Why Do Real-World Drug Studies Often Show Lower Effectiveness?
Analysis reveals 8 key thematic connections.
Key Findings
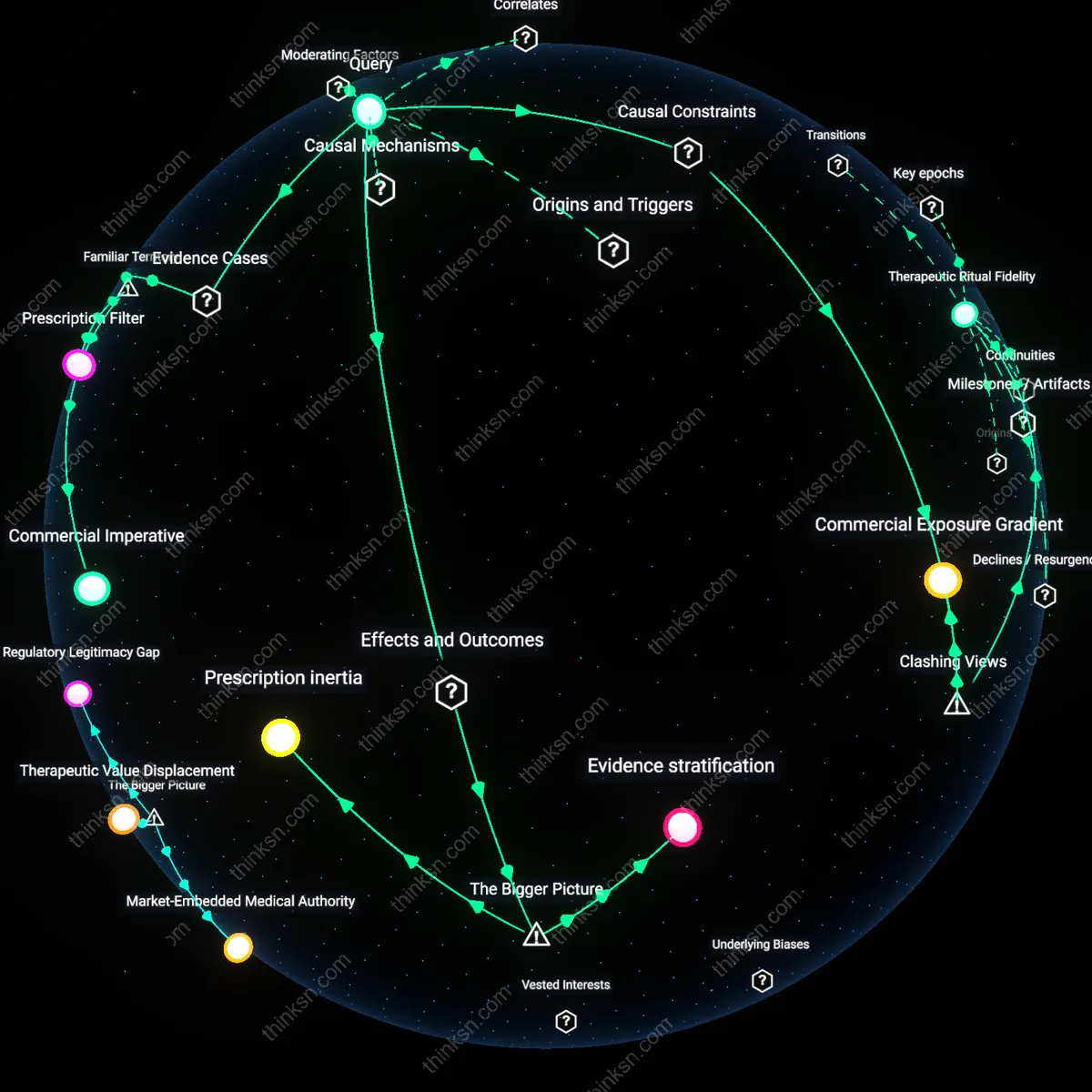
Prescription inertia
Lower real-world drug effectiveness directly triggers delayed de-adoption of the drug in clinical practice, because physicians rely on trial-based guidelines that are slow to update in the face of post-market observational data. Regulatory approvals and clinical guidelines insulate prescribers from real-time performance feedback, maintaining treatment protocols even as effectiveness erodes across diverse populations. This lag is systemically sustained by the misalignment between rapid evidence generation and sluggish institutional reform—clinicians are not incentivized to second-guess approved regimens absent strong contraindications. The non-obvious consequence is that diminished efficacy becomes normalized rather than treated as a signal for change, perpetuating a cycle where outdated standards persist despite mounting disconfirming evidence.
Evidence stratification
Discrepancies between trial and real-world effectiveness reinforce a two-tiered evidence hierarchy in health systems, where academic medicine privileges internal validity while public health systems grapple with external applicability. Pharmaceutical developers optimize trial designs for regulatory approval under controlled conditions, creating a performance gap when drugs encounter comorbidities, adherence issues, and suboptimal monitoring in routine care. This divergence is systemically enabled by fragmented data infrastructures that silo clinical trials from electronic health records, preventing timely integration of effectiveness signals. The underappreciated impact is that this structural separation legitimizes persistent uncertainty about true treatment value, shielding payers and providers from accountability for outcomes beyond trial-defined endpoints.
Therapeutic burden shift
Reduced real-world drug effectiveness redistributes therapeutic risk from manufacturers to patients and frontline health systems, as diminished returns necessitate higher treatment intensity or combination regimens. When a drug underperforms relative to trial results, clinicians compensate by escalating care—adding medications, increasing doses, or intensifying monitoring—without revising the underlying treatment logic. This dynamic is enabled by reimbursement models that reward procedural interventions over preventive optimization, amplifying downstream costs and patient harm. The overlooked systemic effect is that declining drug performance is absorbed locally rather than corrected upstream, transforming pharmaceutical shortfalls into chronic system-level inefficiency.
Therapeutic Ritual Fidelity
Real-world drug effectiveness gaps arise not from scientific failure but from the erosion of ritualized adherence structures that clinically defined protocols depend on; in pivotal trials, patients are embedded in highly supervised, institutionally reinforced routines—daily pill counts, scheduled lab draws, behavioral nudges—whose ritual discipline is absent in decentralized care, where no equivalent system enforces the same temporal and symbolic commitment to treatment. This reveals that pharmaceutical efficacy is co-produced by ceremonial compliance mechanisms that real-world settings do not replicate, challenging the assumption that biological activity alone drives outcomes.
Commercial Exposure Gradient
The decline in observed drug performance reflects a shift from trial-enriched cohorts to commercially driven distribution, where payers and providers prioritize early access over patient stratification, incentivizing use before biomarker-defined responder subgroups are operationally identifiable in routine care; as a result, drugs are systematically exposed to non-responders at scale, breaking the causal link between mechanism and outcome that was preserved in genetically or clinically selected trial populations. This exposes the market—not medicine—as the dominant force shaping therapeutic exposure, contradicting the framing of real-world data as a neutral reflection of clinical reality.
Commercial Imperative
Drug developers optimize trial conditions to demonstrate maximum efficacy, enrolling highly selected patients without comorbidities and ensuring strict adherence through intensive monitoring. This creates an artificial environment starkly different from routine clinical practice, where patients have complex health profiles and variable compliance—conditions visible in post-market studies like those tracking SGLT2 inhibitors in diverse primary care populations across the U.S. Medicare system. The familiar idea that 'clinical trials show best-case results' masks the systemic economic incentive to engineer such conditions, revealing how commercial goals shape what counts as evidence.
Prescription Filter
Physicians prescribe new drugs first to patients they believe will respond best, often excluding those who resemble the frailer, older, or less adherent individuals seen in real-world settings. This 'optimism bias' in early adoption is evident in the rollout of PCSK9 inhibitors, where initial use concentrated in cardiology clinics treating motivated, high-income patients with clean risk profiles, not the broader atherosclerotic population seen in claims databases. While people commonly say 'doctors use drugs differently outside trials,' they overlook how physician triage itself distorts real-world effectiveness downward once broader use begins.
Regulatory Threshold
Regulatory agencies approve drugs based on statistically significant benefits in controlled trials, even when those benefits are modest or measured in surrogate endpoints like tumor shrinkage rather than survival—a pattern clear in oncology approvals such as those for accelerated indications of immune checkpoint inhibitors. The public assumes approval means 'works well for most people,' but the real mechanism is a calibrated leniency that accepts uncertainty, expecting post-market data to temper expectations, which systematically produces the gap between initial hype and later observed performance in electronic health record studies.