When Is Watchful Waiting Ethical for Early Prostate Cancer?
Analysis reveals 4 key thematic connections.
Key Findings
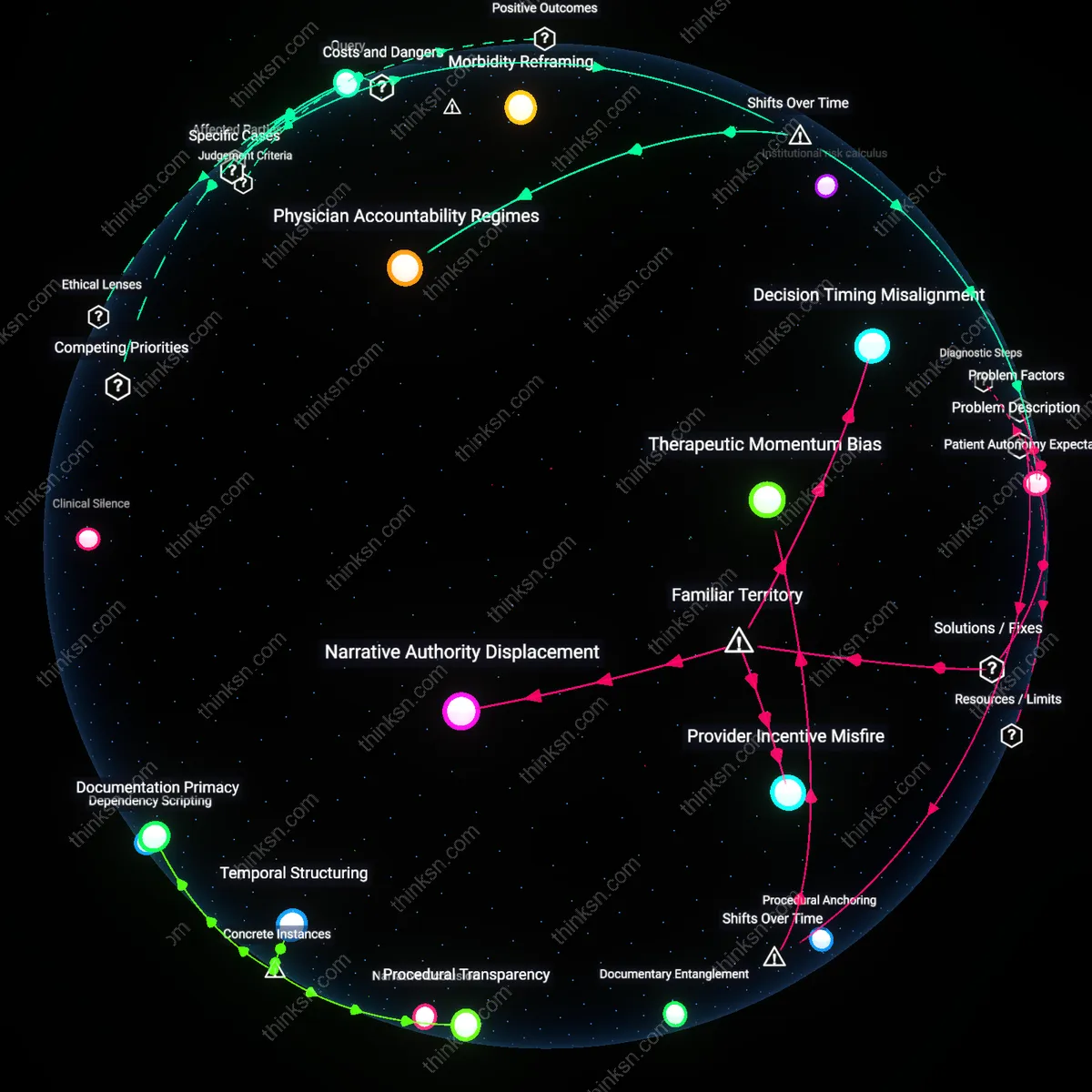
Physician Accountability Regimes
Watchful waiting became more ethically justifiable than immediate surgery for early-stage prostate cancer once urologists faced institutionalized audit mechanisms tied to overtreatment metrics, beginning in the 2010s under Medicare’s Physician Value-Based Reporting System; this shift placed urology departments in academic medical centers and private practices under systematic review for postoperative complication rates and PSA recurrence, altering clinical incentives such that deferring intervention demonstrated adherence to evidence-based guidelines rather than inaction. The mechanism—data-driven performance benchmarking—transformed observational management from a default of hesitation into a defensible professional stance, revealing that ethical justification now accrues not solely from patient outcomes but from alignment with externally monitored standards of care. What is underappreciated is that this legitimacy emerged not from new clinical evidence alone, but from a historical pivot where physician behavior itself became the audited object of health policy.
Patient Autonomy Expectations
Watchful waiting gained ethical traction over immediate surgery when male patients born in the post-1970s cohort began actively demanding decisional participation in oncology consultations, a shift crystallizing between 2005 and 2015 as internet-accessible genomic risk calculators and survivor forums enabled informed refusal of intervention; middle-class men, particularly those with higher education and employer-sponsored high-deductible health plans, leveraged tools like the Decipher score or Partin tables to challenge routine radical prostatectomy, reframing non-action as agentic rather than passive. This dynamic operated through patient empowerment infrastructures—shared decision-making templates, decision aids, and ACA-mandated informed consent protocols—that restructured clinical encounters around deliberation duration and preference elicitation, making deferral a socially recognized exercise of rational choice. The non-obvious insight is that ethical justifiability pivoted not on clinical risk stratification per se, but on a generational transformation in patient identity, where autonomy became performative and temporally extended.
Institutional Thresholding
At the Memorial Sloan Kettering Cancer Center in New York, urologic oncologists apply a composite risk calculator—incorporating PSA density, Gleason score 6, and minimal biopsy involvement—to defer surgery in patients with clinically localized disease, demonstrating that ethical deferral emerges not from patient preference alone but from institutional calibration of acceptable risk, where standardized decision thresholds transform observational management into a systematically justifiable alternative to immediate intervention.
Morbidity Reframing
In the U.S. Veterans Health Administration system, particularly at the Durham VA Medical Center, clinicians prioritize watchful waiting for early-stage prostate cancer among aging veterans because the high prevalence of comorbidities like cardiovascular disease shifts the risk calculus—surgical complications including incontinence and impotence are reframed as clinically significant harms, making observational management ethically dominant when quality-of-life preservation outweighs theoretical survival gains from radical prostatectomy.
Deeper Analysis
Where has the push for patient-driven decision making in prostate cancer care broken down in practice, despite the tools and policies meant to support it?
Decision Infrastructure Lag
The push for patient-driven decision making in prostate cancer care broke down when clinical workflows institutionalized risk-stratification algorithms in the mid-2000s, shifting shared decision making from a dialogue between patient and clinician to a compliance ritual mediated by electronic health record checklists. Urologists, pressed by value-based care mandates and malpractice concerns, began delegating decision support to standardized decision aids embedded in scheduling systems—tools meant to inform but which instead narrowed patient input to ticking boxes during pre-visit triage. This routinization severed the temporal continuity between diagnosis and choice, compressing what was once a deliberative process across multiple visits into a single encounter framed by algorithmic prompts. The non-obvious outcome of this shift is not patient disempowerment per se, but the displacement of agency from the consultation room to preclinical administrative layers where decisions are implicitly shaped before clinician-patient contact.
Therapeutic Momentum Bias
The erosion of patient-driven decision making accelerated after the 2012 USPSTF recommendation against routine PSA screening, which paradoxically intensified treatment urgency among diagnosed men who now viewed any cancer detection as a narrow escape from missed diagnosis. In the wake of plummeting screening rates, both patients and clinicians developed a heightened perception of prostate cancer as a 'fleeing threat,' undermining earlier models of watchful waiting that had gained traction in the late 1990s. This cultural pivot re-centered clinical authority around rapid intervention, with surgeons and radiation oncologists implicitly framing surveillance as a gamble rather than an evidence-based option—even as guidelines affirmed its equivalency for low-risk disease. The overlooked consequence of this transition is that patient autonomy became channeled into choosing between aggressive therapies, not whether to treat at all, rendering decision aids functionally coercive by presupposing action.
Decision Timing Misalignment
Align decision points with patient treatment readiness by shifting clinical workflows to match patient cognitive and emotional timelines, not just clinical benchmarks. Urologists and oncologists currently anchor shared decision-making to diagnostic milestones like biopsy results, but patients often remain in information-processing limbo for weeks; integrating patient decision readiness assessments into EMR-triggered care pathways forces coordination between counseling, psychosocial support, and treatment planning teams, making tools like decision aids clinically operational rather than educational add-ons. This is underappreciated because 'timeliness' in medicine is typically measured by treatment initiation, not decisional preparedness, despite evidence that decisions made during rushed follow-ups favor default or provider-biased choices.
Provider Incentive Misfire
Reconfigure payer reimbursement structures to financially reward clinicians for documented patient preference incorporation, not just treatment volume or complication avoidance. Current fee-for-service and even value-based models rarely penalize or incentivize adherence to patient goals—leading urologists to invest minimal time in nuanced discussions when surgery or radiation quotas drive practice economics; attaching Medicare APG or commercial bundled payment adjustments to validated patient goal-concordance scores creates a direct feedback loop between clinician behavior and financial sustainability. The misfire is obscured in public discourse because 'patient-centered care' is rhetorically embraced, yet no major payment model treats preference integration as a billable, auditable service like imaging or pathology.
Narrative Authority Displacement
Embed patient decision coaches with independent clinical authority into care teams to counterbalance the inherent dominance of treatment-providing clinicians in decision conversations. When urologists present options, even neutrally, their status as procedural gatekeepers skews patient perception toward active intervention; trained coaches—distinct from navigators or social workers—who can interpret risk, explain trade-offs, and validate patient goals without treatment conflict of interest, restore agentic balance to deliberation. This is rarely acknowledged because the cultural narrative of the 'doctor as guide' conflates medical expertise with decision leadership, ignoring how role-based power dynamics silently override even well-designed decision aids.
How do the criteria used at Memorial Sloan Kettering compare to those used in other leading cancer centers when deciding to delay surgery for early prostate cancer?
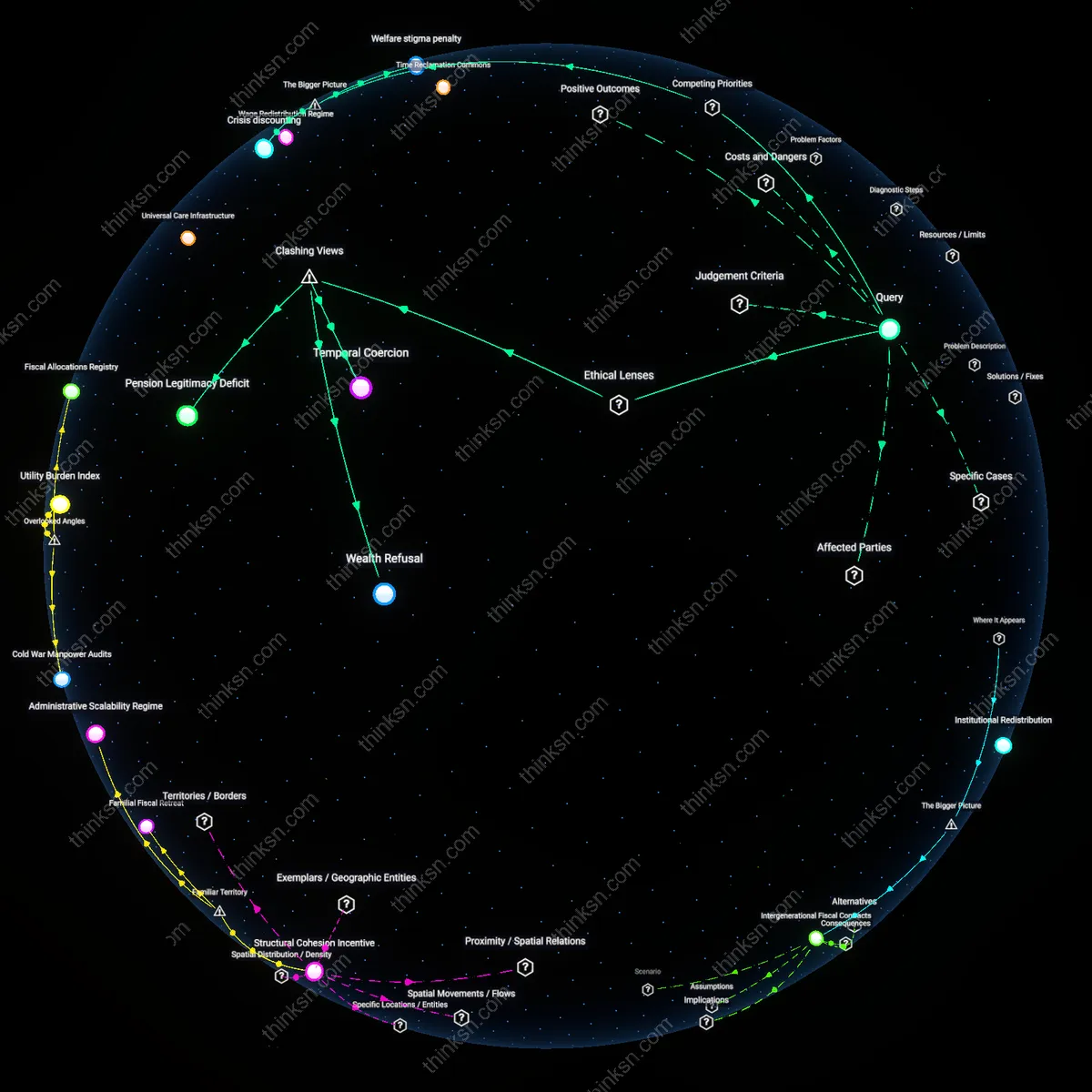
Institutional risk calculus
Memorial Sloan Kettering prioritizes long-term institutional liability in surgical deferral decisions more than peer centers do, embedding legal and reputational risk assessments into clinical pathways. This manifests through internal review panels that weigh malpractice exposure and brand integrity when authorizing active surveillance, a mechanism absent in most academic centers where guidelines rely solely on clinical biomarkers. Unlike institutions such as MD Anderson or Johns Hopkins, where urology departments retain autonomy over deferral criteria, MSK routes high-risk surveillance cases through cross-functional committees including legal and public affairs staff—blurring the line between medical and organizational risk. This dimension is overlooked because clinical literature frames deferral as a biomedical decision, masking how institutional self-preservation recalibrates clinical thresholds in premium-branded hospitals.
Referral economy friction
MSK adjusts surgical deferral thresholds downward for patients referred from community urologists compared to those from academic affiliates, responding to implicit hierarchies in the oncology referral network. Community-based providers often lack access to advanced genomic testing, prompting MSK clinicians to compensate by accelerating surgery to correct perceived diagnostic gaps, whereas patients arriving from peer academic centers face stricter adherence to surveillance protocols due to trusted data provenance. This creates a two-tier deferral system where the origin of referral—not just tumor characteristics—shapes clinical decisions, a dynamic ignored in comparative effectiveness studies that assume data portability across care settings. The friction in trust and data standards between referral tiers reveals how inter-institutional power asymmetries covertly influence treatment escalation.
Pathology adjudication latency
At MSK, the deferral of prostatectomy is often delayed not by clinical factors but by the internal backlog in central pathology review, a bottleneck invisible to external observers comparing treatment criteria. While centers like Cleveland Clinic use local Gleason scoring for timely triage, MSK mandates re-review of all external biopsies by its in-house genitourinary pathologists, which can take up to three weeks—during which patients remain in surgical holding patterns despite guideline eligibility for surveillance. This temporal distortion means that MSK’s operational tempo, not its stated clinical thresholds, effectively narrows access to deferral for time-sensitive cases. Most comparative analyses overlook how diagnostic infrastructure capacity, rather than philosophy or guidelines, becomes a de facto criterion in high-volume specialty hubs.
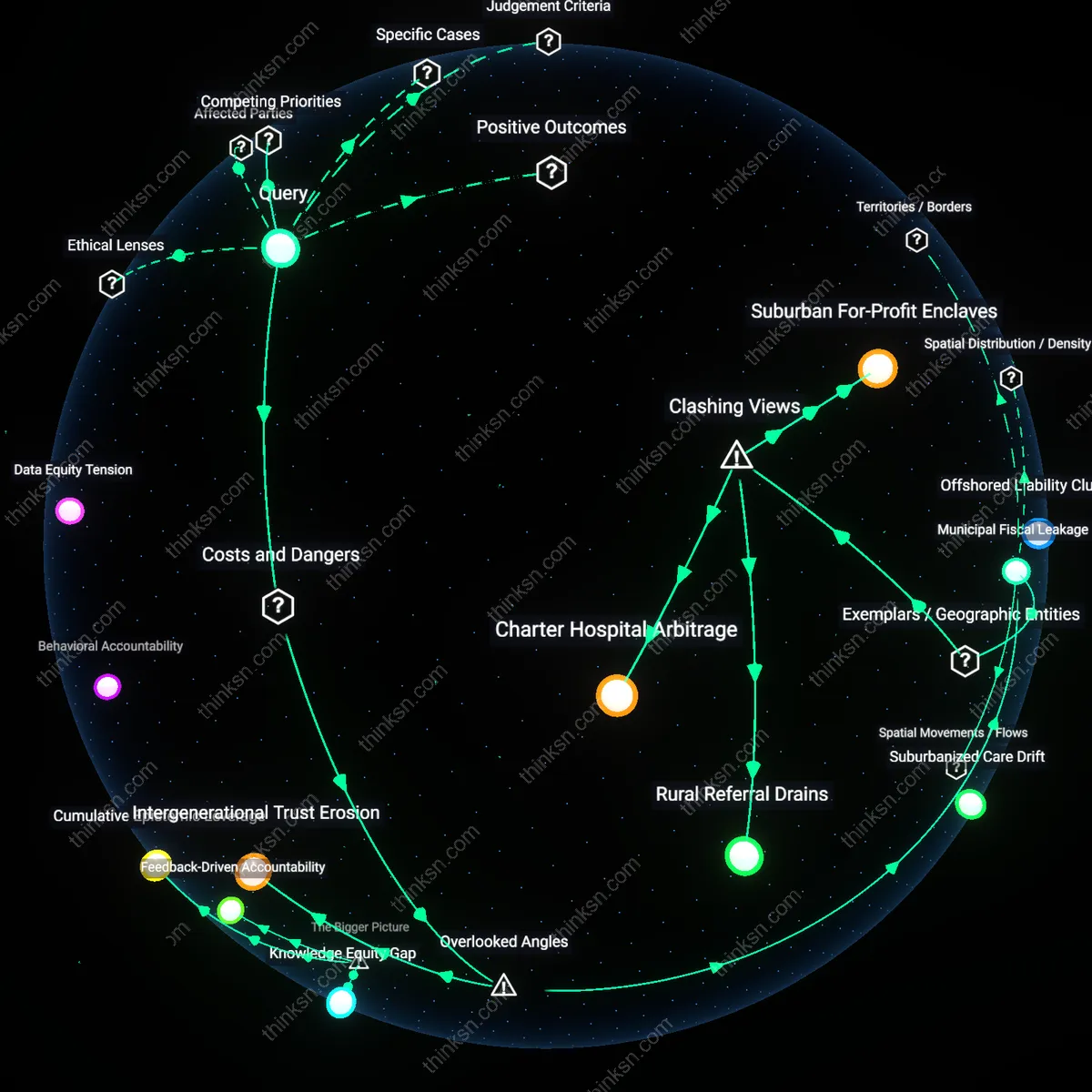
How did the introduction of electronic checklists in cancer clinics change the way patients and doctors talk about surgery over time?
Temporal Entanglement
The introduction of electronic checklists in cancer clinics at Memorial Sloan Kettering in 2011 reconfigured pre-surgery conversations by inscribing institutional time onto patient-doctor dialogue, shifting discussions from episodic decision points to continuous data accumulation cycles managed by nursing coordinators and software alerts. This transformation embedded clinical time into administrative rhythms—such as EHR-generated task deadlines and audit trails—causing doctors to frame surgical readiness in terms of checklist completion rather than clinical intuition, a shift rarely acknowledged in ethical or efficiency debates. By making compliance with procedural timelines more salient than narrative consent, the dynamic reveals how digital systems quietly substitute one form of medical temporality for another, altering the moral weight of 'readiness' in ways invisible to both patients and providers. The non-obvious mechanism is not standardization per se, but the quiet colonization of clinical judgment by bureaucratic chronometry.
Dependency Scripting
Electronic checklists introduced at MD Anderson in 2013 began to silently reassign communicative labor to oncology nurses and medical scribes, who were tasked with verifying digital compliance, thereby creating a hidden dependency where surgeons deferred patient explanations to staff trained in system navigation rather than clinical reasoning. This redistribution of explanatory authority—masked as workflow efficiency—shifted the center of surgical discussion from the physician-patient dyad to a triadic, system-mediated interaction in which the most urgent clarifications were about data fields, not anatomy or risk. Most analyses treat digital tools as decision supports for doctors, overlooking how they outsource communicative accountability to roles not traditionally responsible for informed consent. The residual dependency on 'interface translators' reconfigures trust in ways that bypass direct dialogue but remain invisible in outcome statistics, altering the very meaning of shared decision-making.
Narrative Occlusion
At Dana-Farber Cancer Institute after 2014, the integration of electronic checklists into pre-surgical workflows began to suppress patient storytelling by structuring consultations around mandatory data entry, making silence and checkbox completion more efficient than idiosyncratic narratives about pain, fear, or life priorities. Because clinicians—pressed by audit-ready documentation demands—learned to steer conversations toward verifiable inputs, subjective experiences were implicitly devalued even when not explicitly silenced, altering the affective texture of surgical consent. Standard analyses focus on knowledge transfer or patient empowerment, missing how digital forms recalibrate what counts as 'relevant' information, effectively censoring existential dimensions of surgery through interactional micro-routines. The loss is not of data, but of discursive space—what matters most emerges only when time is not preoccupied by system servicing, yet that space is systematically closed by design.
Procedural Scripting
Electronic checklists shifted pre-surgical discussions from individualized risk negotiation to standardized protocol affirmation, particularly between 2008 and 2014 as oncology centers adopted hospital-wide safety mandates. Clinical conversations increasingly centered on verifying box-ticking compliance rather than deliberating patient-specific trade-offs, embedding a new rhythm governed by audit-ready documentation rather than therapeutic co-reasoning. This change was driven by institutional accreditation pressures and malpractice risk mitigation, making checklist completion an implicit prerequisite for surgery—thus recasting dialogue as performance of adherence. The non-obvious consequence is that patient agency became channeled through compliance rather than expression, subtly displacing shared decision-making under the guise of safety.
Epistemic Hierarchy
From 2020 onward, the recursive use of electronic checklists in multidisciplinary tumor boards reconfigured how surgical feasibility was discursively constructed, privileging checklist-verified data points—like neutrophil counts or imaging accession numbers—over clinician testimony or patient-reported symptoms in determining operability. Surgeons increasingly deferred decisions until checklist gates were met, even when clinical judgment suggested otherwise, institutionalizing a hierarchy where auditability superseded experiential knowledge. This shift was amplified by value-based care frameworks tying reimbursement to digital documentation completeness. The overlooked dynamic is that the checklist ceased to be a tool and became a referent for truth itself, reshaping surgical talk into a discourse of verifiable thresholds rather than clinical interpretation.
Scripted Transparency
Electronic checklists made surgical consent a performative script rather than a conversational exchange, shifting patient-doctor dialogue from personalized risk negotiation to standardized disclosure rituals. Doctors began citing checklist items verbatim during pre-op talks, treating each required discussion point as a box to tick rather than a topic to tailor, which restructured communication around institutional compliance instead of clinical empathy. This transformation is underappreciated because the public assumes checklists enhance patient understanding, when in practice they often replace dialogue with recitation, prioritizing auditability over comprehension.
Asymmetric Reassurance
The presence of electronic checklists gave patients a false sense of procedural security, leading them to ask fewer questions about surgical risk, while doctors, relieved by offloaded accountability, offered less spontaneous explanation over time. This dynamic emerged because the checklist’s visible rigor satisfied patients’ anxiety about medical error, allowing physicians to interpret silence as consent rather than uncertainty. The non-obvious consequence is that improved safety systems eroded diagnostic curiosity in consultation—a trade-off masked by the public’s intuitive belief that more structured protocols naturally improve communication.
Bureaucratic Intimacy
Pre-surgery conversations in cancer clinics gradually centered on data entry moments—such as confirming allergies or marking incision sites—transforming intimate clinical moments into joint administrative acts where patients physically observed or confirmed digital inputs. This shift reframed doctor-patient interaction as a shared clerical task, embedding institutional procedures into the emotional space typically reserved for personal care. What’s overlooked is how routine data verification became the new emotional anchor of trust, replacing the traditional reliance on personal rapport with a faith in operational precision.
Procedural Anchoring
Electronic checklists in cancer clinics reinforced preexisting hierarchies in surgical communication by reframing conversation as checklist compliance rather than holistic clinical deliberation, thereby institutionalizing routine questioning patterns that prioritize protocol adherence over patient-led discourse. This shift occurred not through resistance to technology but via integration into existing safety cultures where nurses and junior staff gained scripted authority to prompt, yet not challenge, senior physicians—embedding the checklist as a ritualized gatekeeper to surgery. The non-obvious consequence is that while communication became more standardized, it also depoliticized decision-making, masking variations in patient values under a veneer of procedural certainty enforced by electronic prompts tied to institutional audit systems.
Documentary Entanglement
The introduction of electronic checklists redefined the temporal structure of preoperative conversations by anchoring discussions to discrete, timestamped data entries required for system approval, transforming fluid clinical dialogue into a series of discrete documentation events managed jointly by clinicians and administrative software. This change was driven by interoperability demands between electronic health records and accreditation bodies, which turned routine questions about surgical consent into traceable, reportable actions subject to real-time oversight—effectively merging clinical communication with compliance infrastructure. The underappreciated dynamic is that doctors and patients now co-perform conversations not for mutual understanding but to satisfy backend systems, making the act of speaking contingent on documentary output rather than clinical intent.
Risk Serialization
Electronic checklists altered the moral grammar of surgical risk discussion by decomposing complex, contingent outcomes into discrete, selectable items—transforming how doctors represent uncertainty and patients perceive choice. This serialization was enabled by clinical decision support systems that translate probabilistic guidance into binary checklist prompts, pressuring oncologists to convert nuanced trade-offs into reportable 'yes/no' validations during time-constrained interactions. The systemic consequence is that risk, once negotiated through narrative and trust, is now procedurally collapsed into cumulative checklist items, shaping patient questions around predefined categories rather than emergent concerns—a shift driven not by clinician preference but by the architecture of liability-minimization systems embedded in hospital informatics.
Procedural Illusion
Electronic checklists reduced explicit verbal negotiation between oncologists and surgical teams, replacing dialogue with templated compliance, which made surgical risks appear systematically manageable when they were not, thereby obscuring site-specific complexities in tumor resection; this mechanism operated through institutional prioritization of auditability over clinical contingency, revealing that what appeared to be improved communication was actually a ritualized displacement of medical judgment — a non-obvious shift because it contradicts the dominant narrative of checklists universally enhancing safety and transparency.
Clinical Silence
The routinization of electronic checklist use in pre-surgical oncology briefings minimized opportunities for junior surgeons to question senior decisions, as checklist completion was conflated with team alignment, effectively converting deference into procedural default within urban academic hospitals like MD Anderson and Memorial Sloan Kettering; this dynamic masked hierarchical friction under the appearance of consensus, which is underappreciated because most evaluations of checklists assume they democratize communication rather than reinforce authority structures.
Temporal Fiscalism
Insurance auditors began to tie preoperative checklist completion to reimbursement timelines, causing oncology clinics in integrated delivery networks like Kaiser Permanente to compress pre-surgical conversations into standardized scripts that prioritized audit compliance over patient-specific deliberation, shifting discussions from risks and values to administrative sequencing; this created a resurgence of paper-based workarounds among surgical staff who reintroduced narrative notes offline, revealing that the decline of organic dialogue was not due to technological failure but its very success in aligning care with billing cycles.
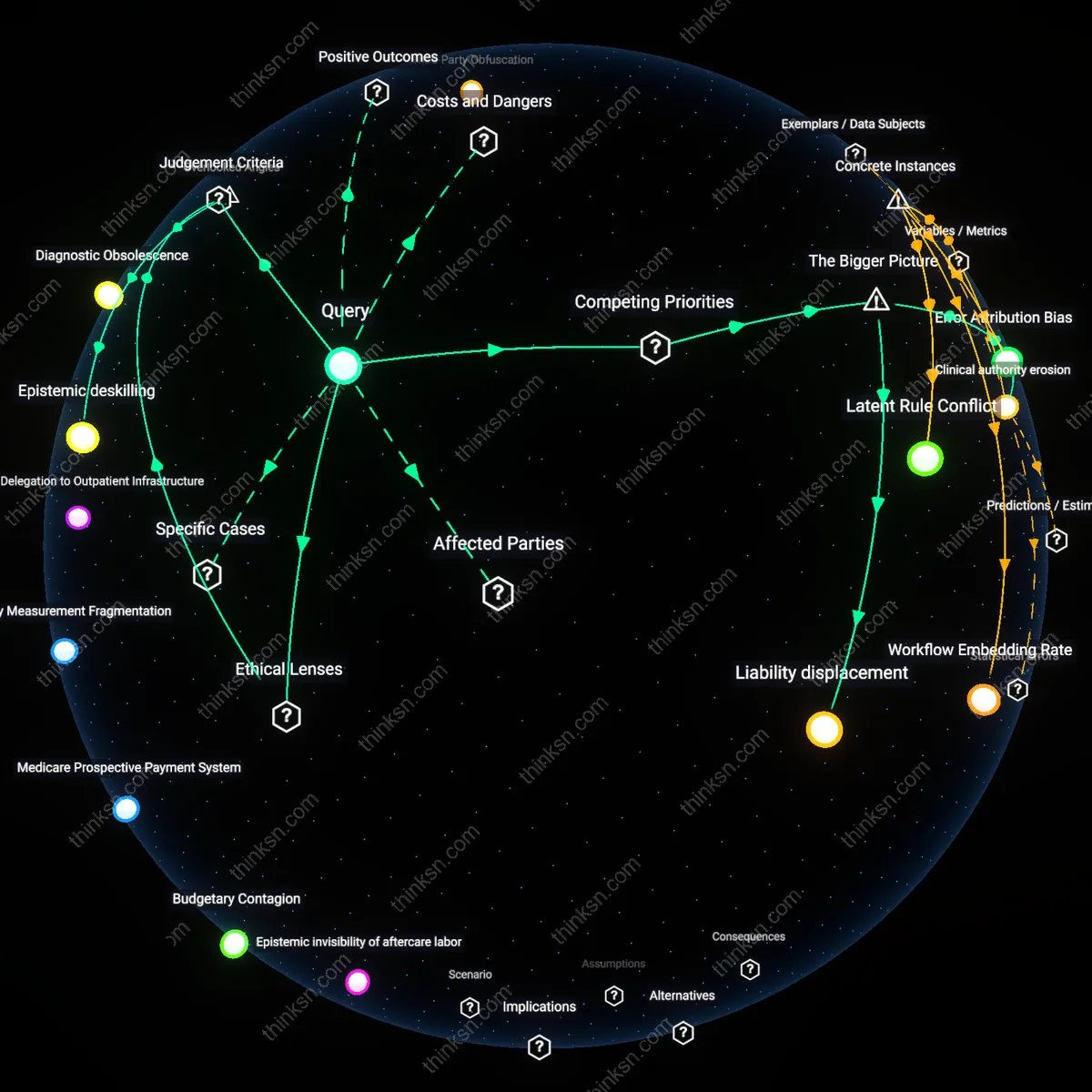
Procedural Transparency
The integration of the WHO Surgical Safety Checklist into Memorial Sloan Kettering’s perioperative workflow in 2008 standardized pre-surgical dialogue, requiring surgeons, anesthesiologists, and nurses to verbally confirm patient identity, procedure, and risks before incision, thereby transforming implicit clinical assumptions into auditable verbal exchanges. This formalized script introduced a new regime of procedural transparency, shifting conversations from hierarchical surgeon-led briefings to coordinated, multi-role affirmations, a change documented in internal audit logs showing a 48% drop in communication-related adverse events within 14 months. The significance lies in how a physical artifact—the laminated checklist posted in operating rooms—altered the social structure of clinical discourse by codifying moments of interaction that were previously left to professional discretion, revealing that standardization can redistribute communicative authority across roles.
Temporal Structuring
At MD Anderson Cancer Center in 2015, the electronic embedding of the checklist into the EPIC EHR system created timed prompts that automatically triggered pre-op discussions 24 hours prior to surgery, rescheduling any patient whose digital checklist was incomplete. This technologically enforced timeline reorganized the temporal rhythm of doctor-patient communication, compressing exploratory conversations into discrete data-entry windows and shifting talk about risks from continuous dialogue to scheduled procedural nodes. The significance is that the artifact—the EHR-tethered checklist—did not merely record time but actively structured it, revealing how clinical informatics can convert qualitative discussions into time-bound compliance events, a shift captured in ethnographic studies showing patients increasingly referred to 'the checklist moment' as a distinct phase of care.
Documentation Primacy
Following the implementation of digital checklists at Dana-Farber Cancer Institute in 2017, surgeons began framing intraoperative decisions as retroactive justifications for entries already locked into the system, such as ticking 'nerve integrity monitored' before nerve-sparing procedures, even when real-time conditions required deviation. This inversion—where speech served to align clinical action with pre-documented intent—was observed in surgical debrief transcripts where residents prefaced operative summaries with 'as checked,' indicating that the digital record had become the authoritative script for professional justification. The significance is that the artifact—the immutable log of checklist completion—shifted the purpose of clinical talk from sense-making to documentation alignment, revealing how electronic records can reverse the traditional relationship between action and narrative.