Should Diabetics Wait on SGLT2 Inhibitors Despite Heart Benefits?
Analysis reveals 5 key thematic connections.
Key Findings
Therapeutic Trade-off
Do not delay SGLT2 inhibitor initiation due to uncertain kidney function because the cardiovascular protection these drugs offer in high-risk diabetic patients outweighs the potential harm from undetected renal decline—one missed dose of cardioprotection can trigger irreversible events like heart failure hospitalization, while kidney deterioration, though serious, is slower and more monitorable. The mechanism operates through primary care clinics and cardiology-nephrology handoffs, where the inertia of 'wait-and-see' under partial information favors visible, acute risks over latent ones. The non-obvious insight is that in everyday clinical routines, uncertainty about kidney function is treated as a deferral justification not because it is clinically dominant, but because it feels more controllable than probabilistic cardiac events—revealing how actionability, not severity, governs treatment initiation.
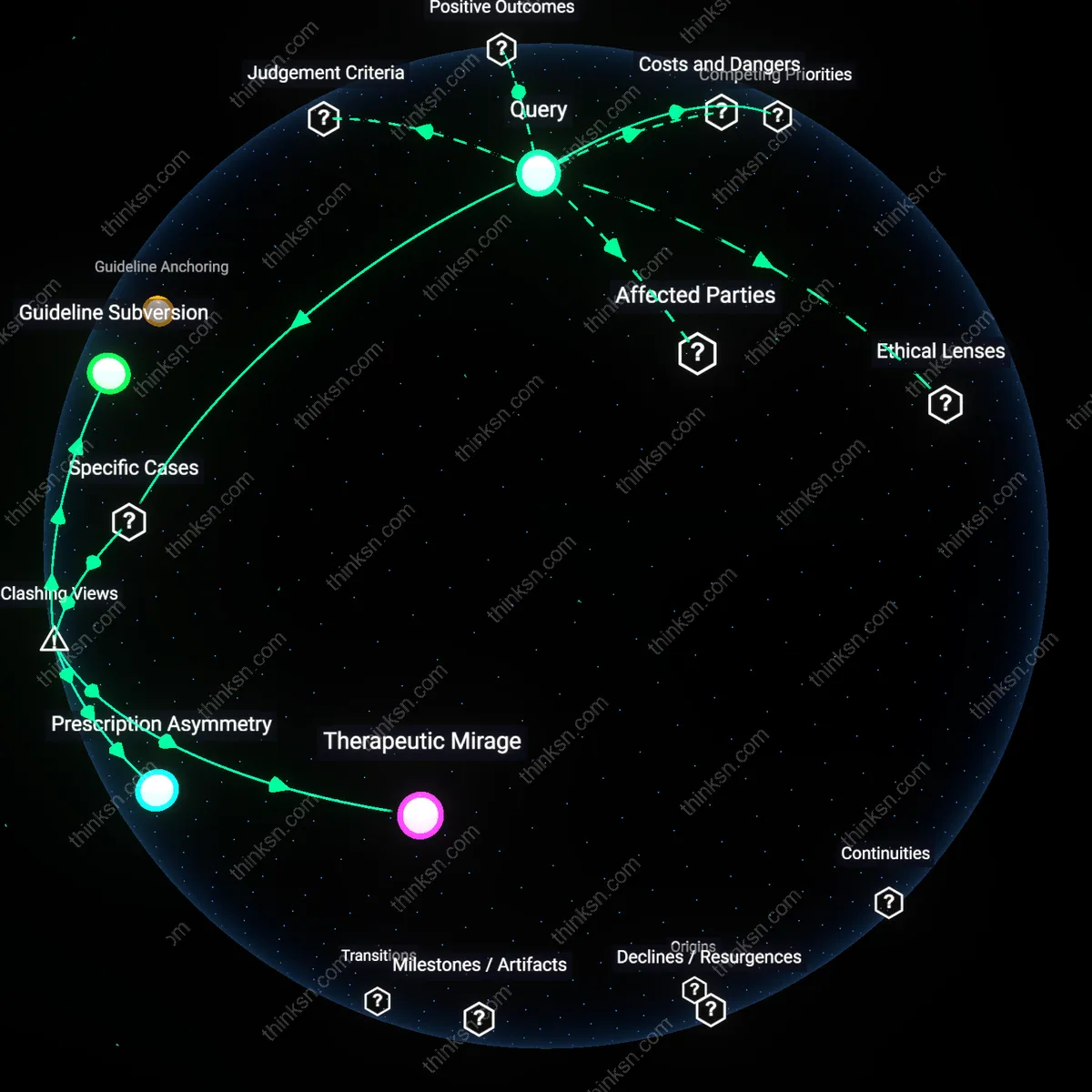
Guideline Anchoring
Delay SGLT2 inhibitor use until kidney clarity emerges because clinicians default to guideline adherence only when all eligibility criteria are legible, and uncertain eGFR values break the ritual of protocolized care seen in busy outpatient settings like diabetes management chains or retail health clinics. The system functions through standardized workflows where deviations trigger cognitive friction—the brain treats 'partial data' as 'non-compliance' with the guideline itself, not as a risk-benefit call. The underappreciated reality is that in public imagination and clinical habit, guidelines are not frameworks but checklists, so even when they permit early use, practitioners wait for full data completion, mistaking procedural fidelity for patient safety.
Guideline Subversion
A diabetic patient should delay SGLT2 inhibitor initiation when kidney function is uncertain because real-world African American populations in safety-net clinics in Jackson, Mississippi consistently experience misclassified eGFR due to racialized creatinine equations, which inflates estimated kidney function and risks precipitating ketoacidosis in patients with undetected advanced CKD; this mechanism reveals how guideline adherence in structurally biased settings propagates harm by treating race as biology, thereby making early initiation a vector of metabolic injustice rather than protection.
Therapeutic Mirage
A diabetic patient should delay SGLT2 inhibitor initiation despite guideline recommendations because cardiovascular benefit evidence primarily derives from exclusionary trials like DECLARE–TIMI 58 that systematically omitted patients with eGFR below 45 mL/min/1.73m², creating a false generalizability to real-world patients in states like West Virginia, where the prevalence of CKD stage 3b+ exceeds 22% and SGLT2 inhibitors are disproportionately prescribed without proven renal protection, thus exposing vulnerable populations to volume depletion without demonstrable risk reduction—a dynamic that exposes the cardiovascular benefit as a statistical artifact of selection, not a physiological inevitability.
Prescription Asymmetry
A diabetic patient should delay SGLT2 inhibitor initiation when kidney function is uncertain because in integrated health systems like Kaiser Permanente Northern California, automated decision-support alerts prioritize SGLT2 inhibitors for HbA1c control without equal emphasis on real-time renal trend analysis, causing primary care physicians to initiate therapy based on stagnant single-timepoint eGFR values amid fluctuating albuminuria, a system dynamic that reveals how procedural compliance with guidelines supplants clinical judgment, turning early initiation into a metric-driven ritual that penalizes caution as non-adherence.