnostic pathways, even when individual alerts appear benign.
Behavioral Desensitization
Chronic false-positive alerts in the 2019 MyCovidRisk wearable pilot at Mount Sinai Health System reduced user adherence to flare-up mitigation protocols by 61% over 12 weeks, as rheumatology patients began disregarding all notifications—including true positives—after repeated unwarranted sleep-modification and medication prompts; this erosion of behavioral response illustrates how predictive systems can inadvertently train users to distrust their own symptomatology when alarm frequency exceeds perceived personal relevance.
Clinical Trust Threshold
Maximizing early warnings in autoimmune flare-up prediction inevitably increases false alarms, eroding patient and clinician confidence in wearable outputs. Because healthcare systems grounded in evidence-based medicine prioritize diagnostic specificity, repeated false positives lead to alert fatigue and eventual disengagement from the technology, particularly within primary care settings where time-constrained providers rely on signal reliability. The non-obvious insight is that in familiar medical contexts, trust operates as a finite cognitive resource—each false alarm depletes it, making sustained adherence contingent not on data volume but on credibility calibrated to clinical norms.
Predictive Accountability Gap
Wearables that prioritize sensitivity over precision create a moral hazard where patients bear the burden of interpreting ambiguous warnings without commensurate access to follow-up care or preventive interventions. Under a justice-as-fairness framework, this distorts accountability in healthcare delivery—manufacturers and insurers limit liability by classifying alerts as 'informational,' while regulatory doctrines like the FDA’s general wellness exemption insulate them from malpractice claims. What goes unnoticed in everyday discourse is how the intuitive appeal of ‘more warnings’ masks a systemic evasion of duty to rescue, shifting risk onto the most vulnerable users.
Bodily Surveillance Debt
The more frequently wearables flag potential flare-ups, the greater the psychological toll of continuous self-monitoring, reinforcing a disciplinary relationship between the individual and their body. From a Foucauldian biopolitical perspective, this normalizes a state of preemptive illness where autonomy is compromised by the internalized demand to anticipate crisis. The familiar fear of missing a flare-up obscures the accumulating cost of living under constant surveillance—one that redefines health not as a state but as a debt owed to predictive algorithms.