Should Mental Health Coverage Riders Weigh More Than Denial Rates?
Analysis reveals 5 key thematic connections.
Key Findings
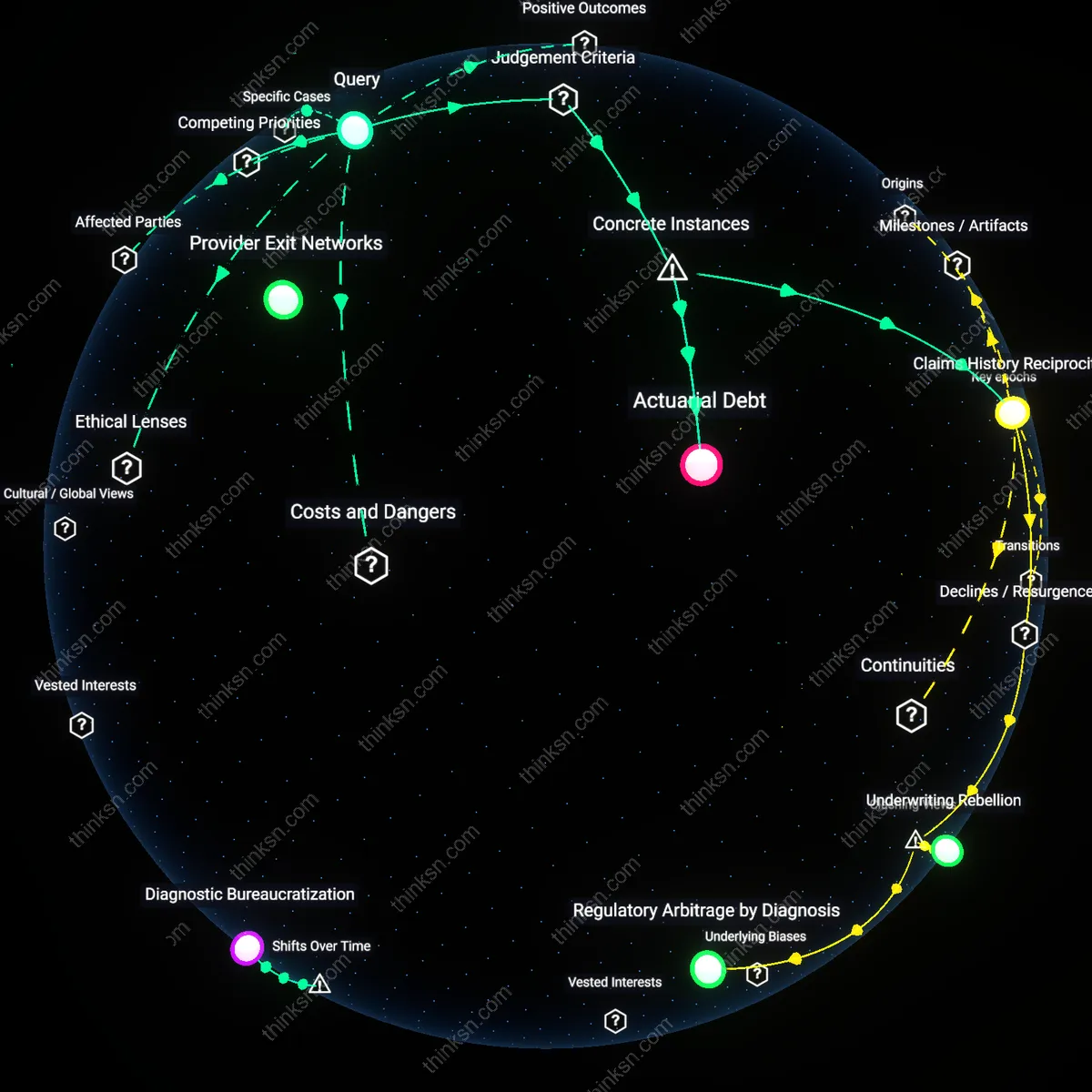
Claims History Reciprocity
Insurers should be required to justify new mental health riders through an audit of their prior claim denial rates, using regulators like the California Department of Insurance that have penalized carriers such as UnitedHealthcare for systemic denials under behavioral health mandates; this creates a feedback mechanism where past performance directly constrains future product expansion, revealing that market trust is not abstract but must be earned through consistent compliance—what appears as product innovation is often a regulatory second chance, which goes unnoticed when coverage is assessed in isolation from enforcement history.
Actuarial Debt
The value of mental health riders must be discounted by the accumulated actuarial debt from underfunded treatments during periods of non-compliance, as seen in the 2019 class-action settlement against Aetna for failing to provide mandated parity in coverage levels across medical and psychiatric care; this recalibration treats historical underpayment as a financial liability that distorts present pricing, exposing how risk models become complicit in inequity when past harms are excluded from cost-benefit analyses.
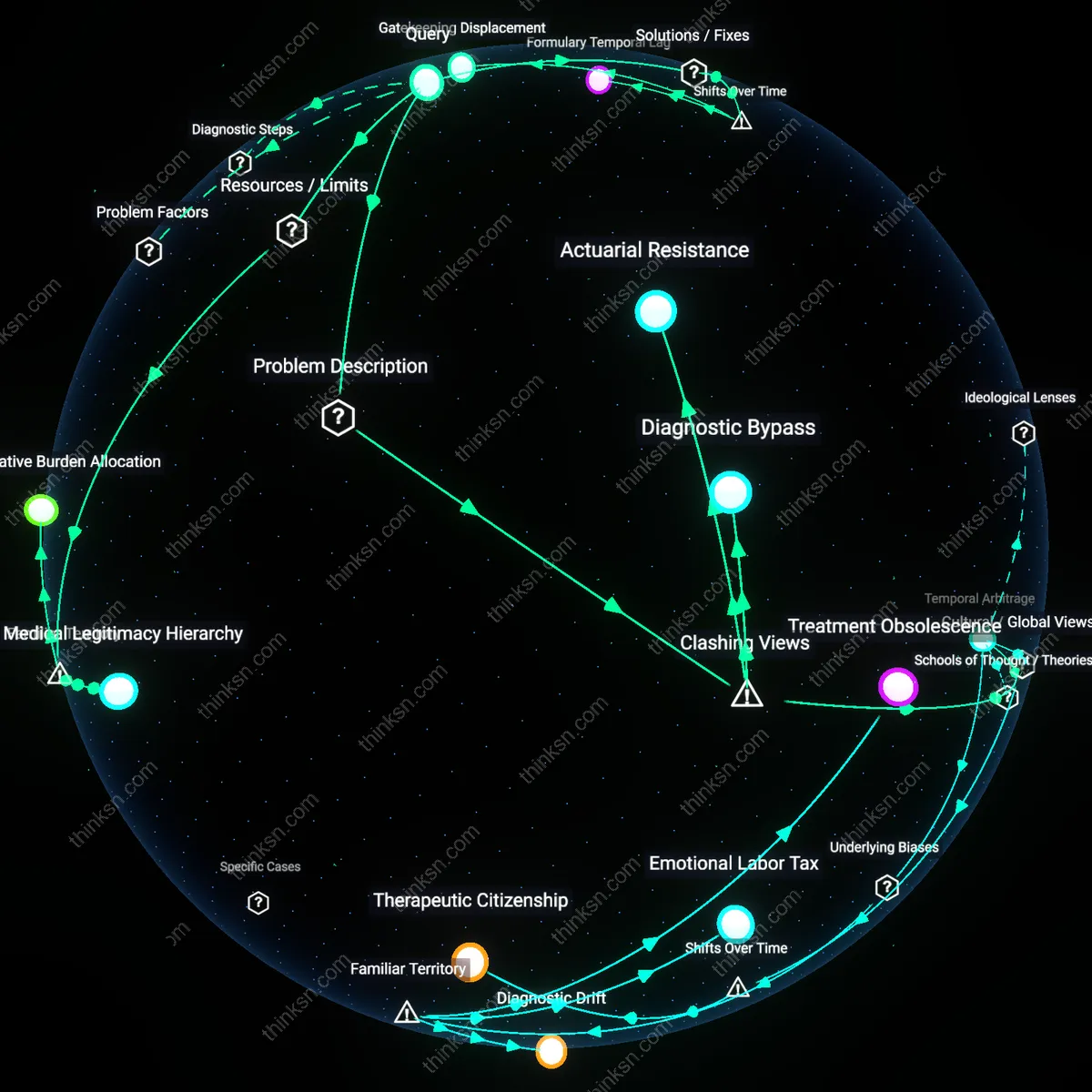
Diagnostic Gatekeeping
Mental health riders should be evaluated by who controls diagnostic entry points within provider networks, exemplified by the exclusion of trauma diagnoses in PTSD claims denied by Veterans Affairs-contracted insurers despite DSM-5 criteria, where gatekeeping operates through clinical discretion rather than cost; this surfaces a hidden hierarchy in which legitimacy, not affordability, is the primary barrier, challenging the assumption that expanded coverage automatically produces access.
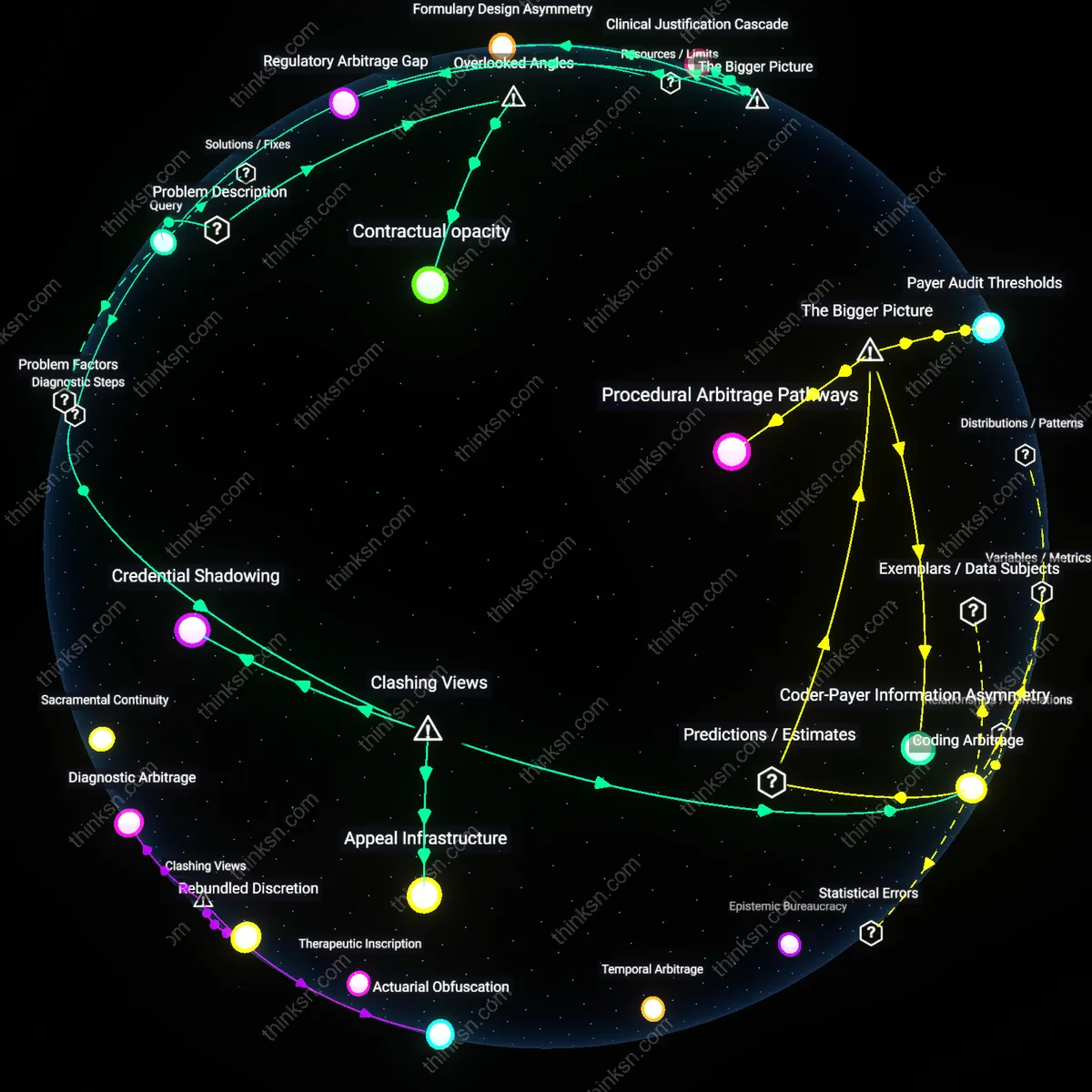
Claims Precedent Gradient
Insurers with a history of denying mental health claims redistribute risk toward future litigation costs rather than patient care, because accumulated denial patterns establish a de facto actuarial standard that skews reserves. Regulatory pressure to add riders is undermined by internal claims databases that silently reinforce underpayment norms, making coverage expansion a performative gesture unless denial thresholds are recalibrated. This exposes a hidden feedback loop where past behavior shapes future financial incentives more than policy mandates do—an effect rarely modeled in benefit valuation. The overlooked dynamic is how institutional memory encoded in claims history distorts the real value of new benefits.
Provider Exit Networks
In regions with concentrated insurer power, mental health coverage riders inadvertently accelerate clinician exodus from insurance panels because reimbursement rates fail to offset the administrative burden of expected denials. The non-obvious mechanism is that a history of denials trains providers to anticipate non-payment, making even 'covered' services functionally inaccessible—turning actuarial coverage into practical exclusion. This shifts the cost of care from insurers to patients via lost access, a dynamic absent in cost-benefit analyses that assume provider participation is static. The residual risk is not financial, but network fragmentation.