Is Private Long-Term Care Worth It When Medicaid Awaits?
Analysis reveals 7 key thematic connections.
Key Findings
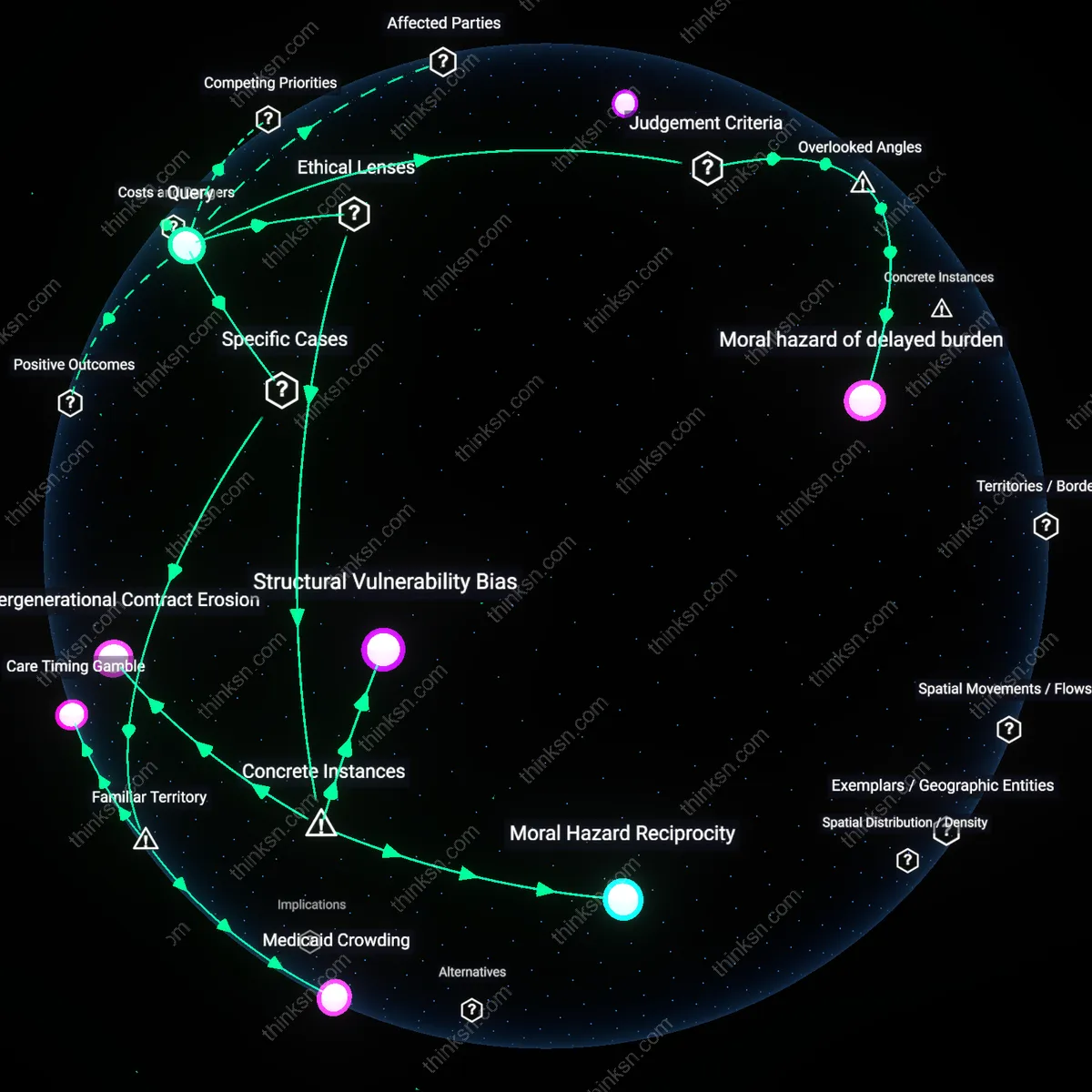
Moral hazard of delayed burden
Purchase private long-term care insurance now to protect future public systems from concentration risk among wealth-tier defectors. High-income households that delay care funding decisions shift actuarial strain onto Medicaid when their health deteriorates, increasing long-run public premiums and eligibility constraints for lower-income citizens; evidence indicates this quiet migration undermines horizontal equity in state-administered care pools. This dynamic is invisible in individual cost-benefit analyses, which ignore how clustered opt-outs at certain wealth thresholds destabilize risk aggregation at the population level, particularly in states like Florida and Arizona with rapidly aging populations and thin Medicaid margins.
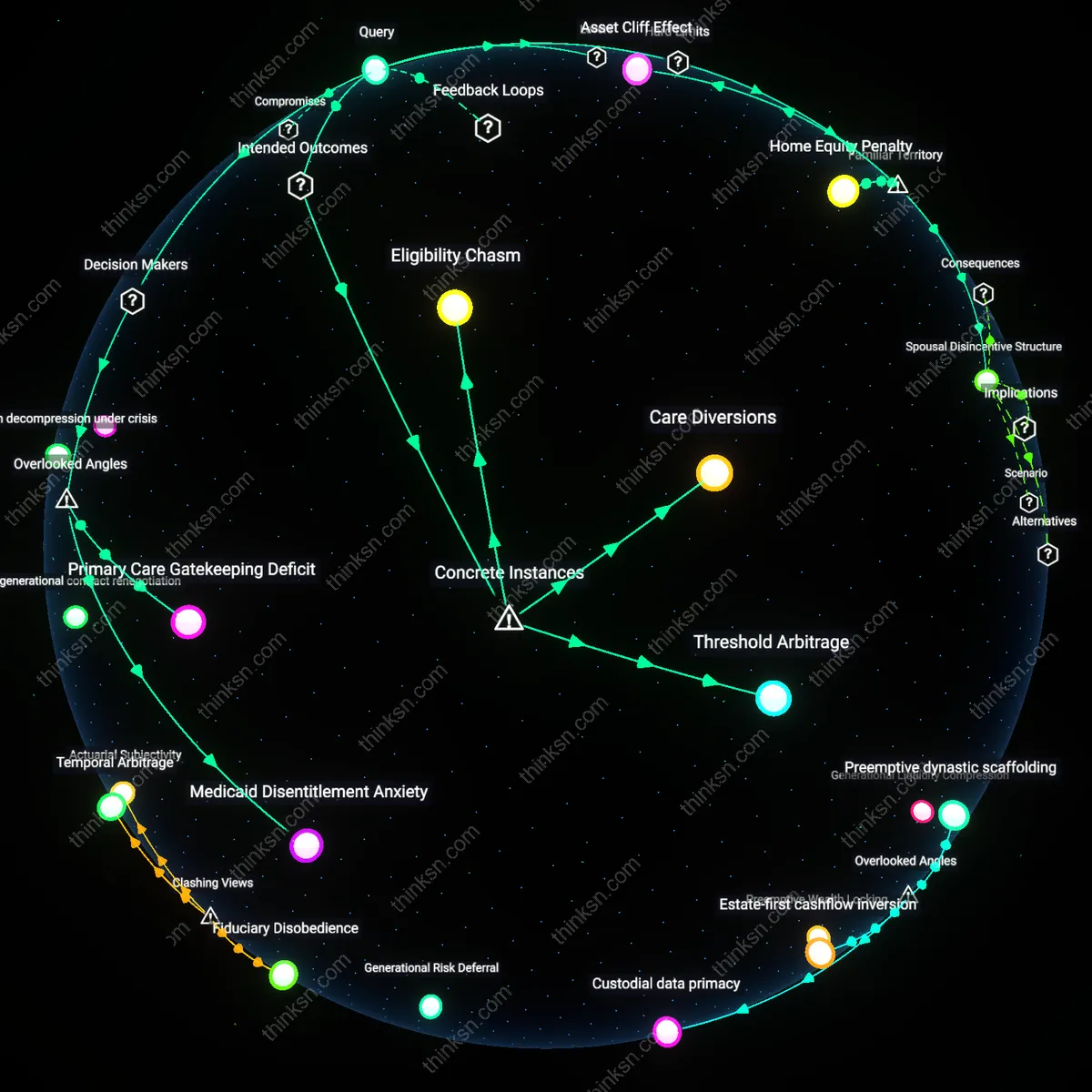
Temporal privilege of anticipatory capital
Recognize that the ability to weigh private insurance against Medicaid is itself a form of temporal wealth, accessible only to those whose health and employment permit long-term planning horizons. Workers in precarious or physically taxing jobs—such as warehouse logistics or home health aides—rarely reach the stable income and cognitive bandwidth required to evaluate LTC options before health shocks occur, locking them into Medicaid by default rather than choice. Research consistently shows that LTC decision-making is not a neutral calculation but a privilege of uninterrupted wellness, which means cost-balancing frameworks inadvertently exclude the majority who cannot engage them in time—revealing that the 'decision' itself is distributed unequally.
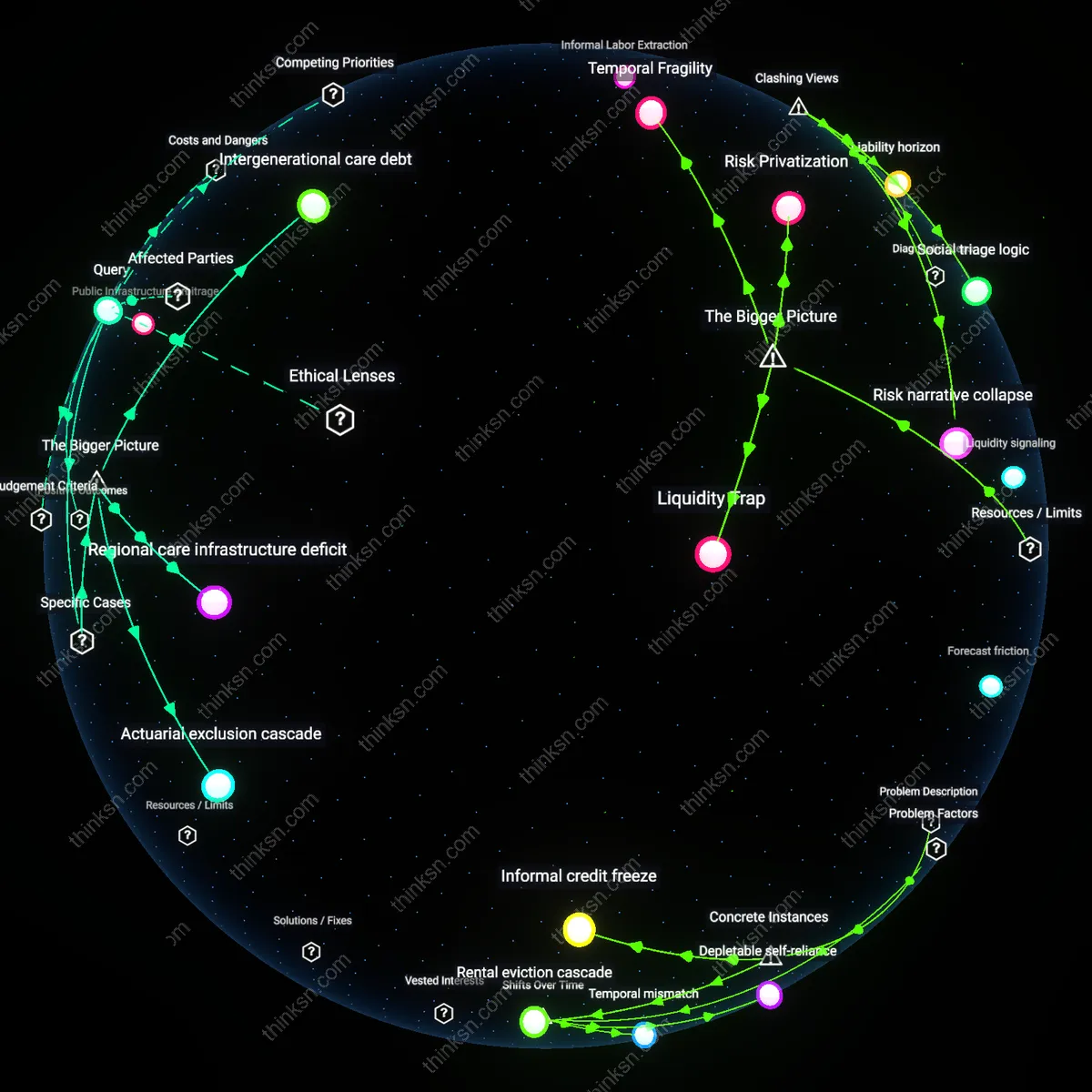
Intergenerational Contract Erosion
Purchase private long-term care insurance to preserve family autonomy under libertarian paternalism, as demonstrated by the 2006 California Partnership for Long-Term Care, where individuals who bought into the asset-protection linkage between private insurance and Medicaid eligibility preserved wealth without burdening public systems; this hybrid mechanism reveals how states incentivize personal responsibility while containing costs, yet its underappreciated consequence is the quiet shift of risk onto future generations who inherit diminished communal expectation of care.
Structural Vulnerability Bias
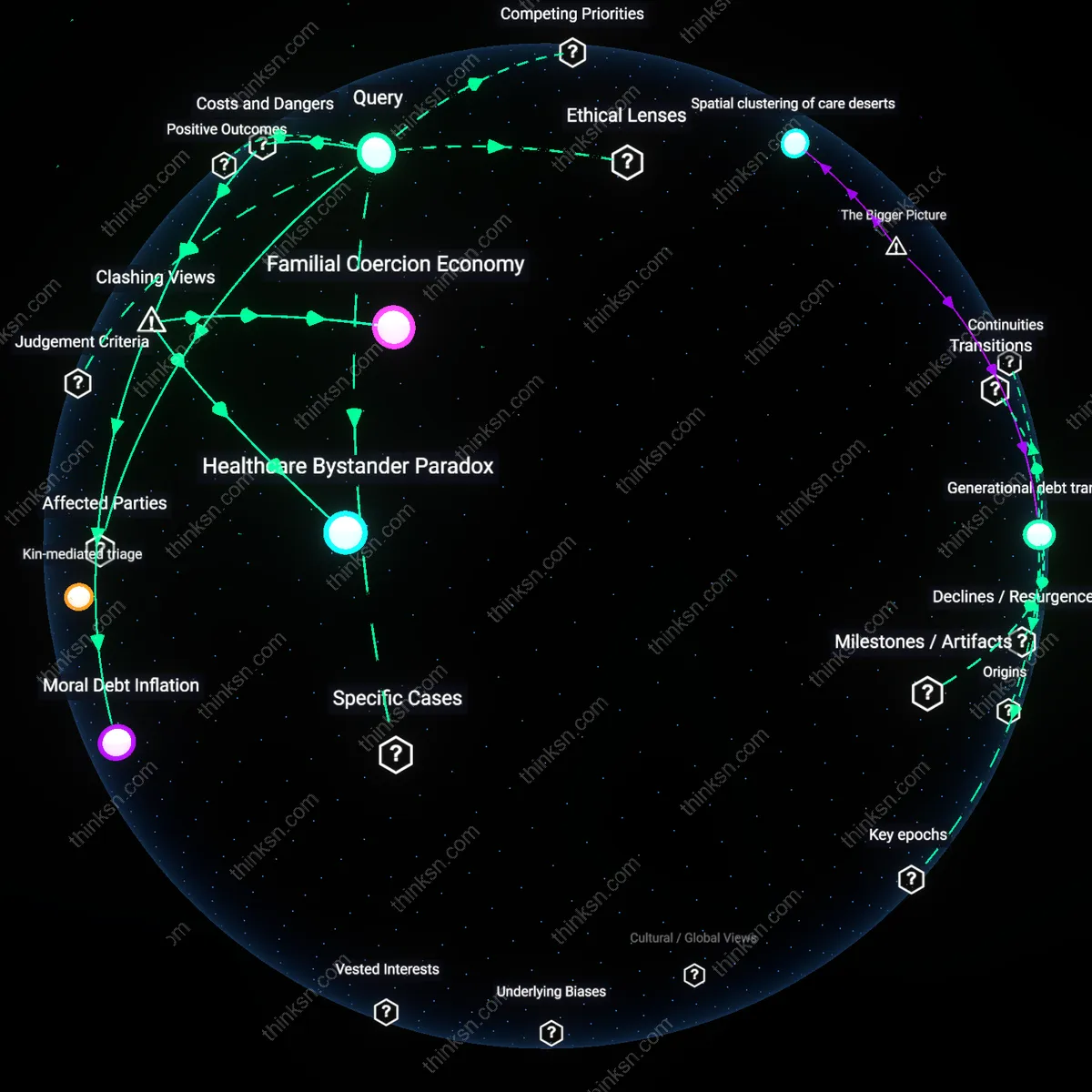
Rely on Medicaid as an ethical imperative grounded in Rawlsian justice, exemplified by Mississippi’s persistent underfunding of home- and community-based services after the 1999 Olmstead v. L.C. Supreme Court decision, where disabled individuals remained warehoused in institutions due to cost-shifting and racialized austerity politics; the non-obvious truth is that Medicaid access is systematically mediated by regional inequity, making reliance not a matter of personal planning but of exposure to structural abandonment.
Moral Hazard Reciprocity
Delay private policy purchase until late midlife to optimize cost-effectiveness under actuarial fairness, as seen in the post-2010 withdrawal of Genworth Financial from high-benefit inflation riders amid rising longevity among insured cohorts in Pennsylvania; what escapes conventional analysis is that insurers themselves recalibrate risk based on collective behavior, creating a feedback loop where responsible individualism undermines the very pool it depends on, exposing the reciprocal nature of moral hazard in private risk-sharing systems.
Medicaid Crowding
Purchase private long-term care insurance to avoid dependency on overburdened state Medicaid systems. As populations age in states like Florida and Arizona—where retiree density is high and Medicaid long-term care expenditures are growing—public programs face strain from rising enrollment, leading to provider shortages and restricted access; this creates a de facto rationing mechanism where eligibility does not guarantee timely or adequate care. The non-obvious implication is that Medicaid, while financially necessary for many, operates as a system of last resort shaped by regional capacity limits, not just individual need.
Care Timing Gamble
Rely on Medicaid eligibility planning through asset restructuring because the largest cost determinant in long-term care is the onset age of severe disability, a variable poorly captured by private insurance underwriting. Families in metropolitan areas like Cleveland or Pittsburgh, where industrial legacies produced chronic health burdens but uneven retirement savings, often engage in deliberate financial downshifts—such as transferring home equity—to meet Medicaid’s means test, betting that delays in cognitive or mobility decline will defer costs beyond their solvency horizon. The overlooked dynamic is that private insurance assumes predictability in health trajectory, while Medicaid dependency strategies treat longevity and disability onset as speculative variables too volatile to insure against actuarially.