Institutional Path Dependency
The Veterans Health Administration adopted watchful waiting for small lung nodules because its existing infrastructure for managing chronic diseases among aging veterans enabled longitudinal CT surveillance, as seen in the 2011 rollout of the Lung Nodule Algorithm at the VA Puget Sound Health Care System, where pre-existing patient tracking protocols from diabetes and hypertension programs were repurposed to monitor nodules instead of defaulting to surgery. This continuity in managing slow-progressing conditions through routine follow-up—rather than acute interventions—reveals that established care workflows, not new evidence alone, determined clinical adaptation. What is underappreciated is that the VA's shift did not stem from surgical risk aversion but from the functional alignment of nodule monitoring with its entrenched model of preventive, visit-based chronic care.
Risk Standardization Routine
The integration of the Fleischner Society guidelines into VA Medical Center protocols starting in 2013 at the Miami VA Healthcare System transformed observational management of lung nodules into a codified, rule-based alternative to surgery by assigning follow-up intervals based on nodule size and patient risk factors. This mechanism replaced clinician discretion with a standardized algorithm, reducing institutional liability and aligning decentralized VA sites under a unified decision framework. The underappreciated reality is that clinical acceptance hinged not on radiological consensus alone, but on the VA’s need for administratively defensible, uniformly applicable rules that could scale across its national network.
Data Feedback Infrastructure
At the VA Palo Alto Health Care System between 2015 and 2018, the development of the NoduleCare electronic dashboard—which aggregated radiology reports, flagged overdue follow-ups, and generated automatic alerts—made longitudinal observation feasible by turning passive waiting into an actively managed process, thereby displacing surgery as the default action for small nodules. This system leveraged the VA’s pre-existing national electronic health record to create a feedback loop where data visibility created clinical accountability. The overlooked insight is that watchful waiting became acceptable only when it was no longer ‘waiting’ at all, but a technologically surveilled workflow resembling disease registry management.
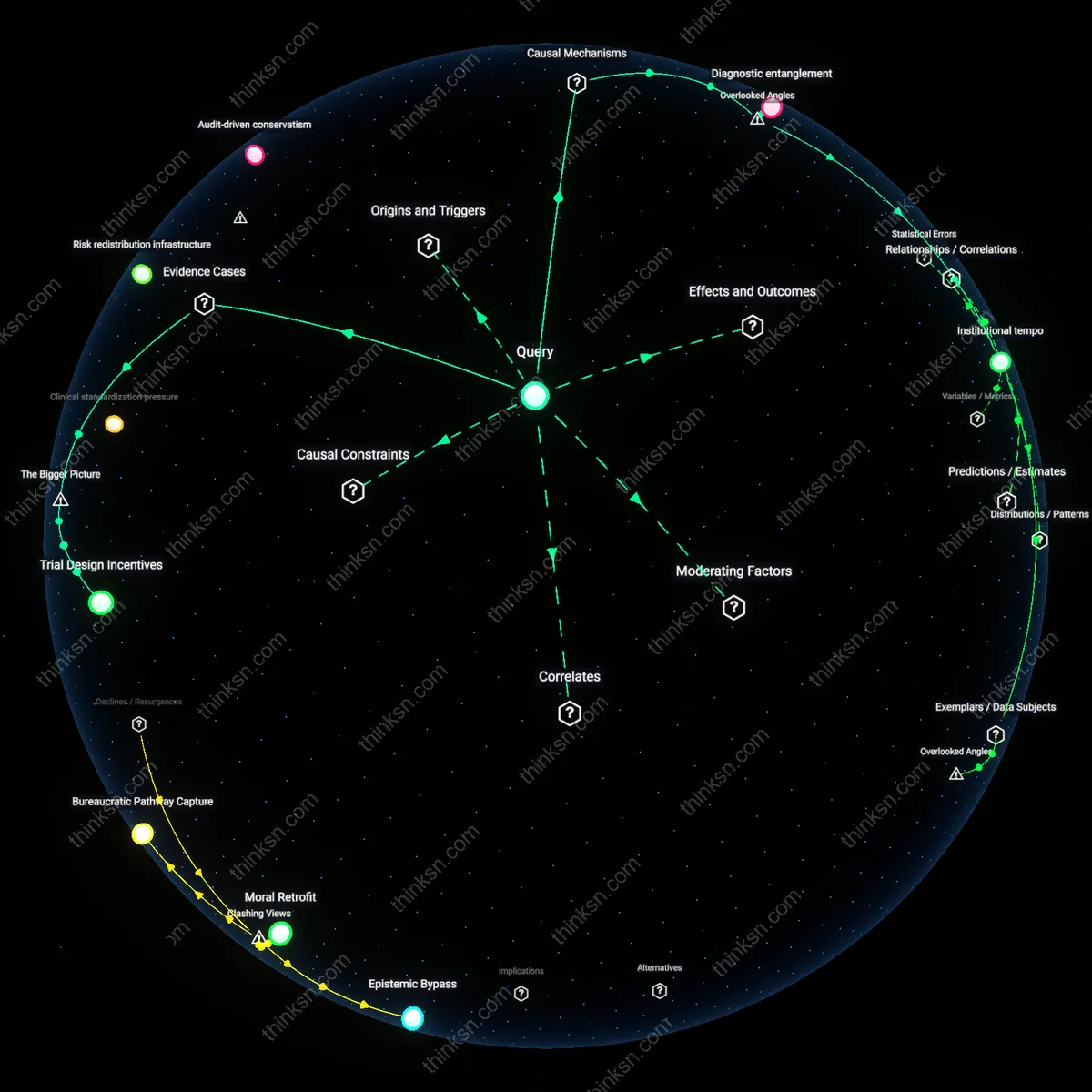
Bureaucratic Pathway Capture
The adoption of watchful waiting for small lung nodules in VA centers succeeded not because of clinical breakthroughs but because administrative systems redefined procedural efficiency as clinical prudence, embedding surveillance protocols into care pathways that privileged system sustainability over intervention. Quality metrics, electronic medical record templates, and tumor board referral criteria were reshaped by VA central offices to constrain surgical referrals, effectively institutionalizing observation as the default—especially for older veterans—by routing decisions through standardized algorithms that masked rationing as best practice. This reframes the 'acceptance' of non-intervention as a quiet reallocation of medical authority from surgeons to administrators operating under resource-constrained mandates, undermining the intuitive narrative of medical consensus driven by improved diagnostics. The non-obvious reality is that this approach spread not via clinician autonomy but through centralized care engineering that turned iteration delays into clinical doctrine.
Epistemic Bypass
Watchful waiting became standard in VA settings not because surgeons were convinced by oncological evidence but because radiologists, through repeated incident reporting and nodal classification systems, redefined ambiguous findings as 'surveillance-eligible' by default, shifting the burden of proof from intervention to inaction. By establishing size thresholds and growth rate benchmarks as de facto decision rules, radiology departments—backed by national guidelines parsed through local interpretation—created a new evidentiary regime where absence of change became data sufficient to justify continuation of observation, fundamentally altering the norms of clinical urgency. This challenges the assumption that watchful waiting emerged from consensus in thoracic surgery; instead, it gained legitimacy through a sideways epistemic capture where one specialty’s categorization practices overrode another’s historical prerogative, revealing how diagnostic hesitation can normalize therapeutic abeyance.
Moral Retrofit
The practice of monitoring rather than removing small nodules was retroactively framed as ethically superior within VA culture, not because outcomes data proved it so, but because failing to do so risked exposing systemic under-resourcing as a driver of delayed care—thus observation was rebranded from cost-contingent passivity to veteran-centered caution. Clinicians and policy advisors reframed surveillance as respect for veteran autonomy and avoidance of overtreatment, aligning with broader post-2010 movements against medical excess, but in the VA context this moralization served to absorb criticism over access delays by transforming wait times into deliberate, value-laden clinical pauses. This dissonance—portraying structural inertia as ethical sophistication—reveals how a practice born of constraint was later resuscitated as progressive, cloaking continuity of care gaps in the language of patient-centered restraint.
Clinical standardization pressure
The adoption of watchful waiting for small lung nodules in VA centers was decisively shaped by the 2005 Fleischner Society guidelines, which provided specific size-based criteria for radiologic surveillance, becoming codified in VA imaging protocols by 2008. This shift was institutionalized through integration into the Veterans Health Administration’s Computerized Patient Record System, where decision support alerts prompted adherence, binding individual clinician judgment to evidence-based thresholds. The non-obvious mechanism here is not medical consensus alone, but the systemic leverage of standardized guidelines through electronic health record architecture, transforming recommendations into enforceable practice.
Risk redistribution infrastructure
The VA’s nationwide rollout of low-dose CT lung cancer screening programs after 2 Newton VA Medical Center pilot programs (2010–2012) generated large volumes of incidentally detected small nodules, overwhelming surgical capacity and forcing nonsurgical management pathways. Centralized radiology review hubs and regional multidisciplinary nodule boards emerged to triage cases, redistributing clinical risk from individual surgeons to collective interpretive panels. This reconfiguration made watchful waiting feasible not because of diagnostic certainty, but because systemic overload necessitated a new risk-bearing apparatus across the VA’s integrated care network.
Audit-driven conservatism
The incorporation of nodule surveillance compliance metrics into the VA’s Office of Quality and Performance dashboards after 2013 incentivized adherence to observation protocols over surgical intervention, as overtreatment began to be measured as a quality failure. Radiologists and pulmonologists faced increasing scrutiny under peer review panels that compared facility-level surgery rates against national benchmarks, creating institutional pressure to avoid resection in boundary-case nodules. The underappreciated force here is not clinical evidence but a bureaucratic realignment of accountability, where prudence became quantified as avoidance of intervention outliers, cementing observation as the default path.