Why Does Insurance Favor Brand Names Over Clinically Equivalent Generics?
Analysis reveals 11 key thematic connections.
Key Findings
Regulatory signaling
The FDA’s approval pathway for brand-name drugs establishes a perception of therapeutic primacy that insurers treat as a proxy for clinical reliability, even when generics are bioequivalent. When Merck’s Singulair (montelukast) faced generic entry in 2012, many insurers retained prior authorization requirements for the brand despite equivalence, because the drug’s initial approval under a full New Drug Application (NDA) created an enduring administrative imprint. This mechanism operates through regulatory memory—where the intensity and scrutiny of the original approval process become embedded in payer risk assessment protocols—revealing that regulatory signaling functions not just as a gatekeeper but as a persistent hierarchy marker in coverage decisions.
Formulary anchoring
Pharmacy benefit managers (PBMs) like Express Scripts anchor drug utilization patterns through initial formulary placement, which persists even after generics enter. When AstraZeneca’s Nexium (esomeprazole) launched in 2001, it was strategically placed on preferred tiers ahead of generic omeprazole, shaping prescribing habits through physician path dependency. Even after generics became available, the entrenched use pattern influenced insurers to maintain brand-name coverage constraints—such as step therapy—because shifting behavior required active de-escalation, a system inertia that exposes formulary anchoring as a structural determinant of insurance design beyond clinical or cost considerations.
Litigation imprinting
Brand-name drugs that have been subject to large-scale litigation acquire risk-averse coverage protocols that outlast the legal cases themselves. After Wyeth’s Fen-Phen (fenfluramine/phentermine) litigation in the late 1990s, insurers began imposing stricter prior authorization and monitoring requirements on all brand-name weight-loss medications, including subsequent entries like Xenical (orlistat), even when structurally unrelated. This occurs because liability exposure imprints on payer risk models, activating durable compliance architectures that treat brand-name status as a surrogate for litigation vulnerability—revealing that legal history, not clinical profile, can drive insurance stringency.
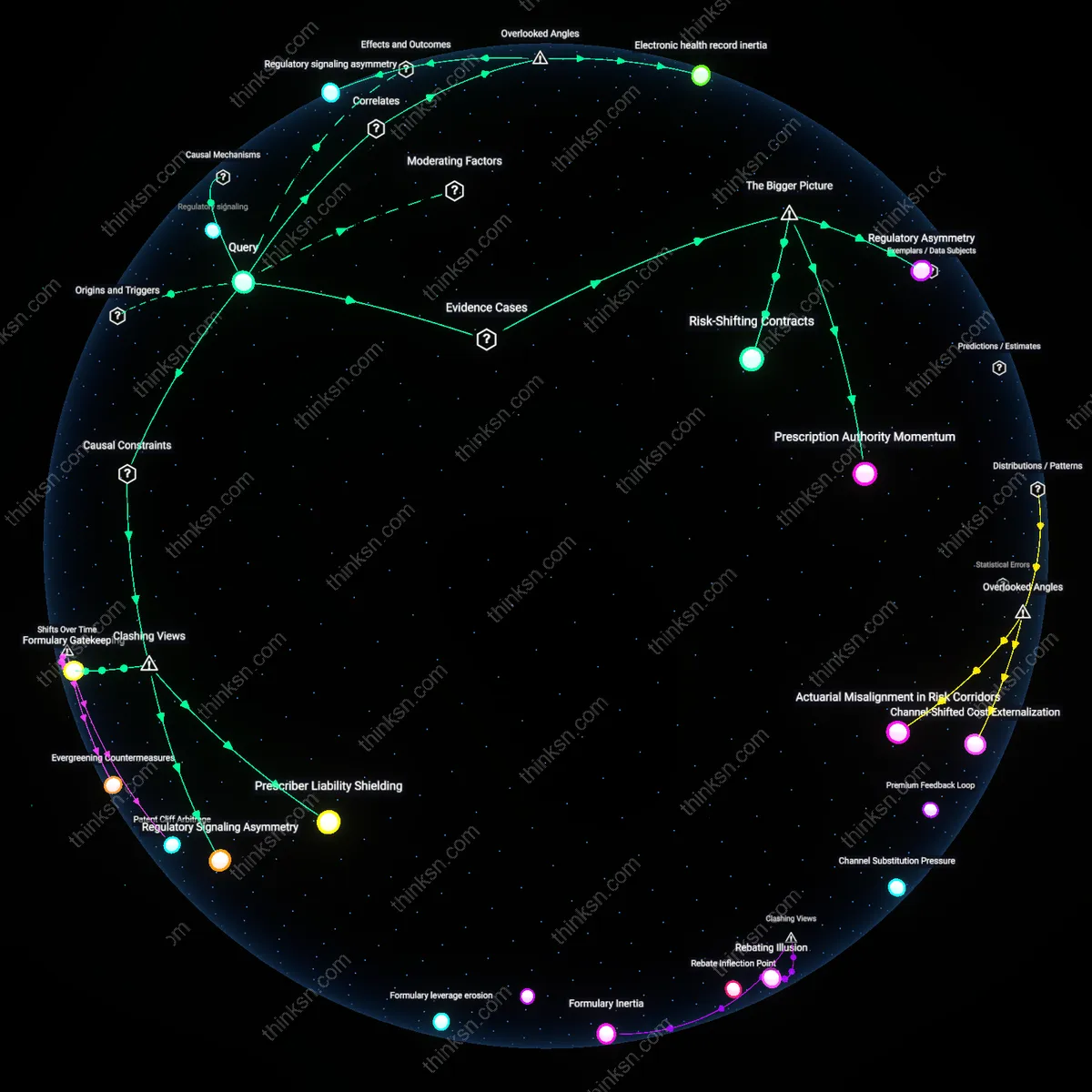
Regulatory signaling asymmetry
Brand-name drug manufacturers exert influence over insurance formulary requirements by submitting more comprehensive post-approval safety dossiers than generic producers, creating a perception of superior regulatory compliance even when clinical equivalence is established. This dynamic operates through the FDA’s passive surveillance systems, where volume and granularity of adverse event reporting become proxies for drug quality, despite no requirement for generics to match this reporting intensity. Insurers, lacking direct mechanisms to assess latent risk, default to these administrative signals, which are shaped more by marketing resources than pharmacological difference. The non-obvious element is that regulatory compliance becomes a performative metric, not a clinical one, altering formulary decisions without invoking cost or efficacy.
Electronic health record inertia
Prescribers using legacy electronic health record (EHR) systems maintain brand-name drugs in active medication lists due to default templates and auto-suggest functions that prioritize historical prescribing patterns, increasing the likelihood that insurance systems register brand-name requests even when generics are appropriate. These EHR pathways embed path dependency at the point of prescribing, where technical affordances—such as slower update cycles for drug nomenclature databases—systematically favor established brand entries over newer generic equivalents. Because insurance authorization is often triggered by the initial EHR-generated prescription code, the digital interface becomes a silent gatekeeper. This exposes how software architecture, not medical judgment or pricing, can propagate brand-centric insurance requirements.
Formulary Gatekeeping
Insurance plans mandate prior authorization for brand-name drugs not because of clinical superiority but because pharmacy benefit managers contractually bind formularies to restrict access unless administrative hurdles are met, revealing that therapeutic equivalence is overridden by contractual governance structures in which payer-controlled workflows act as bottlenecks—this challenges the intuitive view that medical necessity drives drug access, exposing how procedural friction rather than clinical evidence regulates treatment eligibility.
Prescriber Liability Shielding
Physicians disproportionately prescribe brand-name drugs when malpractice risk is perceived to be high, not due to patient demand or efficacy data, because in litigation-prone specialties like oncology or neurology, brand-name prescriptions serve as a defensible default that aligns with precedent-based care, thereby functioning as a causal bottleneck where medico-legal risk constraints override cost-efficiency logic—this inverts the dominant narrative that insurance utilization management drives prescribing, instead showing that clinical autonomy is channeled through liability avoidance systems that insurers must accommodate.
Regulatory Signaling Asymmetry
Brand-name drugs retain preferential insurance coverage because regulatory approval pathways grant them an enduring epistemic authority that generics cannot replicate, even when bioequivalence is demonstrated, since FDA labeling and risk evaluation mitigation strategies (REMS) are often not fully transferable, creating a causal bottleneck where safety governance systems privilege originator data infrastructure—this contradicts the assumption that regulatory equivalence ensures parity, uncovering a hidden hierarchy in evidentiary trust that insulates brands from competitive displacement.
Regulatory Asymmetry
Brand-name drug patents create a regulatory framework where only the innovator can legally market the specific molecular entity, forcing insurance plans to initially cover the branded version despite clinical equivalence to later generics. This occurs because the FDA’s approval pathway for generics requires demonstration of bioequivalence rather than new clinical trials, meaning the first-payer burden falls on insurers during the patent-protected period—commonly seen in cases like Humira, where AbbVie’s patent thicket delayed biosimilar uptake even after expiration. The non-obvious consequence is that insurance design becomes captive to intellectual property law, not clinical guidelines, shaping formulary decisions irrespective of cost. This reveals how legal structures external to medicine alter insurance requirements through timing and access constraints.
Prescription Authority Momentum
Physicians retain stronger prescribing habits and perceived liability protections when initiating treatment with brand-name drugs, especially in high-stakes conditions like oncology or autoimmune diseases, which pressures insurers to include them on formularies even when generics are available. At institutions like the Mayo Clinic or MD Anderson, oncologists often default to branded agents due to familiarity and trial-based experience, creating de facto insurance requirements through volume and clinical inertia. The underappreciated dynamic is that prescriber behavior, shaped by clinical evidence derived exclusively from brand-funded trials, becomes a structural force that insurers must accommodate, not just clinical equivalence. This dependence on physician-driven momentum entrenches brand inclusion regardless of pharmacological interchangeability.
Risk-Shifting Contracts
Pharmaceutical manufacturers of brand-name drugs increasingly use outcome-based or rebatable contracts with pharmacy benefit managers (PBMs) like Express Scripts or CVS Health, tying reimbursement to adherence or efficacy metrics, which incentivizes insurers to prioritize brand drugs despite generic availability. In the case of Novo Nordisk's Ozempic, insurers added the brand to preferred tiers due to contractual arrangements that shift financial risk onto the manufacturer if outcomes aren’t met—creating a backdoor form of value assurance not replicated in generic markets. The systemic implication is that insurance requirements are reshaped not by clinical differentiation but by financial engineering that bundles therapeutic performance with contractual liability, altering risk allocation in ways generics cannot easily replicate due to lack of post-market tracking infrastructure.