Raising Deductibles: Lower Health Costs or Risky Business?
Analysis reveals 6 key thematic connections.
Key Findings
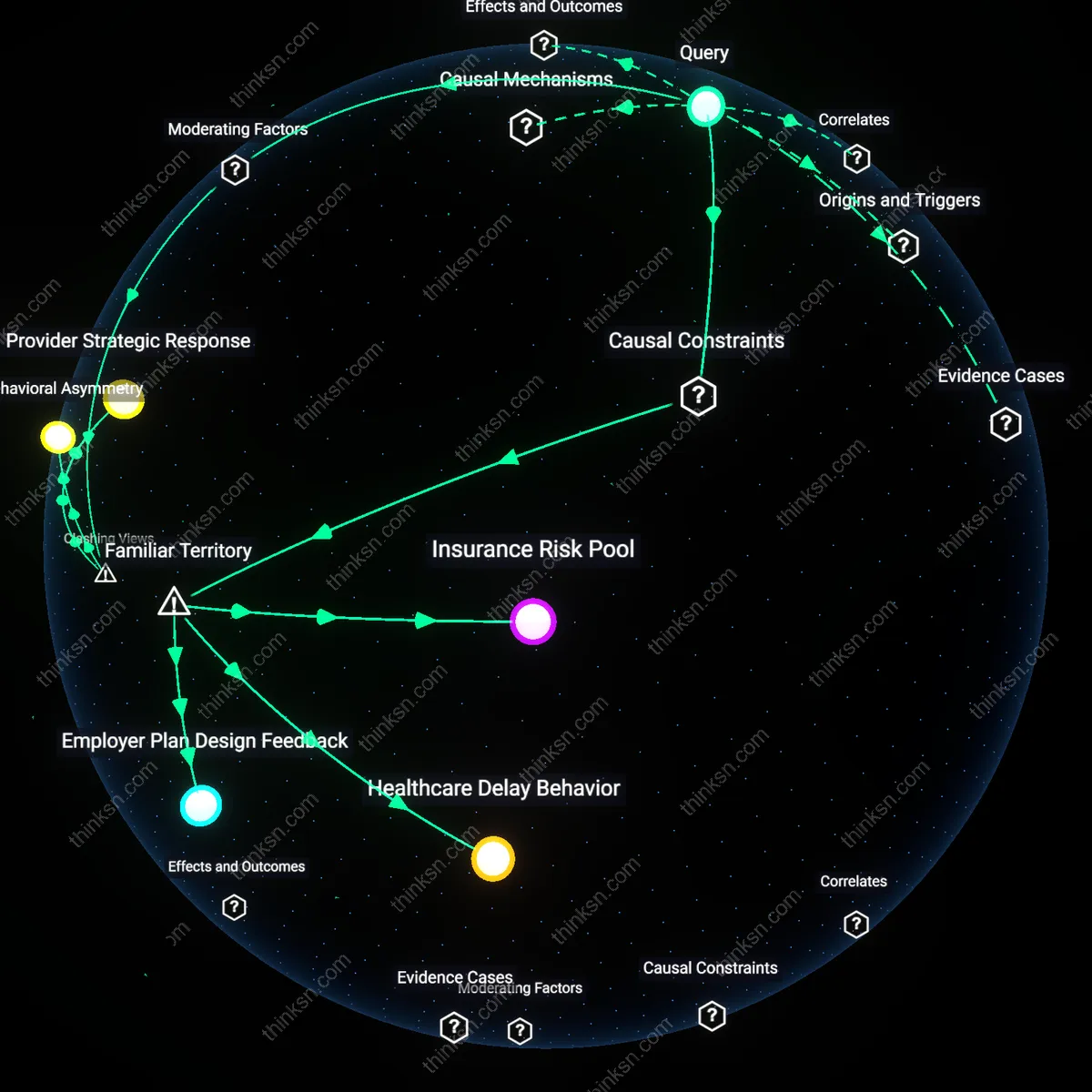
Behavioral Asymmetry
Raising the out-of-pocket maximum on a high-deductible health plan would increase total healthcare spending for a middle-aged person with moderate health risk. Insurers and employers, not patients, are the primary beneficiaries of cost-conscious behavior under high-deductible plans; when the out-of-pocket maximum rises, middle-aged enrollees—facing uncertain but non-catastrophic health trajectories—perceive greater financial exposure late in the plan year, which triggers anxiety-driven utilization such as early specialist referrals or diagnostic imaging to 'front-load' care before potential crises, a response documented in behavioral studies of plan transitions at firms like UnitedHealthcare. This mechanism contravenes the standard assumption that higher cost-sharing uniformly depresses spending, revealing that risk perception, not just price signals, governs healthcare decisions when financial ceilings feel unstable.
Provider Strategic Response
Raising the out-of-pocket maximum would not reduce spending because it weakens providers' incentives to offer discounts or bundled pricing to high-deductible plan patients. Clinics in competitive markets like orthopedics or gastroenterology—where cash flow urgency drives pricing flexibility—routinely adjust billed charges downward when patients face predictable cost ceilings; a higher out-of-pocket maximum disrupts this coordination by extending the period of full-price liability, making providers less willing to negotiate, as observed in billing patterns from Colorado’s high-deductible cohort under the Affordable Care Act. The dominant narrative assumes patient cost-sharing alone drives spending restraint, but this ignores how provider pricing tactics co-evolve with plan design, revealing that financial pressure redistribution can entrench, rather than erode, high list prices.
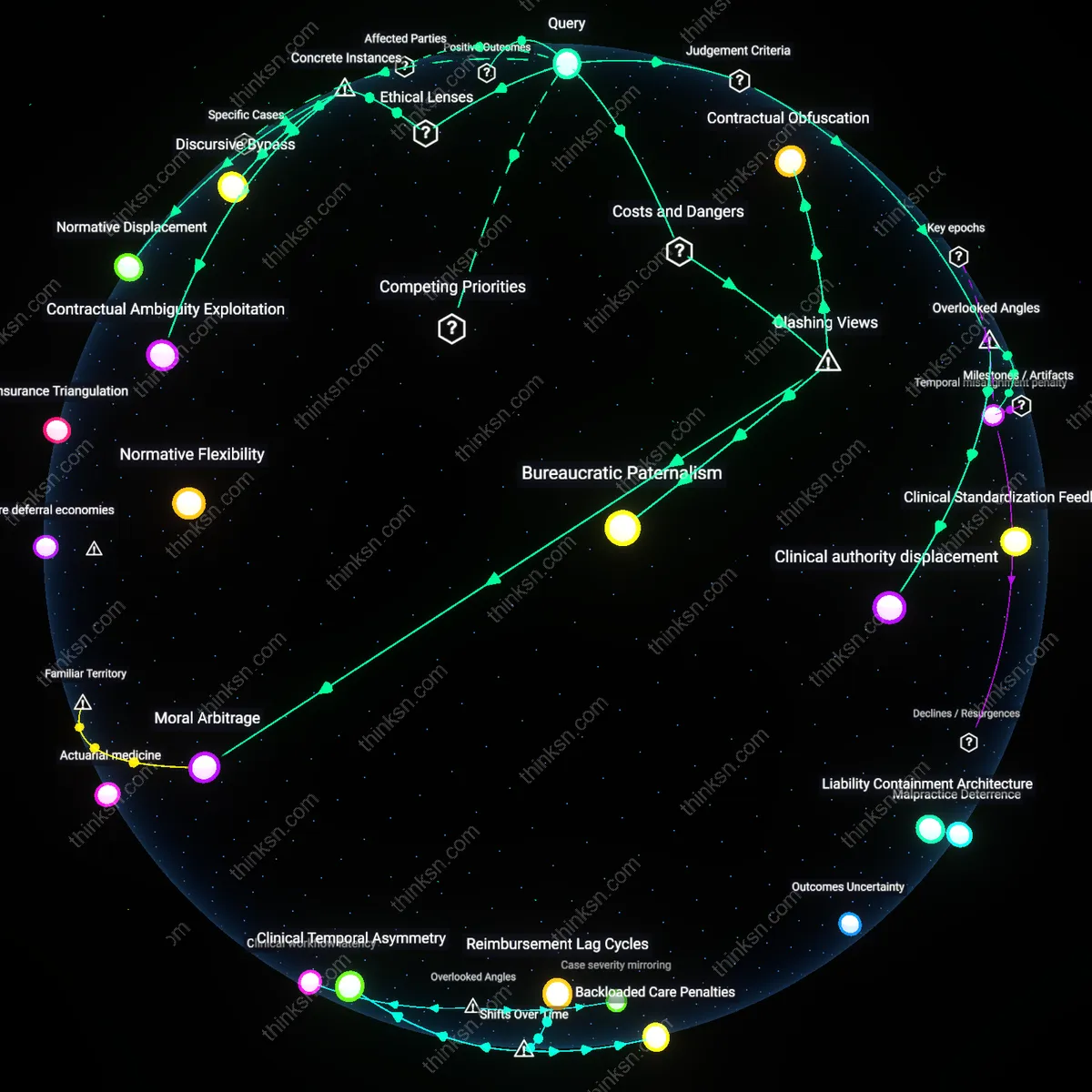
Temporal Misalignment
A higher out-of-pocket maximum increases total spending by decoupling financial consequence from clinical decision-making rhythm. For a 52-year-old software engineer with controlled hypertension enrolled in a Kaiser Permanente HDHP, the annual reset of the deductible means most cost-conscious behavior clusters in Q1 and Q2, but the elevated out-of-pocket cap extends financial vulnerability into Q3 and Q4 without reinforcing earlier incentives, causing inertia in utilization patterns despite accumulated spending—this temporal gap, confirmed in CMS claims lag analyses, undermines the behavioral linkage between cost exposure and restraint. The standard model presumes linear responsiveness to cost-sharing, yet when financial thresholds are distant or ambiguous, decision fatigue and calendar drift mute their effect, exposing a flaw in static economic models of consumer-directed health plans.
Insurance Risk Pool
Raising the out-of-pocket maximum increases expected spending for a middle-aged person with moderate health risk because individuals in high-deductible plans rely on the insurance risk pool being large and stable enough to absorb rare but costly events; when cost-sharing caps rise, healthier enrollees are more likely to exit the pool, reducing cross-subsidization and forcing those who remain—especially those with predictable mid-tier utilization—to bear higher effective prices due to destabilized premiums. This mechanism operates through adverse selection dynamics in the individual insurance market, particularly in state-based exchanges where plan choice is limited and elasticity of enrollment is high. What's underappreciated is that the out-of-pocket maximum isn’t just a personal spending cap—it functions as a signal of inclusion in a shared risk community, and weakening it erodes the very collectivity that makes insurance viable.
Healthcare Delay Behavior
Raising the out-of-pocket maximum increases total healthcare spending for a moderately at-risk middle-aged person because higher cost-sharing triggers delayed or forgone care, particularly for chronic condition management, leading to costlier acute episodes later; this occurs through price-sensitive behavioral responses in outpatient settings like primary care clinics and pharmacy refill systems, where individuals weigh immediate affordability against long-term health consequences. The system responsible is the price-transparent, consumer-directed health spending model that high-deductible plans were designed to promote. What’s counterintuitive in familiar discussions of deductibles is that reducing apparent costs at the point of care often increases total system spending—not because people overuse care, but because they underuse it until crises emerge.
Employer Plan Design Feedback
Raising the out-of-pocket maximum reduces total healthcare spending for a middle-aged person with moderate health risk only if employers simultaneously adjust wage compensation or health account contributions to offset the added financial exposure, which rarely happens in mid-tier private sector firms where benefits are standardized and HR departments operate under fixed budget envelopes; this dynamic plays out through collective bargaining inertia and payroll cost control strategies in industries like manufacturing or regional retail. The non-obvious insight is that while higher out-of-pocket limits may theoretically constrain spending, their real-world effect depends on whether households actually experience income flexibility to manage risk—a condition that’s structurally absent in the majority of employer-sponsored insurance arrangements, rendering the cost cap increase functionally regressive.