Is Your Insurer Denying Mental Health Coverage Legitimately?
Analysis reveals 8 key thematic connections.
Key Findings
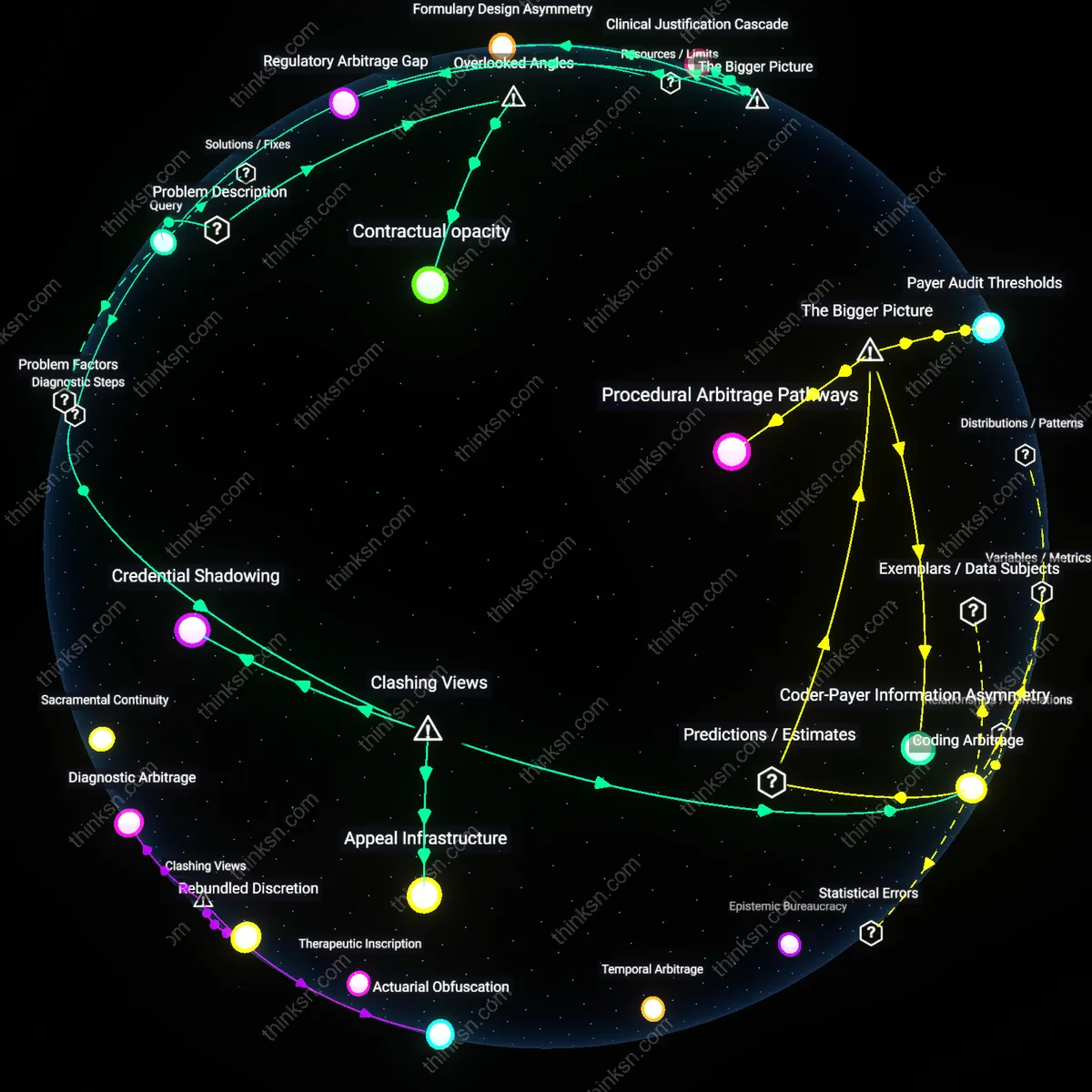
Contractual opacity
A patient can distinguish between legitimate coverage limits and discretionary denials by examining the specific language of their plan’s Summary of Benefits and Coverage for cross-referenced clinical policies, because insurers often embed mental health exclusions in supplementary documents that are not linked in the main benefit summary, creating a deliberate navigational barrier. This fragmentation between publicly accessible summaries and inaccessible clinical review guidelines enables denials to appear legitimate without requiring transparent justification, and the mechanism operates through ERISA-governed plan design choices that privilege administrative obscurity over patient clarity. What is underappreciated is that the denial itself may cite a seemingly valid policy, but the policy’s material terms are hidden in non-integrated administrative manuals, making appeal efforts misdirected or futile—this shifts the focus from intent to architecture.
Utilization threshold drift
A patient can detect discretionary cost-saving denials by tracking the insurer’s evolving use of session limits across time and provider type, because mental health benefit constriction often occurs incrementally through shifting benchmarks in internal utilization reviews rather than through formal plan amendments. These micro-adjustments—such as lowering 'medically necessary' thresholds from 20 to 12 sessions for anxiety—are implemented via non-public Medical Policy Bulletins updated quarterly and applied retroactively by third-party review firms like Carelon or eviCore. The overlooked dynamic is that these drifts mimic clinical standards but are statistically derived from aggregated claims data to minimize payout exposure, not evidence-based care—making denial patterns detectable only through longitudinal, comparative claims analysis, not isolated appeal.
Appeal Infrastructure
Initiate a formal peer-to-peer clinical appeal to expose whether the denial rests on articulated medical criteria or operational inertia. This step involves the treating clinician directly engaging the insurer’s reviewing psychiatrist through documented dialogue, where the standard of care and patient trajectory are defended using DSM-5-TR criteria and treatment response data; it reveals whether the insurer upholds a consistent medical necessity framework or retreats when professional accountability is activated. The non-obvious insight—in direct tension with the assumption that denials reflect policy—is that most coverage rationing occurs not through explicit rules but through asymmetric procedural barriers insurers expect providers to avoid.
Coding Arbitrage
Reclassify the clinical service under a differently reimbursed procedural code to test whether identical care is approved when framed as medical rather than behavioral intervention, such as submitting counseling for major depressive disorder under a chronic pain management code when comorbid somatic symptoms exist. This exploits the systemic bifurcation in insurance design where mental health services are subject to stricter utilization review than identical cognitive-behavioral techniques deployed in primary care settings; the differential outcome exposes that many denials are not clinical judgments but structural cost containment by diagnostic taxonomy. This contradicts the dominant narrative that parity laws already equalize mental health access, revealing instead that coding determines coverage independently of clinical content.
Credential Shadowing
Route counseling through a non-psychiatric provider with delegated supervisory authority, such as a primary care physician who absorbs the therapist into a care team under chronic disease management billing. This bypasses standalone mental health visit limits by embedding therapy within a medically justified longitudinal plan, revealing that the insurer’s coverage architecture treats identical counseling as wasteful when siloed but necessary when medically anchored. This fractures the intuitive belief that denials reflect patient-specific ineligibility, instead exposing a hidden hierarchy in which mental health is only legitimate when subordinated to physical health oversight.
Regulatory Arbitrage Gap
Patients cannot reliably distinguish legitimate coverage limitations from discretionary denials because mental health parity laws like the Mental Health Parity and Addiction Equity Act (MHPAEA) are enforced through decentralized, opaque insurance review processes that prioritize procedural compliance over substantive equivalence in treatment authorization—enabling insurers to exploit gaps between federal mandates and state-level implementation. Insurers leverage asymmetric access to medical necessity criteria and internal appeals logic, which are rarely transparent to providers or patients, allowing them to frame cost-containment decisions as clinically justified under loose regulatory definitions. This dynamic persists because enforcement relies on reactive audits rather than proactive standardization of review protocols, making systematic evasion feasible without legal penalty. The non-obvious consequence is that the structural weakness lies not in the law itself but in the fragmentation of oversight across federal agencies, state insurance commissioners, and employer-sponsored plan exemptions.
Formulary Design Asymmetry
A patient may mistake a cost-saving decision for a legitimate limitation when insurers use tiered network design and differential copays to de facto exclude access to licensed mental health practitioners, even when such services are nominally 'covered' under the plan—this occurs because essential behavioral health benefits are often fulfilled through narrow networks with insufficient provider capacity, particularly for evidence-based or longer-term therapies. Unlike medical services, where utilization management is typically triggered by high-cost procedures, mental health counseling is restricted preemptively through provider scarcity and geographic maldistribution, masking rationing as availability failure. This mechanism is amplified in self-insured employer plans, which are exempt from state licensing oversight and can contract with third-party administrators to set de facto coverage rules without public disclosure. The underappreciated reality is that benefit design itself—shaped by actuarial models predicting low utilization—becomes the rationing tool, not explicit denial.
Clinical Justification Cascade
Insurers obscure the line between legitimate and discretionary denials by outsourcing coverage decisions to third-party utilization review firms that apply proprietary algorithms—such as InterQual or MCG criteria—requiring a documented 'acute symptom trajectory' for ongoing counseling, thereby reframing chronic or preventive mental health care as 'medically unnecessary' despite clinical guidelines. These tools are calibrated for inpatient or short-term intervention benchmarks, misaligned with psychotherapeutic timelines, and applied by nurses or mid-level reviewers without psychiatric training, creating systematic bias against continued outpatient care. The systemic trigger is the misalignment between process-driven insurance risk management and longitudinal therapeutic outcomes, where the insurer’s need for measurable, short-term improvement metrics overrides clinical judgment documented by treating therapists. What remains hidden is that the denial is not based on policy exclusions but on the operational logic of scalability in claims adjudication, which inherently favors categorical cut-offs over individualized treatment plans.