Black Box Warnings vs Corporate Messaging on Drug Risks?
Analysis reveals 6 key thematic connections.
Key Findings
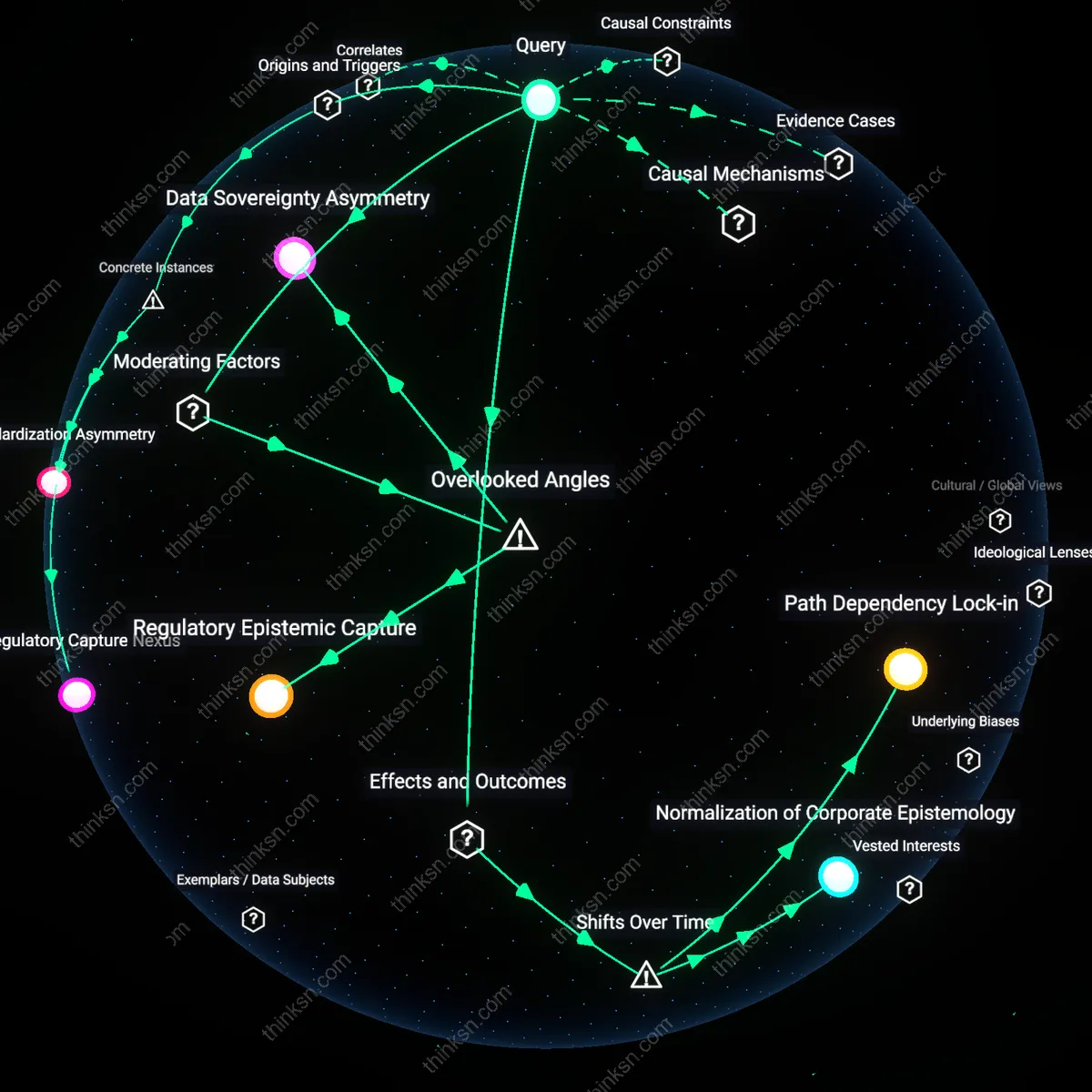
Regulatory Epistemic Capture
Regulatory black box warnings are systematically weakened when corporate marketing narratives infiltrate the epistemic standards of regulatory agencies, such that downplaying risk becomes justified through selectively accepted scientific uncertainty. Pharmaceutical regulators, particularly in the U.S., often rely on industry-generated clinical trial data and risk-assessment models that normalize commercial framing of safety, which subtly reframes adverse effects as outliers rather than systemic threats. This mechanism is invisible in standard critiques because it does not require overt corruption—only the quiet assimilation of corporate epistemology into what counts as 'credible' evidence within regulatory science. The overlooked dynamic is that marketing does not just influence consumers; it reshapes the institutional criteria for evaluating risk itself.
Patient-Performance Economy
Patients internalize marketing messages as part of a performative health identity, which leads them to dismiss black box warnings as irrelevant to their 'responsible' use, thus corporate messaging indirectly disables regulatory caution at the behavioral level. This occurs most visibly in chronic disease markets like psychiatric or metabolic medications, where direct-to-consumer advertising frames adherence as moral self-mastery, transforming drug use into a disciplined lifestyle performance. The non-obvious dependency here is that regulatory warnings assume rational cognitive processing, but they collapse when the deeper social reward of perceived agency—cultivated by marketing—overrides abstract risk information. Most analyses miss that the conflict isn't between regulation and marketing per se, but between two competing systems of meaning in patient subjectivity.
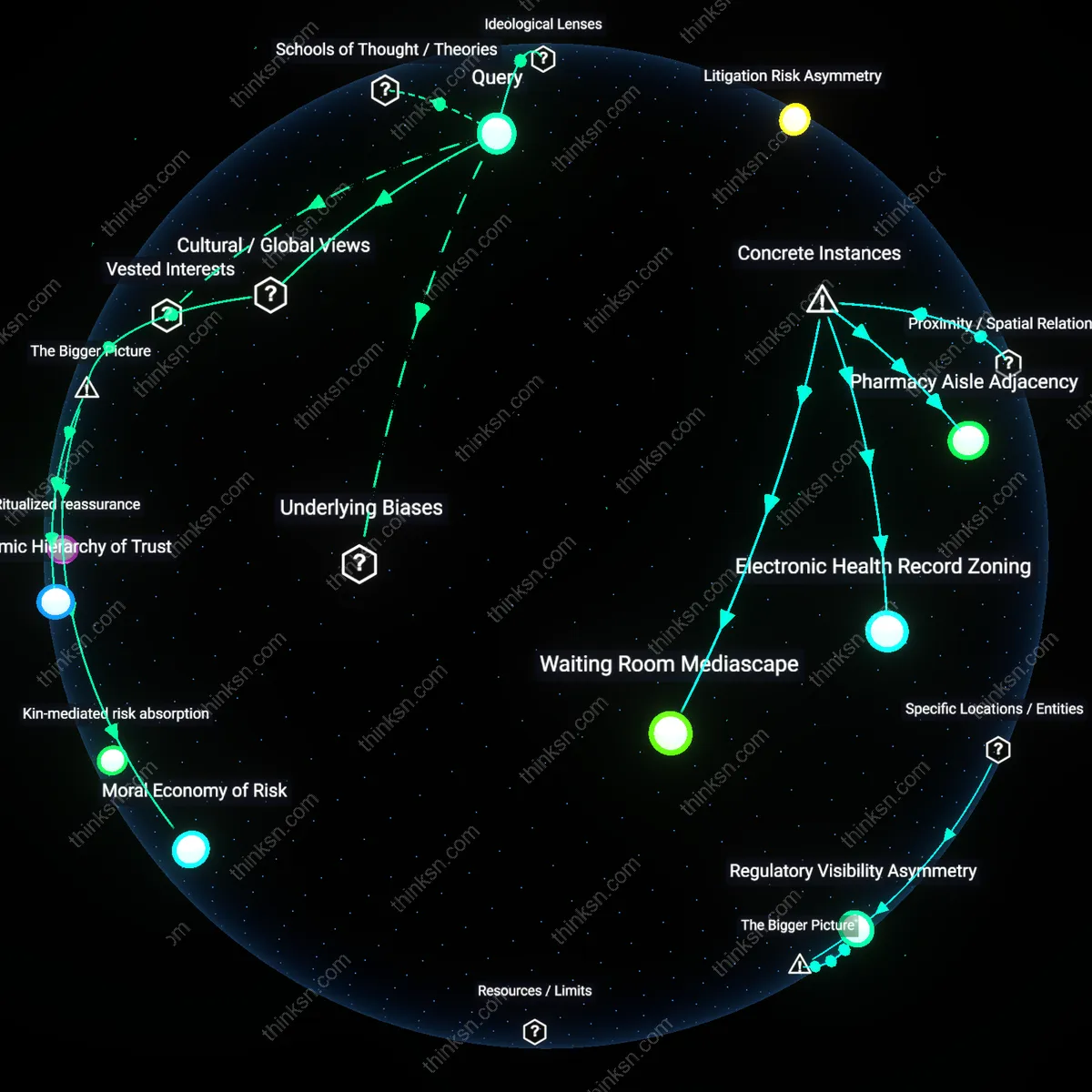
Litigation Risk Asymmetry
Corporate legal departments deliberately allow marketing teams to downplay risks because black box warnings provide a legal 'safe harbor'—once a risk is disclosed, courts are far less likely to award punitive damages, thereby making warnings a liability shield rather than a consumer protection. This creates an incentive for firms to push marketing messages to the edge of deception, knowing that regulators will mandate warnings as a compromise, effectively letting legal and marketing strategies collude across domains. The overlooked dynamic is that regulation does not counter marketing here—it enables it, by absorbing legal risk while marketing captures market share. This reframes the tension not as a failure of enforcement, but as a functional design within corporate risk finance.
Regulatory Temporality Divide
Western pharmaceutical regulators prioritize individual autonomy through rapid black box warnings, whereas East Asian health authorities often delay such measures to preserve social harmony and institutional trust. This divergence reflects a deeper systemic tension where U.S. and EU agencies treat risk disclosure as a legal imperative to protect patient choice, while countries like Japan and South Korea embed warnings within collective decision-making frameworks that defer to physician authority and family consensus. The non-obvious consequence is that corporate marketing in East Asia exploits this delayed temporal window, positioning drugs as socially validated before regulatory warnings gain traction, thus aligning commercial narratives with cultural expectations of medical consensus.
Moral Economy of Risk
In predominantly Catholic regions like Latin America, corporate marketing subtly frames pharmaceutical risks as part of divine suffering or karmic endurance, indirectly countering regulatory warnings framed in secular biopolitical terms. Drug campaigns often employ imagery of hope, resilience, and familial duty—resonant with religious narratives—thereby reframing side effects as moral burdens willingly borne for the sake of healing. This dynamic enables companies to downplay black box warnings not through denial but through spiritual reframing, exploiting a systemic gap between technocratic risk assessment and culturally embedded patient worldviews, where the authority of medicine is interpreted through pastoral care rather than bureaucratic oversight.
Epistemic Hierarchy of Trust
In many African and South Asian markets, corporate marketing co-opts community health workers and traditional healers as intermediaries, positioning pharmaceuticals as modern yet culturally continuous, while regulatory warnings remain confined to distant, colonial-style institutions. This creates an epistemic hierarchy where local trust networks override abstract state mandates, allowing risk-downplaying messages to circulate under the guise of inclusive outreach. The systemic trigger is the historical underfunding of national drug safety agencies, which forces patients to rely on personalized, trusted voices—voices that corporations strategically infiltrate, making black box warnings appear foreign, cold, and disconnected from lived experience.