Single-Payer Savings vs Pharma Innovation Loss?
Analysis reveals 9 key thematic connections.
Key Findings
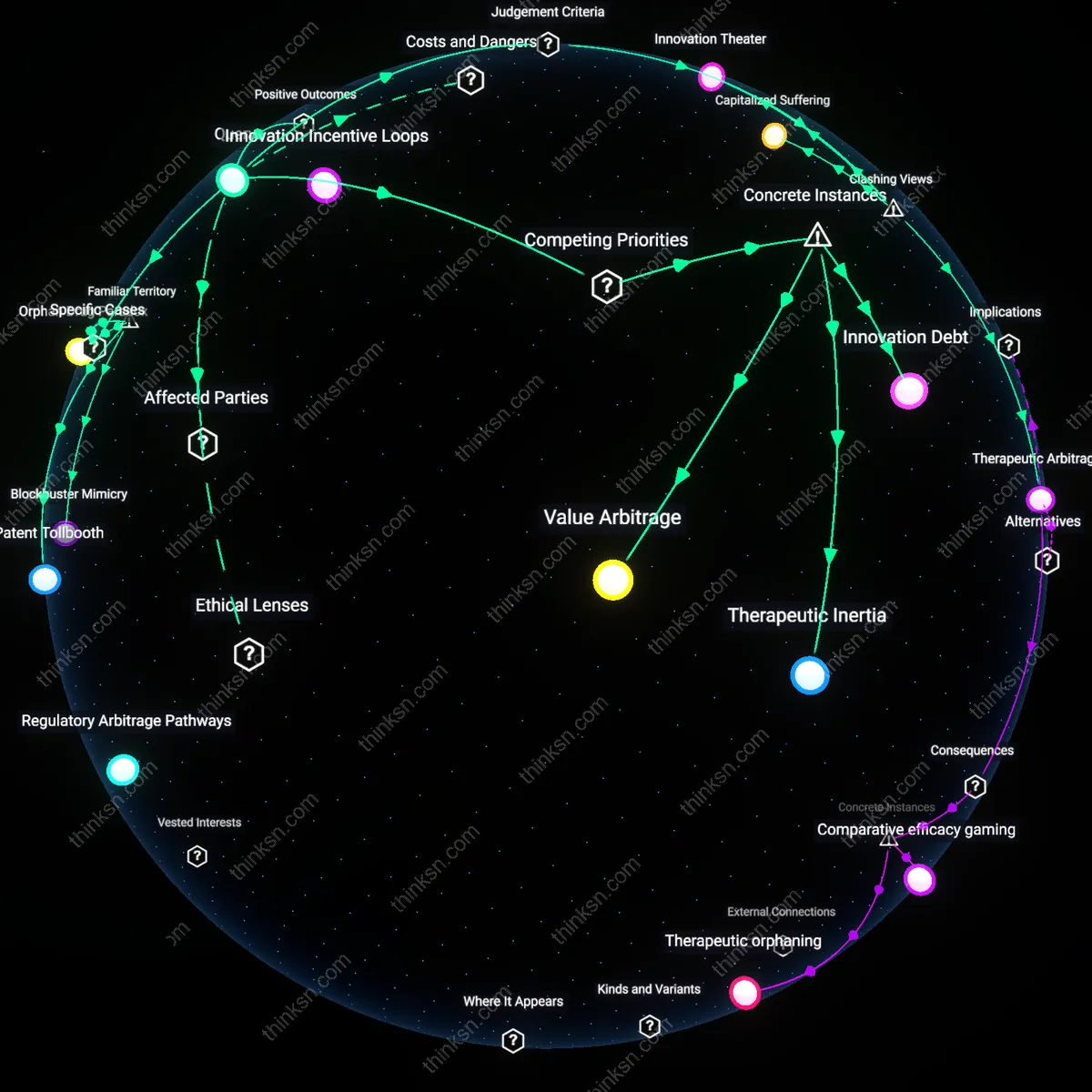
Innovation Incentive Erosion
A policy analyst should prioritize protecting long-term pharmaceutical innovation by recognizing that flatlined R&D investment in high-risk therapeutic areas follows directly from diminished patent revenue under single-payer pricing regimes. Public payers like Canada’s Patented Medicine Prices Review Board constrain drug prices below global benchmarks, reducing marginal returns for biotech firms—particularly small and mid-sized enterprises dependent on blockbuster success—thereby cooling venture capital appetite for early-stage research. This mechanism reveals how fiscal efficiency in healthcare delivery can inadvertently suppress the distributed network of private actors whose risk-taking drives breakthrough therapies, a systemic feedback often obscured by macro-level cost-benefit models.
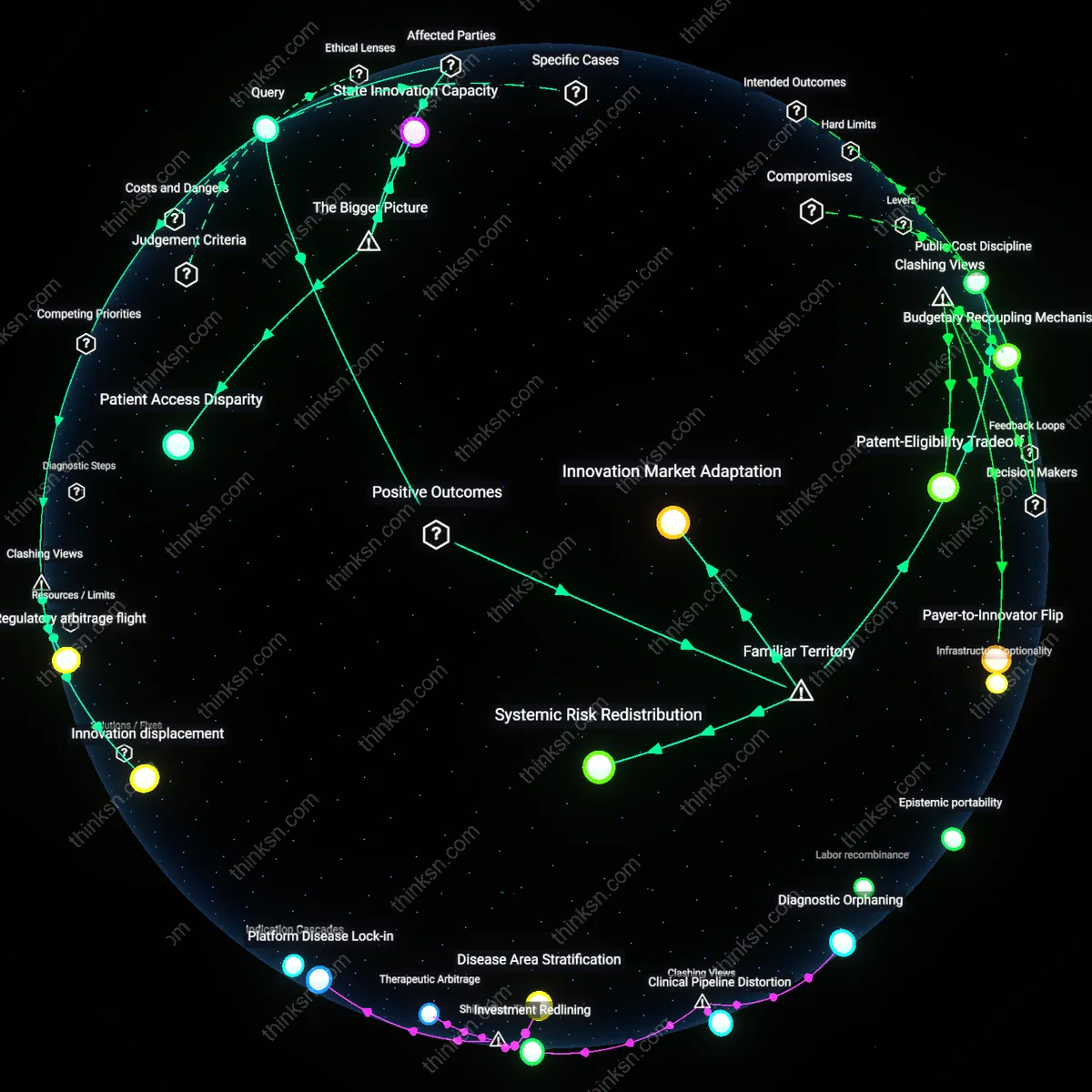
Patient Access Disparity
A policy analyst must weigh administrative savings against unequal patient access to novel treatments, as centralized reimbursement decisions in single-payer systems tend to delay or deny coverage for high-cost, high-efficacy drugs based on narrow cost-effectiveness thresholds. Institutions like the UK’s National Institute for Health and Care Excellence (NICE) routinely reject gene therapies and targeted oncology drugs due to high per-patient costs, disproportionately affecting rural and socioeconomically marginalized patients who lack alternative insurance pathways. This dynamic exposes how systemic cost control can crystallize into spatially and socially uneven health outcomes, shifting the innovation burden onto patients while privileging system-level efficiency.
State Innovation Capacity
A policy analyst should recalibrate the trade-off by leveraging the state’s enhanced bargaining power under single-payer to directly fund priority-driven biomedical research, transforming cost savings into public-sector innovation infrastructure. By redirecting a fraction of administrative savings—such as those achieved by Medicare for All proposals in the U.S.—into entities like the NIH or ARPA-H, the state can crowd in high-impact research on neglected diseases and platform technologies that private firms underinvest in due to uncertain returns. This shift reframes the state not as an innovation suppressor but as a strategic investor, activating a latent public capacity to shape the knowledge economy beyond market signals.
Public Cost Discipline
Adopting a single-payer system strengthens national leverage to reduce administrative overhead, directly freeing up capital for reinvestment in patient care. By consolidating billing, eligibility, and claims processing under one public insurer—like Canada’s provincial systems—redundant private insurance infrastructure is eliminated, saving an estimated 10–15% of total healthcare spending. The underappreciated point is that these savings are not just fiscal efficiency wins but create a stable, predictable funding pool that can be strategically redirected to subsidize access to medicines, partially offsetting innovation concerns without relying on fragmented market incentives.
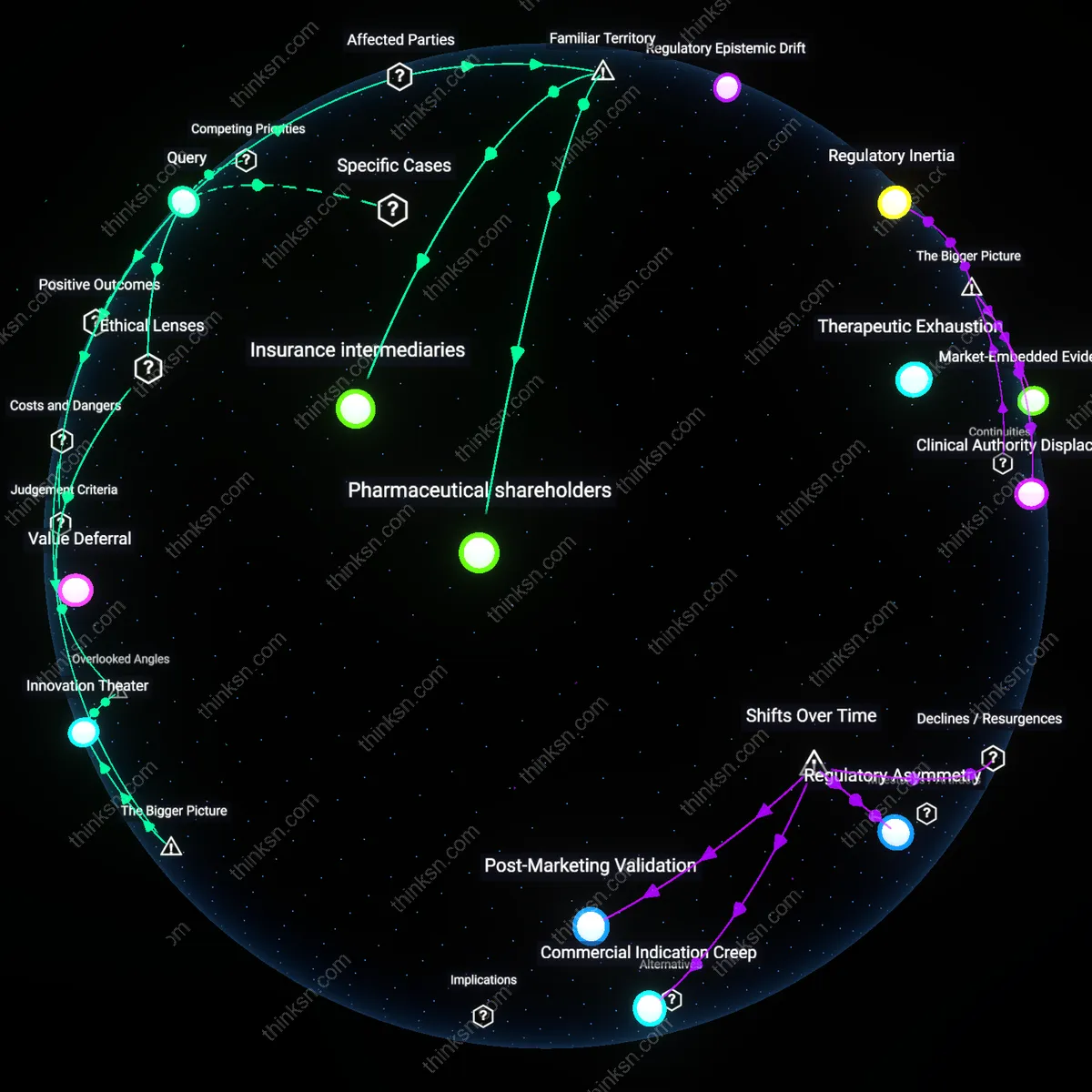
Innovation Market Adaptation
Pharmaceutical firms adjust R&D investment in response to demand signals, not just profit margins, meaning a single-payer can shape innovation direction by setting public health priorities in reimbursement contracts. When entities like the UK’s NHS negotiate drug prices and coverage based on clinical value, companies shift development toward high-impact therapies—such as antibiotics or rare disease drugs—that align with public health needs rather than blockbuster profitability. The overlooked insight is that market competition isn’t the only driver of innovation; coordinated public demand creates a different but equally powerful innovation signal, one more aligned with population health outcomes.
Systemic Risk Redistribution
Shifting to single-payer transfers financial risk from households and employers to the state, stabilizing demand and enabling long-term health planning across the economy. In the U.S., where employer-based insurance ties coverage to employment, economic downturns disrupt both care access and pharmaceutical markets; a public system like Sweden’s decouples this, ensuring consistent medication uptake and predictable drug utilization. What’s rarely acknowledged in the innovation debate is that stable, universal coverage reduces demand volatility—which investors and drug developers value—thus maintaining a reliable innovation ecosystem despite lower per-unit profits.
Innovation displacement
A policy analyst should prioritize single-payer adoption because the administrative savings enable state-directed R&D funding, which can redirect pharmaceutical innovation toward unmet clinical needs rather than marketable indications, shifting innovation from shareholder-driven pipelines to public health-driven ones. This mechanism operates through budget reallocation from insurance overhead to public biomedical grants, particularly within institutions like the NIH or ARPA-H, disrupting the assumption that profit motives are the sole engine of breakthrough discovery. The non-obvious insight is that competition does not disappear under single-payer but is rechanneled through scientific and institutional rivalry, undermining the dominant narrative that market exit equates to innovation loss.
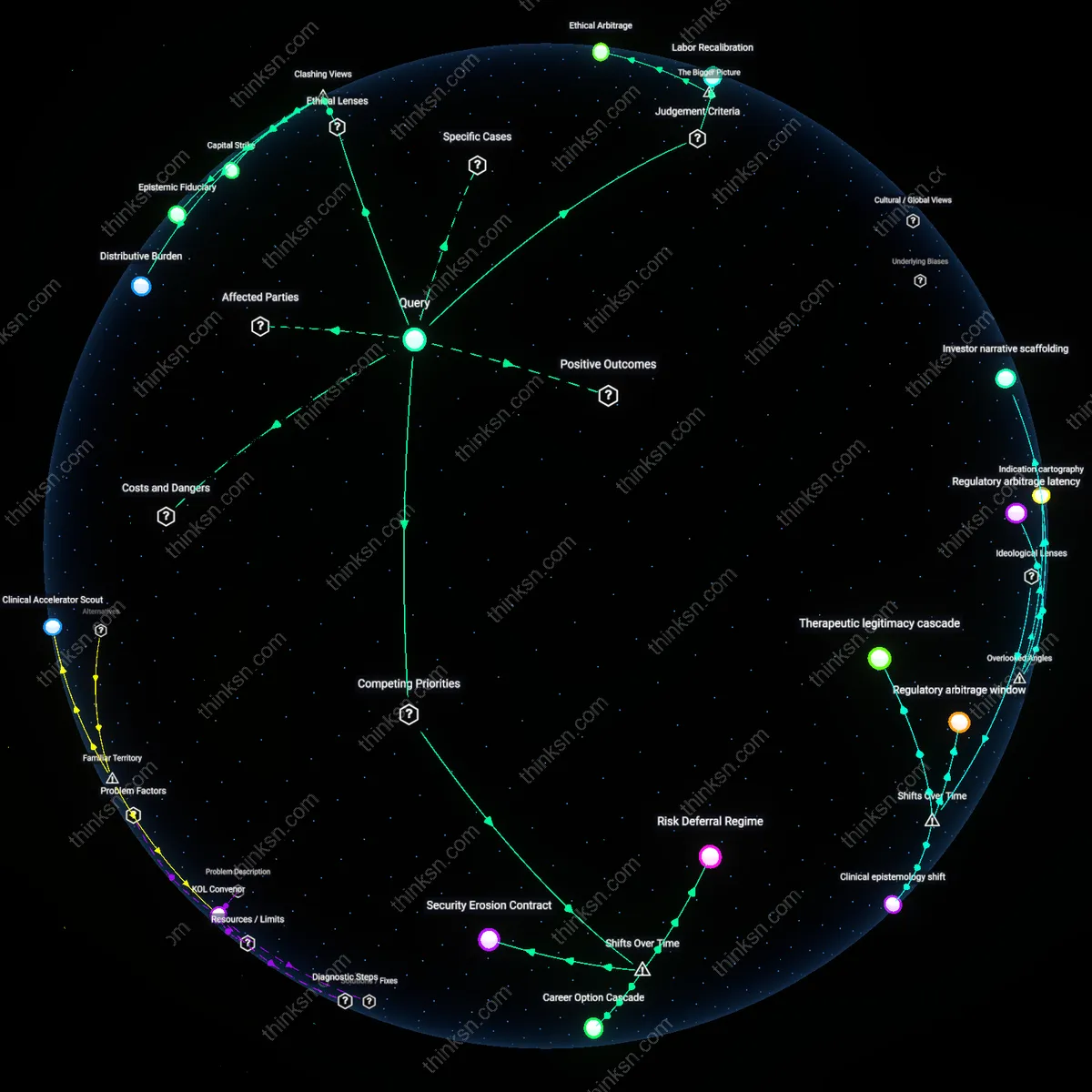
Regulatory arbitrage flight
A policy analyst must treat national single-payer systems as accelerants of pharmaceutical offshoring, where drug developers bypass domestic price constraints by orienting clinical trials, patenting, and revenue capture to more profitable jurisdictions such as the U.S. private market or emerging Asia, weakening the expected trade-off between cost control and innovation. This dynamic functions through global capital mobility and differential pricing regimes, allowing firms to absorb lower domestic returns if offset by international gains, especially in fragmented markets resistant to bulk negotiation. The underappreciated reality is that innovation is not uniformly suppressed by single-payer but instead becomes geographically selective, revealing innovation’s dependence on spatial loopholes rather than competition per se.
Administrative resistance capital
A policy analyst should recognize that projected administrative savings from single-payer are systematically overstated because entrenched insurance and hospital billing infrastructures actively convert cost-cutting mandates into new compliance bureaucracies, preserving employment and influence under the guise of transition management. This process unfolds through lobbying by medical coding associations, EHR vendors, and regional Medicare administrators who reframe efficiency as complexity, embedding themselves in implementation frameworks like HIPAA-compliant data exchanges or prior authorization digitization. The dissonant finding is that administrative overhead is not a flaw to be eliminated but a latent power structure that reorganizes rather than retreats, exposing the myth of frictionless state simplification.