Why Stigma Hinders Medication-Assisted Recovery Despite Proven Success?
Analysis reveals 8 key thematic connections.
Key Findings
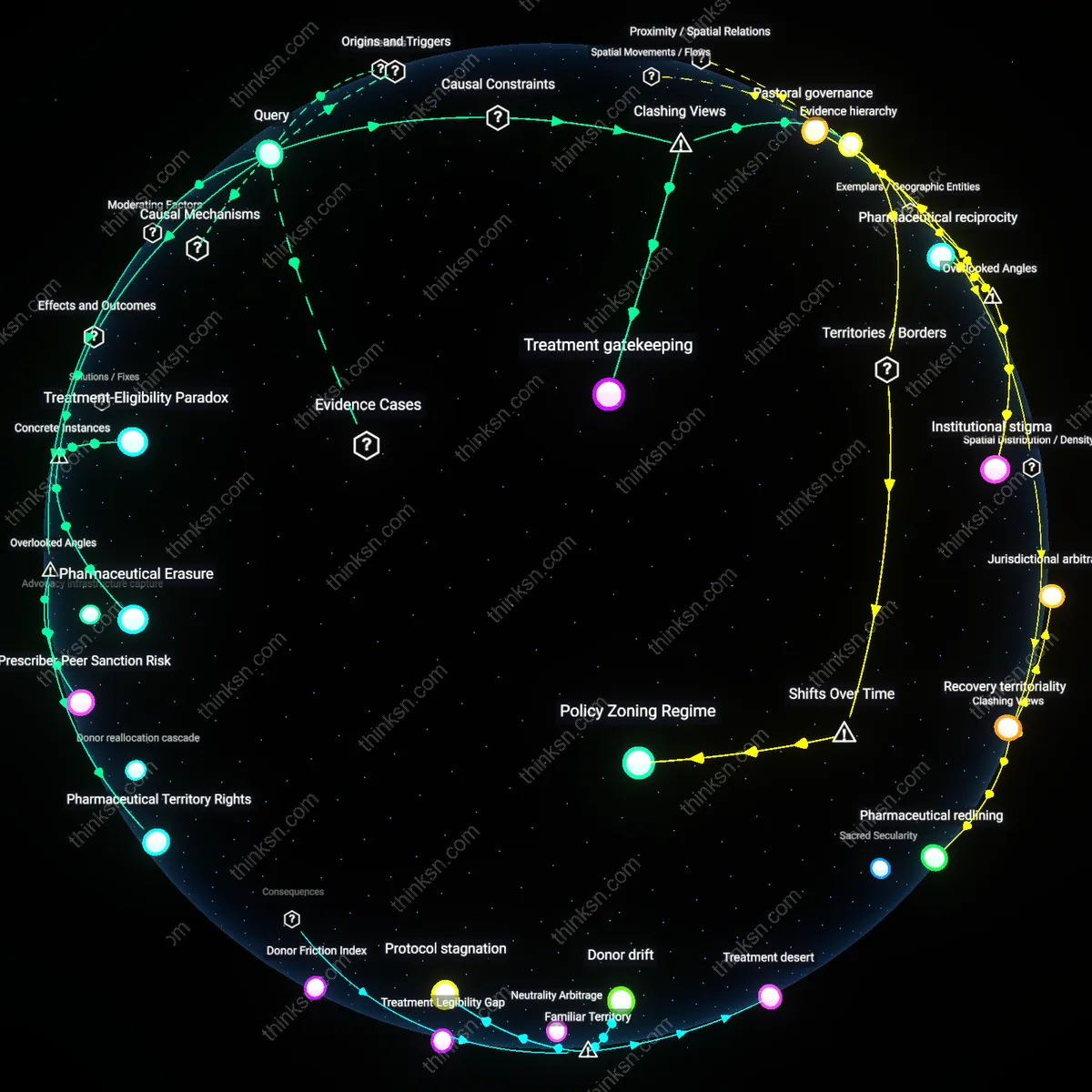
Treatment-Eligibility Paradox
In rural West Virginia, Medicaid expansion under the Affordable Care Act enabled reimbursement for buprenorphine prescriptions, yet primary care providers routinely withheld treatment from patients with active opioid use due to informal clinic policies equating continued use with noncompliance—despite federal guidelines permitting it, this local interpretation of medical adherence excluded eligible patients, revealing that access infrastructure can deepen therapeutic gatekeeping when stigma shapes clinical discretion.
Pharmaceutical Erasure
In the 1990s, France delayed approving buprenorphine for opioid use disorder despite robust trial data, partly because medical authorities associated opioid-based therapies with street drug culture—when Subutex finally entered the market, its prescription surged, reducing overdose deaths by 79% over five years, exposing how professional stigma against pharmacological similarity can suppress life-saving treatments even in evidence-accepting health systems.
Recovery-Identity Conflict
At Alcoholics Anonymous-affiliated recovery homes in Minnesota, residents on naltrexone for alcohol use disorder were historically expelled for using any mood-altering substance, branding medication as incompatible with sobriety—this norm persisted despite clinical endorsements, demonstrating how community-level definitions of authenticity can override medical authority and deter engagement with pharmacologically supported care.
Pharmaceutical Territory Rights
Exclusive distribution agreements between specialty pharmacies and pharmaceutical firms restrict access to medications like buprenorphine in rural regions, thereby intensifying stigma’s deterrent effect by conflating unavailability with clinical disapproval. These territorial exclusions—often dictated by third-party logistics providers rather than medical need—create geographic blind spots where patients interpret absence of supply as evidence of treatment illegitimacy, reinforcing cultural skepticism even when willingness to engage exists. This dynamic is overlooked because policy analyses typically treat medication access as a function of prescriber availability or insurance coverage, not as a consequence of proprietary supply-chain governance that silently shapes local standards of care.
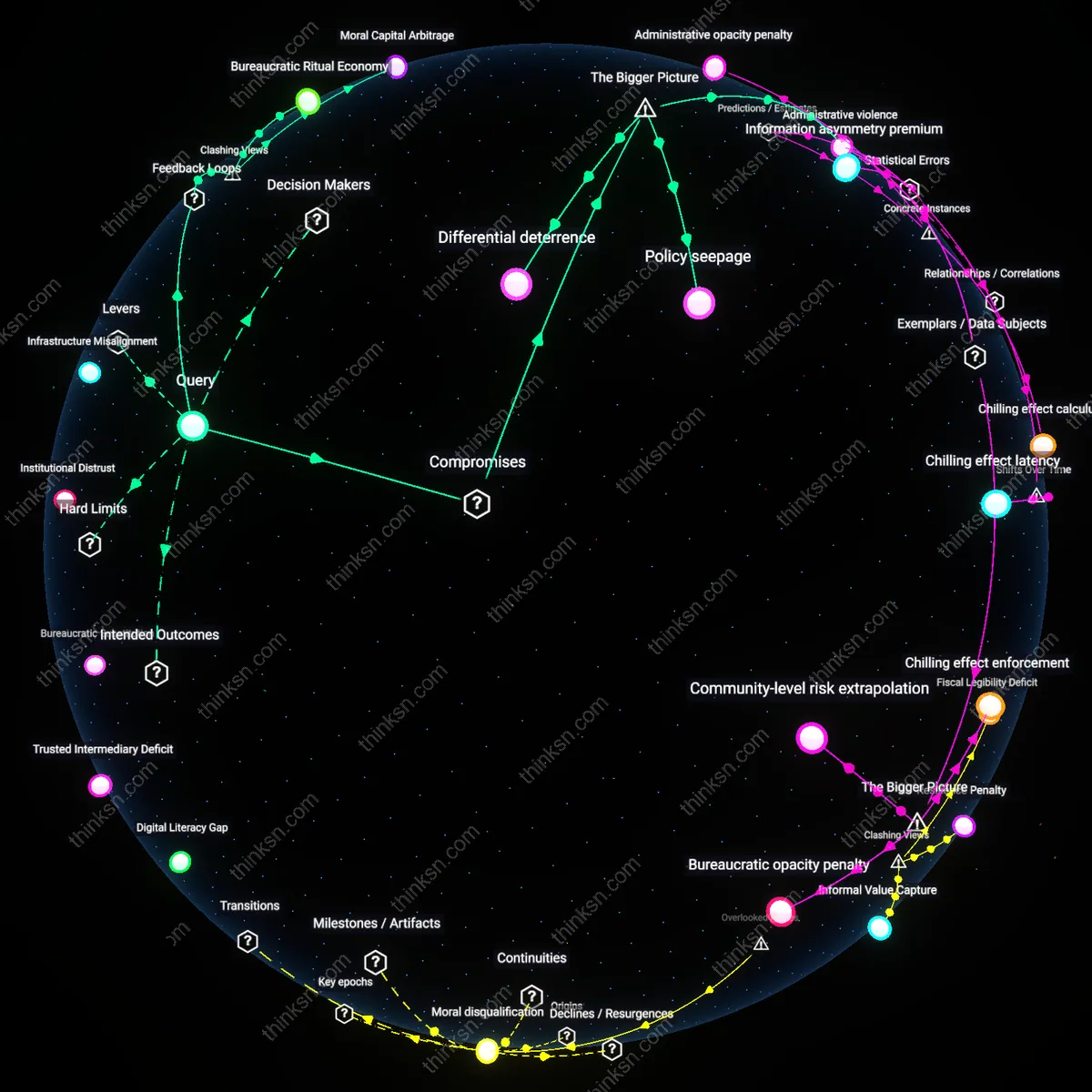
Recovery Infrastructure Franchise Models
Many abstinence-based recovery organizations operate as franchised social enterprises that derive funding and legitimacy from maintaining distinct identity boundaries, making integration of medication-assisted treatment a threat to institutional self-preservation. These programs—such as certain statewide 12-step affiliates receiving block grants—actively downplay or exclude MAT not solely due to ideology, but because program certification and donor support hinge on measurable ‘drug-free’ outcomes that MAT disrupts. This structural dependency on metric purity is rarely acknowledged in debates over stigma, which focus on individual attitudes rather than the institutional incentives that reward symbolic adherence to abstinence as a performance metric.
Prescriber Peer Sanction Risk
Primary care physicians in conservative medical communities avoid obtaining DATA 2000 waivers to prescribe buprenorphine not only due to workload concerns but because of informal professional censure from colleagues who associate addiction treatment with reputational contamination. In tight-knit regional health networks, especially in the Midwest and South, prescribers report social isolation, referral withholding, and exclusion from hospital privileges after initiating MAT services, creating a silent enforcement mechanism that amplifies stigma beyond public discourse. This peer-enforced normativity is underrecognized because regulatory assessments focus on formal barriers like training requirements, not on the social penalties embedded in local medical hierarchies.
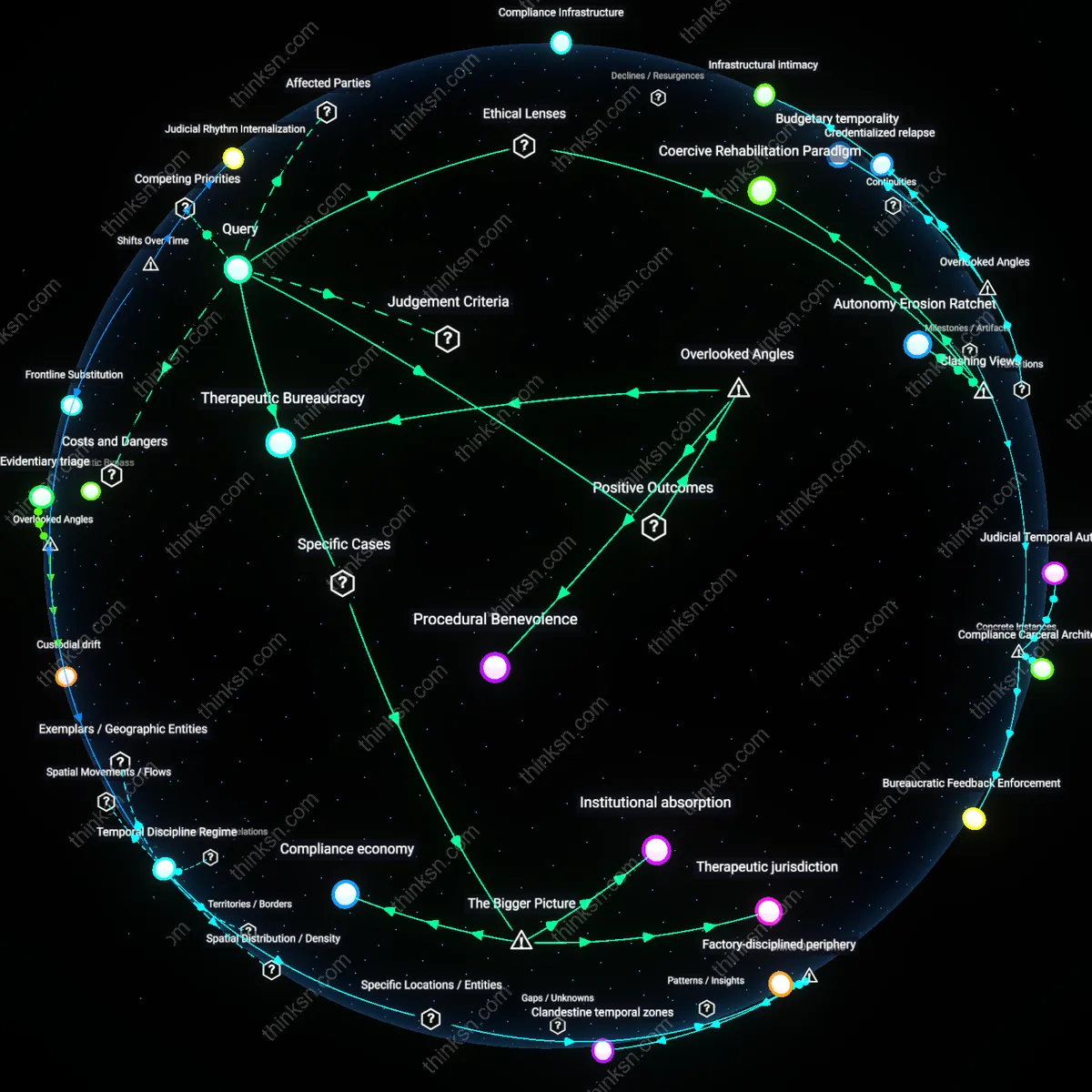
Treatment gatekeeping
Stigma against substance-use disorder treatment inhibits uptake of medication-assisted recovery because clinical gatekeepers—such as primary care physicians and addiction counselors—routinely withhold referrals to MAT programs unless patients first demonstrate abstinence or moral readiness, enforcing a prerequisite of 'proven willpower' before medical eligibility. This bottleneck operates through institutional risk-aversion and professional training that conflates pharmacological intervention with dependency perpetuation, particularly in rural clinics and state-funded rehab centers where abstinence ideology dominates. The non-obvious insight is that stigma does not merely shape public opinion but is institutionalized in procedural decisions by frontline providers who act as moral arbiters, not just medical ones—revealing how clinical access is contingent on character performance, not clinical need.
Evidence hierarchy
Medication-assisted recovery uptake remains low not because of patient resistance but because public health authorities and insurance payers treat abstinence-based outcomes as epistemically superior, requiring longer periods of drug-free urine screens for program graduation while discounting sustained recovery via MAT as 'substituted dependence.' This evidentiary bottleneck privileges a narrow, morally loaded definition of success—complete chemical abstinence—over functional stability, embedding a devaluation of pharmacological normalization in FDA risk-evaluation frameworks and Medicaid reimbursement rules. The dissonance lies in the fact that evidence of effectiveness is not the deciding factor; rather, what counts as valid evidence is pre-filtered by a cultural logic that equates purity with cure, exposing how scientific legitimacy is socially constrained.