Is Insurer Appeal Just Procedure or Real Reconsideration?
Analysis reveals 6 key thematic connections.
Key Findings
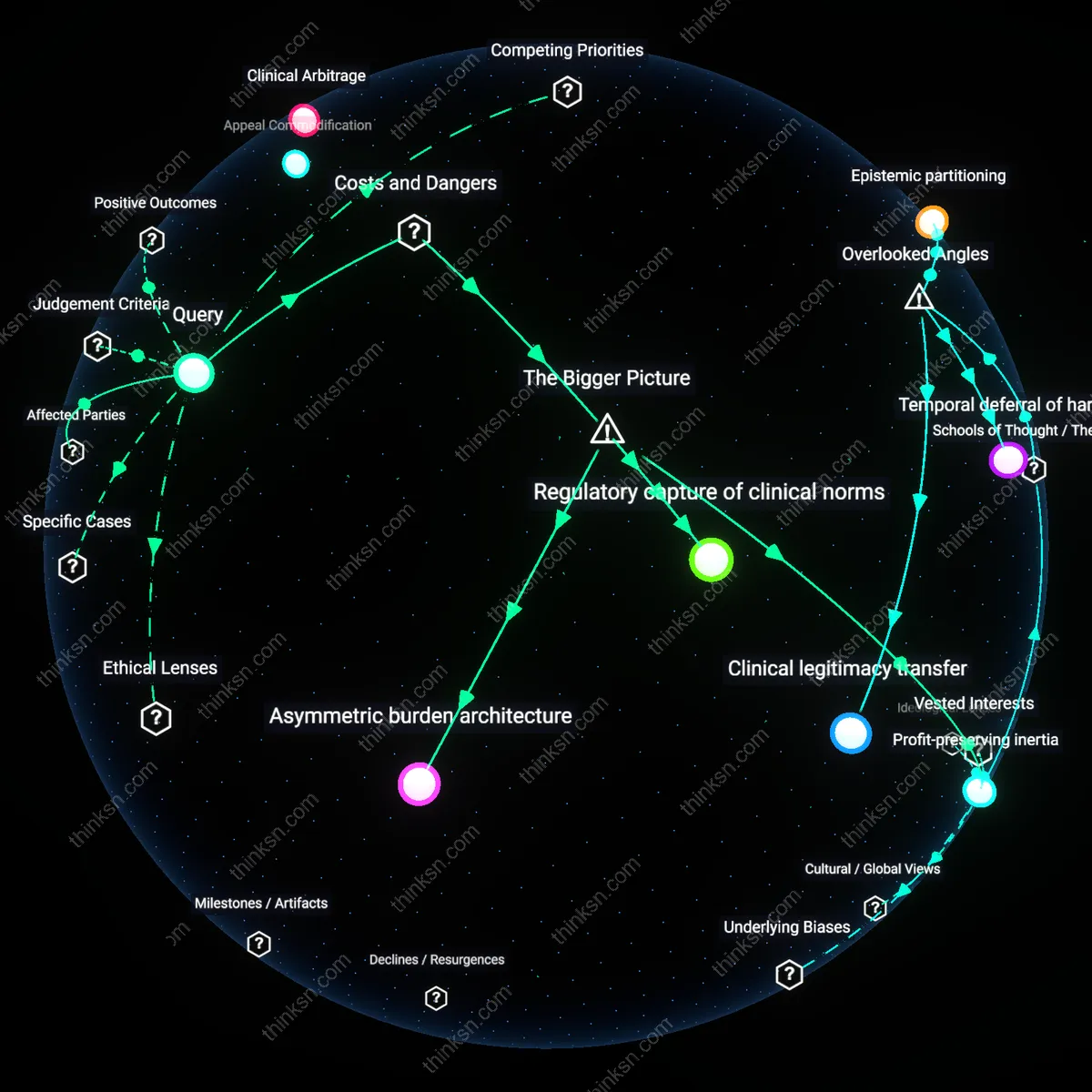
Appeal Commodification
The insurer's internal appeal process has shifted from a clinician-led review to a metrics-driven administrative function, transforming reconsideration into a standardized output. Since the 2000s, managed care organizations expanded tiered review systems staffed by contracted nurses and physician assistants operating under time quotas and corporate performance indicators, prioritizing throughput over clinical nuance. This institutionalization of speed and uniformity, justified by compliance with Affordable Care Act reporting requirements, hollowed out case-by-case reevaluation—especially for marginal or complex claims—revealing that the process now functions less as medical scrutiny than as a compliance ritual producing audit-ready documentation. The underappreciated consequence is that clinical disagreement is no longer resolved but absorbed into a risk-mitigating procedural artifact.
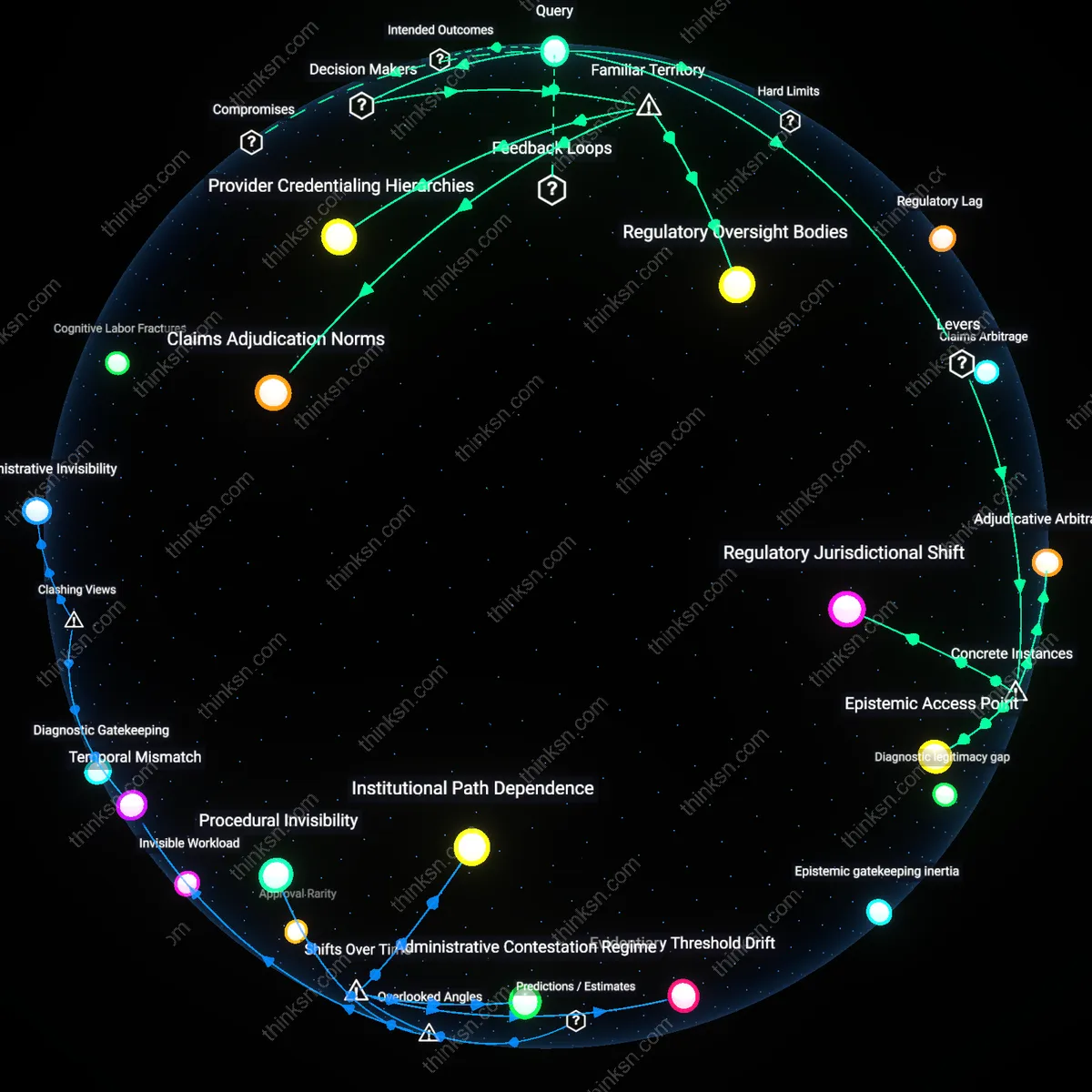
Regulatory Mimicry
Following the 1996 HIPAA appeals provisions and accelerated by post-2010 insurance market consolidation, insurer appeal procedures evolved to mimic legal adjudication without granting equivalent authority, creating a façade of review for regulatory visibility. Centralized appeals units in companies like UnitedHealthcare and Aetna adopted courtroom-like language—'new evidence,' 'independent reviewers'—yet constrained decision-makers with pre-approved templates and non-binding external reviews, ensuring alignment with actuarial models rather than clinical standards. This ritualized structure emerged not from clinical demands but from state and federal oversight requiring 'fair process,' allowing insurers to demonstrate compliance while insulating underwriting assumptions from substantive challenge—making the appeal process a performance of accountability rather than a mechanism of correction.
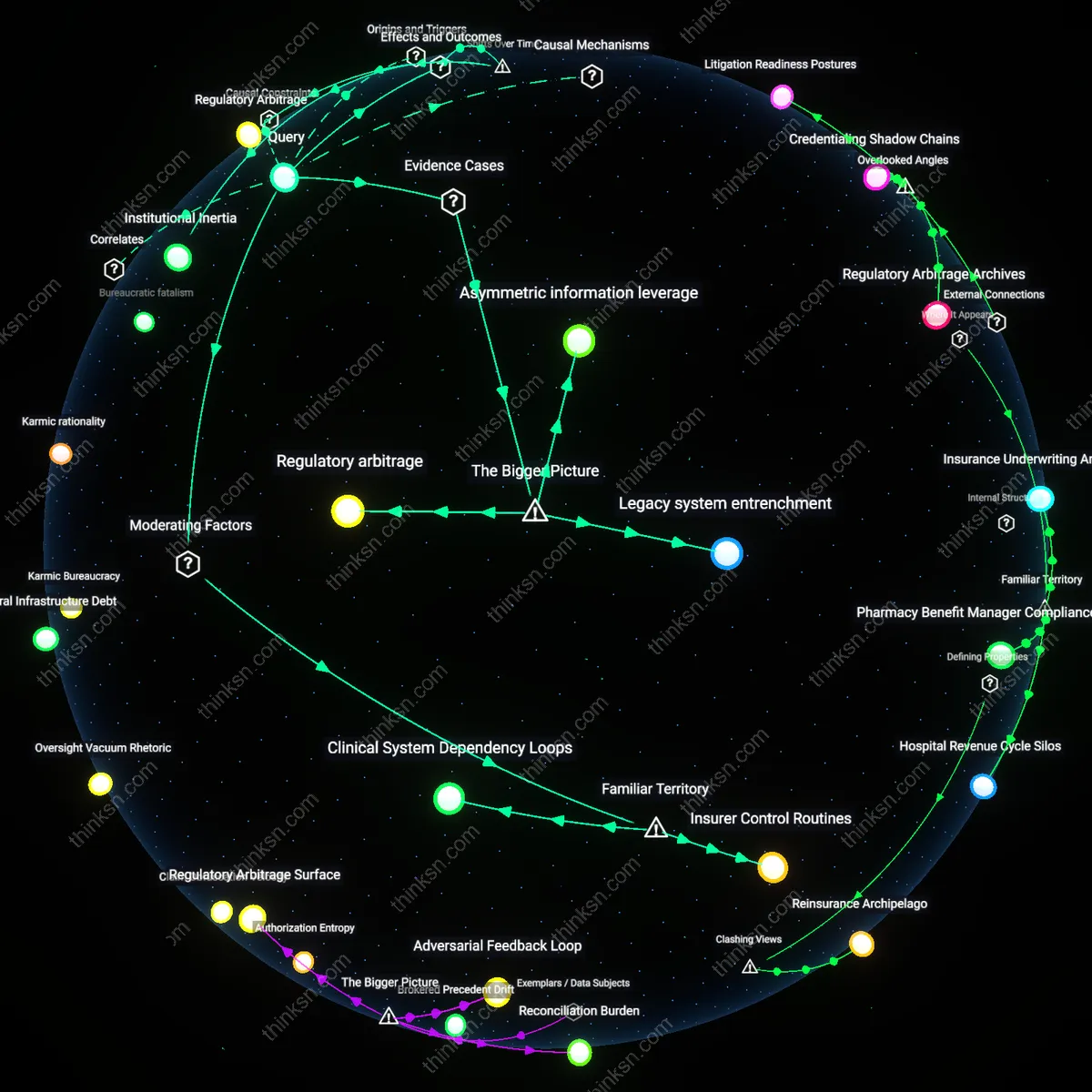
Clinical Arbitrage
Beginning in the 1990s with the rise of proprietary clinical guidelines like InterQual and Milliman, insurers shifted appeal outcomes from individual provider judgment to algorithmic criteria, redefining 'reconsideration' as rule-based validation rather than medical discourse. Utilization management departments began training non-treating physicians to apply decision trees aligned with cost-containment benchmarks, systematically displacing treating clinicians’ contextual assessments with binary compliance checks. This pivot to quantifiable protocols, especially after 2005 when CMS incentivized standardized care pathways, recast appeals as verification of data inputs rather than interpretation of patient need—revealing that the process no longer mediates clinical disagreement but arbitrates between epistemic regimes, privileging codified rules over embodied expertise.
Profit-preserving inertia
An insurer's internal appeal process does not genuinely reconsider rejected clinical justifications because the adjudicators operate within risk-averse medical management units that are structurally incentivized to uphold initial denials to avoid setting precedents that could expand coverage and erode underwriting margins; this replication of denial logic under a veneer of review persists because overturning claims introduces downstream actuarial uncertainty, which finance divisions actively suppress through performance metrics tied to denial uphold rates. The mechanism is embedded in cross-departmental accountability structures where medical directors answer to CFOs, not clinicians, making the appeal process a ritualized confirmation of cost-containment imperatives rather than a clinical reassessment—what is underappreciated is that the process is designed not to fail, but to *succeed* as a stabilization device for financial predictability.
Regulatory capture of clinical norms
Insurer appeal outcomes rarely shift because the clinical guidelines used to justify initial denials are self-referential instruments developed in-house or sourced from industry-aligned entities like Milliman Care Guidelines, which are then shielded from external scrutiny during appeals by citing proprietary methodology; appeal reviewers are contractually bound to work within these frames, rendering challenges to medical necessity inherently circular. The system functions through a feedback loop where state insurance departments accept these guidelines as 'evidence-based' without independent validation, enabling insurers to outsource rationing decisions to ostensibly neutral standards that are in fact calibrated to utilization targets—what remains obscured is that regulation does not merely fail to correct the process, but actively certifies its legitimacy, making appeals a procedural capture of medicine by actuarial governance.
Asymmetric burden architecture
The appeal process systematically disadvantages providers by requiring them to reconstruct and resubmit entire clinical dossiers under tight deadlines while insurers face no reciprocal obligation to justify denials with real-time documentation or peer-reviewed benchmarks, ensuring that cognitive and administrative labor stacks against the treating team. This imbalance persists because accreditation bodies like URAC evaluate appeal 'accessibility' based on timeliness and format compliance rather than outcome equity or evidentiary rigor, creating a façade of due process without correcting for structural power differentials in information control; the underappreciated consequence is that the appeal system functions not as a corrective mechanism but as a depletion strategy, where the cost of persistence falls entirely on clinicians until they disengage—thus automating denial through exhaustion.