Vaccine Without Proof: Who Holds the Power in Your Health Choices?
Analysis reveals 8 key thematic connections.
Key Findings
Diagnostic Sovereignty
The absence of large-scale trial data in vaccine recommendations redistributes epistemic authority from collective regulatory standards to individual physicians, thereby converting preventive care into an act of clinical judgment rather than public health validation. This shift became pronounced after the 2009 H1N1 pandemic, when emergency use authorizations normalized off-protocol vaccine rollout, embedding physician discretion as a structural safeguard—despite unequal access to training or evidence interpretation resources. What is underappreciated is that this reconfiguration does not merely reflect medical uncertainty but institutionalizes a new hierarchy where frontline clinicians, often in resource-constrained settings, bear disproportionate liability for population-level decisions previously guided by phased trial evidence.
Immunogenic Privilege
When doctors recommend unvalidated vaccines, they leverage bodily access and patient trust to generate de facto immunity markets, a transformation rooted in the post-2015 erosion of pharma exclusivity due to biologics competition and digital health tracking. This enables certain providers—especially in urban private clinics in upper-middle-income countries like Brazil or South Korea—to treat vaccine recommendation as a premium service, bundling it with genomic risk assessments despite trial gaps, thereby converting preventive advice into a stratified commodity. The overlooked mechanism is not just information asymmetry but the medicalization of anticipation, where the right to be vaccinated ahead of consensus becomes a marker of status, retroactively legitimizing early adoption through presumed biological prescience.
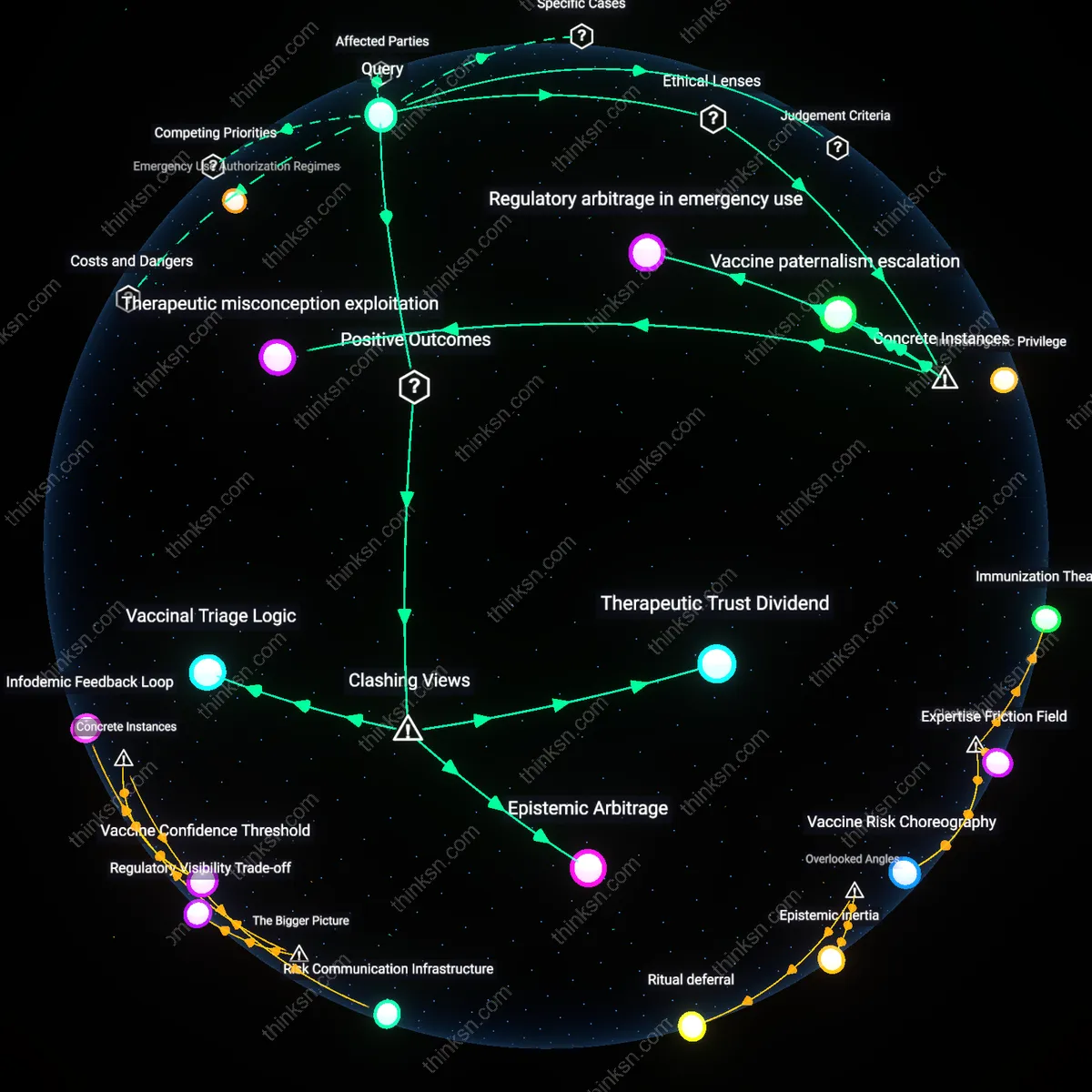
Therapeutic Trust Dividend
Recommending a preventive vaccine without large-scale trial data can strengthen patient-physician trust when the physician transparently communicates uncertainty and involves the patient in risk calibration, leveraging clinical judgment and localized evidence; this dynamic converts epistemic vulnerability into relational capital, especially in underserved communities historically excluded from medical trials, where swift protective action—framed as solidarity rather than experimentation—can enhance long-term engagement with care systems. The non-obvious insight is that perceived paternalism may invert into participatory empowerment when transparency about limited data is used not to deter action but to co-construct responsibility.
Epistemic Arbitrage
A doctor advocating for a vaccine lacking broad trial validation enacts a form of knowledge privileging—favoring epidemiological urgency or mechanistic plausibility over population-level confirmatory data—which advantages institutional speed over democratic deliberation, allowing clinical authority to pre-empt public skepticism and lock in early adoption; this asymmetry benefits public health infrastructure by creating de facto compliance before countervailing narratives emerge, effectively turning medical recommendation into a policy enforcement tool masked as individualized care. The overlooked mechanism is that premature endorsement functions less as clinical guidance than as cognitive framing, shaping perception before evidence can accumulate.
Vaccinal Triage Logic
When physicians recommend unproven preventive vaccines, they implicitly assign higher value to future harm reduction than to present procedural rigor, thus redistributing risk away from patients and onto structural systems that manage outbreaks—this shift benefits public health agencies by compressing decision cycles and enabling rapid downstream coordination in supply chains, surveillance, and risk communication, even if individual justification appears weak; the asymmetry becomes productive when viewed not as a breach of ethics but as a calibrated sacrifice of methodological purity for systemic resilience. The dissonant insight is that medical overreach in recommendation can generate public good by forcing institutional adaptation to emergent threats.
Therapeutic misconception exploitation
When the Tuskegee Syphilis Study researchers administered ineffective treatments to Black sharecroppers while withholding known cures, they framed medical procedures as protective care despite no clinical benefit, thereby leveraging patients’ trust in physician expertise to obscure the absence of valid therapeutic intent. This reveals how preventive recommendations lacking empirical validation can reconfigure the doctor-patient relationship into one of epistemic control, where the appearance of medical authority substitutes for evidence, particularly affecting populations already marginalized by systemic racism. The non-obvious insight is that the guise of prevention can serve as a mechanism of consent manipulation even in the absence of overt coercion.
Regulatory arbitrage in emergency use
During the 2009 H1N1 pandemic, Mexican health authorities fast-tracked the deployment of AS03-adjuvanted influenza vaccines without completed phase IV safety monitoring, privileging rapid immunization over transparent risk assessment in low-income regions while high-income countries delayed rollout until post-marketing data were available. This divergence illustrates how clinical uncertainty in preventive recommendations can become a tool for spatially uneven risk distribution, justified under emergency powers yet reinforcing global health hierarchies. The underappreciated dynamic is that emergency protocols enable states to outsource experimental risk to vulnerable populations under the legitimacy of public health urgency.
Vaccine paternalism escalation
In 1998, when French health officials recommended universal hepatitis B vaccination in schools amid emerging but inconclusive links to multiple sclerosis, the state sustained the campaign even as epidemiological doubts grew, prioritizing institutional credibility over informed refusal. This case demonstrates how preventive vaccine advocacy without robust trial data can morph into institutional self-preservation, where medical authority consolidates power by framing skepticism as public endangerment. The overlooked mechanism is that uncertainty can trigger a defensive professional reflex that transforms precaution into dogma, elevating compliance over critical engagement.