Chemotherapy: Comfort vs. Cost for Middle-Class Families?
Analysis reveals 8 key thematic connections.
Key Findings
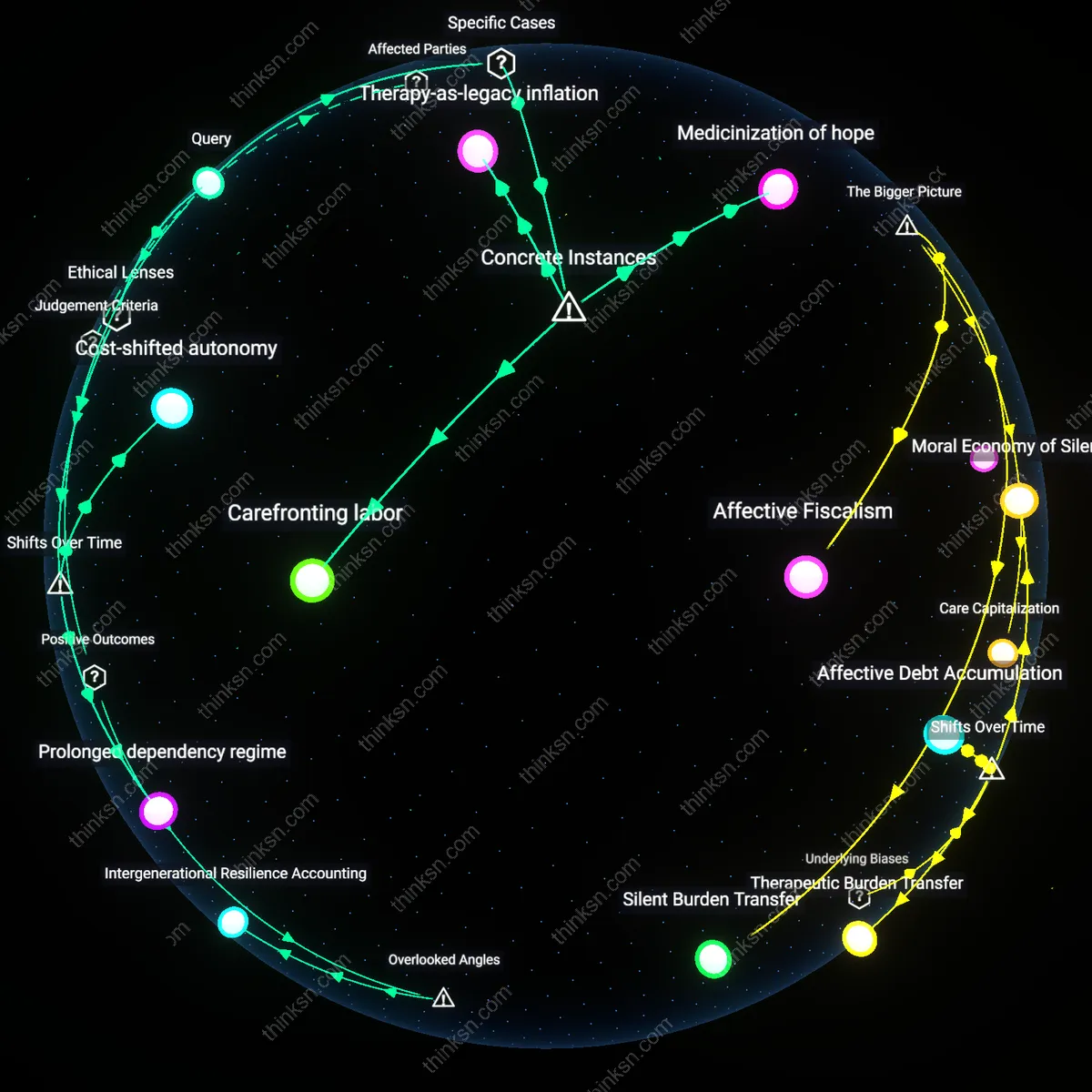
Intergenerational Resilience Accounting
Prioritize chemotherapy when it enables the terminally ill parent to personally transfer critical life narratives, practical skills, or emotional closure to their children, because these exchanges build enduring family resilience that offsets future psychological costs. Middle-class families often overlook this intangible asset formation during treatment decisions, focusing instead on immediate medical or financial metrics; yet the mechanism—transmission of identity-stabilizing knowledge during lucid phases of care—is a hidden dependency in long-term household well-being, altering the cost-benefit calculus by treating emotional continuity as preventative mental health infrastructure.
Somatic Trust Signaling
Administer aggressive chemotherapy when the parent explicitly ties their sense of being loved to the family’s willingness to endure sacrifice for their care, because in such cases, treatment continuation functions less as medical intervention than as a ritual of somatic trust that reaffirms relational bonds under duress. The overlooked mechanism here is not the tumor response but the symbolic calibration of familial loyalty—where the act of financial risk-taking becomes a nonverbal declaration of belonging—thereby stabilizing the emotional ecosystem of the family even if the body declines, a dynamic typically erased in clinical ethics frameworks focused on autonomy or utility.
Therapeutic citizenship
One should prioritize the emotional needs of the family by continuing aggressive chemotherapy, as the post-World War II expansion of American medical entitlements redefined access to extreme care as a moral expectation of middle-class belonging. The rise of Medicare (1965) and private insurance culture transformed terminal care from a domestic, palliative event into a technologically mediated public right, embedding chemotherapy not as medical strategy but as ritual performance of filial duty. This shift obscured the economic precarity such choices entail, making refusal feel like a betrayal of both kinship and national promise—revealing how mid-20th-century welfare-state aspirations inadvertently moralized financial risk in end-of-life decisions.
Cost-shifted autonomy
One should limit chemotherapy when its costs jeopardize the family’s solvency, because the 1980s neoliberal restructuring of U.S. healthcare transferred fiscal responsibility from institutions to individuals while preserving the rhetoric of patient choice. Managed care proliferation and hospital cost containment policies after the HMO Act (1973) and subsequent deregulation made treatment decisions inherently financial calculations, yet bioethics frameworks continued to emphasize autonomy without accounting for economic coercion. This contradiction—between sovereign decision-making and structural constraint—reveals how late-century market logics recast familial sacrifice as freedom, rendering invisible the coercion embedded in 'voluntary' medical debt.
Prolonged dependency regime
One should reject both emotional and financial absolutism by recognizing that the 21st-century biomedical industrial complex has redefined terminal illness as a phase of indefinite technological maintenance, not a finite passage. Since the 2000s, advances in oncology and critical care have aligned with pharmaceutical capital and hospital revenue models to extend treatment regimes far beyond meaningful prognosis, turning what was once a months-long decline into a years-long economic and affective drain. This transformation exposes a new category of social dependency—not of care, but of consumption—where familial love is monetized through continuous therapeutic intervention, normalizing financial ruin as the price of moral adequacy.
Carefronting labor
Prioritizing chemotherapy for a terminally ill parent despite financial strain reveals the hidden work of emotional caretaking performed by middle-class adult children to preserve familial dignity, as seen in the documented experiences of adult children managing parental cancer treatment under high-deductible insurance plans in suburban Ohio during the 2016 opioid and cost-of-care crisis; this emotional labor—distinct from medical or financial decisions—is asymmetrical, gendered, and frequently falls on daughters who absorb psychological stress to maintain the appearance of hope, exposing carefronting labor as a silent mechanism that sustains family cohesion at personal cost.
Therapy-as-legacy inflation
Continuing chemotherapy becomes a proxy for demonstrating filial devotion when future inheritance is uncertain, exemplified by the case of a Vietnamese-American family in Orange County, California, who sustained six months of palliative taxane treatments for a matriarch not because of survival expectancy but to fulfill cultural expectations of exhaustive care before death, revealing a dynamic where medical spending functions not as treatment but as ritual investment in legacy status, thereby inflating the symbolic value of therapy beyond clinical outcomes within diasporic communities facing intergenerational mobility pressures.
Medicinization of hope
In rural Maine, where access to hospice counseling is limited and religious narratives frame suffering as redemptive, families of terminal patients continue chemotherapy not for remission but as a sacramental act—evidenced by documented cases in Washington County clinics where patients exhausted savings on carboplatin regimens after oncologists confirmed futility—demonstrating how biomedical treatment becomes a ritualized vessel for hope when secular palliative frameworks are institutionally absent, turning hospitals into sites of spiritual maintenance rather than medical intervention.