Should I Switch to a Biosimilar? Financial and Therapeutic Risks Explained
Analysis reveals 7 key thematic connections.
Key Findings
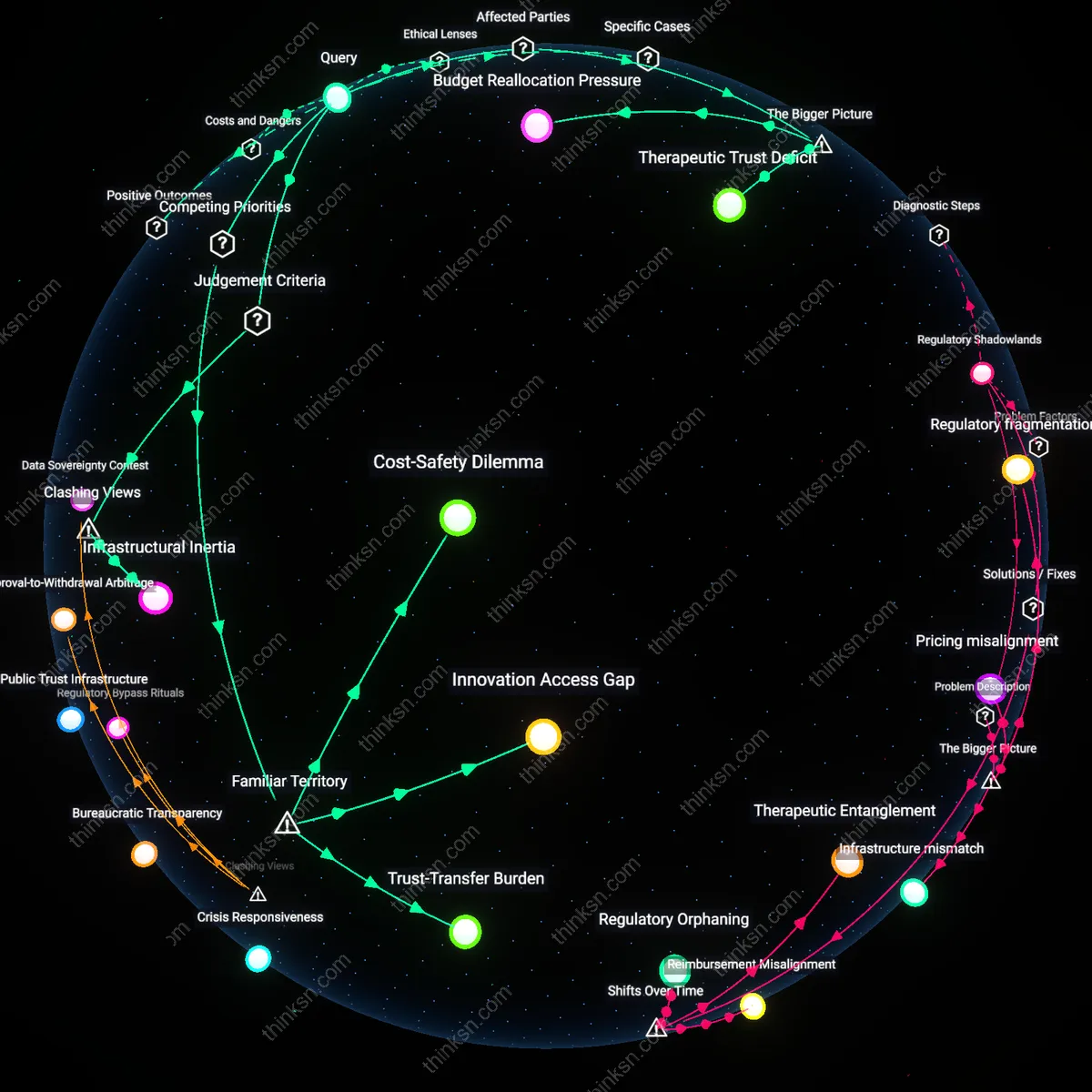
Budget Reallocation Pressure
Payers shifting patients to biosimilars to reduce short-term drug expenditures inadvertently intensify downstream cost burdens on outpatient rheumatology clinics that must absorb unforeseen monitoring and retreatment costs due to variable interchangeability outcomes. Health systems like U.S. Medicare Advantage plans or NHS England face structural incentives to adopt biosimilars early, yet lack risk-adjusted funding mechanisms to manage adverse events from imperfect substitution—triggering cost displacement rather than savings. This dynamic reveals how fiscal optimization at the payer level destabilizes cost predictability at the provider level, a transfer effect rarely accounted for in formulary decision models.
Therapeutic Trust Deficit
Rheumatologists in community practice restrict biosimilar adoption not due to clinical skepticism but because liability exposure and patient attrition risks outweigh institutional incentives when long-term equivalence data are absent—forcing clinicians to mediate systemic evidence gaps through personalized risk aversion. Unlike academic medical centers with trial infrastructure, independent clinics lack resources to generate real-world effectiveness data, leaving them dependent on fragmented post-marketing surveillance that delays confidence-building. This creates a de facto two-tier system where therapeutic trust becomes geographically and institutionally stratified, undermining equitable access to cost-reduced care.
Evidence Generation Asymmetry
Regulatory reliance on extrapolated indications enables biosimilar market entry without condition-specific trial data, privileging biopharmaceutical manufacturers’ speed-to-market strategies over rheumatologists’ need for granular clinical comparability in complex autoimmune presentations. This asymmetry emerges because EMA and FDA approval pathways accept pharmacokinetic similarity and immunogenicity assessments as sufficient proxies across rheumatic diseases, even though conditions like psoriatic arthritis and lupus exhibit divergent biomarker responses not captured in rheumatoid arthritis trials—the dominant data source. As a result, the burden of evidentiary generation shifts from pre-approval regulators and sponsors to post-approval clinicians, who then operate in a state of managed uncertainty.
Infrastructural Inertia
Switching to biosimilars under cost-pressure health systems prioritizes budgetary efficiency over therapeutic individualization, privileging institutional financial resilience at the expense of clinician autonomy in complex rheumatic cases. This occurs because purchasing decisions shift from rheumatologists to centralized procurement bodies—such as NHS England or U.S. group purchasing organizations—that standardize formularies based on population-level savings, not patient-level response variability, thereby embedding fiscal logic into clinical pathways. The non-obvious reality is that the absence of comparative clinical data is not a barrier to adoption but a structural enabler, allowing health systems to rationalize substitution by deeming biosimilars interchangeable in policy despite unresolved immunogenicity risks in subpopulations.
Cost-Safety Dilemma
Adopting biosimilars in rheumatology prioritizes immediate financial relief for health systems over long-term therapeutic confidence, because payers and providers substitute originator biologics with lower-priced alternatives to reduce budget burdens, particularly in publicly funded systems like the NHS or Medicaid. This trade-off functions through reimbursement mandates and formulary restrictions that make biosimilars the default despite individualized uncertainty in outcomes, privileging systemic affordability at the expense of clinical predictability for complex patients. The non-obvious reality is that the familiar narrative of biosimilar equivalence—driven by FDA/EMA interchangeability labels—masks real-world variation in immunogenicity and durability of response, especially among patients previously stabilized on originator drugs.
Innovation Access Gap
Shifting to biosimilars expands patient access to biologic-level therapy in under-resourced settings by lowering entry barriers, as seen in hospital networks across Eastern Europe or rural U.S. clinics where originator drug costs previously excluded most rheumatology patients. This works through procurement-scale savings that free up capital for treating more individuals, yet simultaneously diverts pharmaceutical investment and prescriber attention away from emerging, potentially superior therapies that lack biosimilar counterparts. Crucially, this reveals that the popular perception of biosimilars as unequivocal progress for patient access obscures how cost-driven adoption can freeze therapeutic advancement at the level of yesterday’s molecules, privileging broad coverage over cutting-edge efficacy.
Trust-Transfer Burden
Switching to biosimilars transfers the psychological and clinical burden of uncertainty from regulators to clinicians and patients, because agencies like the EMA approve biosimilars based on analytical similarity and limited clinical bridging studies, leaving rheumatologists to manage real-world outcomes with incomplete comparative data. This dynamic operates through shared decision-making encounters where physicians must weigh payer incentives against patient anxiety about changing stable regimens, particularly for those with hard-won disease control. The underappreciated insight is that the public’s familiar association of biosimilars with ‘same but cheaper’ ignores how trust in therapeutic equivalence is not inherited from the originator but actively constructed—and often frayed—in the consultation room.