When Does a Gene Cure Cross the Ethics Line?
Analysis reveals 8 key thematic connections.
Key Findings
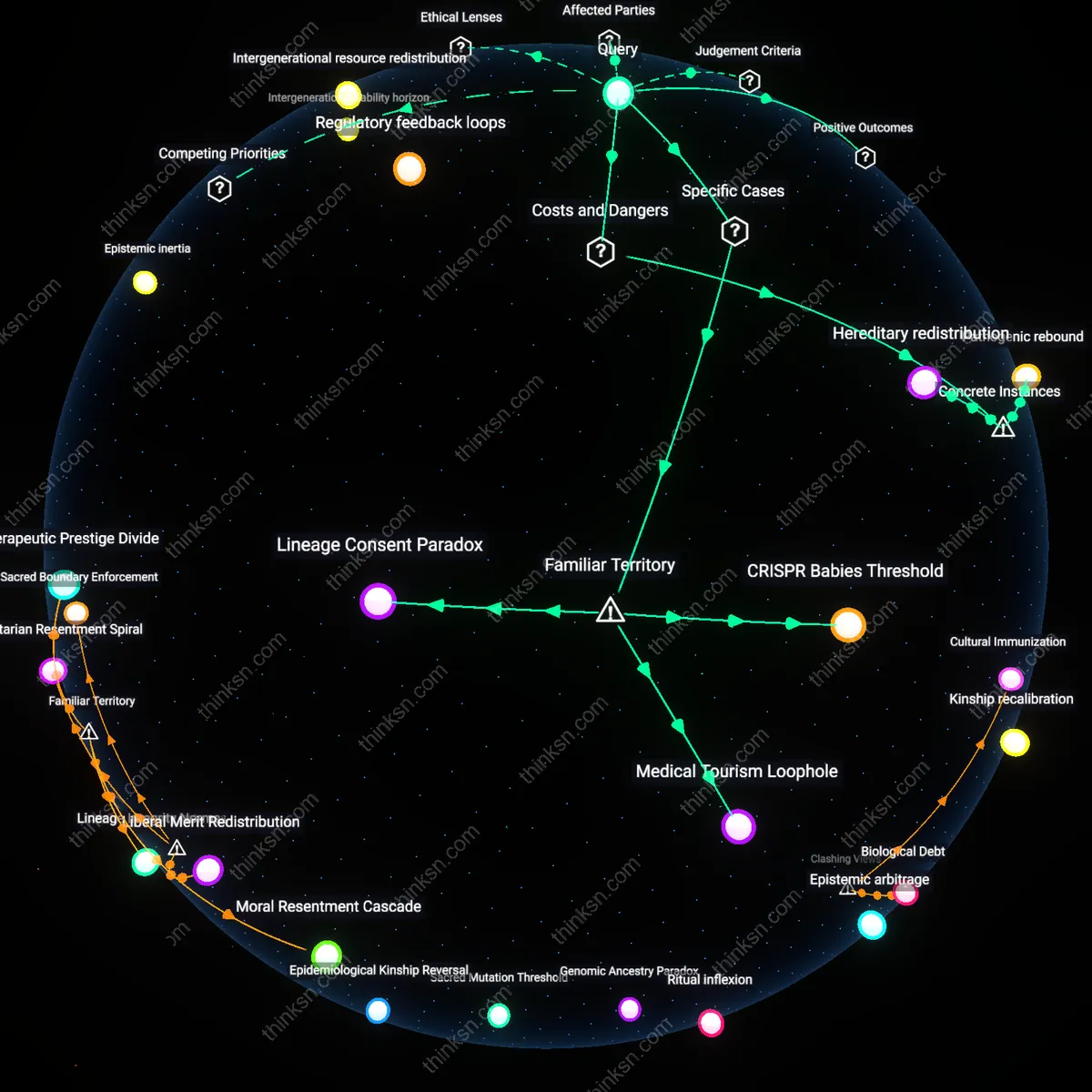
Regulatory feedback loops
Germline gene editing enhances disease eradication in populations only when clinical applications trigger adaptive governance that evolves in tandem with technical capabilities. National regulatory agencies, such as the FDA and EMA, respond to early-stage trials by refining oversight protocols, which in turn enable safer, more targeted interventions—creating a self-reinforcing cycle where public trust and scientific rigor co-develop. This dynamic is underappreciated because most ethical debates assume static regulation, whereas in reality, real-time policy learning amplifies therapeutic utility when oversight is designed to absorb and respond to clinical data, turning risk into systematic resilience.
Epidemiological tipping points
The positive impact of germline editing becomes transformative when interventions reduce the carrier frequency of deleterious alleles below the threshold required for population-level disease persistence, particularly in geographically or culturally isolated communities with high consanguinity rates. In regions like the Baltic states or parts of the Gulf Cooperation Council, where recessive disorders such as spinal muscular atrophy have high prevalence, targeted editing programs could collapse transmission networks through networked kinship structures. The overlooked mechanism here is the nonlinear decline in disease incidence once a critical proportion of future generations are edited—resembling herd immunity but for genetic conditions, powered by kinship demography.
Intergenerational resource redistribution
Germline gene editing yields net societal benefit when healthcare cost savings from preventing monogenic diseases are reinvested into prenatal and neonatal care infrastructure, particularly in middle-income countries undergoing demographic transition. Systems like Brazil’s Unified Health System could redirect long-term expenditures on chronic management of conditions like sickle cell disease toward scalable reproductive health services, creating a fiscal cascade that elevates baseline care. The unseen driver is the temporal arbitrage—upfront editing costs are offset by delayed, compounding savings, which only become actionable when health financing mechanisms are structured to value intergenerational equity over short-term budgeting cycles.
Hereditary redistribution
In 2020, when the UK’s HFEA considered mitochondrial replacement therapy (MRT) for preventing Leigh syndrome transmission, it revealed how germline interventions can reconfigure kinship and inheritance outside medical intent—resulting in children with DNA from three individuals and altering legal and social frameworks around parenthood. The procedure operated through ooplasmic transfer in Newcastle clinics, where paternal mitochondria were replaced to avoid maternal transmission, yet the systemic consequence was a redistribution of genetic lineage claims across familial, legal, and identity domains. The underappreciated risk here is not mutation but ontological reclassification—how treating one hereditary disease triggers societal renegotiation of biological descent.
Pathogenic rebound
In Sardinia, decades of selective pressure from malaria eradication intensified the prevalence of beta-thalassemia despite public health efforts, illustrating how suppressing one hereditary condition can inadvertently elevate another genetically linked disorder when environmental constraints shift. Germline editing aimed at eliminating thalassemia could replicate this dynamic if edits disrupting HBB mutations simultaneously impair fetal hemoglobin regulation or stress response pathways, creating new selective advantages for alternative pathologies under unknown future conditions. The non-obvious danger lies not in the edit’s failure but its success—eliminating a disease allele today may collapse evolutionary buffers that protect against emergent health crises tomorrow.
CRISPR Babies Threshold
The ethical concerns of germline gene editing surpass its potential benefits when a national scientific program advances to the point of producing genetically modified live births intended to confer disease resistance, as occurred with He Jiankui’s 2018 creation of CCR5-edited infants in China to prevent HIV transmission. This event marked a definitive crossing of the clinical ethics boundary because it deployed heritable genome changes outside established safety protocols, bypassed meaningful consent, and exploited a public health rationale familiar to most people—preventing infection—that could not justify the unknown multigenerational risks. What is non-obvious is that the very intuitiveness of using gene editing as a shield against illness made the experiment socially plausible despite its ethical overreach, revealing how protective narratives can camouflage premature application.
Medical Tourism Loophole
Ethical concerns exceed medical benefits when germline editing migrates from regulated research environments in countries like the U.S. or Germany to jurisdictions with permissive oversight, such as certain private fertility clinics in Southeast Asia or Eastern Europe offering experimental gene modification to foreign patients. These cross-border clinics leverage the widespread familiarity with 'designer baby' anxieties to market speculative services under the guise of treating hereditary disorders, effectively turning public fear into a business model. The underappreciated reality is that the moral threshold isn’t crossed solely in labs but in markets—where the intuitive association between genetic medicine and eugenics is monetized, making ethical erosion a consequence of accessible, for-profit innovation.
Lineage Consent Paradox
Germline editing becomes ethically indefensible when interventions affect not only the individual patient but also all their descendants, as seen in proposed mitochondrial replacement therapy programs in the UK, where 'three-parent babies' were approved to prevent inherited metabolic diseases. While the medical intent aligns with common expectations of stopping generational suffering, the innovation implicitly overrides future generations’ autonomy—a consent they cannot give—under the familiar narrative of parental love shielding children from harm. The overlooked contradiction is that the more deeply we embed germline editing into accepted family-protective instincts, the more easily we obscure its irreversible, intergenerational imposition.