Should Clinicians Recommend Annual Skin Checks Without Mortality Benefit?
Analysis reveals 7 key thematic connections.
Key Findings
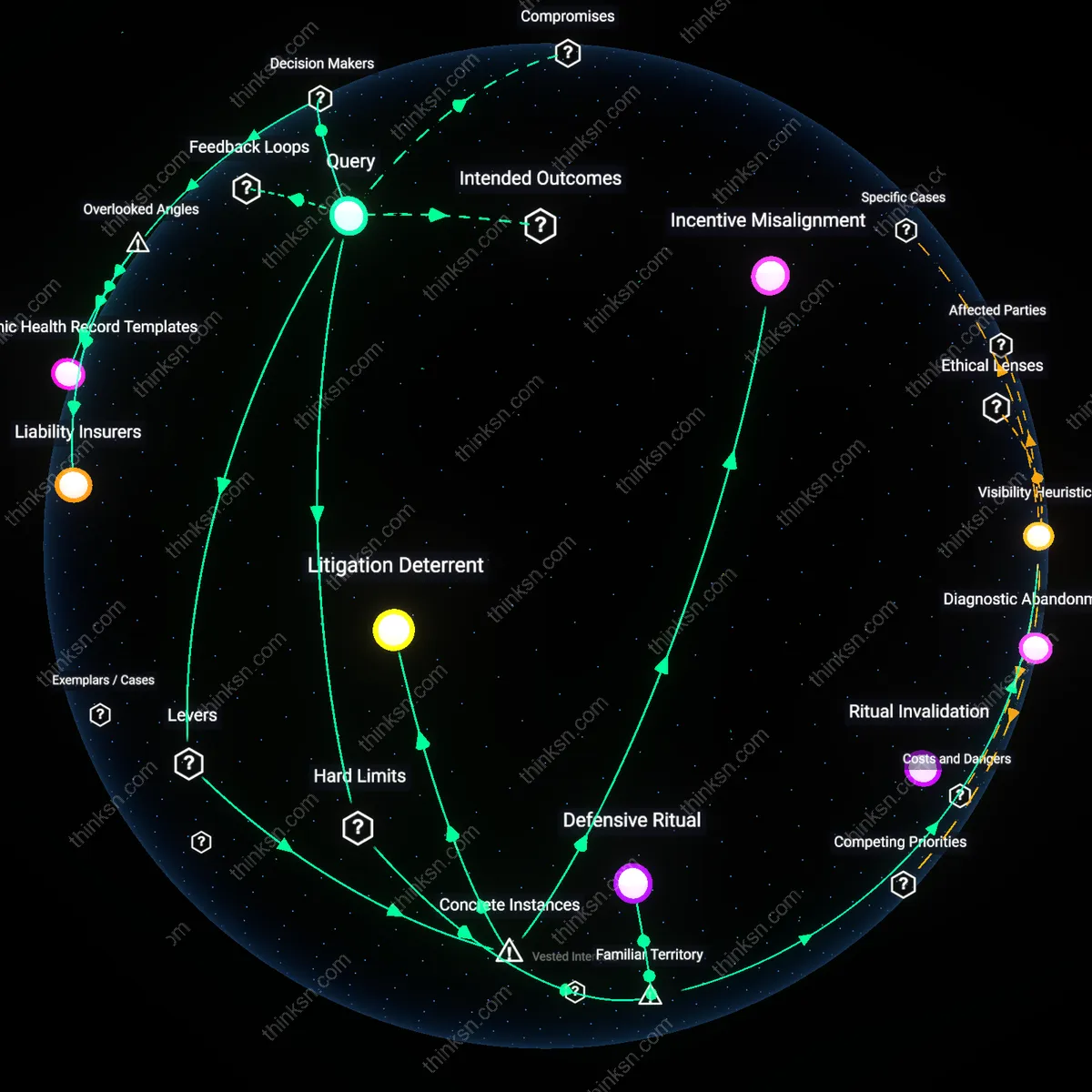
Defensive Ritual
Clinicians should recommend annual skin cancer checks for low-risk adults because failing to do so increases liability exposure in malpractice-prone settings, particularly in the United States where dermatology ranks high in litigation frequency. This practice persists not due to clinical efficacy but as a systemic behavioral adaptation among physicians who operate under the threat of patient lawsuits, especially in visible, image-rich domains like dermatology where a single missed lesion can be retrospectively highlighted. The non-obvious reality is that the ritual of annual checks functions less as preventive medicine and more as a documented performance of diligence—a procedural alibi embedded in electronic health records to satisfy legal expectations during discovery.
Visibility Heuristic
Clinicians should recommend annual skin cancer checks because skin is uniquely visible and culturally associated with immediate health perception, making dermatological neglect more cognitively salient to patients than asymptomatic internal risks. This visibility creates a social expectation of routine inspection, reinforced by public health campaigns and media portrayals of melanoma as a 'photogenic' disease, which pressures providers to conform to patient demands even when guidelines do not support routine screening. The underappreciated dynamic is that skin exams are retained not because of mortality outcomes but because they are tangible, observable acts that fulfill a symbolic role in the clinical encounter—patients feel seen when they are visually examined.
Guideline Arbitrage
Clinicians should recommend annual skin cancer checks because national guidelines from bodies like the USPSTF explicitly state insufficient evidence for or against screening in low-risk adults, creating a permissive regulatory gap that allows local practice norms and malpractice climates to dominate decision-making. In states with high litigation rates like Florida or Texas, this ambiguity is exploited as de facto permission to screen routinely, shielding providers from claims of deviation from standard care. The overlooked mechanism is that guideline uncertainty does not lead to restraint but instead enables institutional and individual risk-transfer strategies where screening becomes a normalized workaround to legal indeterminacy.
Litigation Deterrent
Clinicians should continue recommending annual skin checks for low-risk adults in jurisdictions like Texas, where tort reform following the 2003 Texas Medical Liability Insurance reforms reduced but did not eliminate liability pressure, demonstrating that malpractice concerns still shape clinical behavior even in reformed environments. The mechanism operates through physicians’ continued defensive practice patterns despite evidence showing no mortality benefit, revealing that medicolegal risk perception, not clinical outcome data, becomes the primary driver of recommendation adherence. This reveals the non-obvious dependence of guideline compliance on liability climate rather than scientific consensus.
Incentive Misalignment
In Australia’s privately billed primary care system, the prevalence of bulk-billed full-body photography visits increased after Medicare rebates were structured to reimburse lesion-by-lesion documentation rather than comprehensive risk assessment, making low-yield monitoring more profitable than clinical judgment. This dynamic shows how payment design, not clinical guidelines or legal fears, drives screening intensity—even in a country with strong evidence-based medicine traditions. The underrecognized leverage point is that financing mechanisms quietly override both medicolegal and scientific inputs in routine decision-making.
Liability Insurers
Clinicians continue annual skin cancer checks for low-risk adults primarily because medical malpractice insurers exert implicit pressure to maintain defensive practices, even absent mortality benefit. These insurers, though not direct healthcare providers, shape clinical guidelines through risk-pooling contracts and coverage stipulations that incentivize volume-based surveillance over evidence-based restraint, creating a misaligned payoff structure where omission is costlier than commission. This shifts clinical decision-making from epidemiological logic to actuarial logic—a dynamic rarely acknowledged in guideline deliberations, where insurers are absent from the room yet dictate risk tolerance.
Electronic Health Record Templates
Annual skin cancer checks are perpetuated in low-risk adults because preconfigured EHR templates automatically prompt total body skin exams during wellness visits, and clinicians who deactivate such prompts face higher cognitive workloads and documentation risk during audit cycles. These templates, designed by template managers at large EHR vendors (e.g., Epic, Cerner) under advisory input from specialty societies, encode outdated consensus standards into routine workflows, making non-recommendation the path of most friction. The hidden dependency is not clinician fear or patient expectation, but the default architecture of clinical software, which silently enforces pattern compliance through interaction design.