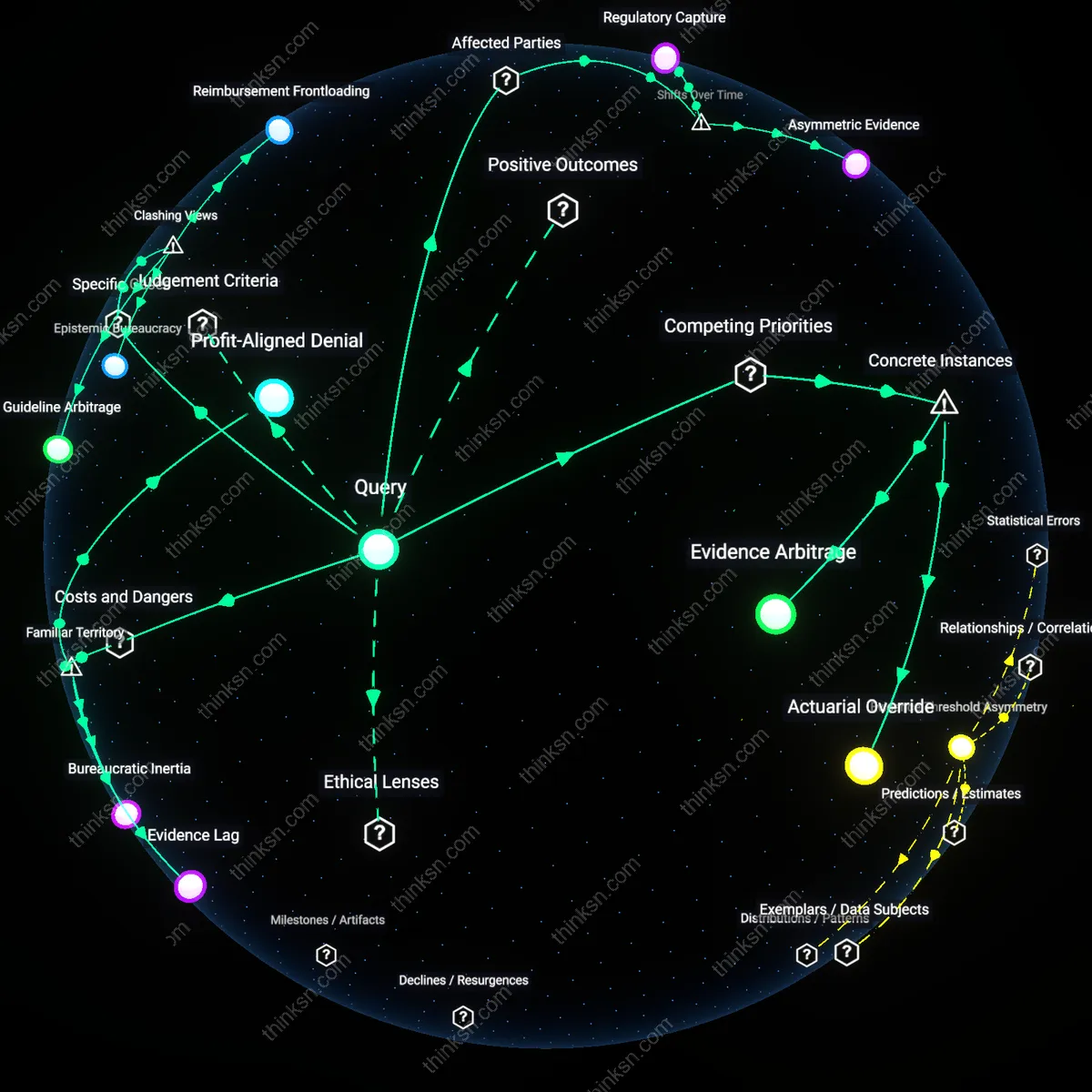
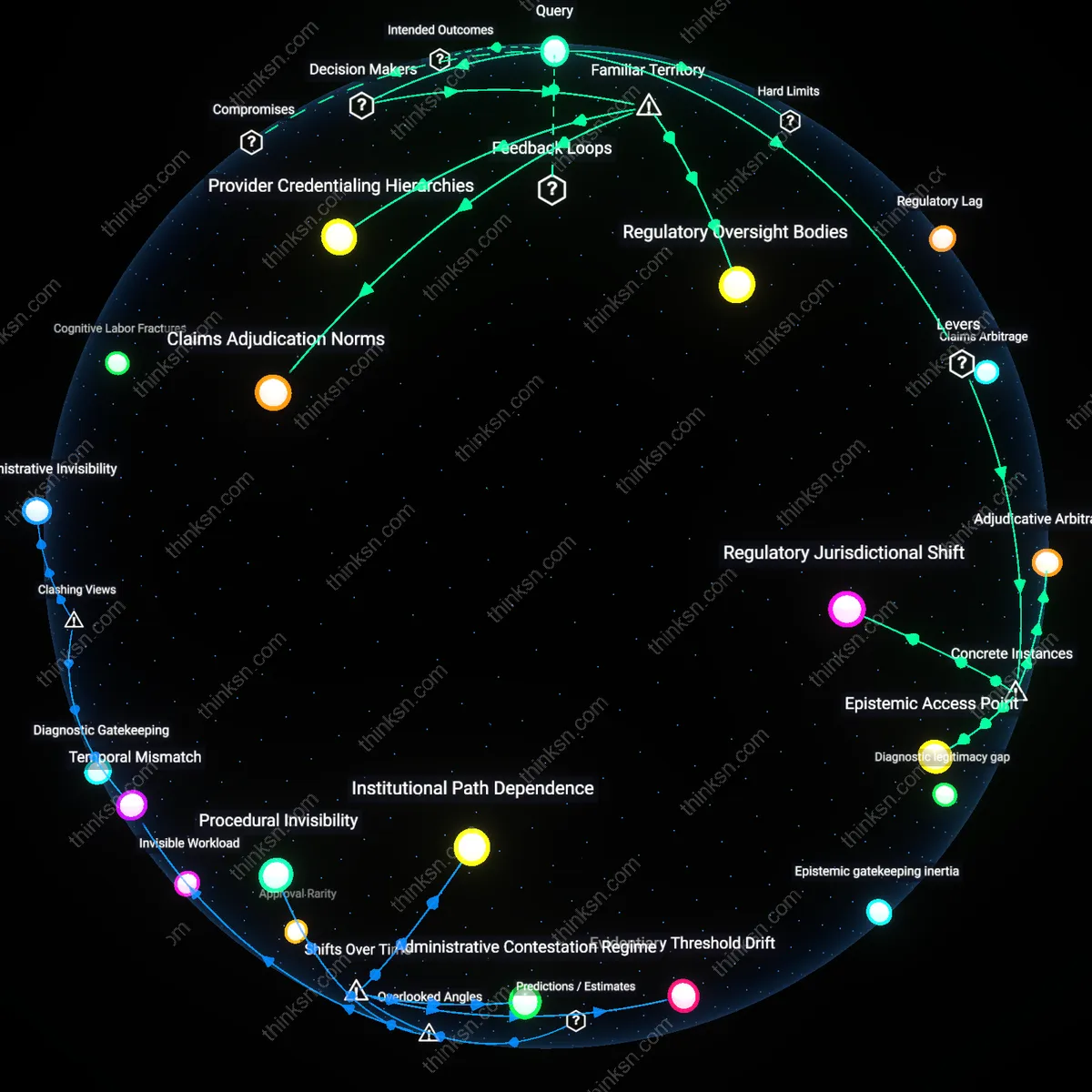
Do Insurer Guidelines Hide Cost Agenda Behind Best Practice?
Analysis reveals 11 key thematic connections.
Key Findings
Regulatory Capture
Insurers' clinical guidelines increasingly reflect cost-containment logics because the late 1990s shift toward managed care empowered insurance actuaries—rather than clinicians—to lead guideline development, embedding financial risk models into medical necessity criteria; this reconfiguration transferred clinical authority from medical institutions to insurance underwriting departments, making denial appeals subject to actuarial justifications disguised as medical standards. The non-obvious consequence of this transition was not reduced care quality per se, but the systemic substitution of peer-reviewed treatment timelines with utilization thresholds calibrated to premium stability, particularly evident in mental health and chronic pain management where subjective metrics dominate.
Epistemic Bureaucratization
Clinical guidelines now prioritize procedural defensibility over therapeutic innovation because the 2000s expansion of external review mandates forced insurers to standardize denial rationales in anticipation of legal contestation, causing medical policies to evolve into audit-proof administrative artifacts rather than living interpretations of science; this shift privileged static, citation-heavy documentation frameworks that favor retrospective validation over frontline clinical judgment. The underappreciated effect has been a freezing of guideline revision cycles, as legal risk incentivizes adherence to outdated but legally settled criteria—evident in delayed adoption of CAR-T therapy coverage despite FDA approval.
Asymmetric Evidence
Insurers selectively operationalize best practices by leveraging their post-2010 dominance in real-world data collection to redefine 'evidence' around cost-avoidant outcomes, such as hospitalization avoidance rather than disease remission, thereby constructing internal clinical algorithms that favor generic or earlier-line treatments with lower price points; this data asymmetry allows insurers to present denials as evidence-based while suppressing longitudinal efficacy data that contradicts cost targets. The critical but invisible shift occurred when private insurers began funding their own comparative effectiveness research, positioning themselves as epistemic authorities in coverage decisions—exemplified by UnitedHealth’s Optum Evidence Group shaping prior authorization rules for Medicare Advantage plans.
Profit-Aligned Denial
Insurers deny appeals because clinical guidelines are calibrated to prioritize financial thresholds over clinical efficacy. Actuarial teams and medical directors at major insurers like UnitedHealthcare and Aetna routinely adjust guideline stringency in real time based on cost-impact modeling, directly linking denial rates to budget forecasts. This mechanism embeds economic logic beneath a veneer of clinical objectivity, making the appeal process a managed cost-control valve rather than a medical review—what feels like a medical decision becomes a balance-sheet enforcement point masked as prudence.
Evidence Lag
Insurers rely on outdated clinical benchmarks because adopting new standards triggers coverage expansion and immediate cost inflation. Guidelines from bodies like NCCN or ACOG often take 18–36 months to be incorporated into payer policies, during which time newly established treatments—like CAR-T for certain cancers or GLP-1 agonists for obesity—are systematically denied despite peer-reviewed validation. The delay is not accidental but structurally advantageous, creating a compliance-safe window where denials are shielded by the appearance of conservatism, even as patients face preventable deterioration.
Bureaucratic Inertia
Insurance medical policies resist updates because the internal approval process requires consensus across legal, finance, and underwriting departments, not just clinical staff. This multi-departmental gatekeeping means that even when medical directors recognize a practice as standard of care, implementation stalls without financial sign-off. The resulting inertia transforms guidelines into static artifacts that weaponize procedural legitimacy against innovation, allowing insurers to cite 'policy compliance' as a final defense in appeals—turning administrative rigidity into a deniability scaffold.
Actuarial Override
California's 2021 enforcement of SB 188 revealed that insulin rationing appeals were denied despite ADA standards because actuaries embedded cost ceilings into coverage algorithms, which forced clinicians to justify care beyond predefined expenditure bands, demonstrating that underwriting models actively recalibrate medical necessity when treatments exceed actuarial thresholds. This mechanism operates through embedded financial triggers in electronic health record systems linked to preauthorization databases, where therapeutic appropriateness is downgraded if population-level cost projections exceed risk pools, making cost containment structurally prior to adherence to evolving clinical consensus. The non-obvious insight is that denial is not always retrospective or punitive, but often algorithmically anticipatory — built into real-time decision architecture.
Evidence Arbitrage
During 2015 Medicaid non-coverage decisions in Mississippi for hepatitis C antivirals like sofosbuvir, state panels accepted insurer-backed ICER analyses that prioritized trial data over population health outcomes, thus classifying curative regimens as 'low value' due to high upfront cost, even as post-treatment reinfection rates proved negligible in managed cohorts. This functions through the institutional substitution of short-term pharmacoeconomic modeling for longitudinal epidemiological evidence, allowing payers to treat cost-effectiveness ratios as fixed scientific truths rather than contingent valuations. The buried dynamic is that insurers reframe clinical evidence hierarchies—promoting certain types of data (RCTs, QALYs) while marginalizing others (real-world durability, transmission reduction)—to manufacture scientific uncertainty where clinical consensus exists.
Guideline Arbitrage
Insurers exploit ambiguities in evidence-based medicine by selectively adopting clinical guidelines that prioritize cost-containment metrics over outcomes, as seen in UnitedHealthcare’s restriction of CAR-T cell therapy for late-stage cancer patients despite FDA approval and NCCN endorsement, where their internal utilization review committees override real-time oncology consensus using retrofitted 'value frameworks' tied to drug price rather than survival benefit—revealing a system in which clinical authority is subordinated to actuarial logic, not corrupted outright but structurally redirected to delay or dilute access under the guise of rigor.
Epistemic Bureaucracy
Medical policy units at insurers like Aetna and Cigna systematically reframe clinical innovation as 'unproven' by demanding impractical levels of site-specific evidence for established treatments, such as when appeals for robotic-assisted hysterectomies were denied across multiple states despite peer-reviewed validation and ACOG guidelines, exposing not malice but a manufactured epistemology where clinical equivalence is undermined by procedural hyper-skepticism designed to shift burden of proof onto providers—a dynamic that legitimizes rejection through faux rigor rather than overt cost rhetoric.
Reimbursement Frontloading
Prior authorization protocols at Humana function less as clinical filters than as behavioral nudges that exploit clinician inertia, where even likely-approved therapies like PCSK9 inhibitors for familial hypercholesterolemia require multi-step appeals known to have 40% attrition before review, demonstrating that denials operate not through explicit guideline manipulation but through procedural friction timed against clinical urgency—challenging the assumption that interference requires doctrinal distortion, when in fact delay calibrated to provider fatigue achieves the same cost-saving ends with lower visibility.