Charitable Donations or Out-of-Pocket: Weighing Tax Deductions vs Cash Flow
Analysis reveals 8 key thematic connections.
Key Findings
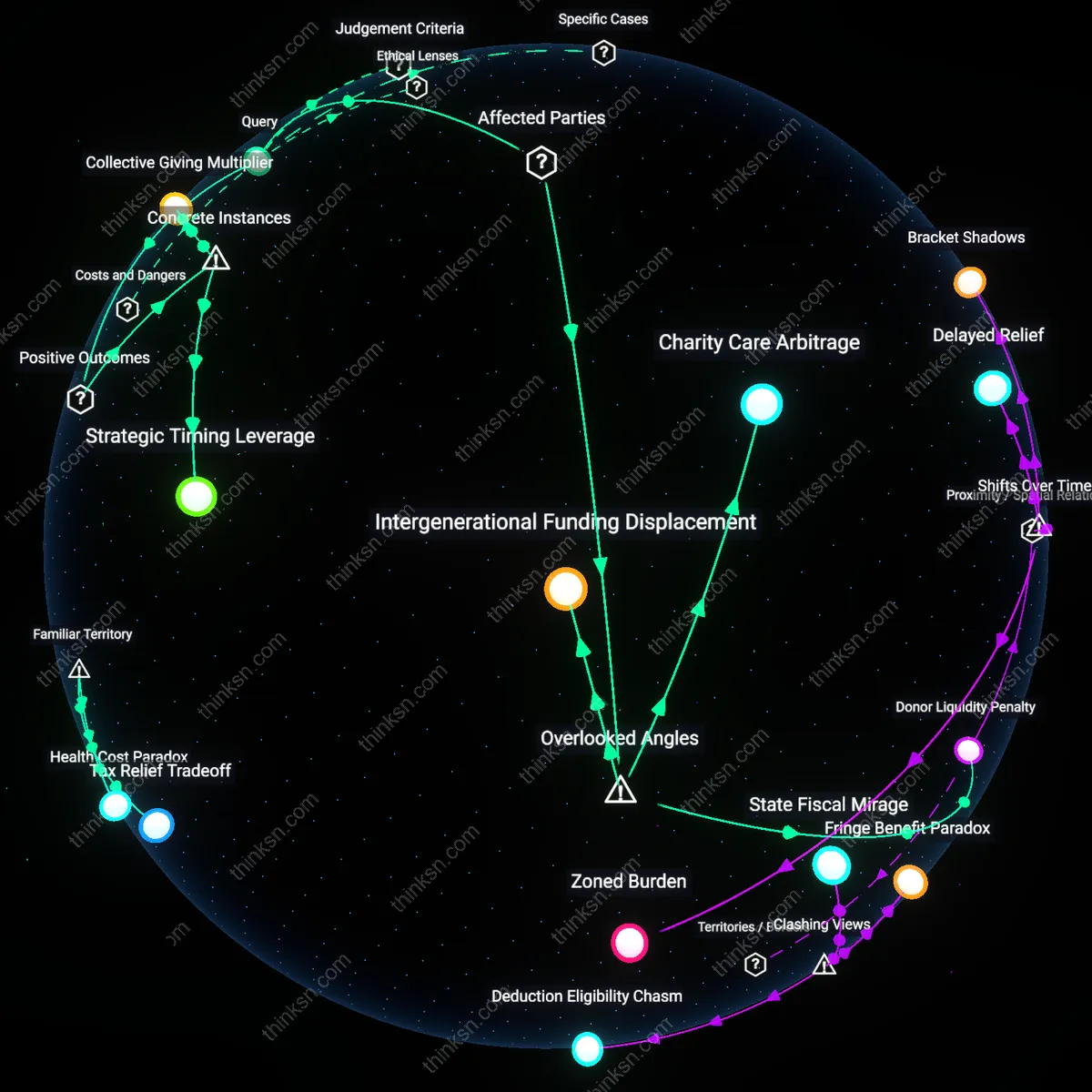
Donor Liquidity Penalty
Maximizing tax deductions for charitable medical donations intensifies short-term financial strain on middle-income donors who must frontload cash before reimbursement. Unlike high-wealth individuals with access to liquid reserves or tax-advantaged instruments, these donors face a temporal mismatch between out-of-pocket payments and tax return cycles—often twelve months apart—creating a de facto penalty for those utilizing deductions to subsidize care. This dynamic disproportionately affects salaried professionals such as teachers, nurses, and mid-level administrators who itemize deductions but lack staggered income or immediate liquidity, exposing a structural inequity in how tax policy rewards timing over intent. Most analyses assume tax savings neutralize out-of-pocket burden, but the reality of cash-flow lag reveals a hidden cost borne only by constrained earners—making tax optimization a privilege of liquidity.
Charity Care Arbitrage
Hospitals in states that have not expanded Medicaid selectively promote donation-based billing relief to channel indigent patients into charitable status while deferring uncompensated care costs to community foundations. By guiding low-income patients toward donor-designated medical payments—which are then tax-deductible—the hospital reduces its own bad debt burden while enabling tax savings for donors, but simultaneously reduces pressure to advocate for systemic coverage reform. This shifts moral responsibility from institutional actors to individuals, obscuring the role of hospital finance departments in reproducing financial precarity. The overlooked dynamic is that tax-deductible donations function as a shadow reimbursement stream for providers, enabling them to maintain profitability without expanding direct charity care—turning philanthropy into a fiscal buffer rather than a safety net.
Intergenerational Funding Displacement
Families directing retirement funds toward immediate medical donations for elderly relatives sacrifice long-term wealth preservation in exchange for short-term tax benefits, effectively displacing future bequests onto younger generations. When adult children use IRA distributions or 401(k) withdrawals to finance parents’ care and claim deductions, they deplete tax-deferred assets that would otherwise pass to heirs, converting intergenerational wealth into time-limited fiscal relief. The IRS does not distinguish between charitable donations for strangers versus kin, creating a perverse incentive to treat family care as philanthropy—blurring ethical boundaries and distorting estate planning. This hidden trade-off reveals how tax policy inadvertently penalizes familial responsibility by making caregiving financially rational only through charitable frameworks, thus commodifying intimate familial obligation.
Strategic Timing Leverage
Donors in high-income years can maximize tax relief by concentrating charitable medical contributions during periods of elevated taxable income, as demonstrated by donors to the Mayo Clinic's patient assistance fund who coordinate large gifts in years of bonus payouts or capital gains realizations. This intertemporal alignment of giving with income spikes converts otherwise burdensome tax liabilities into immediate care funding, exploiting marginal tax rate differentials to amplify the effective value of each donated dollar—a mechanism underappreciated because it treats philanthropy not as a static expense but as a dynamic financial instrument tied to personal fiscal cycles.
Institutional Bridge Financing
Massachusetts General Hospital’s partnership with the Boston Medical Gift of Life program enables donors to pledge medical expense payments that are immediately disbursed to patients while tax deductions are secured in the same fiscal year, even if full cash settlement occurs later. By decoupling the timing of tax documentation from out-of-pocket reimbursement through institutional credit backing, the hospital transforms liquidity constraints into structured philanthropic leverage—an arrangement rarely seen outside major academic medical centers that reveals how trusted intermediaries can function as fiscal shock absorbers.
Collective Giving Multiplier
The Houston Methodist Employee Giving Campaign aggregates thousands of small employee donations toward employee medical hardship cases, allowing participants to pool contributions and exceed the standard deduction threshold, thereby unlocking itemized tax benefits that individuals alone couldn’t access. This collective action converts otherwise non-deductible personal giving into tax-efficient charitable deduction pools, demonstrating how workplace-enabled solidarity networks generate fiscal efficiency through scale—an insight obscured by the usual focus on individual donor behavior in tax planning discourse.
Tax Relief Tradeoff
One must delay charitable medical deductions until tax filing to gain monetary benefit, forcing patients to absorb immediate cash burdens without institutional support. This temporal mismatch between out-of-pocket payments and tax refunds institutionalizes financial strain for middle-income households managing chronic illness, especially under U.S. healthcare's cost-shifting regime. The non-obvious reality is that the tax code incentivizes donation timing over health outcomes, reframing generosity as a liquidity-dependent choice rather than a moral impulse.
Health Cost Paradox
Claiming medical donations as deductions presumes surplus income, yet the same conditions that necessitate large medical outlays—job loss, long-term treatment, underinsurance—routinely deplete that surplus before tax season arrives. This contradiction reveals how tax policy treats medical charity as voluntary when it’s often coerced by billing pressure, especially in states with aggressive collections regimes like Texas or Florida. The unspoken norm is that relief follows wealth, not need—making equity the casualty of eligibility.