Why Early MS Treatment Proves Effective Yet Fears Persist?
Analysis reveals 7 key thematic connections.
Key Findings
Therapeutic Trauma Transference
Patients with multiple sclerosis fear long-term side effects because early aggressive treatments are administered during periods of diagnostic uncertainty, when the trauma of receiving a life-altering diagnosis amplifies risk aversion—this emotional imprint becomes transferred onto the therapy itself, making the treatment symbolize existential threat rather than intervention. Neurologists often initiate high-efficacy disease-modifying therapies within weeks of diagnosis, coinciding with patients’ incomplete cognitive and emotional processing of MS as a chronic illness, which causes them to conflate the disease’s unpredictability with the drug’s potential harm. The mechanism operates through affective forecasting errors in high-stress medical encounters, where the salience of immediate pharmacological intrusion overwhelms statistical literacy about long-term benefit, a dynamic rarely acknowledged in clinical guidelines that assume rational risk calculus. This dimension matters because it reveals that fear is not of side effects per se but of their symbolic role in retriggering diagnostic trauma—shifting the standard understanding from informational deficit to psychodynamic resonance.
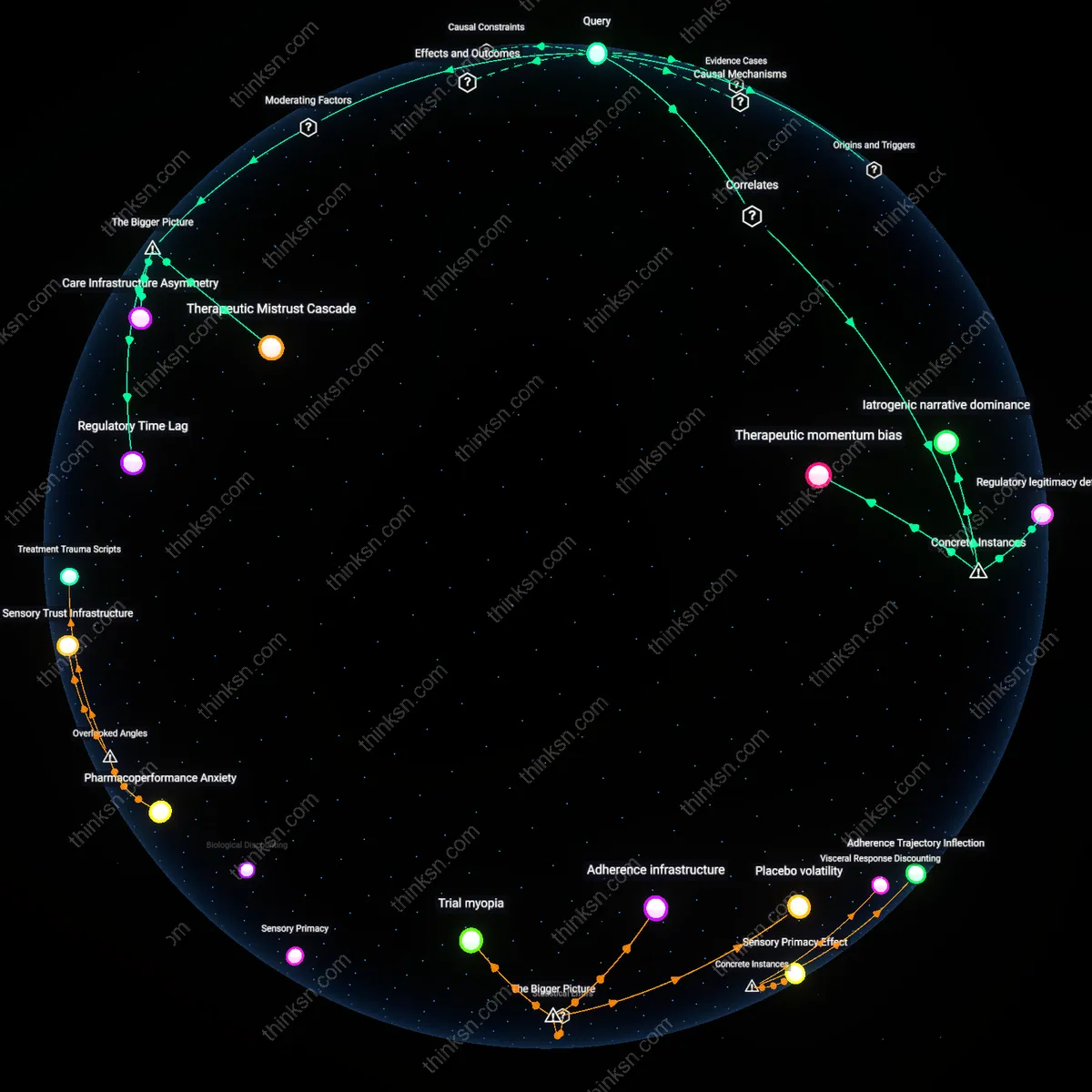
Therapeutic Mistrust Cascade
Patients with multiple sclerosis fear long-term side effects because aggressive early treatment disrupts the perceived symmetry between medical authority and patient autonomy, triggering a reflexive skepticism rooted in past experiences with pharmaceutical harm. Neurologists, operating under evolving treatment guidelines, advocate early high-efficacy drugs like ocrelizumab or natalizumab, but patients recall high-profile drug withdrawals or safety scandals—such as Tysabri’s initial market removal due to PML cases—which recalibrate their risk calculus. This dynamic is amplified by online patient communities where anecdotes of delayed adverse effects circulate disproportionately, reframing clinical evidence through lived vulnerability. The non-obvious consequence is that evidence strength alone cannot override a systemic erosion of trust when treatment intensity outpaces experiential validation.
Regulatory Time Lag
Patients fear long-term side effects because the temporal horizon of clinical trial data does not align with the lifelong reality of MS progression, creating a temporal mismatch between regulatory approval and personal risk exposure. Drug approval relies on 2–5 year trial outcomes, but aggressive therapies carry unknowns over decades—especially concerning immunosuppression-induced comorbidities like cancer or infections. Regulatory agencies, pharmaceutical companies, and reimbursement systems prioritize short-term efficacy metrics, inadvertently disincentivizing long-term safety monitoring infrastructure. This systemic myopia makes delayed adverse effects structurally invisible, rendering patient fears rational within a system that does not track what happens after year ten.
Care Infrastructure Asymmetry
Patients fear long-term side effects because access to specialized monitoring required for aggressive therapies is unevenly distributed, converting medical benefit into geographic and socioeconomic risk. High-efficacy treatments demand regular MRI surveillance, infectious disease screening, and neuroimmunology expertise—resources concentrated in academic centers, often inaccessible outside urban or insured populations. When patients anticipate living with treatment for decades but lack reliable access to the systems necessary to detect complications early, they rationally de-prioritize efficacy in favor of manageable risk. The underappreciated systemic flaw is that treatment aggressiveness assumes a level of healthcare continuity that most patients cannot count on, making caution a form of resilience.
Therapeutic momentum bias
Patients in the CHAMPS trial feared long-term side effects of interferon beta-1a because early treatment created a perceptual trade-off between immediate intervention and future risk, even though delayed therapy showed worse outcomes; clinicians observed that the very act of initiating treatment intensified anxiety about downstream consequences, revealing that therapeutic momentum—once a drug regimen begins—amplifies risk attribution to the treatment rather than the disease's progression. This dynamic operates through patient expectations shaped by exposure to early adverse events, which become cognitively anchored more strongly than the diffuse threat of neurodegeneration, making the treatment appear riskier over time regardless of efficacy data. The non-obvious insight is that aggressive early action, while clinically superior, inadvertently increases perceived treatment-specific danger by creating a temporal association between symptom onset and drug initiation, regardless of causality.
Iatrogenic narrative dominance
At the University of California, San Francisco MS Center, patient focus groups conducted in 2015 revealed that stories of secondary autoimmune conditions—like thyroiditis or lupus-like syndromes—emerging months after starting natalizumab were disproportionately remembered and shared, despite epidemiological data showing lower overall harm than untreated progression; these anecdotal clusters formed a narrative field where treatment-induced illness was more narratively coherent than random disease worsening, thus dominating risk perception. The mechanism works through communal sense-making in chronic illness communities, where rare but dramatic adverse events are storied and transmitted more efficiently than silent axonal loss, skewing group-level risk assessment. The underappreciated dynamic is that narrative fidelity to visible, timed events over invisible degeneration makes iatrogenic outcomes feel more intentional and therefore more feared, even with lower incidence.
Regulatory legitimacy deficit
Following the 2006 FDA’s partial withdrawal of approval for mitoxantrone due to cumulative cardiotoxicity and leukemia risk, patients across Europe and North America began to generalize regulatory caution to newer high-efficacy agents like alemtuzumab, despite distinct pharmacological profiles and improved monitoring protocols; the residual distrust in long-term safety monitoring systems persisted even when clinical evidence supported early use, as patients associated aggressive therapy with delayed regulatory reckoning. This operates through institutional memory of past drug withdrawals, where risk mitigation appears retrospective rather than preventive, weakening confidence in current safety assurances. The non-obvious insight is that regulatory interventions—intended to enhance trust—can create a legitimacy deficit by signaling that delayed harms are inevitable and systematically underestimated in early approval phases.