Standardized Chemo Protocols vs Patient Autonomy: A Complex Debate?
Analysis reveals 8 key thematic connections.
Key Findings
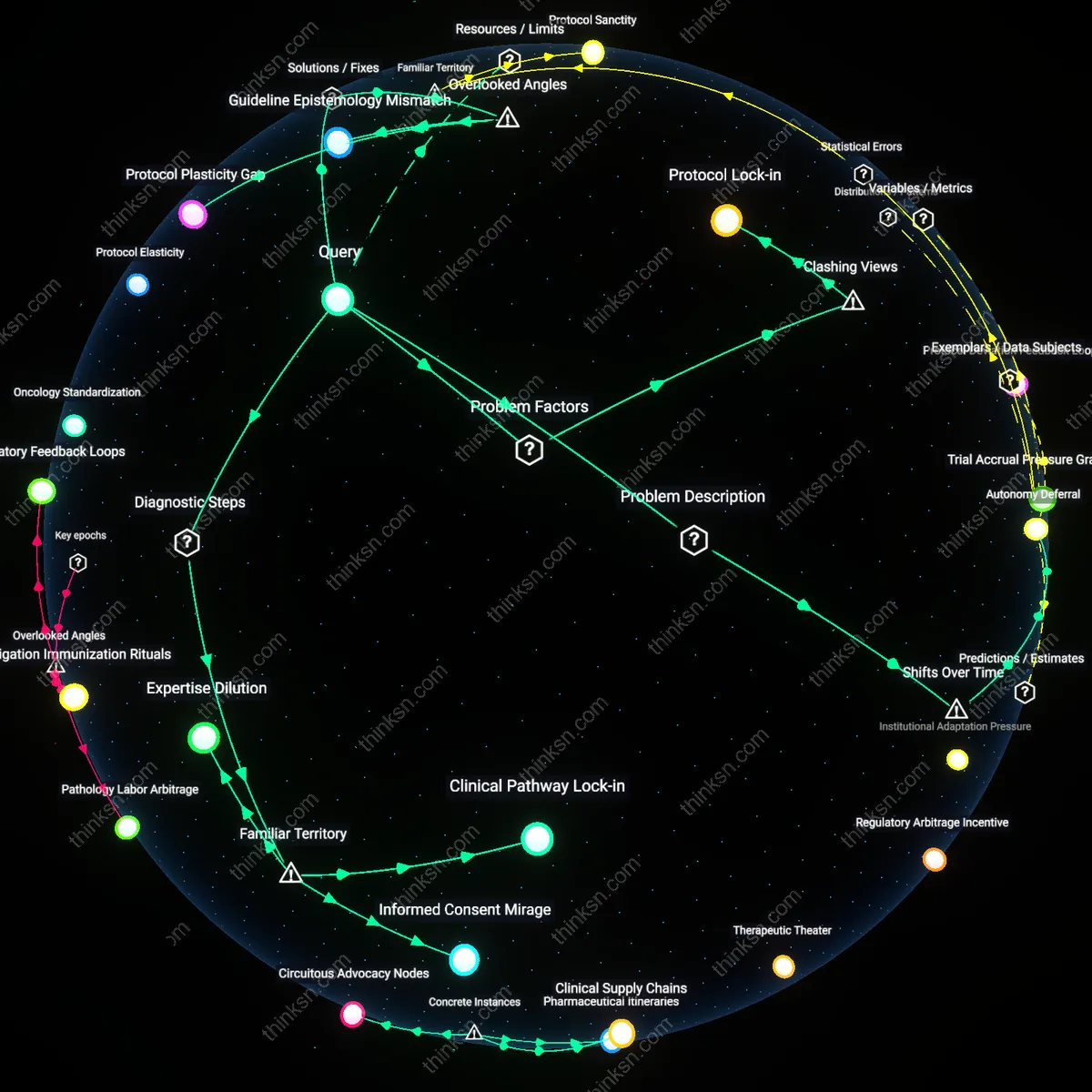
Autonomy Deferral
Patient autonomy is systematically deferred in standardized chemotherapy protocols not through overt denial but through a temporal displacement of decisional authority—once situated at the bedside, now centralized in prior authorization systems and institutional review boards that emerged robustly after the 2010 Affordable Care Act expansion. As insurance carriers and integrated delivery networks aligned protocols with cost-containment objectives, the moment of clinical choice receded from the point of care to pre-approval algorithms, making deviation functionally impossible even when medically warranted. This shift reframes noncompliance not as ethical dilemma but as operational breach, exposing how autonomy has been administratively rescheduled into irrelevance rather than outright revoked.
Protocol Lock-in
A standardized chemotherapy protocol undermines patient autonomy by binding clinicians to institutional pathways that prioritize system-wide efficiency over individualized care, as seen in integrated health networks like Kaiser Permanente where formulary restrictions and clinical decision support systems automatically deprioritize off-protocol regimens. This mechanism operates through administrative governance structures—such as pharmacy benefit managers and institutional review boards—that codify consensus guidelines into operational mandates, effectively removing negotiation space between patient and oncologist. The non-obvious aspect is that it is not physician paternalism or patient ignorance that erodes autonomy, but the quiet automation of care standards into backend systems that make deviation technically difficult and professionally risky.
Expertise Redistribution
Patient autonomy is compromised not because clinicians override preferences, but because standardization shifts medical authority from bedside providers to remote guideline panels—such as the National Comprehensive Cancer Network (NCCN)—whose classifications dictate what treatments are even available for discussion. These panels, though expert, embed values about risk, survival, and quality of life that are rarely transparent to patients, and their recommendations become law through payer reimbursement rules and electronic health record defaults. The dissonance lies in recognizing that autonomy is not just limited by paternalism but actively reshaped by the invisible layering of expert judgment into infrastructure, where treatment options are pre-filtered before they reach the clinical encounter.
Clinical Pathway Lock-in
A standardized chemotherapy protocol restricts oncologists from adjusting treatment based on individual patient biology, because institutional guidelines mandate uniform drug regimens regardless of molecular tumor profiles, genomic markers, or patient comorbidities. This operates through hospital accreditation requirements and insurance reimbursement structures that penalize deviation, making oncologists de facto administrators of policy rather than interpreters of clinical nuance. What’s underappreciated is that even when experts contest the protocol’s applicability—such as in aggressive subtypes or rare cancers—the system enforces compliance, rendering patient-specific judgment clinically permissible in theory but institutionally unviable in practice.
Informed Consent Mirage
Patients believe they are making autonomous choices about chemotherapy because they sign consent forms and hear phrases like 'shared decision-making,' but the menu of options presented is pre-filtered by system-mandated protocols that exclude equally valid but non-standard regimens. This occurs within oncology clinics where time pressures and institutional norms lead physicians to present only guideline-endorsed treatments, framing them as medically necessary rather than context-dependent. The non-obvious reality is that consent becomes performative—ritualizing patient involvement while the actual decision space is contractually bounded by third-party payers and clinical governance boards.
Expertise Dilution
When a health system enforces a single chemotherapy protocol across diverse cancer centers, it supplants local oncological expertise with centralized algorithmic rules, privileging statistical averages over clinician experience in managing outliers. This dynamic plays out in regional hospitals where tumor boards may advocate for off-protocol therapies based on emerging research or patient history, but are overruled by administrative directives tied to national quality metrics. The overlooked consequence is that expert disagreement—once a signal for clinical deliberation—is reclassified as non-compliance, systematically eroding the role of professional judgment in tailoring care.
Protocol Plasticity Gap
Introduce adaptive feedback loops into chemotherapy protocol design that require oncology teams to document and justify deviations in real time using structured clinical rationale forms. This creates a dynamic revision mechanism where institutional guidelines evolve based on frontline clinical judgment, thereby embedding practitioner discretion into the formal protocol. The non-obvious insight is that standardization undermines autonomy not through rigidity alone but via the absence of documented, systematic exceptions—making invisible the accumulated dissent of clinicians whose on-the-ground assessments are overruled; this gap between formal rigidity and informal practice erodes trust in both the protocol and patient consent processes.
Guideline Epistemology Mismatch
Establish independent 'contradiction panels' composed of ethicists, patient advocates, and dissenting oncologists to publish counter-guidelines alongside official protocols, explicitly cataloging where expert disagreement persists and how it affects treatment options. The overlooked dynamic is that standardized protocols are treated as settled science even when the underlying evidence base is fractious—this mismatch between the epistemological uncertainty of the field and the certainty implied by institutional protocol creates a legitimacy gap that quietly invalidates patient choice, because patients cannot autonomously weigh options they are not told are contested.