How Anecdotes Dictate Assisted Living Quality and Equity?
Analysis reveals 9 key thematic connections.
Key Findings
Regulatory Vacuum Feedback Loop
The absence of federal quality benchmarks in U.S. assisted-living facilities after the 1987 Nursing Home Reform Act exempted these settings catalyzed reliance on word-of-mouth assessments by families in states like Arizona, where rapid for-profit expansion outpaced oversight. This mechanism allowed operators like those in Scottsdale’s senior living corridor to shape reputations through marketing and selective family testimonials rather than auditable outcomes, embedding subjective evaluation into care selection. The non-obvious consequence is that deregulatory policy choices—from which nursing homes were deliberately excluded—become self-reinforcing, as public uncertainty legitimizes anecdotalism, undermining demand for standardization.
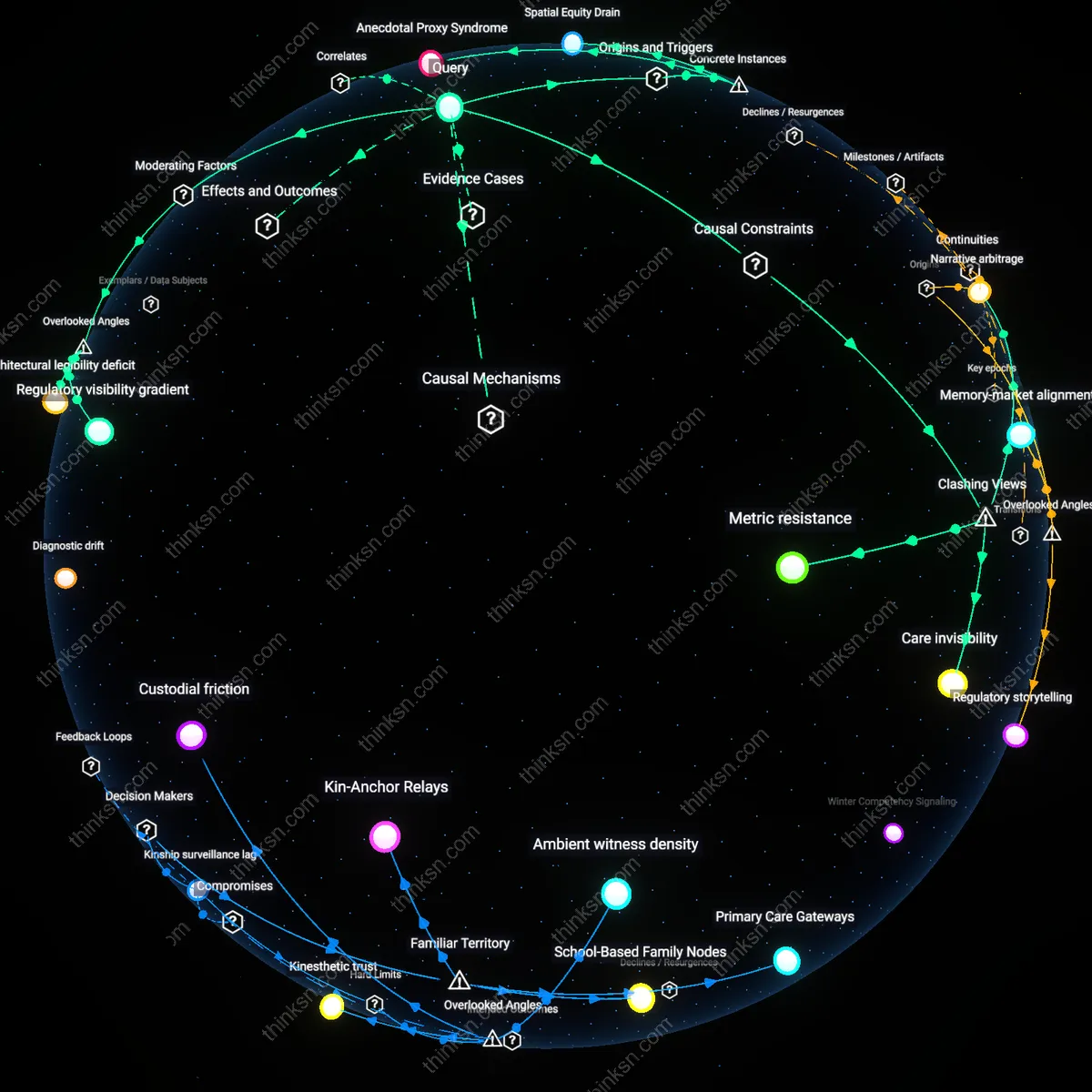
Anecdotal Proxy Syndrome
In Ontario’s long-term care crisis during the 2020 pandemic, families used WhatsApp groups and media reports from facilities like Eatonville Care Centre to gauge safety because the province’s inconsistent inspection data and withheld staffing metrics rendered official information unusable. Over time, these informally sourced narratives became the de facto standard for assessing quality, not because families were uninformed but because they rationally substituted peer experience for absent institutional signals. This reveals how systemic information deficits promote improvised social networks as epistemic substitutes, normalizing anecdote as authoritative despite its selection bias.
Spatial Equity Drain
In post-Katrina New Orleans, the closure of public nursing infrastructure and uneven reintroduction of private assisted-living facilities like those in the Gentilly neighborhood created ZIP-code-dependent access to reliable care information, where white, wealthier families could hire geriatric care managers to gather qualitative insights while Black families relied on overburdened community health workers. This geographic stratification of informational labor reinforced by market-based care models means that the absence of standardized metrics functions as a redistributive mechanism—channeling knowledge capital toward those who can already afford supplemental services. The overlooked insight is that metric scarcity does not affect all communities equally but actively amplifies pre-existing spatial disparities in social capital.
Regulatory visibility gradient
The absence of standardized quality metrics increases family reliance on anecdotal information most acutely in states where regulatory inspections are publicly reported less frequently, because families in these regions lack even minimal formal data to counterbalance word-of-mouth, making informal networks the de facto evaluation system; this uneven distribution of institutional transparency creates a visibility gradient across jurisdictions that is rarely acknowledged in policy discussions, which assume uniform access to oversight data, thereby masking how federalism fragments the evidentiary landscape families must navigate.
Kinship information burden
Families with members dispersed across multiple geographic regions depend more heavily on anecdotal information because they lack embodied, repeated exposure to facility environments and must rely on fragmented updates from distant relatives, creating a hidden labor of information synthesis that falls disproportionately on the most mobile or linguistically fluent family member; this kinship-mediated filtering process distorts quality perceptions in ways invisible to both providers and regulators, revealing that the social structure of caregiving networks—rather than individual decision-making—is a determinant of informational reliability.
Architectural legibility deficit
The physical design of assisted-living facilities—specifically, the absence of publicly observable care cues such as visible staff-resident interactions, accessible common areas, or transparent care routines—forces families to infer quality from indirect social evidence like peer testimonials, because environmental cues that could serve as real-time quality proxies are deliberately obscured by privacy-focused layouts; this architectural legibility deficit shifts evaluative authority from observational assessment to narrative accounts, a dependency rarely considered in debates about transparency that focus on data reporting rather than spatial semiotics.
Metric resistance
The absence of standardized quality metrics does not push families toward anecdotal information because of information scarcity, but because state licensing agencies actively resist adopting outcome-based measures that would enable comparisons, privileging procedural compliance over resident experience; this institutional inertia—exemplified by the reliance on checklist-style surveys in states like Florida and Texas—preserves regulatory minimalism and shields operators from public scrutiny, revealing that the bottleneck is not data availability but political aversion to enforceable quality benchmarks, which contradicts the common view that families lack tools due to market failure rather than deliberate regulatory design.
Narrative arbitrage
Families rely on anecdotes not as a fallback but as a privileged form of intelligence in a market where occupancy rates and private pay status function as de facto quality signals, allowing wealthier facilities to cultivate curated testimonies that mimic objectivity while excluding low-income applicants; this dynamic operates through real estate-driven senior housing investment firms like Brookdale and Holiday Retirement, which deploy marketing teams to amplify selective resident stories, thereby converting subjective narratives into financial leverage—a mechanism that inverts the assumption that anecdotal use reflects vulnerability, instead showing it serves as a gatekeeping tool in equitized eldercare access.
Care invisibility
Equity gaps emerge not because anecdotes are less reliable, but because standardized metrics would expose the systemic reliance on underpaid, racialized labor performing unmeasured emotional and physical care work, particularly in facilities serving Medicaid beneficiaries in urban markets like Chicago and Detroit; the absence of metrics thus functions as a concealment mechanism, where the bottleneck is the industry’s dependence on labor conditions that cannot survive scrutiny, challenging the dominant framing of measurement gaps as technical oversights rather than intentional structuring to maintain exploitative care regimes hidden from public accountability.