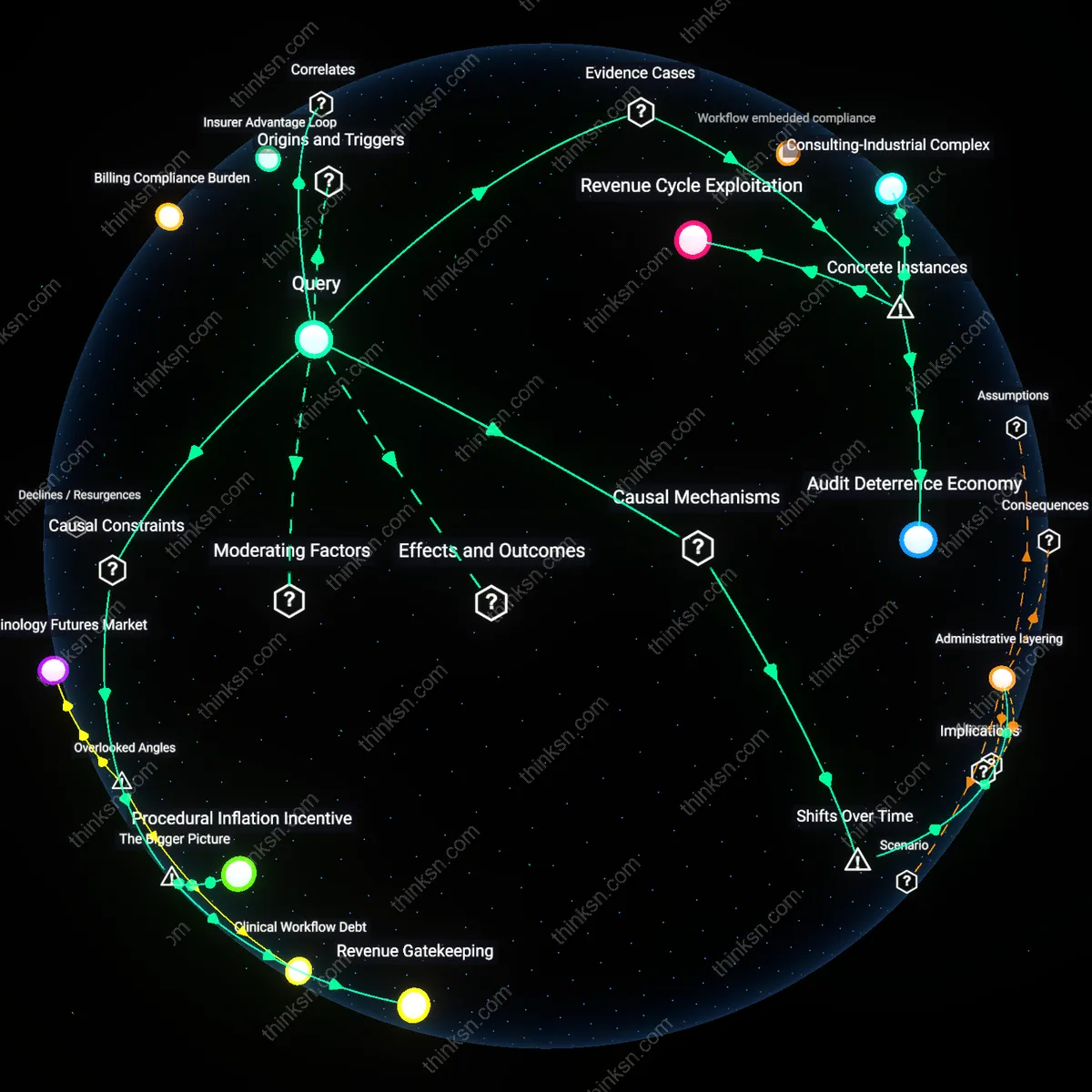
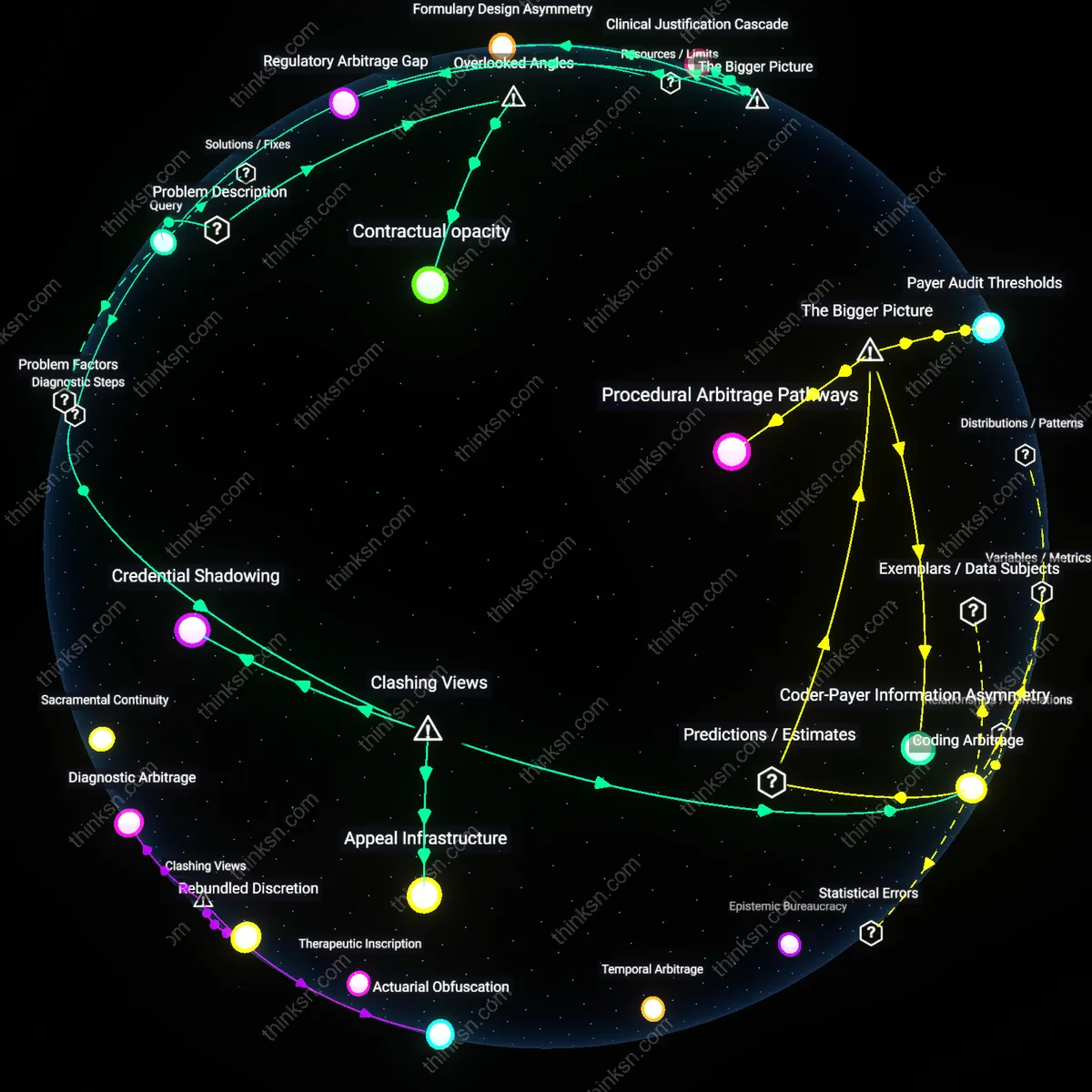
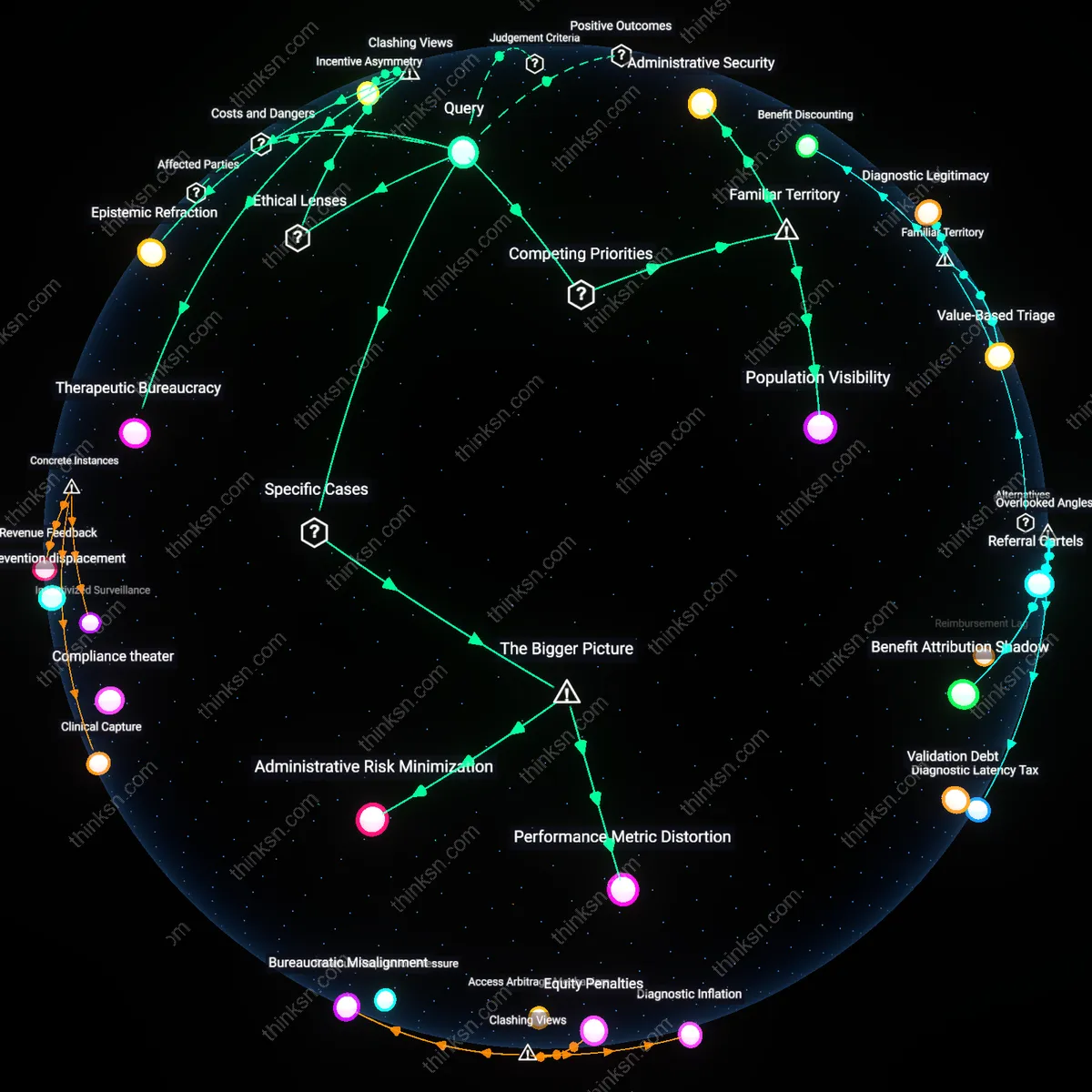
Who Benefits from Complex Plan Tiering as Consumers Struggle?
Analysis reveals 10 key thematic connections.
Key Findings
Actuarial opacity
Insurance providers benefit from the complexity of health plan tiering because the unpredictability of individual medical costs creates a knowledge asymmetry that insulates premium pricing from consumer resistance. Actuaries within large insurers use risk segmentation models—classified by age, geography, and claims history—not to clarify options for enrollees but to justify tiered premium differentiation under the guise of personalization, even when cost tiers misalign with actual utilization. This system leverages regulatory tolerance for statistical aggregation to maintain margin stability, revealing that the real product being priced is not healthcare access but uncertainty management for underwriters.
Provider rent extraction
Hospital systems and specialized care networks benefit from health insurance tiering by capturing differential reimbursement rates across plan levels, transforming administrative complexity into a mechanism for revenue stratification. When high-tier plans direct patients toward preferred providers with higher payout structures, the financial incentive shifts medical decision-making toward expensive facilities regardless of clinical necessity—effectively using consumer confusion about tier implications to justify cost-escalating referrals. This dynamic reveals that complexity functions not as a market inefficiency but as an institutionalized channel for rent extraction embedded in network negotiation protocols.
Regulatory arbitrage
State and federal regulators benefit from the opacity of health plan tiering by outsourcing actuarial accountability to private insurers, allowing public oversight bodies to appear cost-conscious while evading responsibility for affordability outcomes. By endorsing tiered structures as consumer-choice mechanisms, agencies like the CMS or state insurance departments shift blame for unpredictable out-of-pocket costs onto individual decision-making, even when plan designs are too convoluted to allow informed selection. This reveals that the political function of tiering is less about risk alignment than about enabling systemic deflection of policy failure through manufactured individual responsibility.
Regulatory legitimacy surplus
State insurance regulators benefit from the complexity of health insurance plan tiering because the appearance of structured consumer choice generates a legitimacy surplus that insulates agencies from political pressure, even when tiering fails to improve outcomes. This operates through the dynamic in states like North Carolina and Michigan, where regulators adopt federally recommended tier frameworks to signal compliance and technical rigor, thereby outsourcing accountability to 'market design' while avoiding direct intervention in pricing. The non-obvious point is that tiering complexity serves a bureaucratic function—maintaining the perception of oversight—rather than an economic one, turning incomprehensibility into a quiet asset for agencies that gain political cover without delivering clarity or affordability.
Administrative Rent Extraction
Insurance companies benefit from tiered health plan complexity because it inflates administrative costs that are passed directly to employers and the federal government under risk-adjusted payment models, as demonstrated by UnitedHealthcare’s systematic overreporting of patient risk scores in the Medicare Advantage program from 2010 to 2017. This generated billions in excess payments not tied to actual care delivery, revealing that complexity enables a form of bureaucratic rent-seeking where entities profit from interpreting and managing opaque rules rather than improving health outcomes. The mechanism hinges on asymmetrical data access and regulatory toleration of marginal coding expansion, which rewards granular classification of illness severity without requiring commensurate improvements in care access or quality. This exposes how the appearance of actuarial precision legitimizes cost inflation disguised as risk management.
Cognitive Burden Privilege
Large self-insured employers such as Walmart benefit from the complexity of health insurance tiering because it creates a barrier to employee mobility and unionization, allowing the company to maintain lower labor costs while offering nominally comprehensive coverage. Between 2005 and 2015, Walmart leveraged tiered formularies, narrow networks, and variable cost-sharing to design plans that were difficult for workers to fully understand, thereby reducing claims utilization and discouraging workforce organizing around health benefits. The deliberate obscurity functions not as a flaw but as a feature that exploits unequal health literacy and time poverty among low-wage workers. This reveals how complexity becomes a tool of labor control, where predictability of cost matters less to employers than the suppression of worker bargaining power.
Regulatory Arbitrage Opportunity
State Medicaid agencies, such as Ohio’s Department of Medicaid under its 2016 managed care expansion, benefit from tiered health plan complexity by outsourcing actuarial risk and service coordination to private insurers while retaining oversight responsibilities, thus shifting financial volatility onto enrollees without relinquishing political accountability. By structuring managed care organizations (MCOs) into multiple benefit tiers with divergent provider networks and copayment schemes, the state created a tiered accountability structure where poor outcomes could be attributed to MCO underperformance rather than policy design. This allows public agencies to appear market-oriented while insulating themselves from blame, illustrating how complexity facilitates a strategic diffusion of responsibility that preserves institutional legitimacy regardless of service quality. The non-obvious insight is that complexity serves bureaucratic survival by enabling plausible deniability.
Insurer Advantage
Insurers benefit from health insurance plan tiering because complexity increases consumer uncertainty, reducing price sensitivity and enabling higher premiums. The tiered structure obscures true cost differences between plans, which allows insurers to design benefit designs that appear generous but restrict access to high-value care through narrow networks or high out-of-pocket costs. This dynamic persists because regulators accept actuarial logic as justification, even when consumers cannot parse it—making opacity a built-in profit safeguard. The non-obvious insight is that in familiar public discourse, choice and competition are seen as solutions, yet the system rewards structures that make meaningful comparison impossible.
Employer Leverage
Large employers benefit from complex tiering because it shifts financial risk and administrative burden away from the company and onto employees. By offering a menu of opaque plans, employers can contain premium contributions while advertising broad 'choice,' aligning with widely accepted norms of flexibility and personalized decision-making. The mechanism operates through payroll-integrated benefits systems, where HR departments rely on defaults and nudge-based designs that assume employee comprehension. What’s underappreciated is that this familiarity with 'plan choice' as a standard benefit masks how the complexity actually undermines equitable health outcomes, particularly for lower-wage workers.
Regulatory Plausibility
Government regulators benefit politically from tiered complexity because it allows them to claim broad coverage access without enforcing transparent value comparisons across plans. Tiering provides a façade of consumer empowerment—anchored in popular ideas like 'options' and 'individual responsibility'—that legitimizes market-based reforms over systemic cost control. This justification works through standardized plan labels (e.g., Bronze, Silver) that create an illusion of clarity while preserving industry flexibility. The non-obvious consequence is that the very transparency tools meant to guide decisions end up naturalizing complexity, making it seem necessary rather than strategic.