Who Wins When Disability Claims Need Extensive Proof?
Analysis reveals 6 key thematic connections.
Key Findings
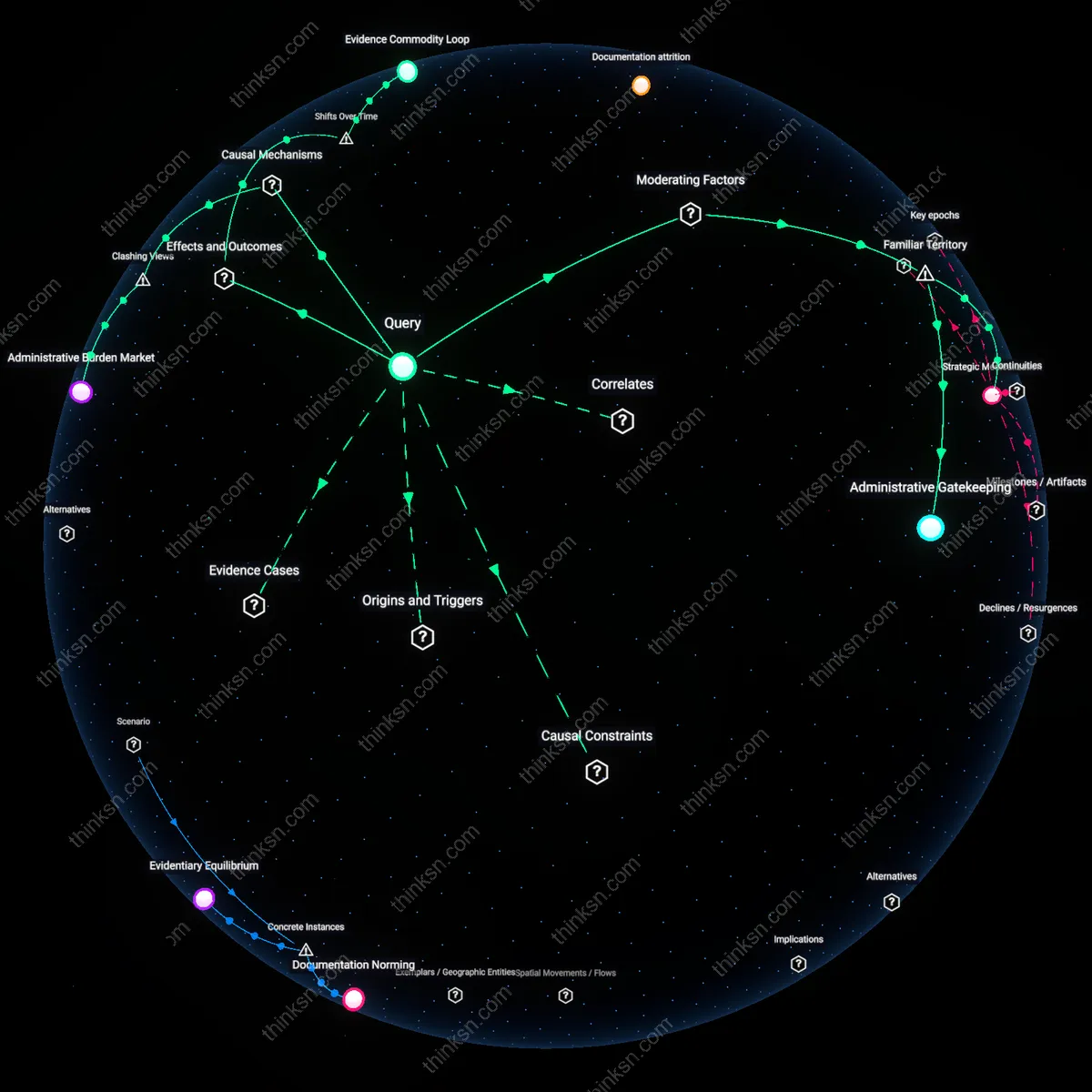
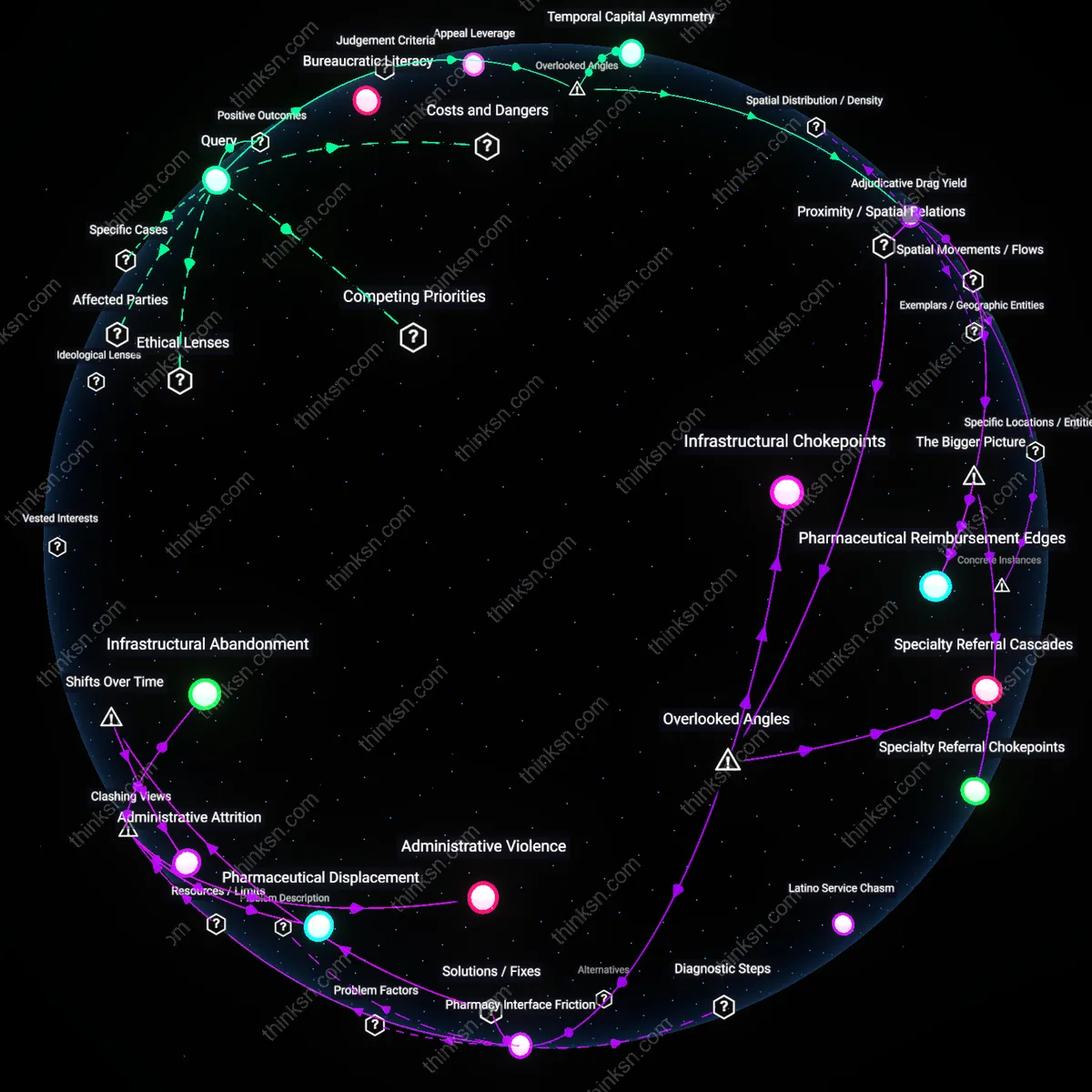
Administrative Burden Market
Insurers’ documentation requirements primarily benefit third-party medical evaluators who profit from producing disability assessment reports, not the insurers themselves. These evaluators—often contracted through regional networks like Independent Medical Examination (IME) firms—generate revenue per report, creating a financial incentive to expand documentation volume rather than verify legitimacy, which in turn forces applicants to anticipate and preemptively align with evaluative templates, distorting their narratives into bureaucratic genres. This reveals a system where disability verification is less about risk assessment and more about outsourcing adjudication to a monetized documentation economy, undermining the assumption that insurers tighten scrutiny to reduce payouts.
Strategic Narrative Inflation
Disability applicants who succeed do so not by meeting documentation standards but by exceeding them preemptively, thereby benefiting future claimants who use approved cases as templates—creating an evolutionary drift toward increasingly exaggerated symptom reporting. This escalation is driven by applicants observing that borderline cases are approved only when documentation is excessive, thus gaming the system through narrative inflation rather than authenticity, which in turn feeds insurers’ justifications for tighter requirements. This undermines the intuitive view that documentation ensures accuracy, instead revealing a feedback loop where fraud prevention mechanisms generate the very distortions they claim to prevent.
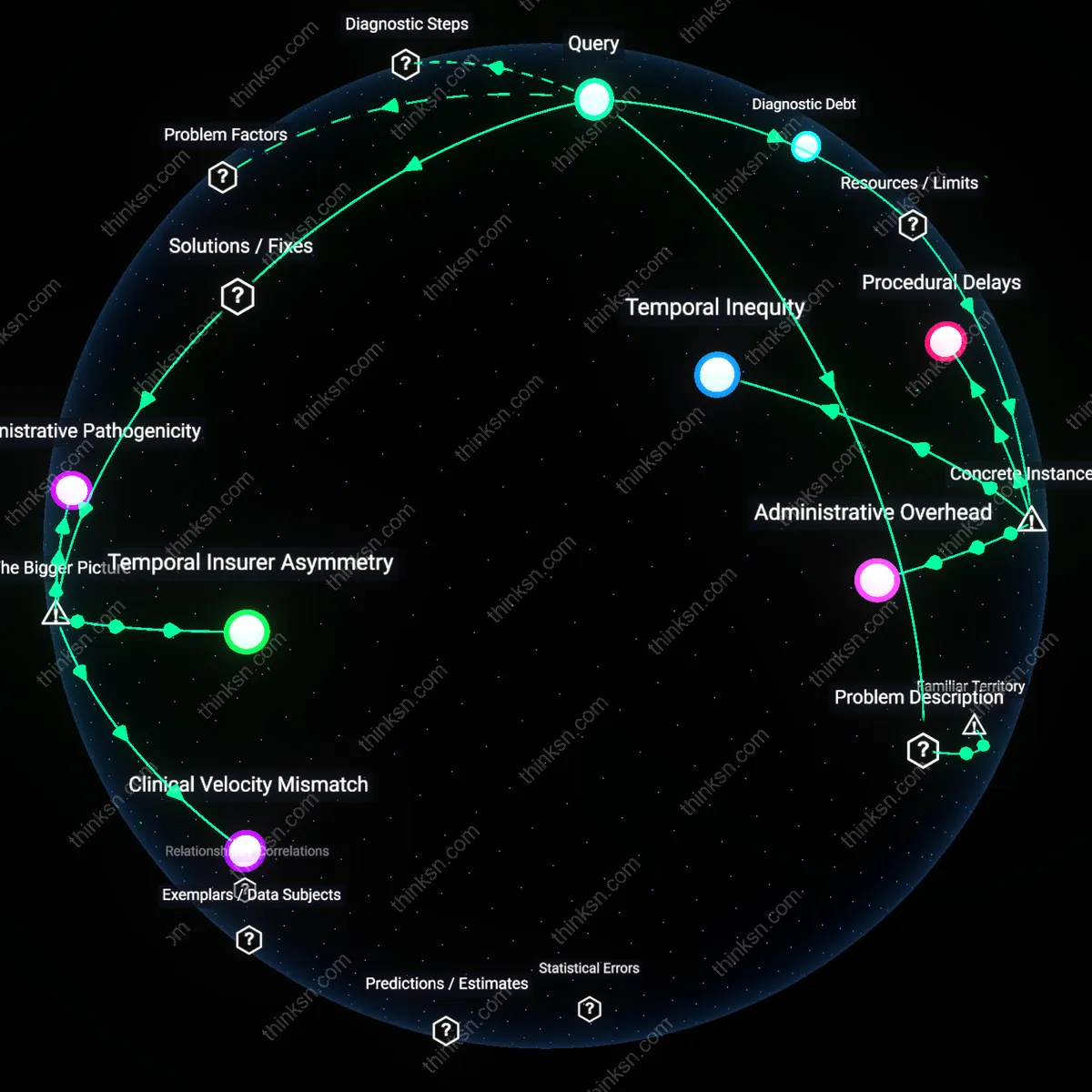
Temporal Erosion Effect
The prolongation of documentation timelines disadvantages applicants whose conditions fluctuate or degrade slowly, marking a decisive shift from early 20th-century models that recognized acute, categorical illnesses toward contemporary frameworks that govern chronic, contested conditions like fibromyalgia or mental health disorders. As insurers demand longitudinal records to confirm persistence—often spanning 12–24 months—applicants must navigate a system designed for industrial injuries that no longer reflects the epidemiological reality of service-sector disablement, where symptoms may be intermittent or environmentally triggered. This temporal mismatch advantages insurers by increasing case dropout rates and shifting interpretive authority to retrospective narratives, which are more vulnerable to skepticism. The shift exposes how time itself has become an instrument of exclusion, where the requirement to document over time produces delay, and delay produces disqualification.
Evidence Commodity Loop
Medical documentation has evolved into a tradable administrative currency, where the value of clinical notes lies less in diagnostic accuracy than in their alignment with insurance coding standards—a transformation accelerated by the integration of electronic health records (EHRs) post-2009 under U.S. HITECH incentives. Physicians, pressed by time and billing constraints, now produce documentation shaped by anticipated insurer scrutiny, not patient narrative, creating a feedback loop where only data formatted for third-party validation gain traction in claims processes. Applicants respond by targeting providers known for 'strong' letters, effectively shopping for documentation that conforms to bureaucratic templates rather than seeking holistic care. The non-obvious result is that evidence is no longer a neutral representation of condition but a manufactured product within a shadow market, where clinical authority is selectively monetized and disability is filtered through the logic of auditability.
Administrative Gatekeeping
Insurers' documentation requirements benefit internal claims reviewers by concentrating interpretive authority over medical evidence, enabling them to standardize evaluations across diverse conditions through rigid procedural compliance. This occurs within bureaucratic adjudication systems where consistency is prioritized over clinical nuance, making the reviewer’s control over eligibility thresholds more decisive than treating physicians’ assessments. Though commonly framed as ensuring fairness, this structure systematically advantages institutional risk management by rendering subjective medical realities into auditable paperwork trails, a shift whose opacity is rarely acknowledged in public debates about claim denials.
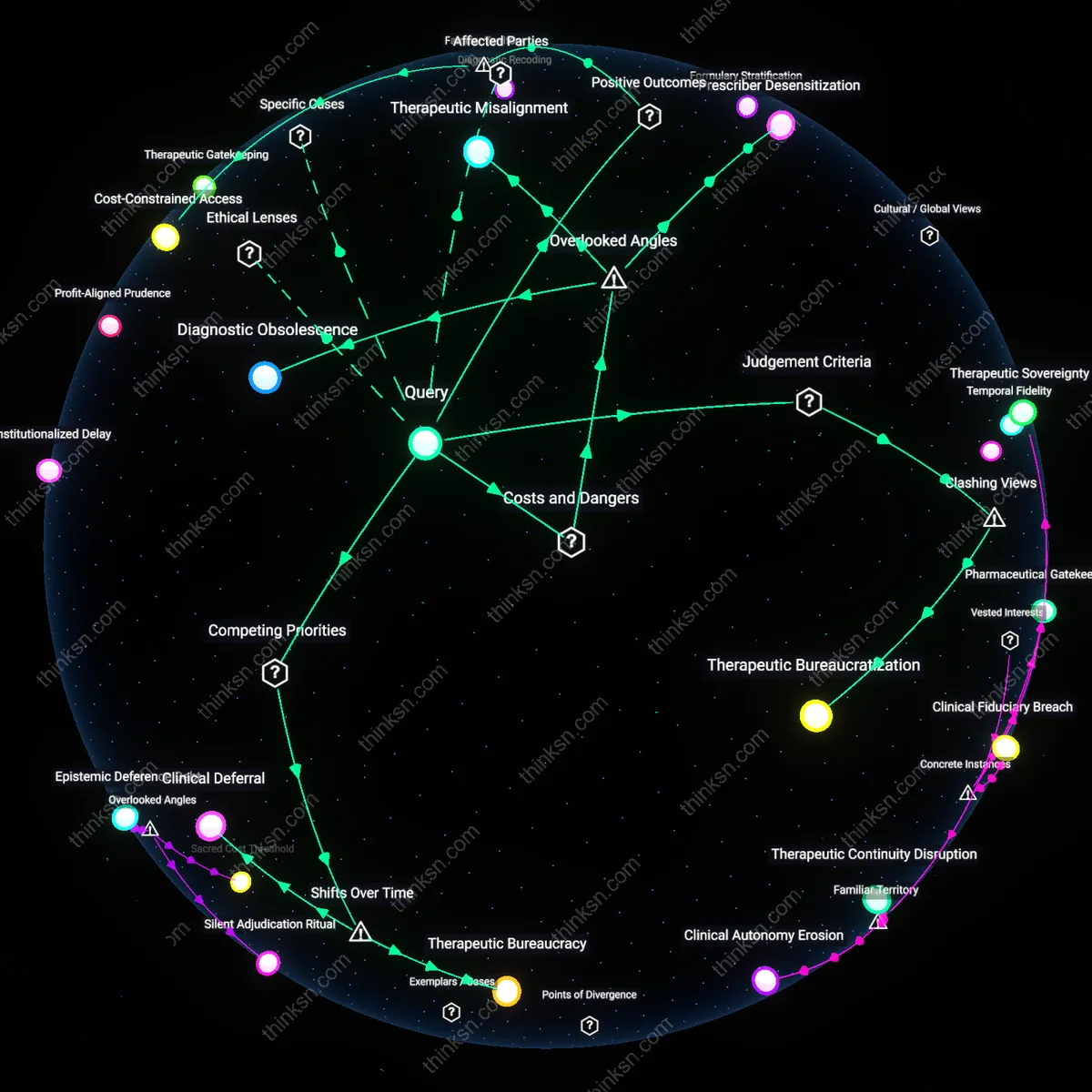
Strategic Medicalization
Treating physicians emerge as indirect beneficiaries of stringent documentation demands because patients compel them to produce justificatory narratives tailored to insurance criteria, expanding clinicians’ involvement in administrative labor that blurs therapeutic and evaluative roles. This dynamic operates through clinical settings where time and medical authority are diverted from treatment to producing ‘insurability-worthy’ records, reinforcing the public assumption that more medical documentation equals legitimacy. The underappreciated consequence is that physicians become de facto allies in applicants’ bureaucratic survival strategies, even as this inflates system-wide medicalization without necessarily improving health outcomes.