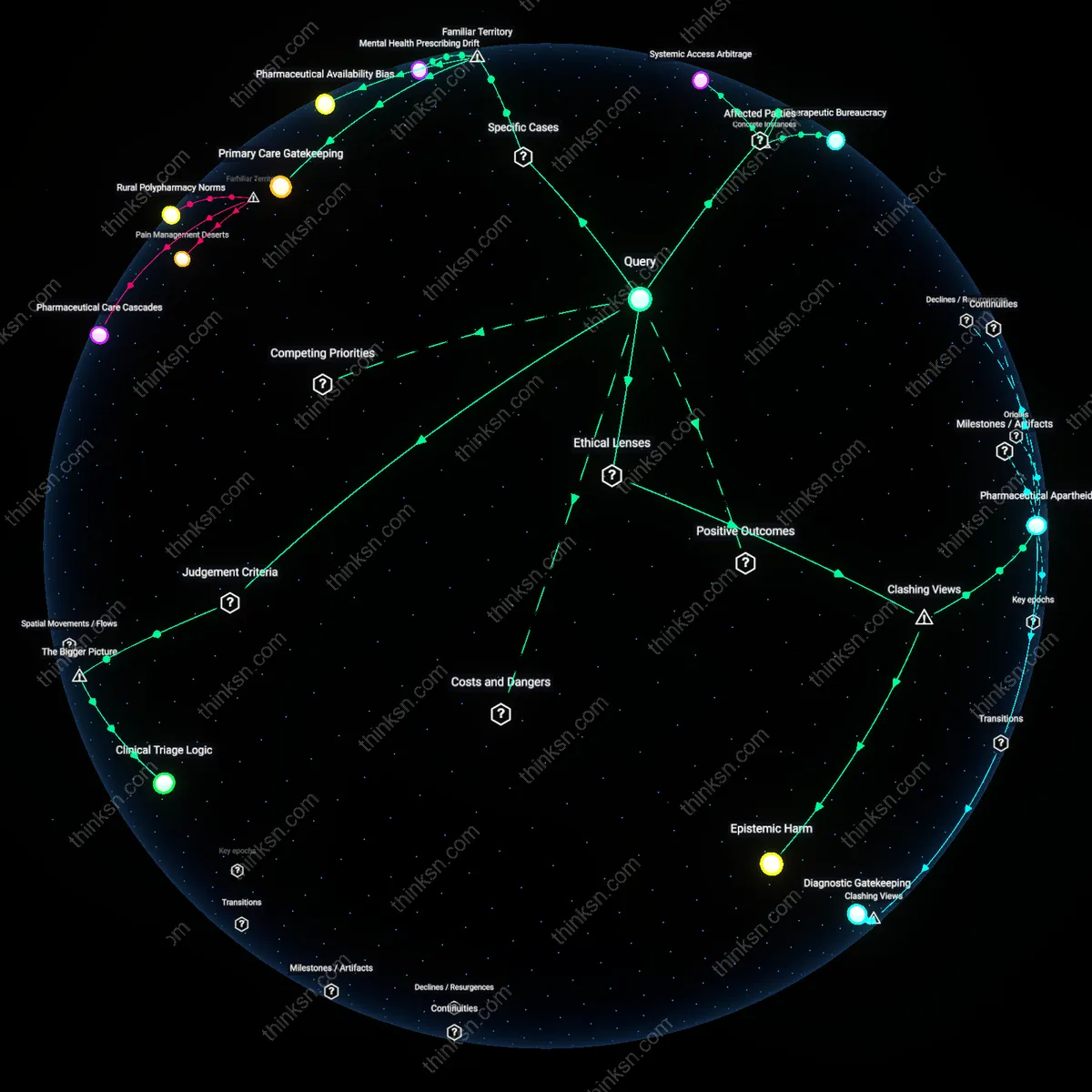
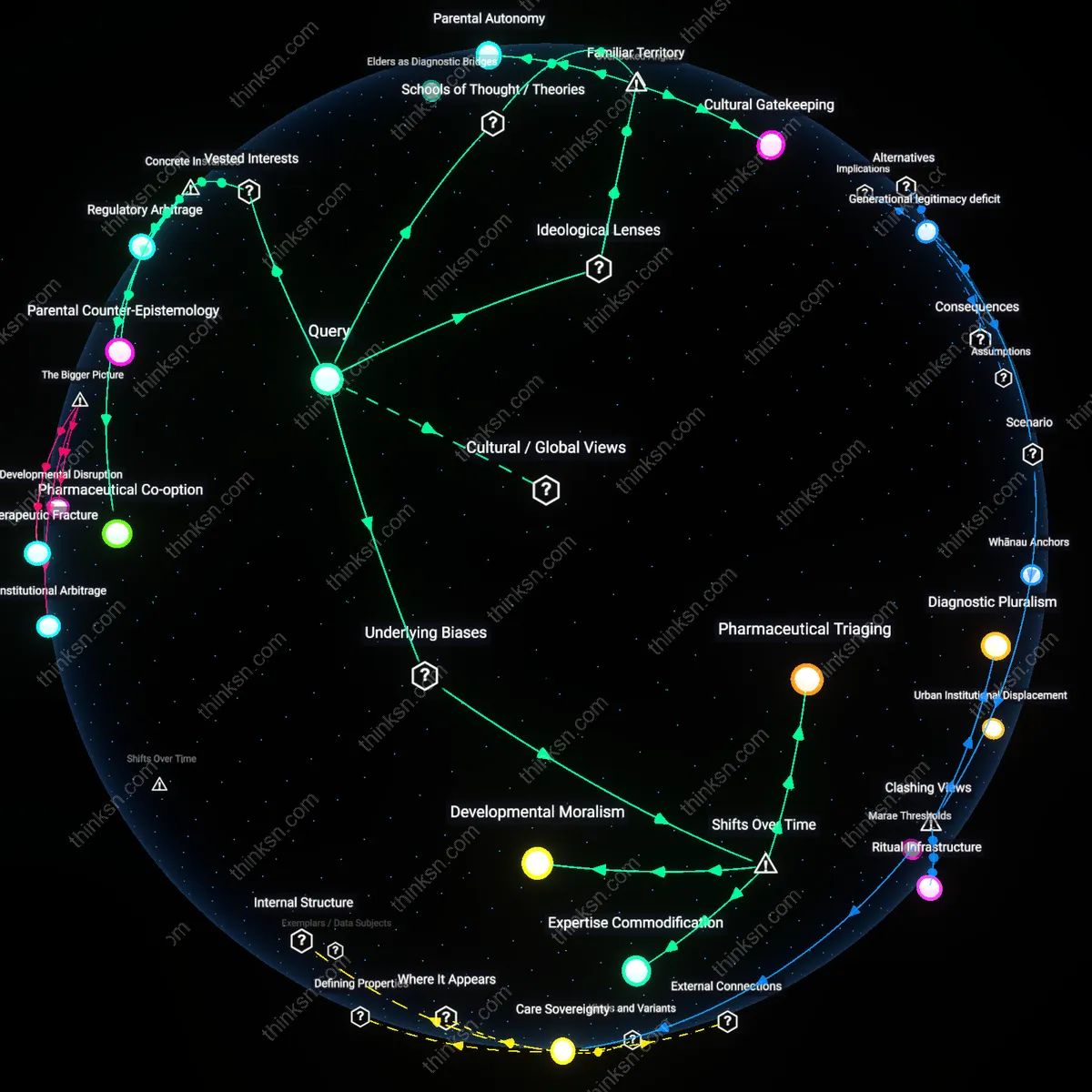
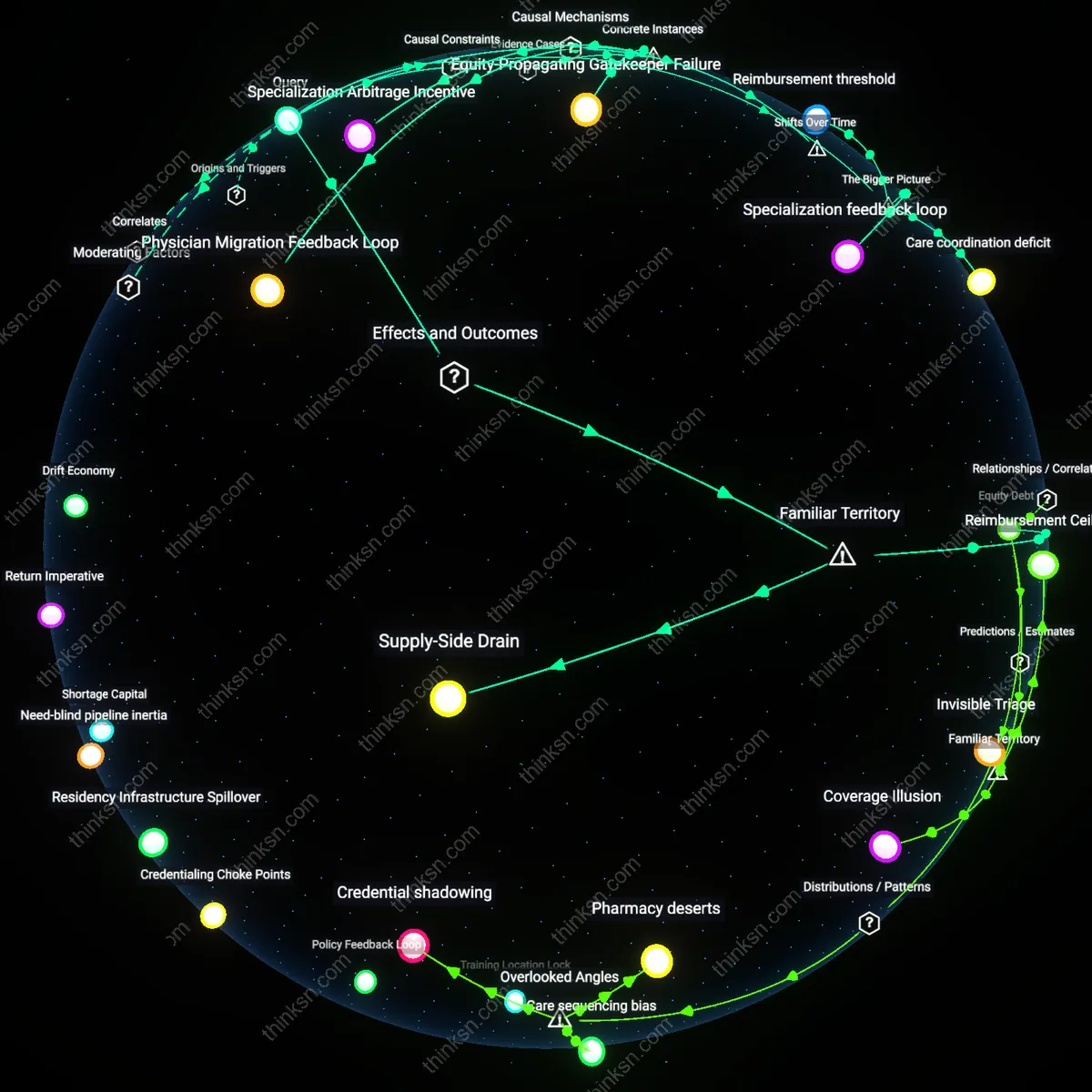
Medicate Mind or Body? Navigating Chronic Pain and Anxiety Trade-offs
Analysis reveals 10 key thematic connections.
Key Findings
Care Coordination Failure
A patient in rural West Virginia managing both fibromyalgia and generalized anxiety disorder must navigate separate Medicaid-restricted providers for mental health and pain, resulting in an unintentional benzodiazepine-opioid co-prescription that escalates overdose risk—this outcome stems not from individual clinician error but from structural misalignment between behavioral health and primary care under siloed reimbursement models, revealing how fragmented eligibility criteria rather than clinical complexity primarily drive polypharmacy dangers in underserved regions.
Systemic Access Arbitrage
In 2018, the launch of the Kaiser Permanente Colorado Integrated Pain and Behavioral Health Program allowed primary care teams to co-locate psychologists and pain specialists, reducing new opioid initiations by 40% over three years among patients with comorbid depression and chronic back pain—this shift occurred not because pharmacological options were eliminated, but because behavioral interventions became systematically easier to access than prescriptions, demonstrating how adjusting institutional workflow inertia can quietly reshape treatment selection more effectively than guideline changes or patient education.
Therapeutic Bureaucracy
Following the 2016 CDC Opioid Guideline release, Veterans Health Administration clinics in Minneapolis began requiring PTSD and chronic pain patients to enroll in Cognitive Processing Therapy before authorizing long-term oxycodone renewals, effectively using administrative gatekeeping to steer multimorbid individuals toward integrated care—not because psychotherapy was proven superior for pain relief, but because the VHA’s centralized electronic health record and accountability metrics allowed policy to be operationalized as clinical ritual, exposing how bureaucratic enforceability, not evidence strength, often determines which treatment pathway becomes the path of least resistance.
Clinical Triage Logic
Prioritize integrated behavioral health care because it aligns with clinical triage logic that deprioritizes high-risk polypharmacy in comorbid conditions under fragmented insurance coverage; this approach is driven by frontline providers in safety-net clinics who must navigate conflicting treatment guidelines and limited formulary access, using risk stratification tools to avoid opioid initiation when anxiety could be exacerbated by sedation or psychiatric side effects. The systemic pressure of disjointed reimbursement between mental health and primary care incentivizes bundled psychosocial interventions over specialist referrals, making collaborative care models the default despite underfunding—what’s underappreciated is that this 'default' functions as a de facto gatekeeping mechanism shaped less by patient preference than by payer-driven care rationing.
Pharmaceutical Entanglement
Choose psychiatric medication cautiously, recognizing that off-label use of SSRIs or SNRIs for pain reflects pharmaceutical entanglement in chronic pain management, where drug development economies favor repurposing psychotropics over funding non-opioid analgesic innovation; academic pain centers and VA systems increasingly adopt these regimens due to regulatory aversion to opioids post-2016 CDC guidelines, but this shift entrenches reliance on medications that require slow titration and carry sexual or gastrointestinal side effects poorly tolerated by anxiety sufferers. The non-obvious consequence is that pharmaceutical workarounds become medically rational at the individual level while reinforcing polypharmacy as a systemic norm, particularly when insurers reimburse pharmacotherapy more readily than psychological services.
Pharmaceutical Apartheid
Such a patient should, in many cases, opt for psychiatric medication over opioid management because regulatory risk aversion has produced a de facto Pharmaceutical Apartheid, in which Black and low-income patients are systematically denied opioids but prescribed psychotropics at higher rates, while wealthier, white patients receive opioid prescriptions under the guise of pain legitimacy. This distribution is ethically grounded in a neoliberal distortion of utilitarianism—where public health risk is calculated per population, not person—making the 'choice' of psychiatric drugs less a clinical preference and more a foreclosed alternative under racialized regulatory regimes. The dissonance lies in reframing medication selection not as patient autonomy but as enforced pharmacological stratification.
Epistemic Harm
The patient should reject both opioid management and standalone psychiatric medication in favor of integrated behavioral health care because polypharmacy risk is not primarily physiological but epistemic—doctors treating pain or anxiety in isolation produce Epistemic Harm by erasing the causal entanglement of the conditions, a fragmentation reinforced by fee-for-service models that reward discrete diagnoses over holistic understanding. This occurs within a healthcare imaginary shaped by Cartesian dualism in medical training and insurance coding, where billing categories preclude the recognition of co-occurring disorders as a unified clinical reality. The underappreciated point is that choosing integration is not therapeutic pragmatism but resistance to institutional epistemologies that pathologize complexity.
Primary Care Gatekeeping
Patients should default to integrated behavioral health care because primary care clinics—such as federally qualified health centers in rural Appalachia—are structured to triage both anxiety and chronic pain through colocated psychological and medical services, reducing polypharmacy risks by limiting independent prescribing across fragmented specialists. These clinics operate under value-based care models that incentivize non-opioid, non-psychotropic first-line interventions and rely on care managers to coordinate treatment—making them the most accessible and systemically coordinated option in regions where opioid overprescription and mental health deserts are historically entrenched. The non-obvious insight is that primary care, often seen as a bottleneck, becomes a protective filter against polypharmacy precisely because its limited resources enforce stricter treatment integration.
Pharmaceutical Availability Bias
Someone with anxiety and chronic pain is more likely to receive opioid management when treated in for-profit specialty pain clinics—such as those historically tied to OxyContin distribution networks in West Virginia—because these clinics are financially incentivized to offer rapid, pharmacologic solutions that align with patient demand for immediate relief and insurer preferences for short appointment durations. The mechanism is a care cascade shaped by drug availability, prescriber habit, and patient expectation, where opioids become the path of least resistance despite comorbid anxiety being worsened by sedation and dependence. The underappreciated reality is that pharmaceutical access, not clinical need, often determines treatment entry points in fee-for-service environments, reinforcing the public’s intuitive association between pain clinics and opioids.
Mental Health Prescribing Drift
Psychiatric medication is often prioritized in urban university-affiliated clinics—like those within the Massachusetts General Hospital system—where anxiety is clinically foregrounded and chronic pain is interpreted through a somatization or central sensitization lens, leading to SSRIs or SNRIs as first-line treatment regardless of pain severity. This reflects a diagnostic hierarchy in academic medicine where mental health symptoms are treated as drivers of physical complaints, and where opioid avoidance is a deeply institutionalized response to the addiction crisis. The overlooked consequence is that pain relief may be delayed or insufficient, not due to misuse risk, but because the epistemic authority of psychiatry in these settings redefines pain as a behavioral manifestation, making pharmacological mood regulation the default intervention.