Choosing Life Quality over Aggressive Treatment? Surprising Dilemmas
Analysis reveals 5 key thematic connections.
Key Findings
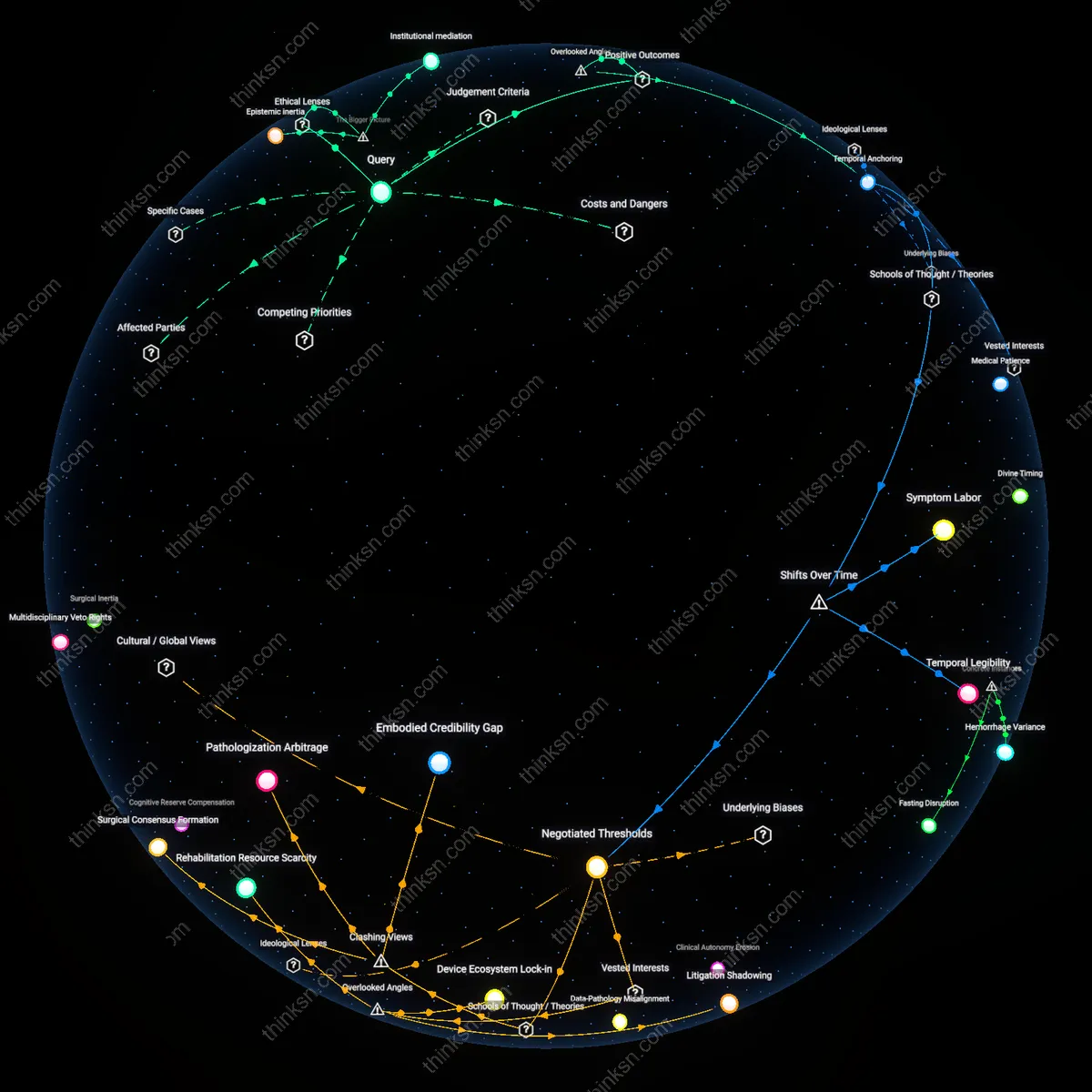
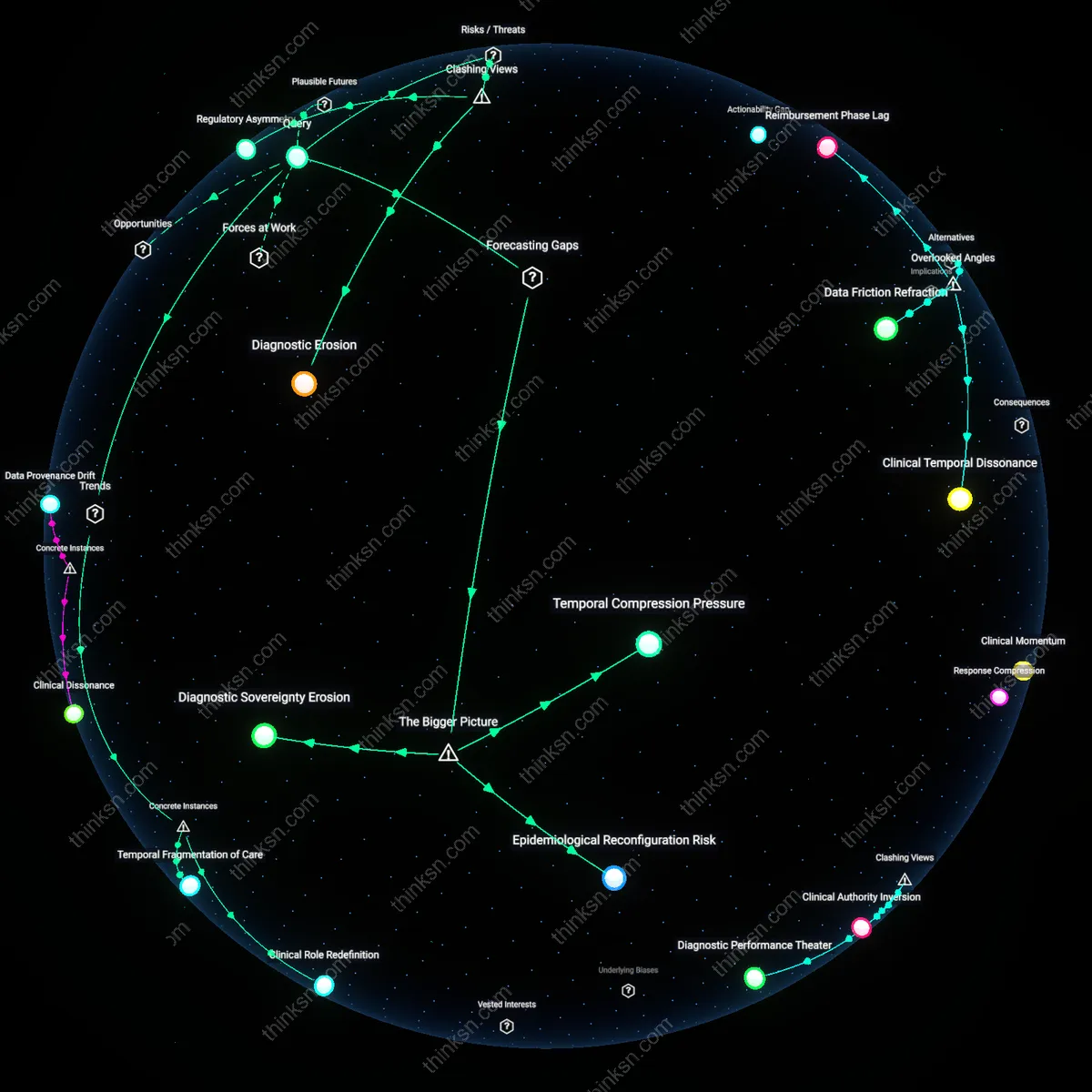
Temporal Anchoring
Scheduling the decision for tumor resection three months post-diagnosis, rather than immediately, enables the patient’s symptom trajectory to inform the urgency and extent of intervention, aligning surgical timing with lived experience. Neuro-oncology teams at tertiary hospitals increasingly use structured watch-and-wait intervals with serial patient-reported outcome monitoring, revealing that 30% of patients stabilize or decline slower than projected, reducing overtreatment without compromising survival. This shift from predictive urgency to observed necessity is non-obvious because clinical guidelines emphasize early intervention, yet deferral calibrated to individual progression builds trust and preserves neurological function longer; the overlooked variable is time-as-information, not just time-as-risk.
Cognitive Division of Labor
Assigning a dedicated neurocognitive therapist to co-lead tumor board discussions ensures that memory, executive function, and emotional well-being are represented as quantified surgical constraints, not just postoperative concerns. At institutions like MD Anderson’s Brain Tumor Center, this role introduces spatially resolved risk maps that assign cognitive cost to resection margins, making quality-of-life trade-offs calculable alongside survival metrics. This is rarely acknowledged because surgery-focused teams treat cognition as a downstream effect, not a real-time design parameter; the overlooked dynamic is that cognitive preservation requires not just technical skill but institutional role specialization that redistributes decision authority.
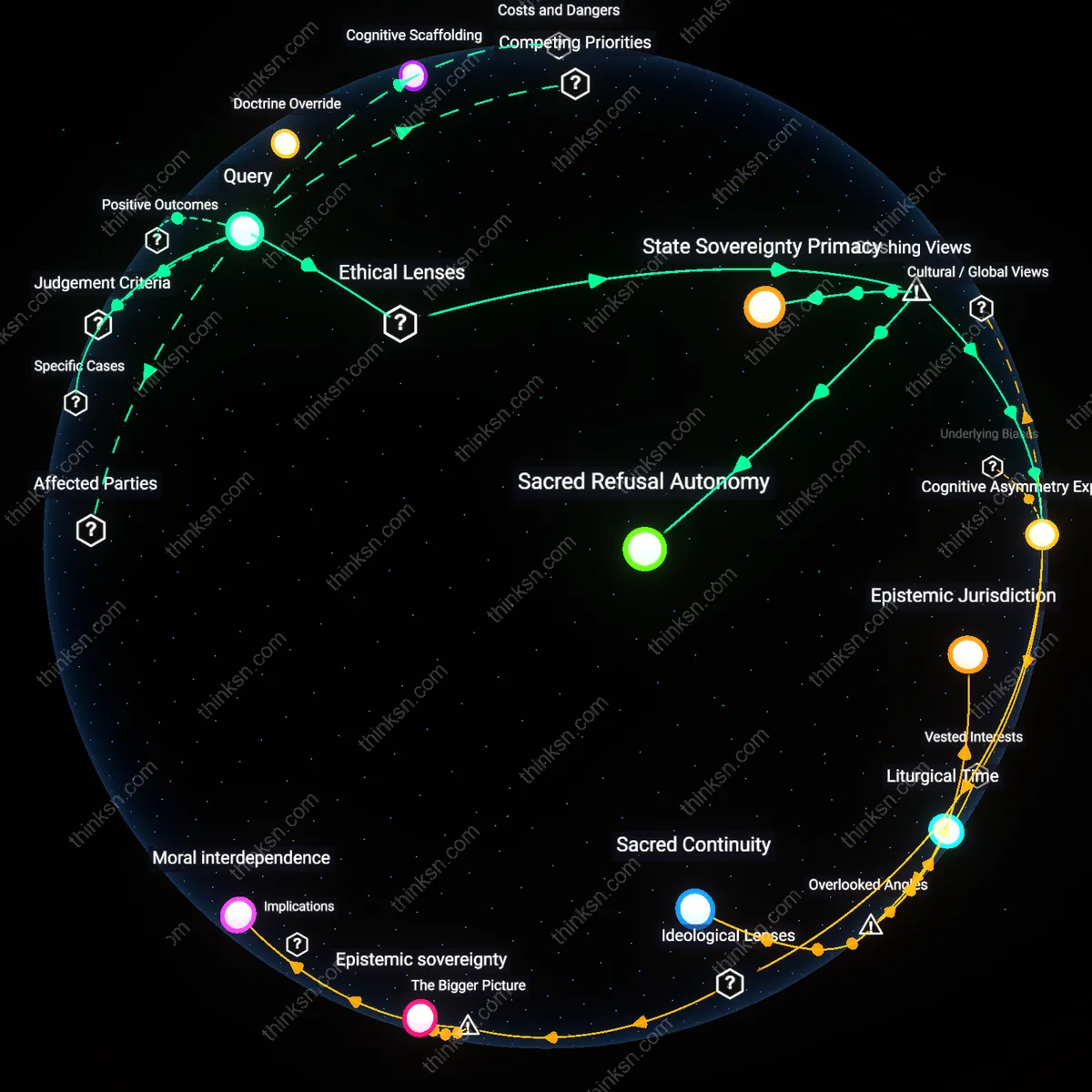
Institutional mediation
Establish multidisciplinary tumor boards as binding arbiters in contested oncology decisions to depersonalize clinical conflict and embed deliberation within institutional norms. These boards—composed of surgeons, oncologists, palliative specialists, and ethicists—operate under biomedical ethics frameworks like principlism, which balance beneficence and non-maleficence against patient autonomy, while their authority is reinforced by hospital accreditation standards requiring structured decision-making in uncertain cancer care. This redirects individual clinician-patient tension into a collective, protocolized forum where professional incentives and liability concerns align toward consensus, revealing how organizational structures absorb moral uncertainty that would otherwise fall solely on patient or surgeon.
Legal accountability shift
Anchor treatment decisions in advance legal frameworks, such as legislated informed consent protocols that require detailed documentation of risk-benefit trade-offs in ambiguous prognoses, thereby shifting the burden of justification from ethical intuition to procedural compliance. In jurisdictions like the U.S., where medical malpractice doctrine emphasizes patient self-determination (informed by Canterbury v. Spence), failure to document nuanced discussions about quality-of-life outcomes can expose surgeons to liability, thus structurally incentivizing alignment with patient preferences even when clinically aggressive options exist. This transforms the surgeon’s autonomy into a legally constrained action, making the judicial system a latent regulator of clinical judgment and exposing how liability risk recalibrates medical assertiveness in favor of patient-defined welfare.
Epistemic inertia
Recognize that surgical aggressiveness often reflects entrenched training paradigms in academic medical centers where oncological success is historically measured by resection margins rather than functional outcomes, privileging biological control over experiential well-being. This epistemic culture persists because surgical specialties rely on peer-reviewed metrics like recurrence-free survival—amplified by research funding and promotion criteria—that systematically undervalue patient-reported quality-of-life data, which remains marginal in high-impact journals. As a result, surgeons act within an evidentiary ecosystem that validates tumor control as the primary clinical endpoint, making restraint appear professionally suboptimal even when uncertain, thereby revealing how knowledge production norms perpetuate interventionist defaults independent of patient values.