Could Unforeseen Inflation Drain Your 20-Year Retirement Savings?
Analysis reveals 12 key thematic connections.
Key Findings
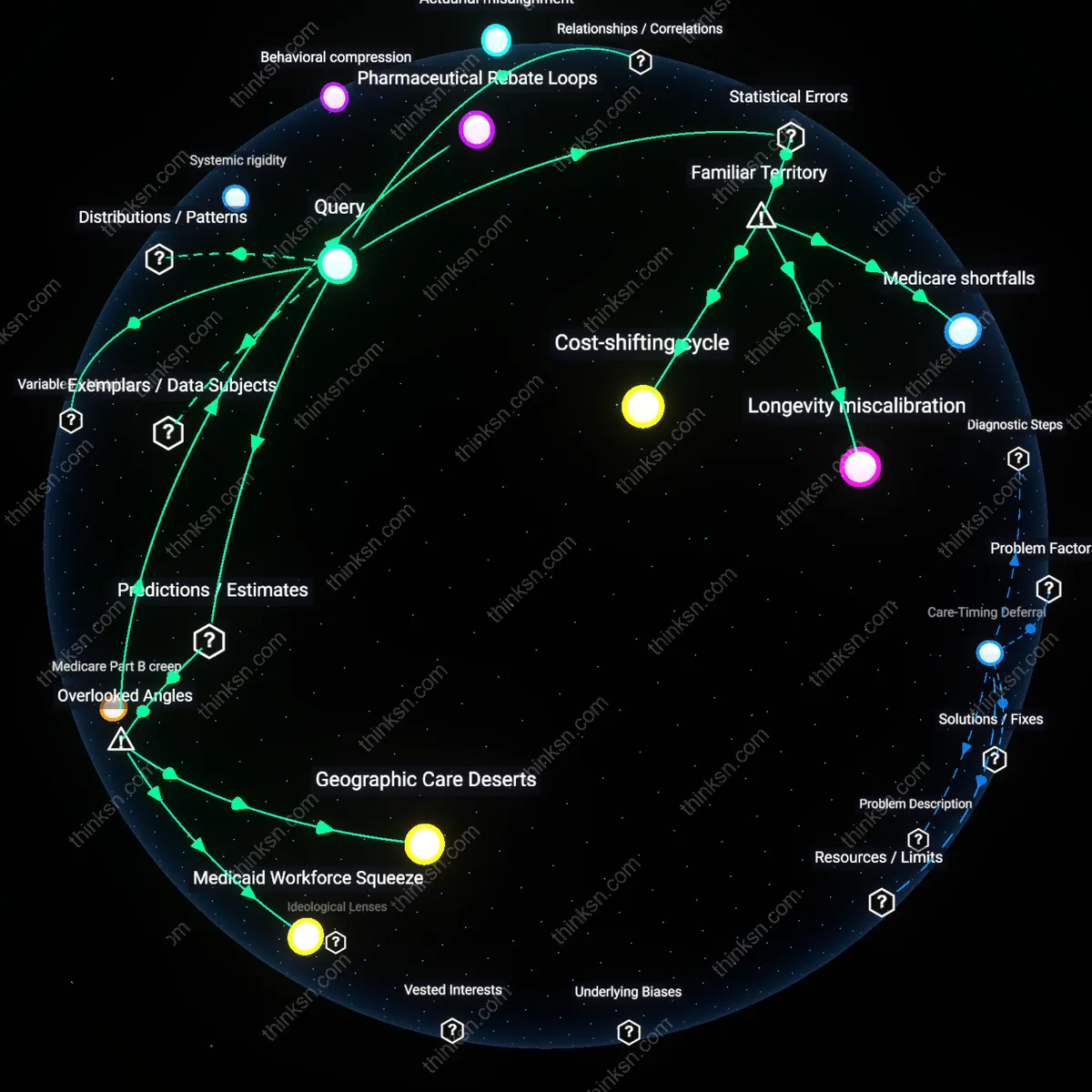
Medicare Part B creep
Healthcare inflation in the U.S. forces retirees to withdraw more than 5% annually because Medicare Part B premiums are tied to medical inflation and income, causing premium spikes that consume an increasing share of Social Security income—evident in 2023 when high-income retirees saw their Part B premiums rise by nearly 15% year-over-year, effectively forcing higher withdrawals from retirement accounts to cover fixed costs. This dynamic operates through the income-related monthly adjustment amount (IRMAA) surcharge, which scales with both inflation and past income, creating a feedback loop where medical costs grow faster than retirement income. The underappreciated mechanism is that retirees do not need to use more healthcare services to face higher withdrawals—the cost shift occurs automatically via premium indexing.
Long-term care overhang
Retirees in Japan withdrew over 5% annually during the 2010s due to rising out-of-pocket costs for non-covered long-term care services, despite national health insurance covering basic medical care—this occurred as Japan’s rapidly aging population overwhelmed public LTC capacity, forcing families to privately fund assisted living and nursing care, often depleting retirement savings prematurely. The dynamic operates through the mismatch between public insurance coverage and actual care needs in super-aged societies, where functional dependence increases faster than policy adaptation. The non-obvious insight is that even with universal healthcare, retirees face effective inflation in care access, not just prices, which triggers accelerated withdrawals.
Provider consolidation drain
In Florida between 2015 and 2020, retirees experienced effective healthcare inflation above broader CPI due to hospital consolidation under chains like AdventHealth, which increased prices for outpatient services by up to 30% post-acquisition, leading retirees on fixed incomes to exceed 5% withdrawal rates to maintain access. This operates through reduced price competition in local healthcare markets, where monopolistic providers shift costs to fee-for-service retirees without insurance bargaining power. The underappreciated factor is that healthcare inflation is not systemic or macro in nature—it can be geographically hyper-local and institutionally driven, making it invisible to national indices but devastating at the household level.
Systemic rigidity
Healthcare inflation is negatively correlated with retirement withdrawal rates because rising medical costs suppress discretionary spending, forcing retirees to absorb shocks internally rather than increase withdrawals—this occurs as fixed-income portfolios and pension structures resist liquidity adjustments, binding retirees to withdrawal caps despite cost pressures. The mechanism operates through the mismatch between inflexible retirement income systems and variable healthcare cost trajectories, particularly in Medicare-attached cohorts in the U.S. South, where out-of-pocket growth exceeds national averages. This insight challenges the dominant narrative that cost increases directly necessitate higher withdrawals, revealing instead a systemic failure to adapt that constrains behavior.
Behavioral compression
Higher healthcare inflation correlates with lower-than-expected withdrawal rates because retirees reinterpret financial norms under sustained cost pressure, recalibrating lifestyle expectations downward rather than breach symbolic thresholds like the 4% rule. This dynamic plays out through cognitive anchoring in financial planning communities, especially among middle-income retirees in suburban Arizona and Florida who prioritize rule adherence over consumption maintenance. The phenomenon undermines the intuitive claim that inflation forces higher draws, exposing a latent behavioral floor beneath which retirees refuse to go, even at the cost of health service deferral.
Actuarial misalignment
The likelihood of exceeding 5% withdrawals rises not with realized healthcare inflation, but with its mispricing in annuity and pension models, where insurers systematically underestimate late-life cost gradients, creating a lagged funding gap that retirees must resolve through abrupt withdrawal increases. This occurs primarily in private sector defined-contribution plans managed by firms like Fidelity and Vanguard, where projection models smooth medical cost curves, decoupling them from regional price spikes such as those in post-2018 telehealth deserts. This contradicts the assumption that personal spending responses track actual inflation, revealing instead a structural delay that forces steeper, more concentrated withdrawals later in retirement.
Medicare shortfalls
Healthcare inflation will compel retirees to exceed 5% withdrawal rates because Medicare premiums, deductibles, and uncovered services are rising faster than general inflation and fixed incomes. As medical prices grow at approximately 4–6% annually—outpacing Social Security COLAs—retirees on traditional Medicare face widening gaps in out-of-pocket liability, especially for supplemental coverage and long-term care. This mechanism forces drawdown acceleration not through voluntary spending but systemic underinsurance, a risk most retirees underestimate despite widespread familiarity with Medicare’s existence. The non-obvious insight is that Medicare operates as a cost-deferral system, not a cost-elimination one, making its perceived reliability a source of financial vulnerability.
Longevity miscalibration
Retirees will likely exceed 5% withdrawals because public perception of life expectancy lags behind demographic reality, compressing the assumed retirement window below 20 years when population-level data increasingly exceeds it. Many retirement plans rely on retiring at 65 and lasting only to 80 or 82, but U.S. life expectancy for healthy 65-year-olds now averages 85+, with higher longevity among wealthier, better-insured cohorts who also have higher healthcare utilization. This mismatch propagates through financial planning models that embed optimistic survival assumptions, making 5% rules appear sustainable when actuaries know they fail under extended lifespan scenarios with rising medical costs. The underappreciated point is that longevity, though intuitively associated with retirement, is mentally discounted in withdrawal planning, treated as a distant risk rather than a near-certain cost driver.
Cost-shifting cycle
Healthcare inflation will push withdrawal rates above 5% because employer and government cost-containment strategies systematically transfer expense risk onto retirees through higher deductibles, narrower networks, and reduced retiree health benefits. Between 2005 and 2023, the share of firms offering retiree medical coverage dropped from 34% to under 15%, pushing retirees into individual markets where premiums and drug prices fluctuate with minimal regulation. This shift operates through institutional retreat from post-employment liability, amplifying exposure just as healthcare intensity increases with age. Though people commonly associate retirement healthcare with personal responsibility, few recognize how formally, systematically, and predictably institutional disengagement has recalibrated financial risk onto individuals.
Pharmaceutical Rebate Loops
Healthcare inflation will likely force retirees to withdraw more than 5% annually because opaque pharmaceutical rebate agreements between insurers, pharmacy benefit managers (PBMs), and drug manufacturers systematically inflate list prices, shifting cost volatility onto beneficiaries using Medicare Part D or supplemental plans; this mechanism—hidden from public and retiree awareness—creates a ratcheting effect where nominal price increases, even without real therapeutic innovation, force higher out-of-pocket costs during late-life prescription spikes, a dynamic rarely captured in standard retirement withdrawal models that assume linear drug cost growth.
Geographic Care Deserts
Retirees in rural counties across the Mississippi Delta and northern Appalachia will disproportionately exceed 5% withdrawal rates because hospital closures and specialist shortages have created care deserts that force medically necessitated long-distance treatment travel, converting inflation into logistical and ancillary costs—hotels, transport, caretaker time—that compound the official medical CPI; this spatial tax on access is omitted from national-average inflation models but materially impacts outlays for 18% of retirees who live outside metropolitan service hubs.
Medicaid Workforce Squeeze
The reliance of home- and community-based senior care on Medicaid-funded aides creates a latent inflation multiplier, as persistently low reimbursement rates produce chronic turnover and labor shortages, compelling private-pay retirees to offer 25–40% wage premiums to secure equivalent services—this parallel wage inflation in the informal care economy, driven by systemic public underfunding, leaks into retiree budgets in ways unrecorded by formal healthcare CPI indices, which do not track privately negotiated hourly rates for personal care.