Do Charitable Donations Enhance Equity or Perpetuate Hierarchy in Hospitals?
Analysis reveals 9 key thematic connections.
Key Findings
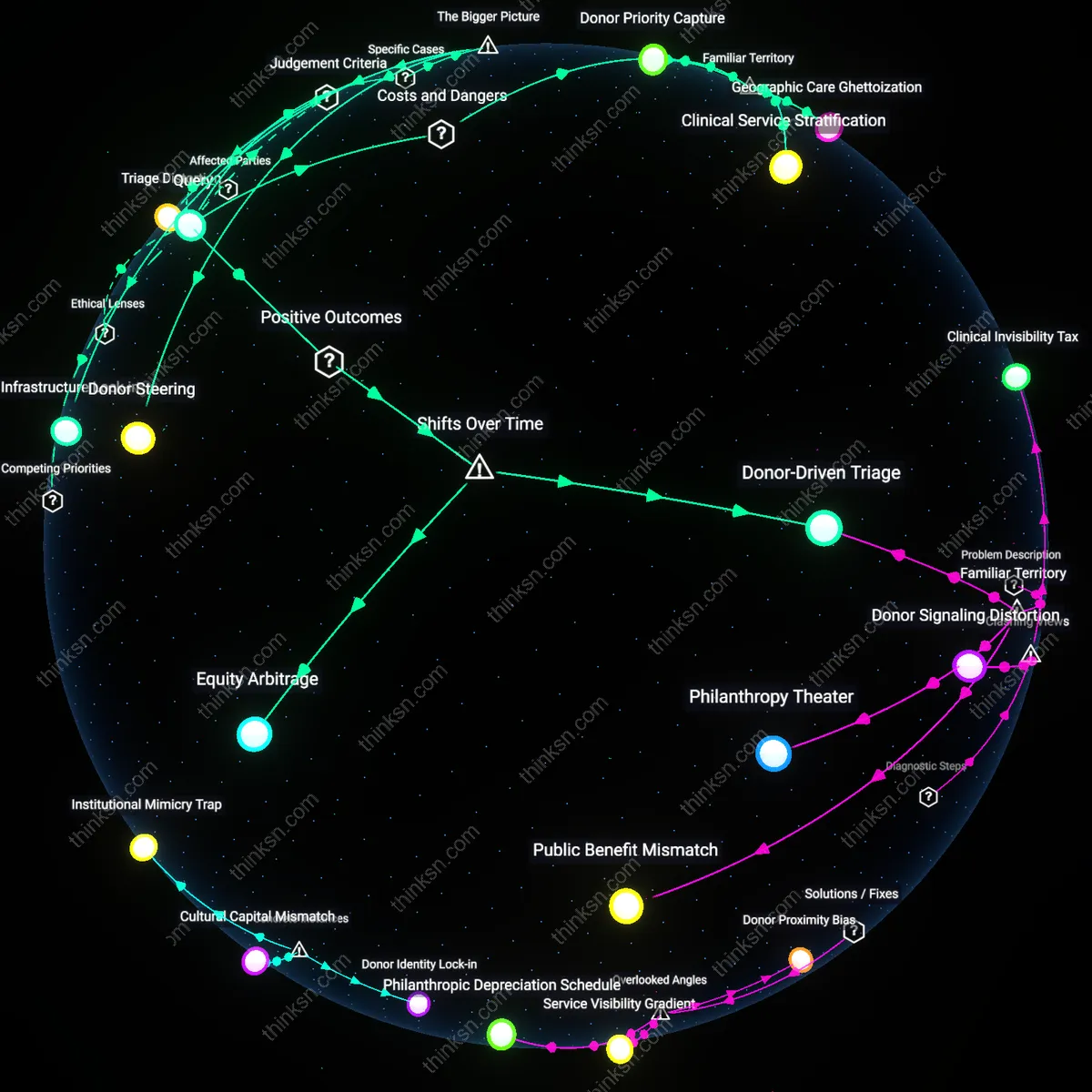
Donor-Driven Triage
Restricted charitable donations have improved care equity by redirecting private capital toward historically underfunded pediatric and maternal services in urban public hospitals during the 2010s, a shift enabled by the post-Affordable Care Act realignment of hospital accountability metrics, which incentivized philanthropic targeting of high-visibility care gaps to offset regulatory penalties—revealing that donor restrictions can function not as barriers but as correction mechanisms when aligned with policy transitions, a function previously obscured by assumptions that restricted giving always entrenches privilege.
Service-Line Stratification
Restricted donations have deepened service line disparities since the 1990s, as academic medical centers in the Northeast began monetizing naming rights for cardiac and oncology wings, channeling donor intent into already dominant specialties, thereby leveraging the tax-driven growth of mega-philanthropy to accelerate resource asymmetry—this commercialization of charitable intent marked a decisive break from mid-century models of general support funds, exposing how temporal shifts in nonprofit finance transformed altruism into a competitive differentiator among elite institutions.
Equity Arbitrage
The rise of corporate-designated giving to hospital emergency departments in underserved Sun Belt regions after 2020 reflects a strategic recalibration of restricted philanthropy into a risk-sharing instrument, where employers and insurers co-invest in acute care infrastructure to preempt public health collapse, bypassing traditional funding lags—this pivot from discretionary enhancement to systemic stabilization reveals a new temporality in health governance, where donor restrictions are no longer seen as constraints but as time-bound interventions to bridge institutional fragility during demographic transition.
Donor Priority Capture
Restricted charitable donations to hospitals deepen care inequity by aligning service expansion with donor interests rather than community health needs. Wealthy benefactors typically direct funds toward high-visibility departments like cardiac or oncology care in urban academic medical centers, reinforcing prestige-driven investment over primary or preventive services in marginalized neighborhoods. This distorts hospital resource allocation by institutionalizing donor preference as operational policy, creating de facto tiers of care access determined by philanthropy rather than epidemiological demand. Under the familiar assumption that 'more funding helps everyone,' the non-obvious risk is that unrestricted need-based financing is crowded out by donor-designated capital that serves institutional branding more than population health.
Geographic Care Ghettoization
Restricted donations concentrate specialized capabilities in already-resourced hospitals, widening the clinical desertification of rural and low-income urban zones. When charities fund discrete equipment or programs—such as robotic surgery units or neonatal ICUs—only at donor-preferred sites, they cement infrastructure asymmetries that patients cannot bypass due to transportation, insurance, or referral barriers. This dynamic turns geographic location into a de facto rationing mechanism, where proximity to a philanthropy-favored institution predicts access to advanced care. Though donors believe they are 'giving back,' the systemic cost is the normalization of spatially stratified medicine, where charitable intent accelerates rather than corrects the segregation of clinical excellence.
Clinical Service Stratification
Restricted funding entrenches hierarchies among hospital departments by privileging those that attract donor attention—such as cancer or heart programs—over stigmatized or less visibly dramatic fields like mental health, geriatrics, or addiction treatment. This creates internal inequities within hospitals where nursing staff, space, and administrative support are diverted to donor-visible units, weakening baseline care capacity. The mechanism operates through performance metrics tied to fundraising success, making departments compete for survival rather than coordinate around patient need. While the public sees charity as filling budget gaps, the underappreciated damage is that it reorganizes clinical priorities around spectacle and sentiment, not burden of disease or equity of outcomes.
Donor Steering
Restricted donations to specialized pediatric oncology units at institutions like St. Jude Children’s Research Hospital strengthen existing disparities by aligning private capital with already-preeminent service lines. This occurs because affluent donors often direct funds toward emotionally resonant, high-visibility programs rather than underfunded primary or preventive care, reinforcing institutional incentives to prioritize prestige over population health. The non-obvious dynamic is that donor intent—not clinical need—becomes the de facto allocator of capital within hospital ecosystems, privileging those departments capable of storytelling over those addressing structural inequities.
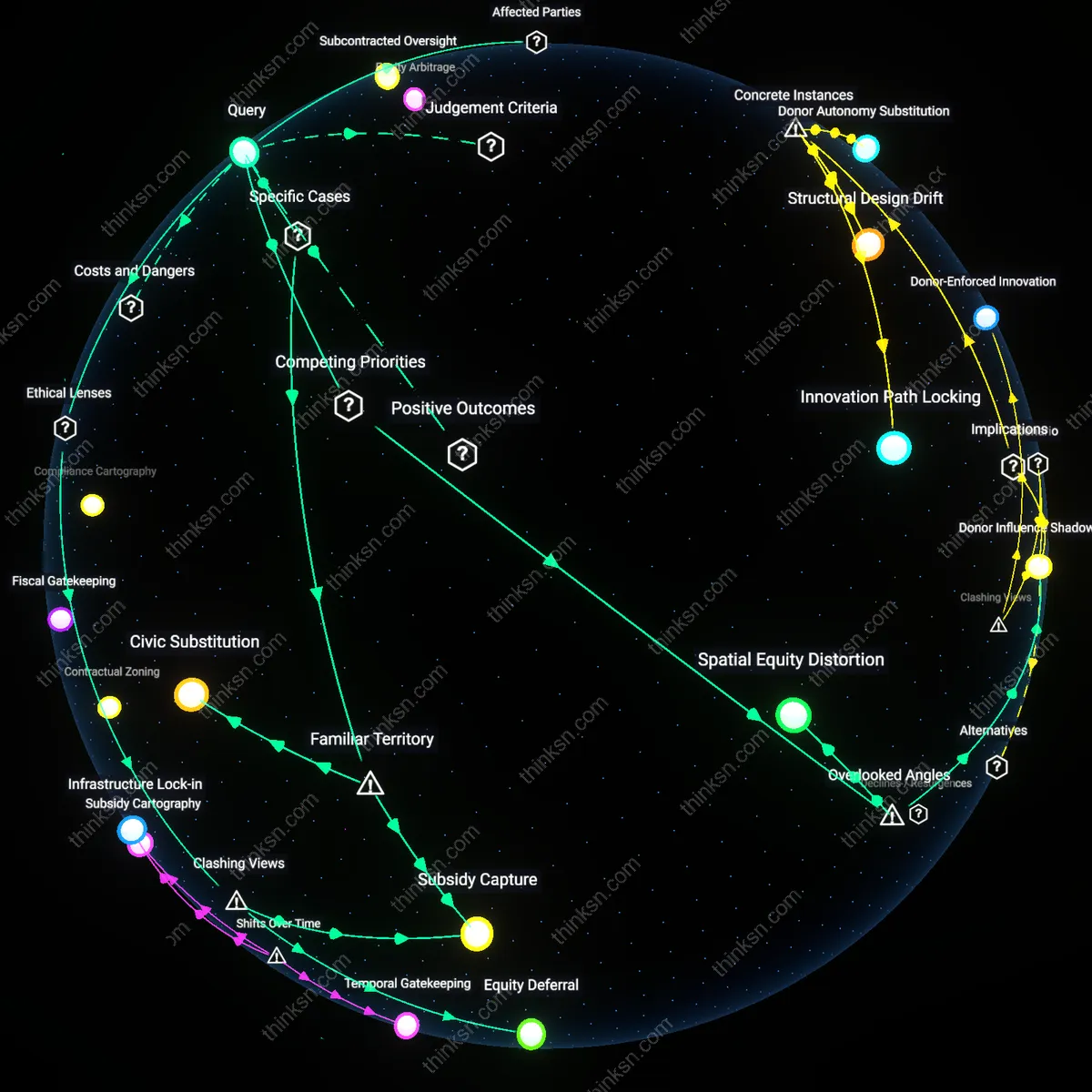
Infrastructure Lock-in
When the University of Pittsburgh Medical Center receives restricted gifts for transplant surgery expansion, it deepens resource asymmetry by binding public matching funds and workforce development to donor-specified domains. This happens because conditional private donations trigger institutional dependencies—facilities, staffing, and administrative pathways—that ossify around the endowed service, making reallocation politically and logistically difficult. The underappreciated consequence is that charity, even when well-intentioned, creates path dependency, where future care capacity is determined not by equity metrics but by historical gift restrictions.
Triage Distortion
At public safety-net hospitals like Cook County Health in Chicago, restricted philanthropy directed at specialty clinics reshapes triage logic by enabling auxiliary services that bypass systemic underfunding, creating a two-tier referral ecosystem. This emerges because restricted donations allow elite physician groups to offer expedited access to select treatments, distorting patient flow and eroding trust in universal care pathways. The overlooked mechanism is that targeted charity alters provider behavior and patient expectations alike, weakening the normative claim of equitable access in favor of performance stratified by donor-defined eligibility.