Is Your Medical Appeal Denial Just Clinical Reasoning or a Legal Roadblock?
Analysis reveals 6 key thematic connections.
Key Findings
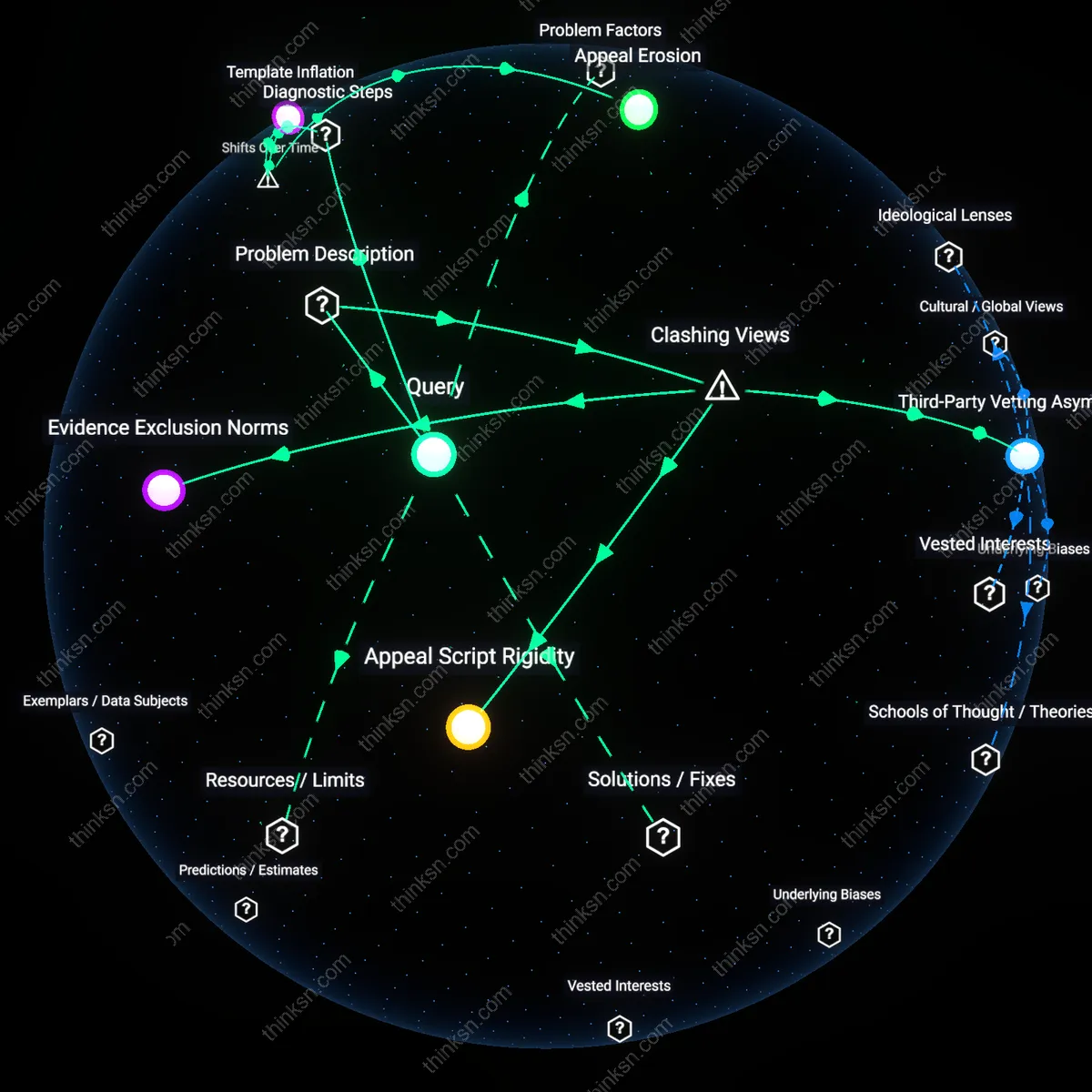
Appeal Script Rigidity
A patient can detect a template-based denial by identifying invariant clinical language across medically dissimilar cases, which reveals that insurance reviewers are required to anchor determinations in pre-approved phrases regardless of case-specific evidence. This rigidity emerges from centralized medical policy units at insurers like UnitedHealthcare or Aetna, where non-negotiable language modules are embedded in decision software used by junior medical directors, making individualized clinical judgment mechanically impossible. The non-obvious truth here is that the denial is not a failure of review quality but a designed outcome of scalable, legally defensible standardization meant to withstand litigation, not clinical scrutiny.
Third-Party Vetting Asymmetry
A patient can expose a template-driven denial by requesting the external peer review log and comparing the citing physician’s credentials and specialty against the clinical complexity of the case, as many insurers contract narrow panels of part-time reviewers from geographically distant markets who lack subspecialty alignment with the treatment in question. This mechanism—used by carriers such as Cigna in high-volume commercial plans—relies on rapid, low-cost evaluations that prioritize payer liability reduction over clinical fidelity, masked by the appearance of independent oversight. The dissonance lies in the fact that external review is structurally disincentivized from contesting insurer policy, rendering the appeal verification process a procedural formality rather than a substantive check.
Evidence Exclusion Norms
A patient can identify a non-clinical denial by documenting whether new, time-stamped medical evidence submitted post-initial decision was acknowledged in the appeal response, since automated systems like Anthem’s AIM platform routinely process appeals without human forwarding to clinical staff, filtering submissions through AI triage that disregards updates outside predefined intake windows. This creates a systemic blind spot where appeals are adjudicated on static, outdated records, even when fresh imaging or specialist letters are provided. The underrecognized issue is that timely medical evidence is not merely overlooked but institutionally excluded to preserve throughput and minimize variance in denial consistency.
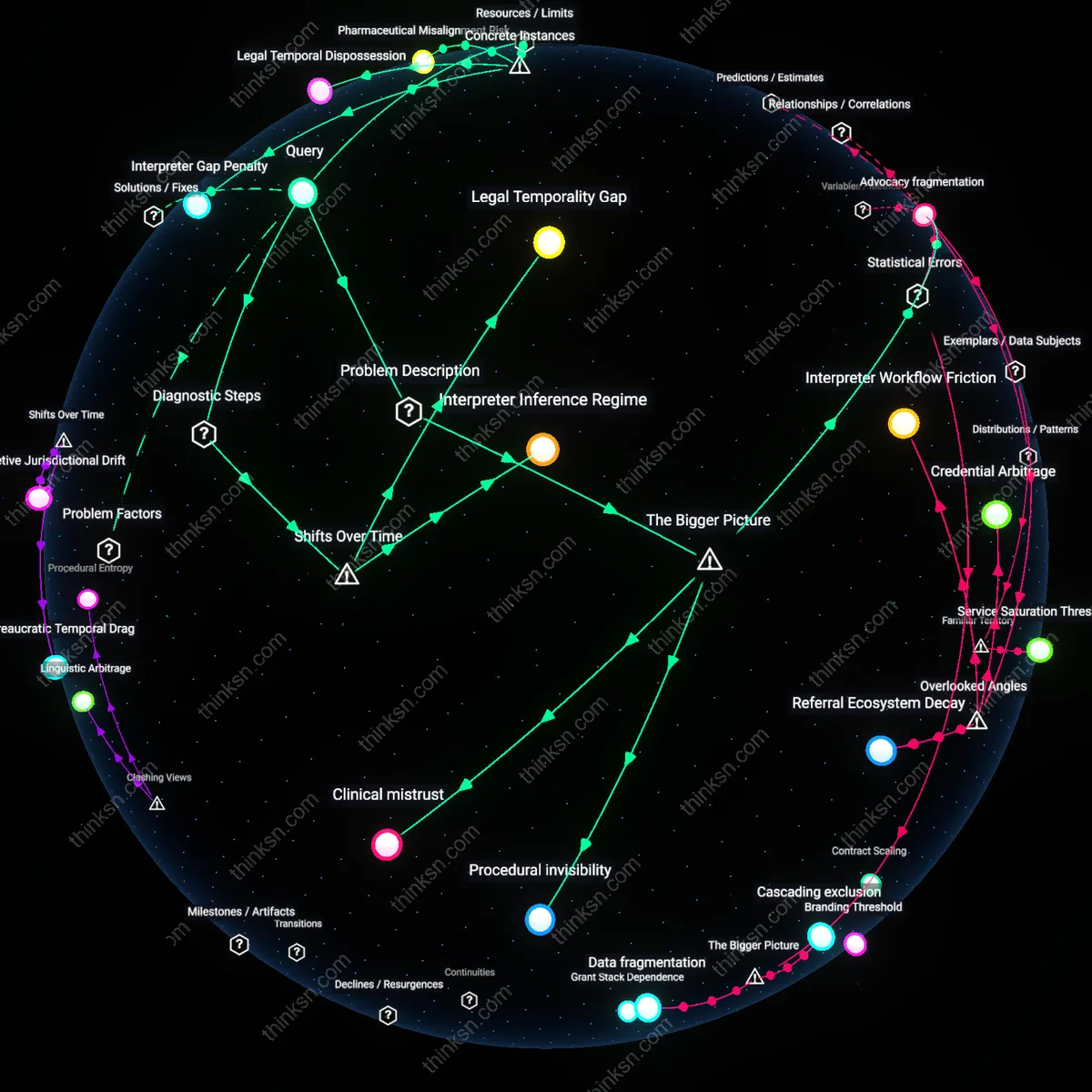
Template Inflation
A patient can detect a standardized denial by comparing the clinical specificity of the insurer's cited guidelines against current National Comprehensive Cancer Network (NCCN) benchmarks, because post-2010, private insurers increasingly adopted layered template language that mimics individualized review while referencing outdated or generalized protocols. This mechanism operates through decentralized medical director sign-offs that rubber-stamp algorithmic determinations masked as clinical judgment, and its significance lies in how post-Affordable Care Act regulatory pressures incentivized the appearance of compliance without substantive review. The non-obvious shift is that denials became more linguistically sophisticated after 2015, not more clinically rigorous, revealing template inflation as a response to heightened appeal volumes.
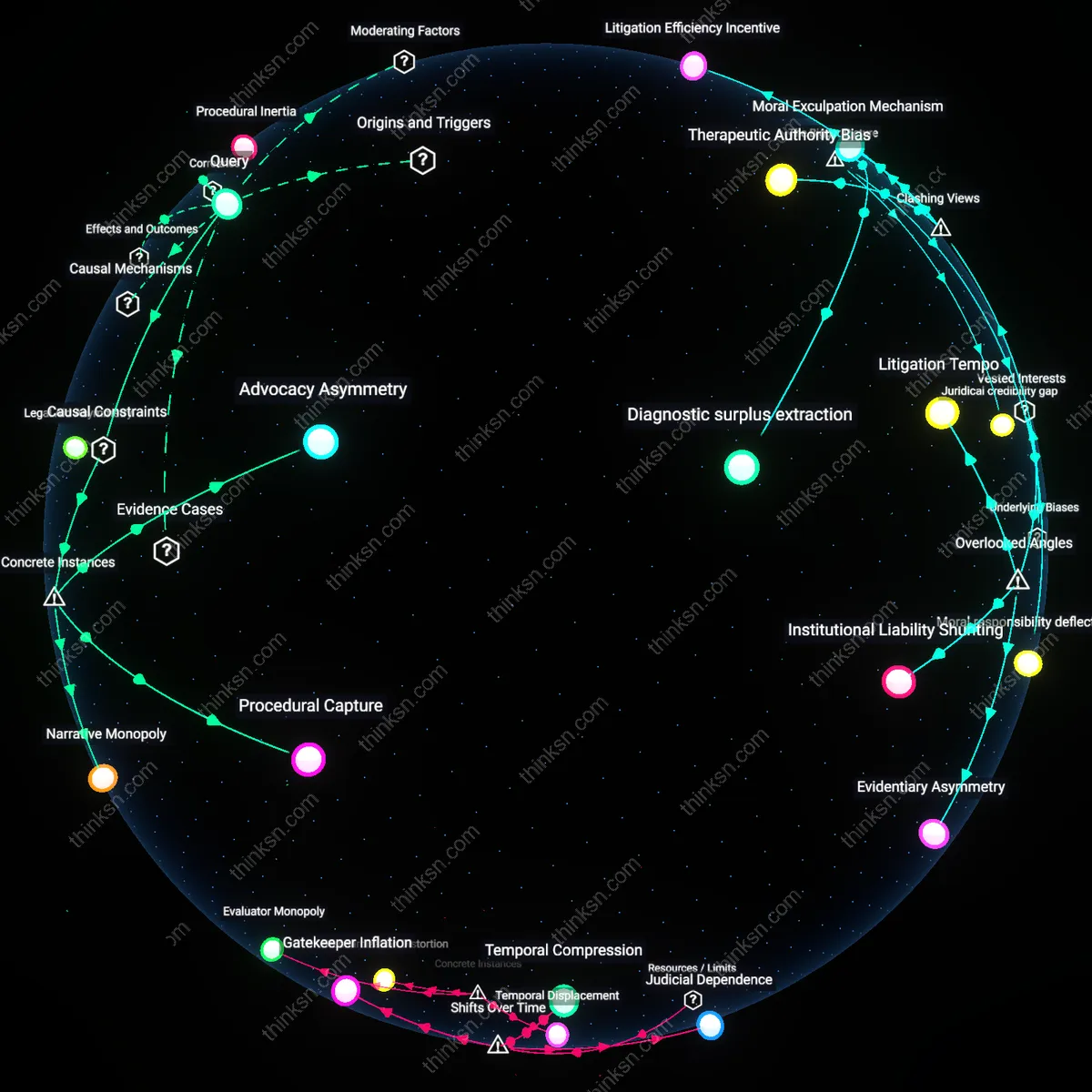
Appeal Erosion
A patient should assess the temporal consistency of denial reasoning across successive appeals, because prior to the 2000s, insurers rarely maintained longitudinal records, but after electronic case management systems became standard post-2008, repeat denials began exhibiting identical phrasing despite new evidence, indicating a systemic drift from adaptive review to procedural exhaustion. This occurs through legacy workflows in third-party utilization review vendors who prioritize closure rates over re-evaluation, and it reveals how automation has shifted the purpose of appeals from validation to delay. The underappreciated consequence is that the process now functions not to assess care but to wear down claimants, producing appeal erosion as a structurally embedded outcome.
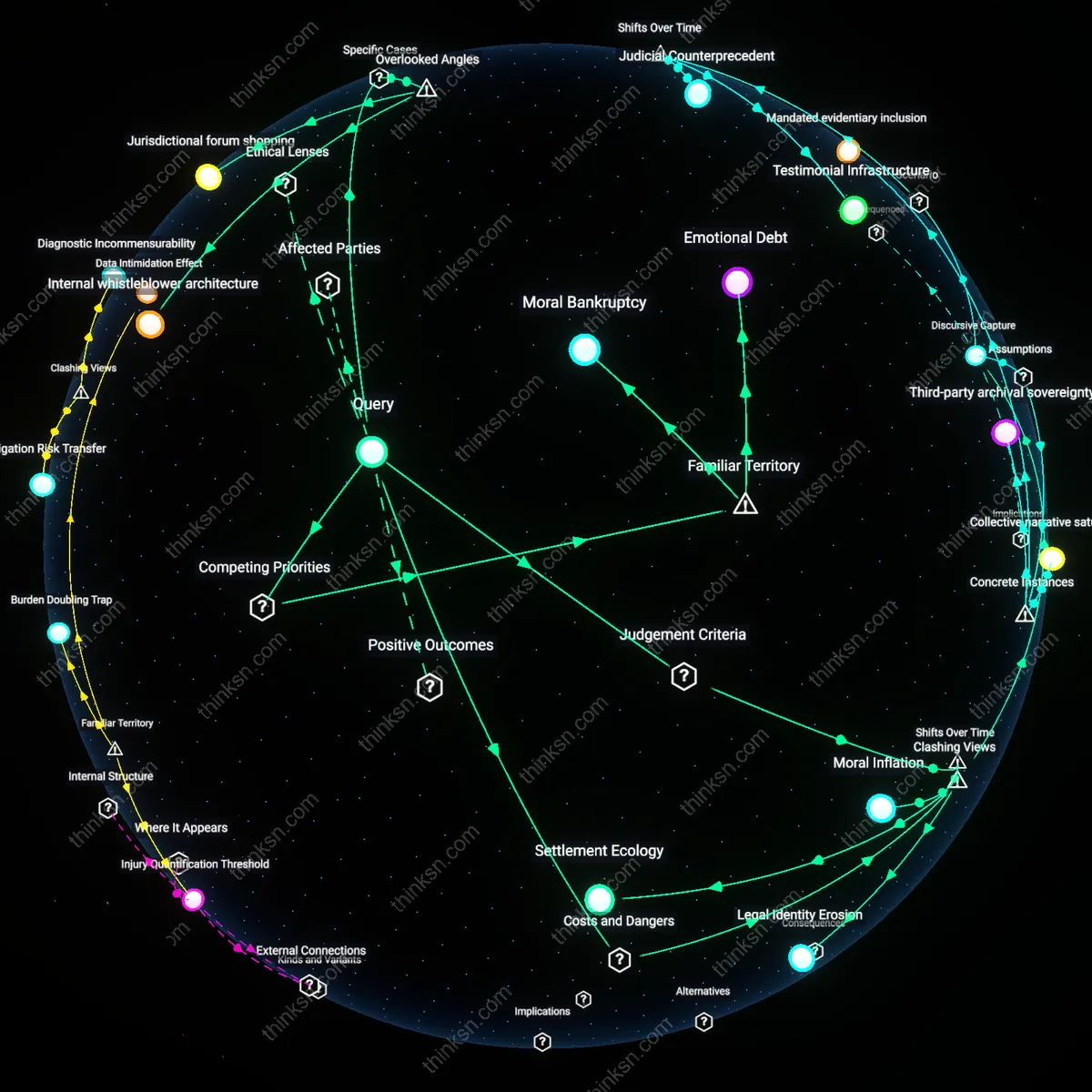
Clinical Theater
A patient can identify a template denial by examining whether the insurer's medical reviewer practices in the same specialty as the treating physician, because after the 1990s shift from in-house physicians to contracted external reviewers, clinical justifications increasingly came from generalists evaluating highly specialized treatments, creating a performance of expertise without domain-specific engagement. This dynamic persists through outsourced review mills like HMS or eviCore, where financial incentives favor rapid turnover over deep analysis, and its significance is that the denial’s content now serves regulatory optics rather than medical discourse. The overlooked result of this 1990s privatization wave is clinical theater—an evaluative façade evolved to satisfy legal scrutiny, not clinical standards.