Medical Miscarriage Management vs Abortion Bans: Legal Risks?
Analysis reveals 6 key thematic connections.
Key Findings
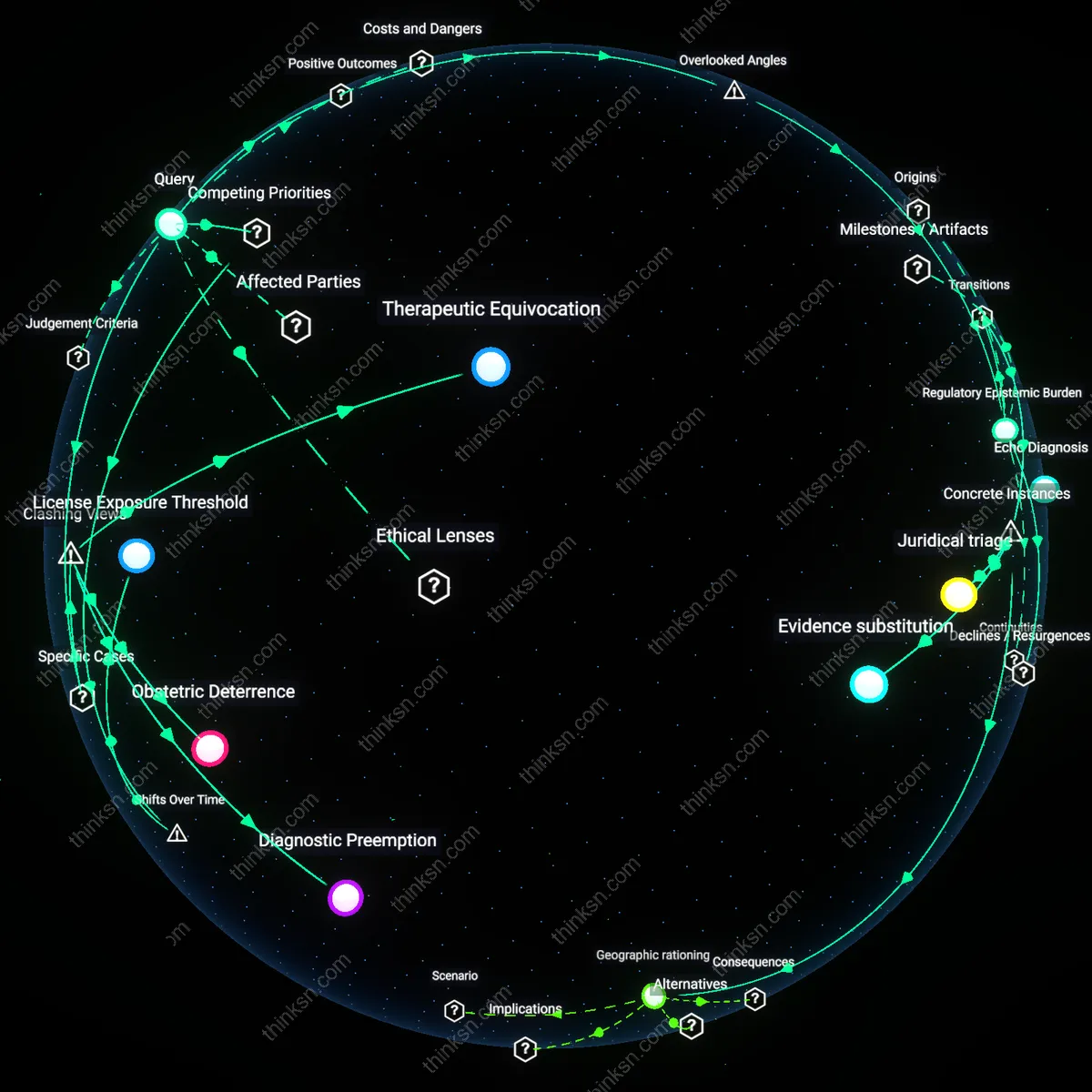
Regulatory Epistemic Burden
Ambiguity in abortion statutes heightens the epistemic responsibility of clinicians to prove their medical decisions were exclusively for managing nonviable pregnancies, imposing a legal justification requirement beyond clinical judgment. In states like Ohio or Louisiana, where abortion is banned except when ‘necessary to save the life of the mother,’ physicians managing miscarriages must now document not only fetal nonviability but also rule out any implication of intent—despite no such intent existing—because the absence of intent is not self-evident under the law. This creates an unseen cognitive and bureaucratic load that distorts clinical workflows, shifts medical reasoning toward legal defensibility, and elevates the risk of licensure review even in uncontested cases of spontaneous pregnancy loss. The overlooked dynamic is not the risk of prosecution per se, but the systemic induction of epistemic overproduction—clinicians must generate evidence not for patient care but for potential adjudication—a burden absent from the medical standards themselves.
License Exposure Threshold
Strict abortion laws post-Dobbs explicitly blur the distinction between induced abortion and miscarriage management, creating a retrospective zone of liability for clinicians who cannot retroactively prove intent, a shift from pre-2022 standards where medical judgment in uterine evacuation was protected under broader clinical discretion. As states criminalize pregnancy termination without recognizing the diagnostic uncertainty inherent in early pregnancy loss, physicians face prosecutorial scrutiny not for violating clear rules but for acting within now-ambiguous standard of care—turning medical discretion into legal jeopardy. This threshold—where routine care becomes prosecutable—emerged only after the collapse of federal constitutional protection eroded the shared understanding of lawful medical practice. The non-obvious consequence of this shift is that licensure, once a shield of professional autonomy, now functions as a vulnerability in jurisdictions with trigger laws lacking explicit clinical exceptions.
Clinical Judgment Erosion
Prior to 2010, miscarriage management operated largely within a framework of maternal safety protocols where uterine evacuation timing and method followed hemodynamic stability and patient symptoms, but the rise of fetal personhood statutes has reversed that priority by making fetal status retrospectively determinative of a clinician’s legal risk. This inversion means that decisions once guided by obstetrical urgency are now filtered through post-treatment forensic review, where pathology reports or delayed hCG curves can be weaponized to challenge medical intent. The transformation from real-time clinical reasoning to after-the-fact legal reconstruction undermines the temporal integrity of emergency care, revealing how the erosion of physician judgment in the name of fetal protection has produced a climate where non-intervention is safer legally than timely treatment.
Therapeutic Equivocation
State abortion bans create legal ambiguity that directly endangers clinicians managing miscarriages because the definition of abortion often omits explicit exception for spontaneous pregnancy loss, forcing physicians in Texas and Ohio to delay treatment until fetal demise is unequivocally documented, thereby risking patient sepsis and disciplinary action by medical boards. This occurs not from overt prohibition of miscarriage care but from prosecutorial discretion weaponizing statutory vagueness to retroactively frame standard obstetric interventions as illegal abortions, revealing that the law's ambiguity functions not as a loophole but as a disciplinary tool against clinical judgment.
Diagnostic Preemption
Clinicians in states like Idaho and Oklahoma self-censor miscarriage interventions not because they misdiagnose pregnancy loss but because abortion bans retroactively criminalize medical decisions made under diagnostic uncertainty, such as when ultrasound findings are inconclusive in early pregnancy; the fear of felony prosecution skews clinical thresholds toward waiting for definitive signs of fetal demise, even when earlier intervention aligns with standard care, demonstrating that legal definitions don't just shape treatment but actively restructure the timeline and criteria of diagnosis itself.
Obstetric Deterrence
The closure of obstetrics units in rural Alabama hospitals results not from direct legal threats to individual doctors but from hospital risk-aversion policies triggered by state abortion laws, where administrators restrict all uterine evacuation procedures—regardless of clinician intent—to avoid any potential legal exposure, thus displacing the threat to institutional governance and revealing that legal ambiguity exerts its most severe impact not at the bedside but through organizational withdrawal of reproductive care infrastructure.