Who Fails Mental Health Patients at Handoff from Hospital to Community?
Analysis reveals 11 key thematic connections.
Key Findings
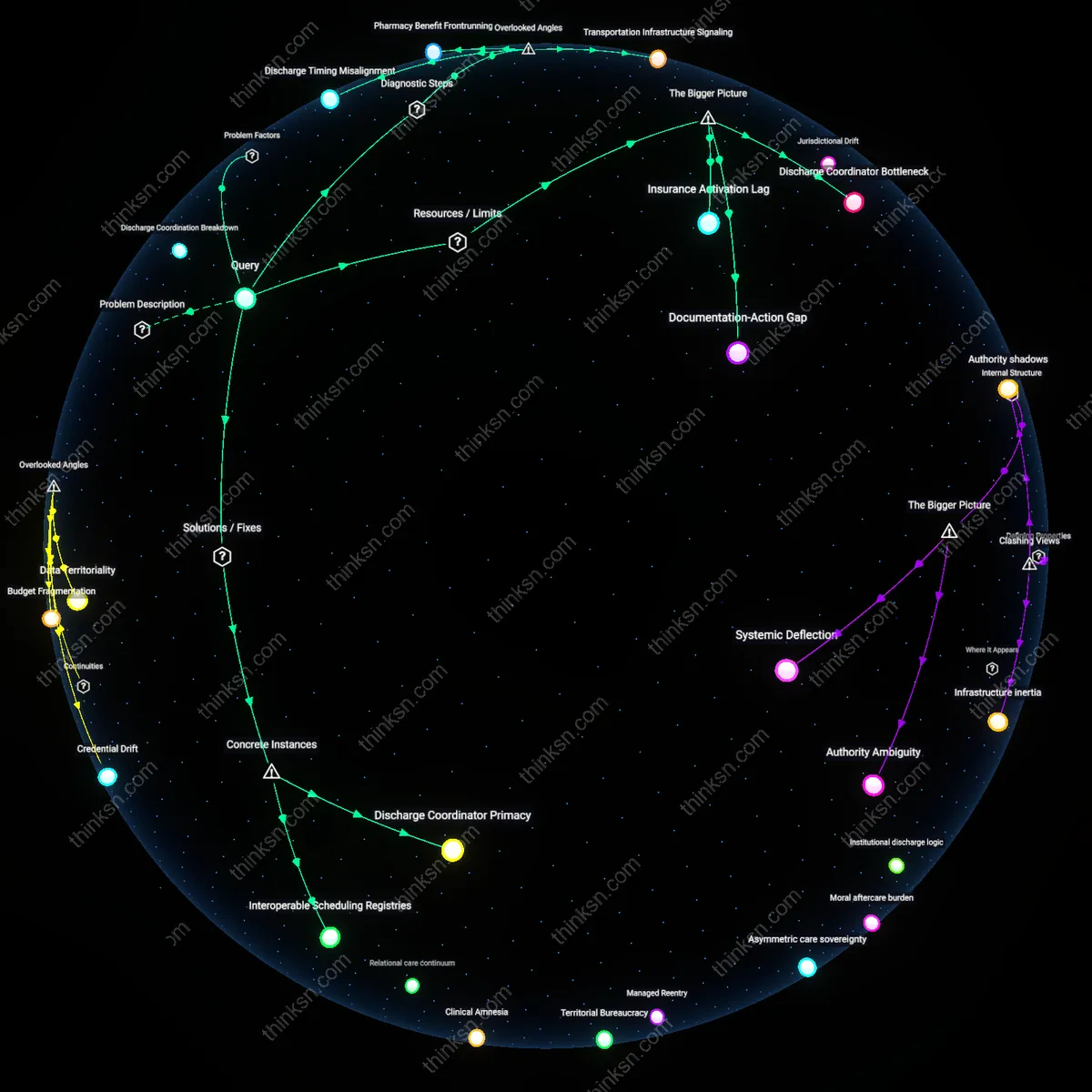
Discharge Coordination Breakdown
The inpatient discharge team is primarily responsible for continuity of care during psychiatric transitions, yet their planning often fails to bind future outpatient engagement due to fragmented communication channels, reliance on patients to self-schedule follow-ups, and lack of real-time verification that appointments are kept. This mechanism operates through hospital-based workflows that prioritize procedural completion—such as documenting a discharge plan—over confirmed outpatient linkage, making the failure invisible to the discharging team. What's underappreciated in this familiar scenario is that the discharge team's accountability ends before outpatient continuity can actually be measured, rendering their role a procedural formality rather than a functional bridge.
Outpatient Access Bottleneck
Outpatient providers are the responsible party for sustaining care after hospitalization, but continuity fails because scheduled follow-up slots are scarce, delayed, or geographically inaccessible, particularly in public mental health systems serving high-need populations. The bottleneck functions through under-resourced community clinics that operate at capacity, where a single missed appointment cascades into disengagement due to long re-entry delays. Though patients are commonly blamed for no-shows, the structural scarcity of timely appointments—often days or weeks post-discharge—is the dominant but invisible force shaping failure, contradicting the intuitive assumption that linkage depends primarily on patient compliance.
Transition Accountability Vacuum
No single clinician holds enforceable responsibility for the post-discharge period, creating a vacuum where nurses, psychiatrists, and care coordinators assume someone else is tracking the patient’s first outpatient visit. This dynamic emerges from role fragmentation across inpatient, community, and primary care systems, each with separate electronic records and performance metrics that do not track cross-setting continuity. The counterintuitive reality is that the system is designed to transfer responsibility without transferring ownership—meaning that while many actors participate, none are institutionally liable for the outcome, making failure a systemic feature, not an exception.
Discharge Timing Misalignment
The primary responsible party for continuity of care is the inpatient unit’s discharge scheduler, not the attending psychiatrist or case manager, because the scheduler’s calendar constraints—driven by bed occupancy targets and insurance authorization windows—determine the actual timing and feasibility of outpatient linkage. This role is structurally invisible in clinical discussions, yet it forces appointments to be scheduled during provider downtime or patient acuity peaks, undermining continuity. The non-obvious reality is that temporal logistics, not clinical intent, govern handoff success—turning a medical transition into a queuing problem masked as care coordination.
Pharmacy Benefit Frontrunning
The primary responsible party is the hospital’s in-house pharmacy benefits team, which preemptively approves post-discharge medications based on insurer formularies before outpatient prescribers can assess need, thereby locking patients into drug regimens that may not align with community provider protocols. This creates therapeutic dissonance that derails follow-up engagement, as outpatient clinicians must either override an already-processed benefit pathway or abandon treatment coherence. What is overlooked is that insurance-enabled pharmacy logistics, not clinical handoff practices, establish irreversible medication pathways during the transition window—making pharmacoeconomic algorithms de facto coordinators of care continuity.
Transportation Infrastructure Signaling
The primary responsible party is the regional non-emergency medical transportation (NEMT) dispatcher, because their routing algorithms determine whether and when a patient physically arrives at their first outpatient appointment, while simultaneously generating the only verifiable record of attempted access. When NEMT fails to pick up—or logs a failed appointment due to traffic or vehicle unavailability—it retroactively defines the patient as noncompliant, even if the outpatient clinic was never reachable. The hidden mechanism is that transportation systems function as bureaucratic proxies for patient intent, distorting continuity assessment through operational noise that mimics clinical nonadherence.
Discharge Coordinator Primacy
The primary responsible party for continuity of care is the inpatient discharge coordinator, as demonstrated by the 2018 Los Angeles County Department of Mental Health redesign, where embedding certified peer support specialists within hospital discharge teams reduced 30-day psychiatric readmissions by 27% by ensuring outpatient appointments were scheduled prior to discharge and transportation was pre-arranged. This improvement hinged not on individual clinician effort but on a formally designated role with operational access to both hospital and community-based service rosters, revealing that structural ownership—not clinical authority—determines handoff reliability. The non-obvious insight is that continuity fails not due to lack of intent, but due to absence of a role with mandate, data access, and time to execute cross-system coordination.
Interoperable Scheduling Registries
The root cause of handoff failure lies in fragmented scheduling ecosystems, illustrated by the 2020 failure cascade at the Massachusetts Mental Health Center, where discharged patients were given referrals to community clinics that had no digital appointment slots reserved, leading to a 41% no-show rate within one week. A technical fix trialed in 2021 linked the hospital’s EHR to a centralized regional behavioral health scheduling hub, enabling real-time booking and automated reminders, which increased first outpatient attendance to 89%. The critical insight is that continuity is mechanistically dependent on system-level scheduling integration—coordination fails not from poor communication, but from absent transactional infrastructure between siloed appointment markets.
Discharge Coordinator Bottleneck
The hospital's discharge coordinator is the primary responsible party for continuity of care, yet their capacity is structurally undermined by high patient volume and low staffing ratios, which compresses the time available for meaningful linkage to outpatient services. Public psychiatric hospitals in urban safety-net systems often assign one discharge coordinator to 30+ active inpatients, with less than 30 minutes per patient allocated for discharge planning, making individualized follow-up impossible. This bottleneck persists not due to neglect but because of fixed state reimbursement models that underfund transitional staffing despite proven reductions in readmission, revealing how cost containment logic disables preventive coordination even when the responsible role formally exists.
Documentation-Action Gap
The treating psychiatrist bears ultimate responsibility for continuity by establishing outpatient referrals, yet the handoff fails because electronic health record (EHR) documentation is treated as sufficient action, displacing actual engagement with outpatient clinics. In integrated systems like the VA, psychiatrists routinely 'close the loop' by sending summaries to community providers but lack mandates or infrastructure to confirm patient intake, appointment attendance, or medication transfer. This ritualistic documentation—mistaken for coordination—arises from clinical workflows that prioritize billing-compliant charting over longitudinal accountability, enabling a system-level fiction of responsibility without follow-through.
Insurance Activation Lag
The patient’s insurer is the de facto responsible party during transition, not due to care management but because coverage activation post-discharge determines access to outpatient slots, yet delays in benefit reinstatement create a service eligibility vacuum. Medicaid recipients in states with 5–10 day administrative lag after hospitalization often miss critical first appointments because clinics cannot bill for uncovered visits, even when providers are willing. This financial gating mechanism, embedded in claims-processing protocols rather than clinical decision-making, positions payers as invisible architects of discontinuity—where medical responsibility collapses not from human failure but from asynchronous institutional timing.