Whose Values Prevail in Medical Treatment Disputes?
Analysis reveals 11 key thematic connections.
Key Findings
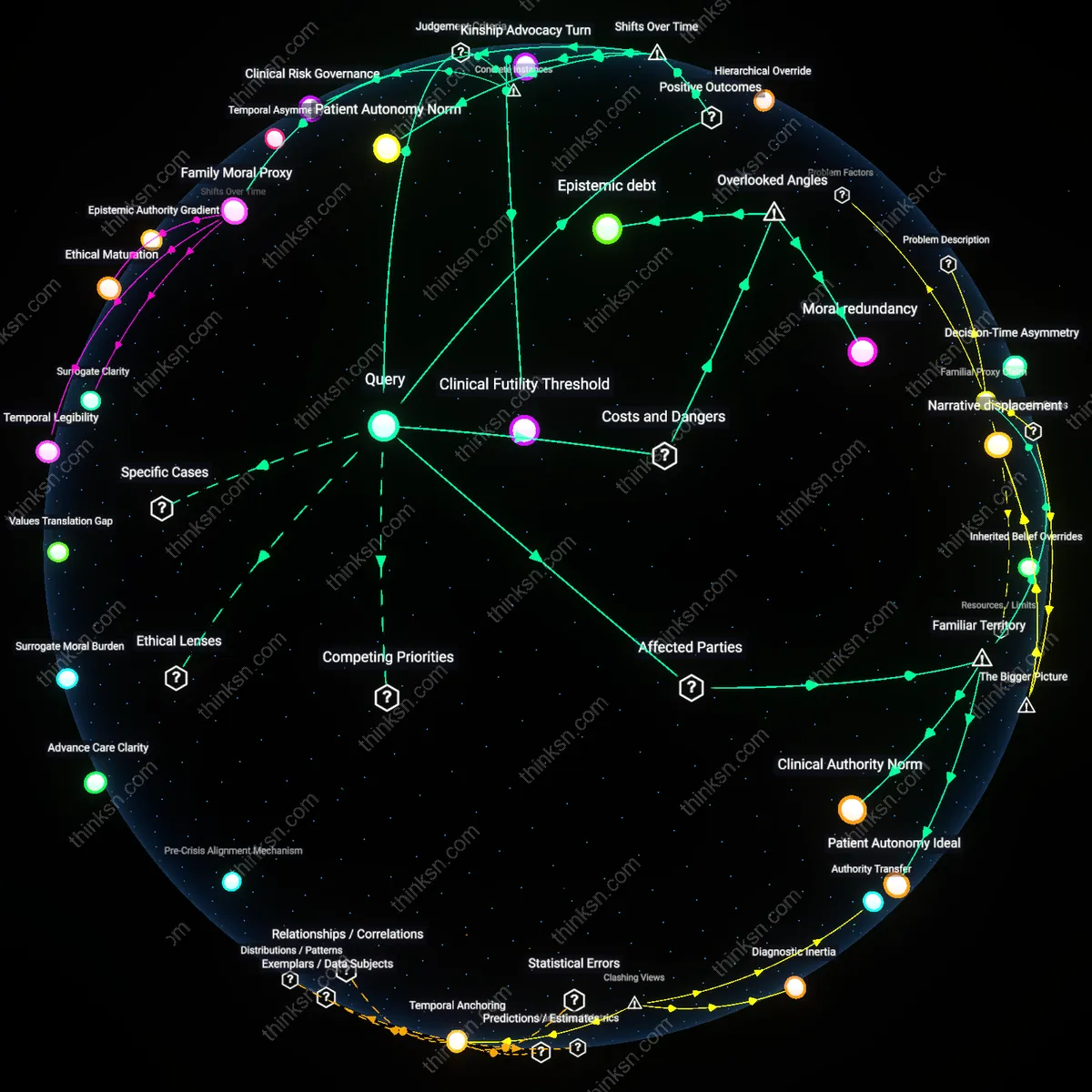
Patient Autonomy Ideal
The patient’s own values must take precedence in medical decision-making, regardless of family pressure or physician caution. This is enforced through legal and ethical frameworks like informed consent and advance directives, which vest ultimate authority in the individual when decisional capacity is present; the mechanism operates through hospital ethics committees and legal liability systems that protect clinicians who honor patient autonomy, even against familial insistence on aggressive care. What is underappreciated in public discourse is that the ‘family’ is not a rights-bearing entity in medical ethics—their role is advisory, not determinative—yet cultural intuition often treats familial consensus as morally binding, obscuring the foundational primacy of the patient’s self-determination.
Clinical Authority Norm
The physician’s recommendation should prevail when it reflects evidence-based standards of care and professional consensus. This precedence is institutionalized through medical licensing bodies, hospital credentialing systems, and peer-reviewed clinical guidelines that empower physicians to withhold or withdraw treatments deemed medically inappropriate; the dynamic functions via professional autonomy protected by medical boards and malpractice jurisprudence. While lay intuition often frames medicine as a shared or negotiable decision-space, the non-obvious reality is that physicians are trained and legally authorized not merely as advisors but as fiduciaries of medical appropriateness, giving them the right—and duty—to resist aggressive interventions that violate standard of care, even in the face of family demand.
Familial Proxy Claim
The family’s values should take precedence when the patient lacks decision-making capacity and the family acts as the legally recognized surrogate. This is operationalized through state-specific surrogate decision-making statutes and hospital admission protocols that prioritize next-of-kin in absence of advance directives; the system depends on the assumption that families best know the patient’s preferences and are motivated by care, not interest. What remains underacknowledged is that this norm relies on a culturally idealized image of the cohesive, altruistic family—yet in practice, familial decisions are often shaped by unresolved dynamics, differing interpretations of love, or religious convictions, which can distort rather than reflect the patient’s authentic values.
Clinical Futility Threshold
The physician's judgment should prevail when treatment fails to meet an institutional standard of medical futility, as seen in the 2005 Texas case involving Terri Schiavo, where a hospital ethics committee invoked state law to override family demands for continued life support after neurological examinations confirmed irreversible brain damage; this mechanism operates through legally codified futility policies that limit non-beneficial interventions, revealing that medicine’s epistemic authority is bounded not by personal opinion but by consensus-derived thresholds of physiological possibility.
Family Moral Proxy
The family's values should take precedence when the patient’s prior autonomy is best interpreted through intimate knowledge, exemplified by the 2014 Oregon Death with Dignity Act cases where family testimony was central in verifying a terminally ill patient’s enduring wish for physician aid-in-dying despite physician hesitation; this dynamic functions through the legal and ethical recognition of surrogates as interpreters of biographical intent, exposing that clinical caution can underappreciate the normative weight of relational identity in reconstructing patient autonomy.
Resource Equity Constraint
Societal values grounded in distributive justice should mediate between family and physician positions, as demonstrated during Italy’s 2020 ICU triage protocol in the COVID-19 surge, where regional health authorities implemented age and comorbidity scoring systems to allocate ventilators when families demanded aggressive care for elderly patients beyond the threshold of clinical priority; this system acted through publicly legitimized triage committees that depersonalized decision-making, underscoring that individual medical choices are constrained by systemic capacity and the moral imperative to equitably distribute scarce goods.
Patient Autonomy Norm
The values of the patient must take precedence in medical decision-making because the post-1970s professionalization of bioethics institutionalized informed consent as a binding clinical standard, shifting authority from familial and physician paternalism to individual choice. This change emerged through landmark legal cases like *Cruzan v. Director, MDH*, which established that competent patients have a constitutional right to refuse treatment, thus codifying personal values as the ethical and legal priority under modern medical governance. The non-obvious element is that family insistence on aggressive care now operates not as a moral appeal but as a procedural challenge to a system designed to override both family and physician preferences if they conflict with documented patient wishes.
Clinical Risk Governance
Physician caution should prevail when it aligns with evidence-based standards because the transformation of medical practice into protocol-driven systems after the 1999 IOM report *To Err Is Human* redefined professional responsibility around population-level safety and liability minimization. In this regime, aggressive interventions unsupported by clinical guidelines expose institutions to systemic risk, triggering audit, reimbursement penalties, and malpractice scrutiny—mechanisms that have quietly elevated standardized practice over familial advocacy. What is underappreciated is that family demands for escalation are no longer assessed morally but as deviations in a quality assurance framework, where the physician acts as a regulatory node rather than a negotiator.
Kinship Advocacy Turn
Family values gain decision-making weight when the patient lacks capacity, a shift accelerated by the rise of aging populations and chronic critical illness in the 2000s, which expanded the default decisional role of surrogates in ICU settings where prolonged ambiguity replaces acute resolution. In this context, hospitals have developed ethics consultation and shared decision-making protocols that treat families not as obstacles but as embedded stakeholders whose emotional and cultural investments contribute to care sustainability and institutional trust. The overlooked dynamic is that medicine now accommodates family insistence not because it is ethically superior, but because the longevity of critical care regimes requires durable social compliance—a pragmatism that grants kinship networks enduring influence even when statistically unwarranted.
Epistemic debt
The patient’s values should defer to the physician’s when family demands aggressive treatment because each deviation from clinical judgment accumulates undervalued informational harm in the medical record system. When physicians override evidence-based restraint to appease family, they introduce treatment distortions that become invisible inputs into institutional learning loops—distorting outcome benchmarks, training algorithms, and audit trails used to refine standards of care. This hidden degradation of data integrity, rarely acknowledged in bedside ethics, systematically undermines future decision-making at scale, particularly in hospitals reliant on retrospective data for protocol development. Most analyses focus on immediate risks to the patient, but the slow corruption of clinical knowledge infrastructure is a deferred cost paid by subsequent undiagnosed victims of skewed norms.
Moral redundancy
The physician’s values should prevail because familial insistence on aggressive treatment often performs symbolic caretaking rather than medical advocacy, reinforcing kinship roles at the expense of patient welfare. In ICU settings, family members’ demands for intervention function less as medical input and more as ritualistic demonstrations of loyalty, witnessed by extended kin and interpreted as moral performance—refusing to ‘give up’ becomes socially obligatory. This dynamic inserts non-medical intent into treatment escalations, forcing clinicians to participate in ethically redundant acts that preserve family identity cohesion but increase iatrogenic risk. Standard bioethics frames this as a conflict of values, but misses that the family’s stance may serve a psychological or social function unrelated to the patient’s well-being—rendering their advocacy morally inert despite its emotional intensity.