Do Big Pharma Lobbying Efforts Overshadow Independent Medical Research?
Analysis reveals 12 key thematic connections.
Key Findings
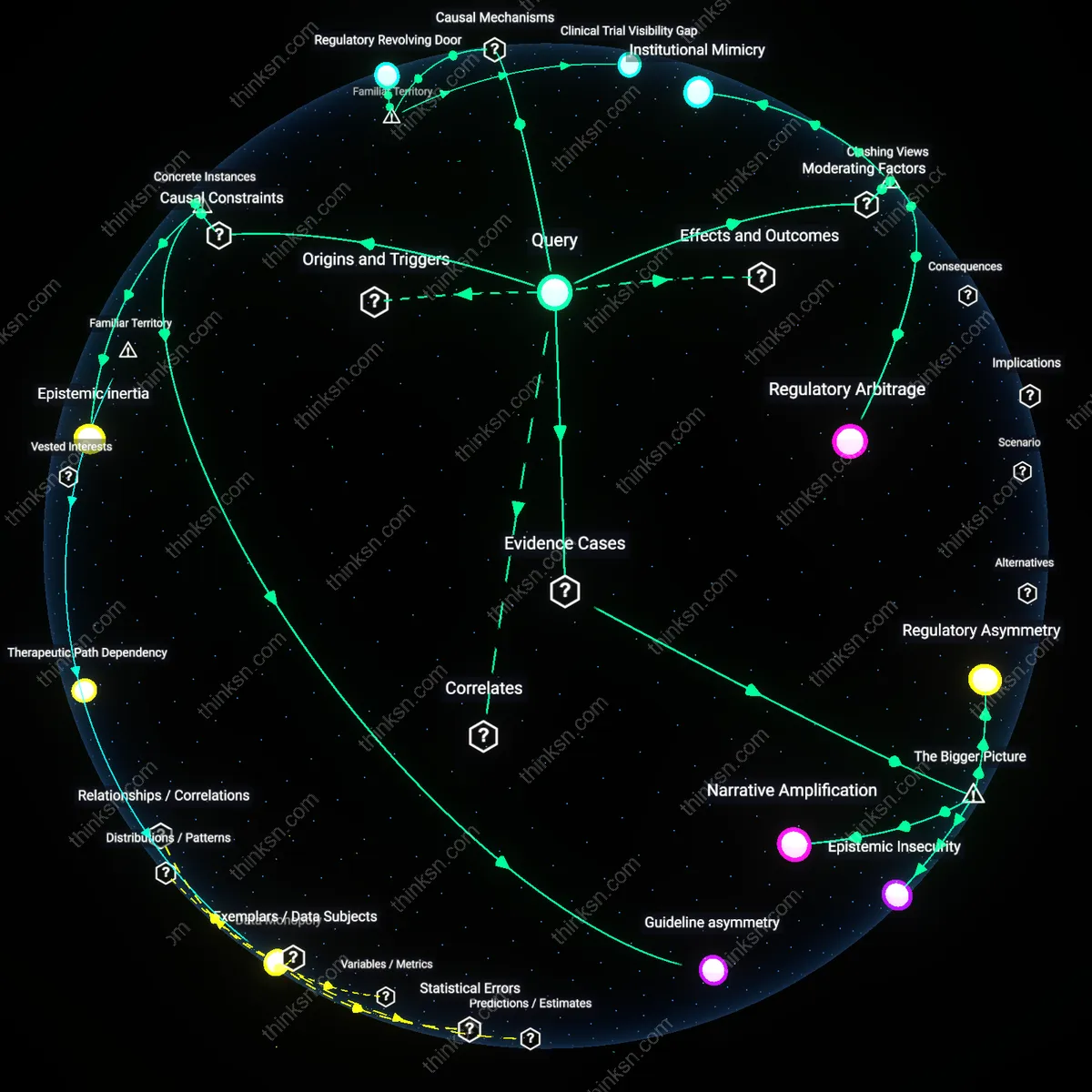
Regulatory Revolving Door
Big pharma shapes medical guidelines through direct placement of former executives and lobbyists into regulatory agencies like the FDA and EMA, where they influence approval standards and advisory panel decisions. This pathway functions through structured career mobility between industry and oversight bodies, enabling informal but durable alignment between commercial priorities and regulatory science. What feels like institutional independence is often habitually undermined by shared professional networks and tacit norms of cooperation, a dynamic invisible to public scrutiny but decisive in shaping outcome.
Clinical Trial Visibility Gap
Medical guidelines appear swayed by big pharma because industry funds over 60% of late-phase clinical trials, controlling data access, publication timing, and authorship lists, which systematically skews the evidence base toward favorable outcomes. Independent researchers rarely have equivalent resources or access to raw data from these trials, creating a perception gap where the volume and visibility of industry-generated science mimics scientific consensus. The underappreciated mechanism is not overt coercion but epistemic dominance—the ability to set the terms of what counts as evidence.
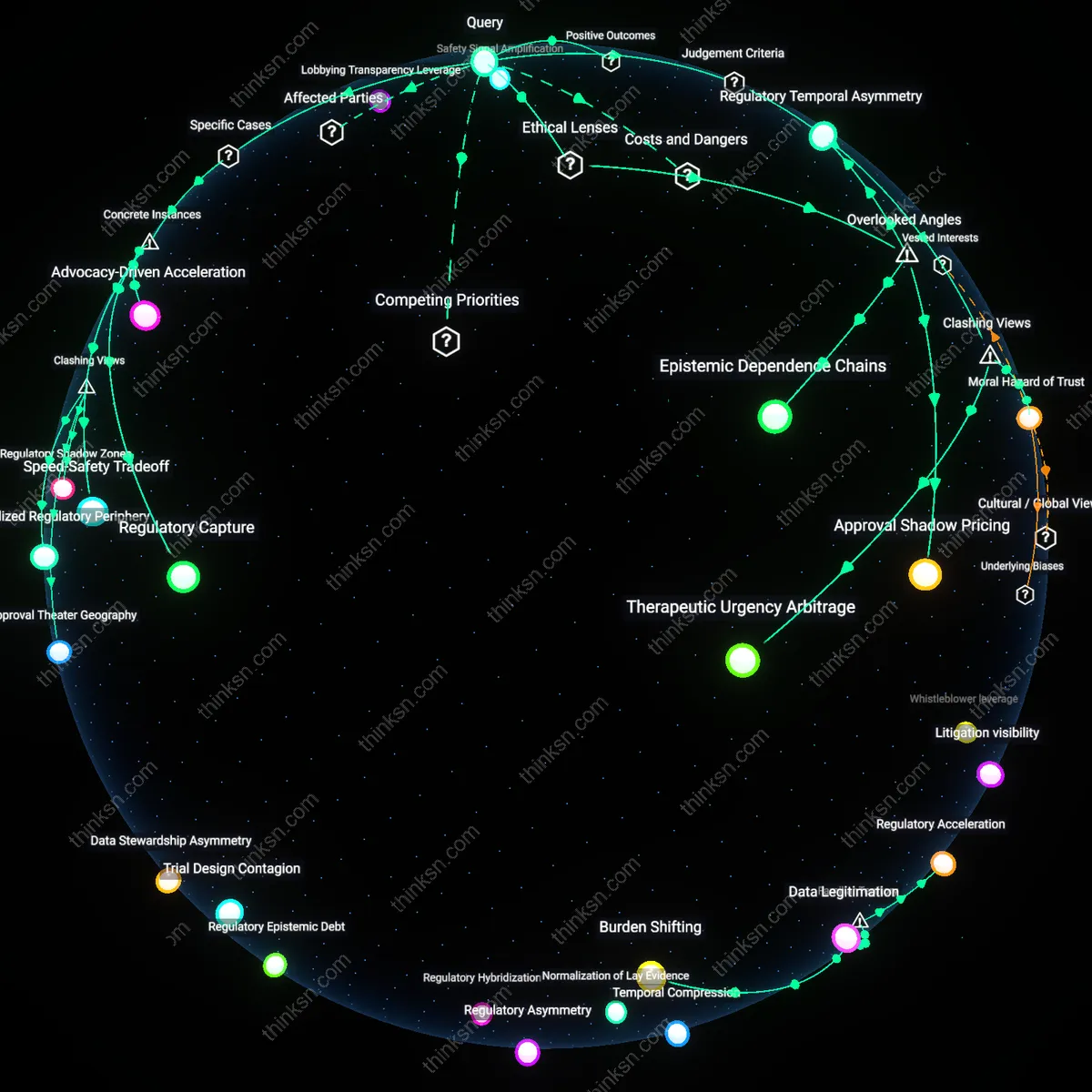
Expert Authority Capture
Key opinion leaders in medicine—those whose endorsements carry weight in guideline committees—frequently receive speaking fees, consulting contracts, and research funding from pharmaceutical companies, aligning their public recommendations with sponsors’ interests through incremental normalization rather than explicit instruction. This operates through social and reputational economies within academic medicine, where credibility is both currency and vulnerability. The non-obvious effect is not corruption per se, but the gradual calibration of what experts consider 'reasonable' treatment thresholds, invisible even to themselves.
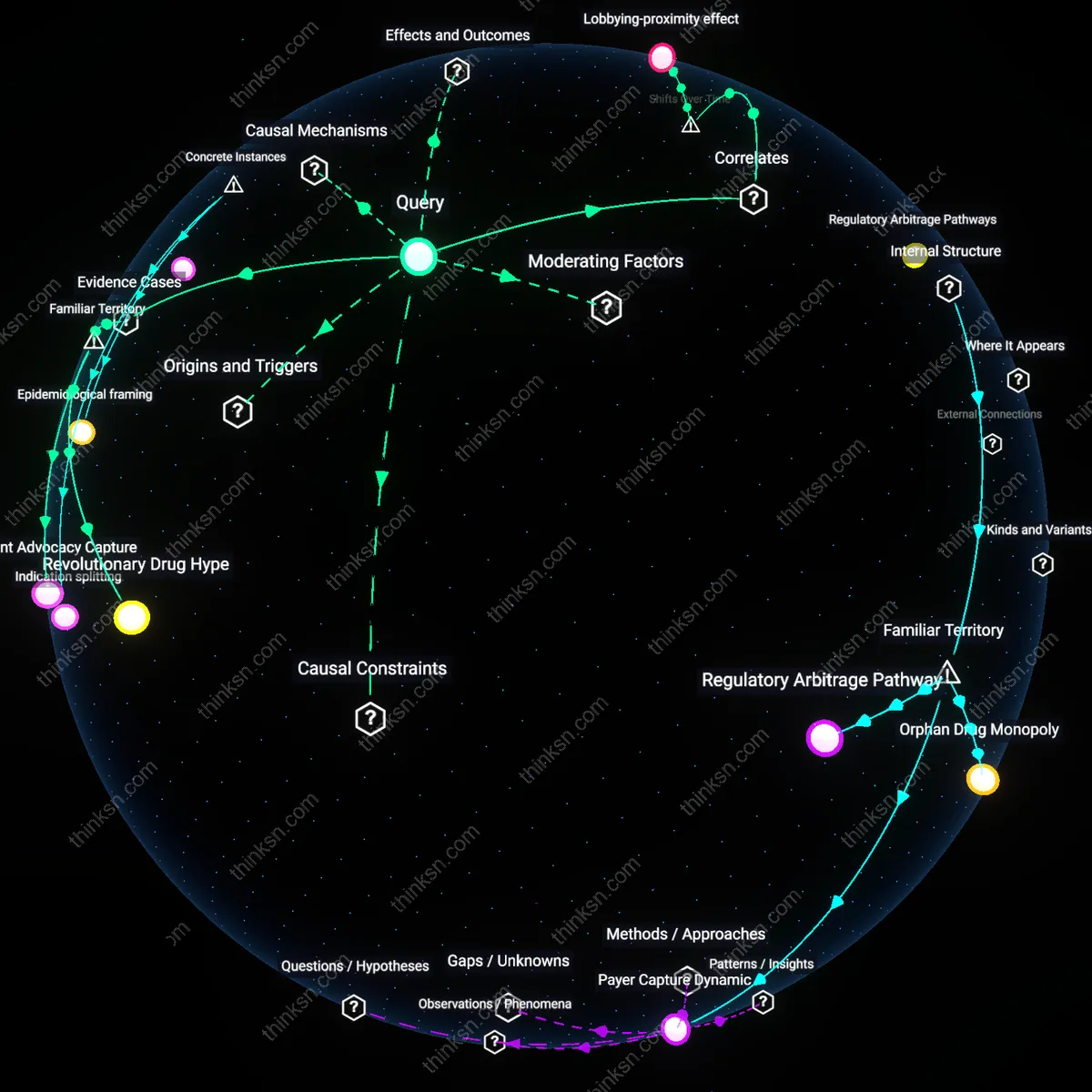
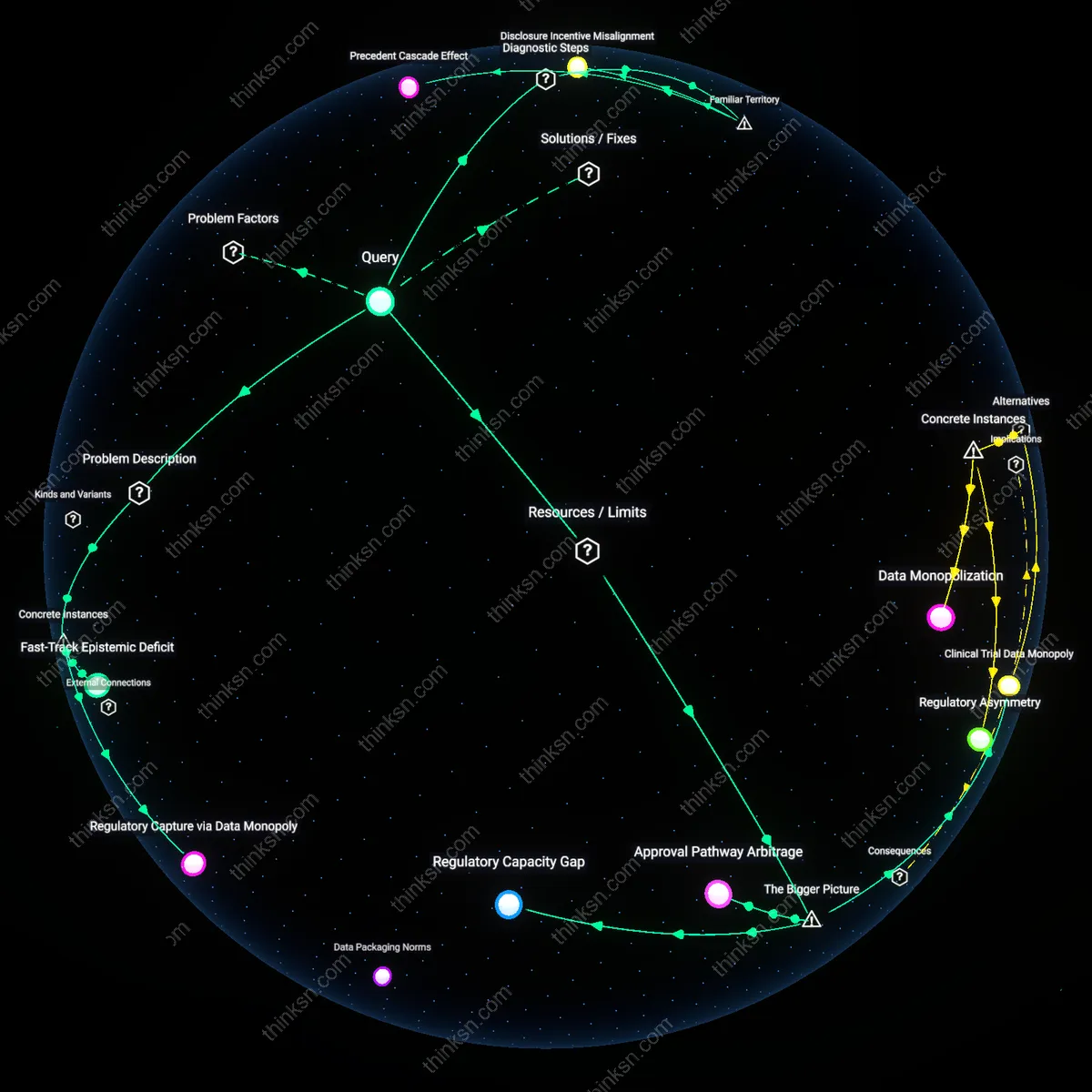
Regulatory Arbitrage
The perception of big pharma influence stems more from regulatory arbitrage than from direct lobbying or inflated power, because pharmaceutical firms exploit jurisdictional discrepancies in drug approval standards to shape clinical practices indirectly. By aligning trial designs with the most permissive agencies—such as the FDA’s accelerated pathways—and then leveraging those approvals as de facto global benchmarks, companies like those behind monoclonal antibodies for Alzheimer’s disease bypass stricter national review bodies without explicit pressure. This mechanism, anchored in institutional fragmentation rather than overt influence, quietly recalibrates guideline development through precedents that appear independent but are structurally preordained. Contrary to the dominant narrative of lobbying as the primary lever, the non-obvious reality is that systemic regulatory misalignment—not corruption or coercion—creates permissive channels through which commercial data assimilate into public health standards.
Epistemic Dependence
The perception of big pharma influence arises more from medicine’s epistemic dependence on proprietary data infrastructures than from either lobbying or independent research dynamics, because clinical guidelines rely on trials that only industry can fund and execute at scale. When entities like Roche or Novartis generate massive genomic datasets tied to expensive therapies, advisory panels at institutions like NICE or the EMA become functionally dependent on private analytics to assess efficacy, blurring the line between evaluation and adoption. This dependence masks itself as neutrality while privileging industry-designed endpoints, as seen in oncology guidelines shaped by response rates over survival outcomes. Against the intuitive critique of corruption, the deeper issue is a knowledge asymmetry so entrenched that even adversarial review cannot extract public-interest conclusions from private evidence frameworks.
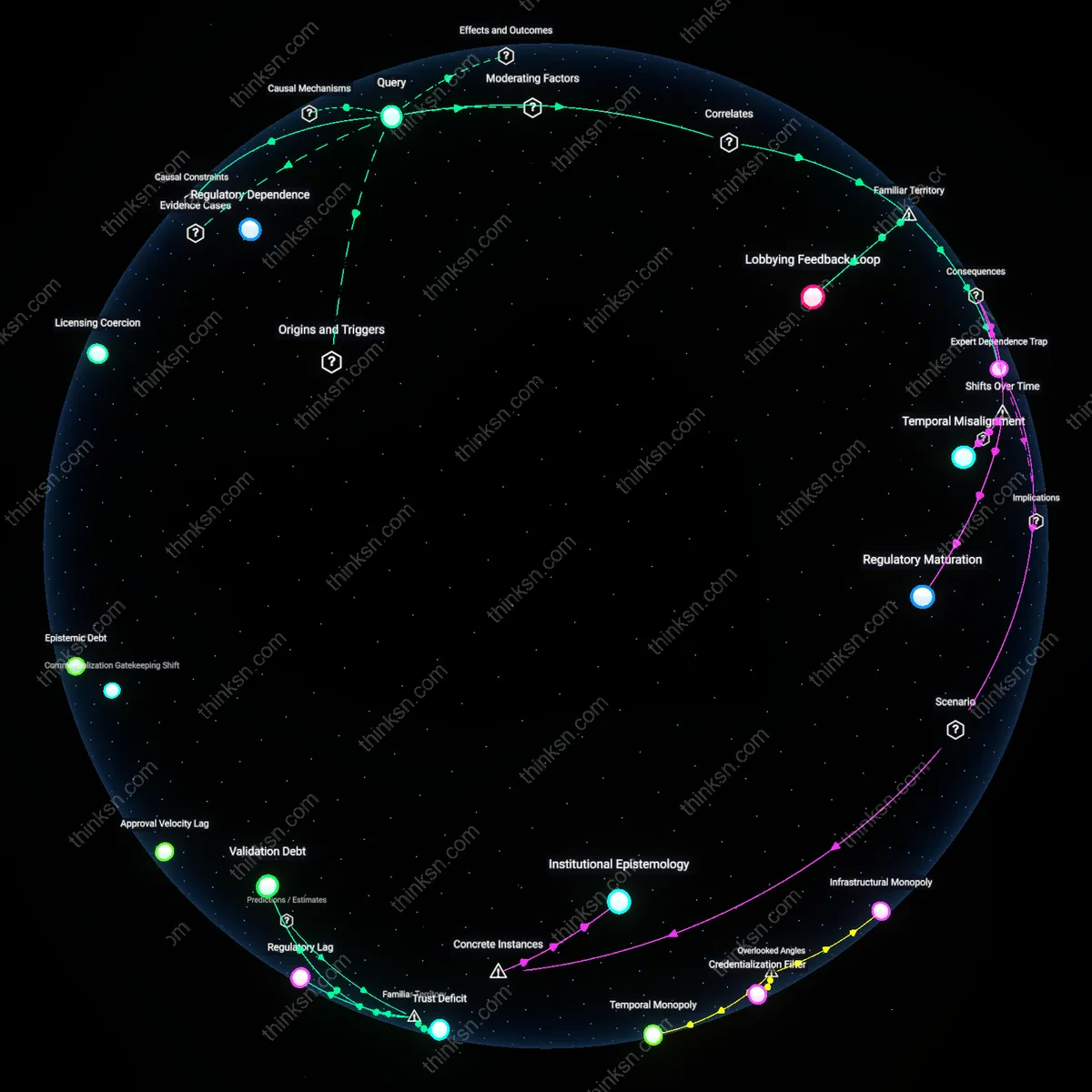
Institutional Mimicry
The perception of big pharma influence is amplified less by lobbying or research imbalance than by institutional mimicry, where independent bodies unconsciously replicate industry epistemologies in response to performance metrics and crisis legitimacy. When the WHO or CDC issue rapid guidelines during pandemics—such as those for mRNA vaccines—they adopt pharma’s temporal and evidentiary frameworks (e.g., surrogate endpoints, compressed trial phases) not due to coercion but to mimic the agility of private actors under public scrutiny. This convergence generates the appearance of capitulation, even when no direct lobbying occurred, because legitimacy now accrues to speed and scalability rather than distance from commercial interests. Unlike the standard view that sees power as exerted through pressure, the dissonance here reveals power as normative—big pharma sets the mold of what timely science looks like, and public institutions, striving to keep pace, become imitators by necessity.
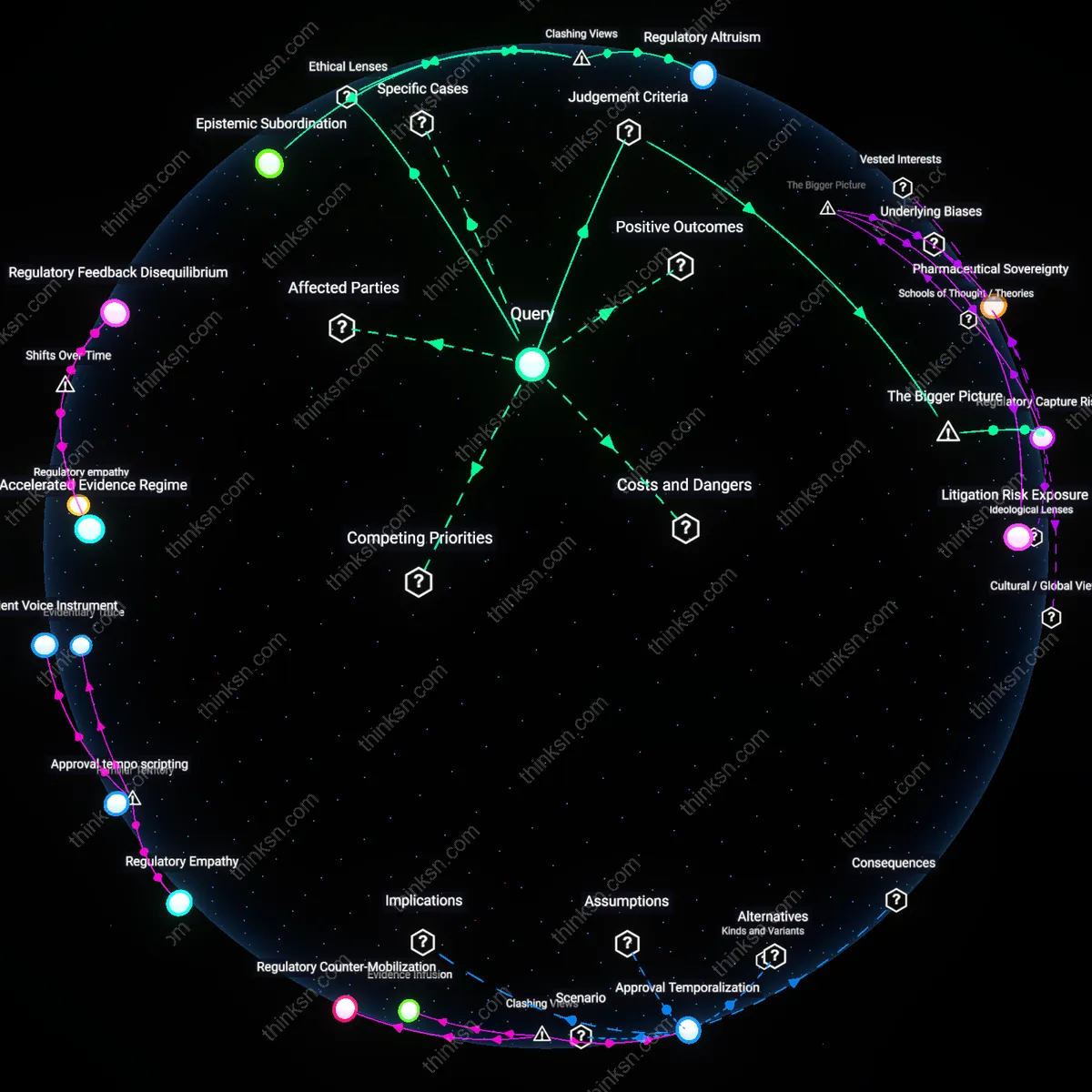
Regulatory dependency
The 2004 FDA approval of rosiglitazone (Avandia) proceeded despite internal advisory committee dissent and emerging cardiovascular risk data because the agency relied on clinical trial designs and safety assessments outsourced to the manufacturer, GlaxoSmithKline; this dependency on industry-generated evidence creates a structural bottleneck where independent research cannot influence regulatory decisions without access to raw trial data or authority to reanalyze outcomes, revealing that lobbying succeeds not by overt coercion but by engineering institutional reliance on proprietary knowledge infrastructures.
Guideline asymmetry
In the 2013 American Heart Association and American College of Cardiology cholesterol guidelines, the expert panel’s risk calculator was later shown to overestimate cardiovascular risk by 75% to 100%, yet the recommendations favored broad statin use—a position aligned with manufacturers like AstraZeneca; the persistence of the flawed tool stemmed not from pharmaceutical lobbying per se, but from the marginalization of epidemiologists and methodologists in the drafting process, demonstrating that the perception of Big Pharma dominance emerges from procedural vulnerabilities in guideline formation rather than direct influence.
Epistemic inertia
Following the publication of the 1998 Vioxx (rofecoxib) trials in the Journal of the American Medical Association, Merck funded symposia and reprints promoting the drug’s gastrointestinal safety while downplaying early thrombotic signals, which shaped prescribing norms despite independent studies in The Lancet questioning its cardiovascular profile; the lag between contradictory evidence and clinical revision reveals that perception of pharmaceutical sway is amplified by the slow integration of counterevidence into medical consensus, a bottleneck rooted in the time and legitimacy required for independent research to overcome entrenched clinical narratives.
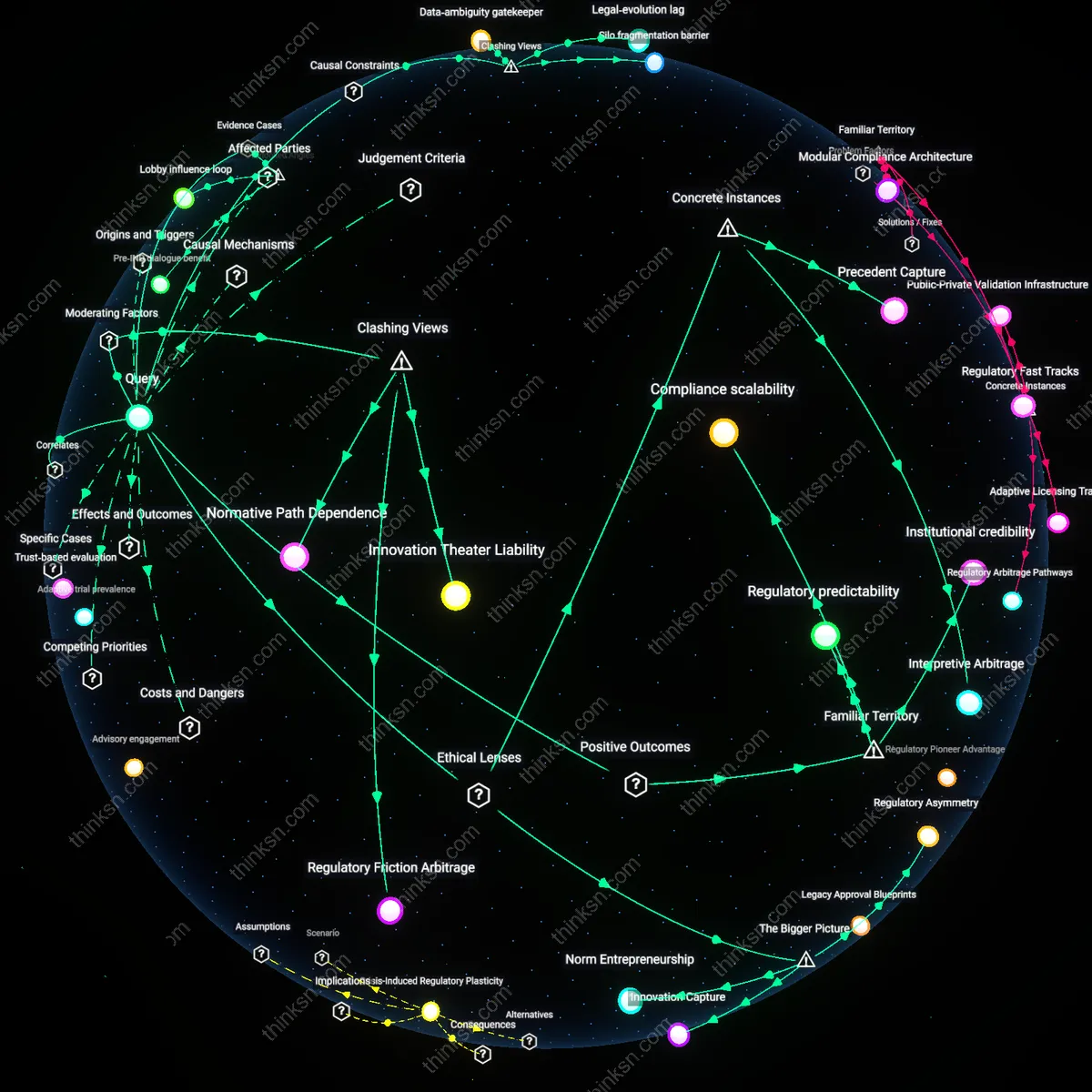
Regulatory Asymmetry
Lobbying by pharmaceutical firms systematically shapes medical guidelines because regulatory agencies like the FDA rely on industry-funded trials for approval decisions, creating a structural dependency that elevates commercial evidence over independent research; this dynamic is most visible in the accelerated approval of drugs like Aducanumab, where weak clinical data was accepted due to political and institutional pressure from Biogen and allied patient advocacy groups amplified by industry lobbying. The mechanism operates through formal channels of rulemaking and informal networks of advisory committees, which are skewed toward experts with financial ties to industry, making the influence not covert but embedded in the governance model of drug evaluation. What is underappreciated is that the legitimacy of guidelines stems from this regulated science framework, meaning the power of 'big pharma' is institutionalized rather than conspiratorial.
Epistemic Insecurity
The perception of pharmaceutical influence exceeds its direct lobbying impact because independent research institutions, such as academic medical centers and professional societies, increasingly depend on industry funding to sustain large-scale trials, as seen in the American Heart Association’s partnerships with companies like Pfizer—this financial entanglement does not always alter outcomes but erodes public trust by blurring the boundary between autonomous science and sponsored research. The systemic issue lies in the underfunding of public health research infrastructure, which forces credible institutions to accept conditional grants that confer legitimacy on sponsors without requiring overt manipulation. The non-obvious consequence is that skepticism toward guidelines arises not from proven manipulation but from structural uncertainty about where independent judgment ends and commercial interest begins.
Narrative Amplification
Public belief in 'big pharma' dominance over guidelines is disproportionately fueled by high-profile litigation and media scandals—such as the Purdue Pharma opioid case—not because such cases reflect widespread guideline manipulation, but because they crystallize diffuse anxieties about medical authority into tangible symbols of corruption. The dynamic operates through news ecosystems and social media, where legal settlements and whistleblower accounts are stripped of context and recast as proof of systemic capture, even when the actual influence on entities like the CDC’s opioid prescribing guidelines involved fragmented, indirect inputs rather than coordinated control. The underappreciated reality is that symbolic events shape perception more than the routine, opaque processes of evidence review, meaning distrust is sustained not by ongoing lobbying but by the cultural resonance of past misconduct.