Should Freelancers Keep Health Emergencies Separate from Savings?
Analysis reveals 9 key thematic connections.
Key Findings
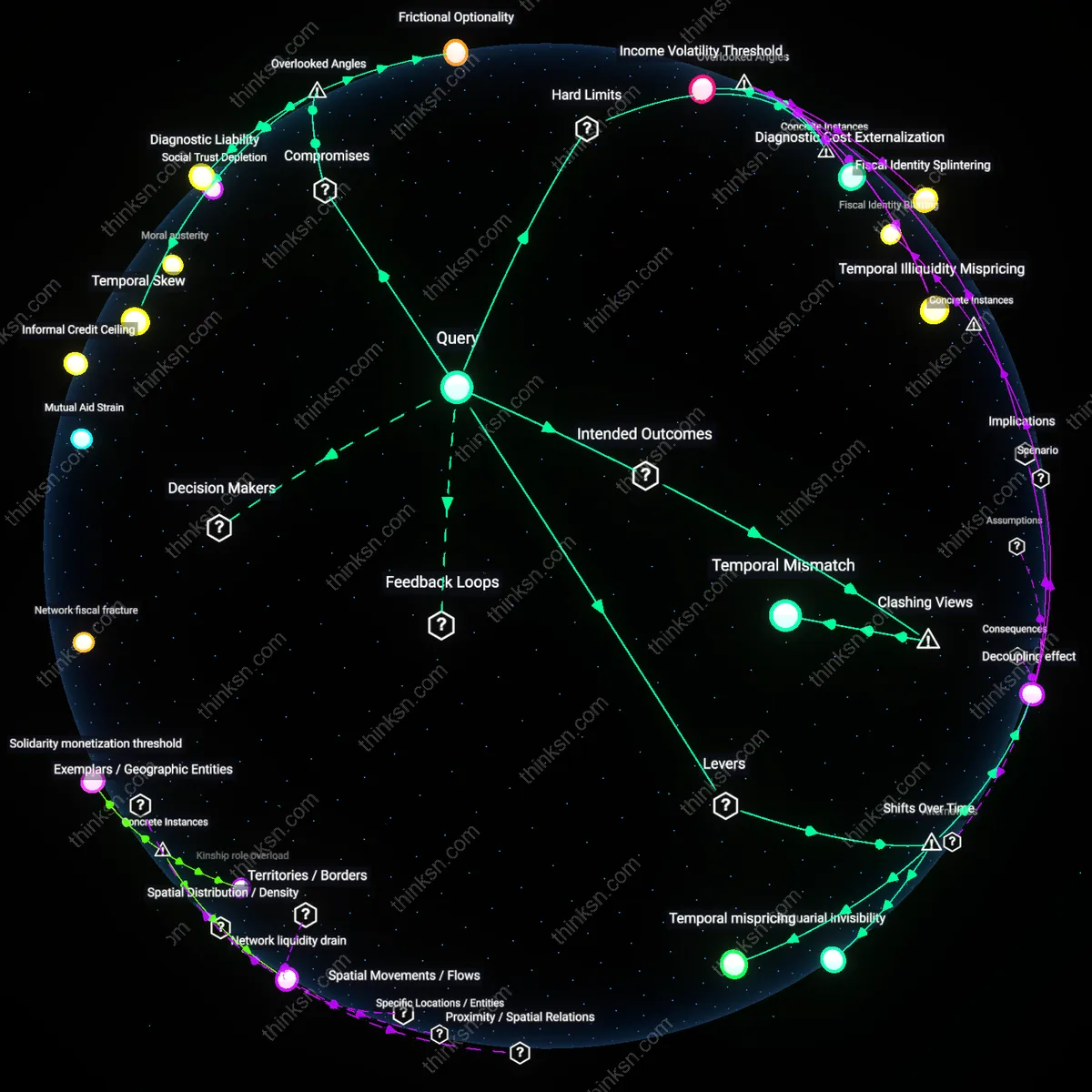
Income Volatility Threshold
Self-employed professionals should integrate healthcare costs into a general emergency fund because unpredictable revenue streams make segregated reserves impractical under real-world cash flow constraints, as demonstrated by ride-share drivers during the 2020–2021 pandemic lockdowns. When Lyft and Uber drivers faced sudden income drops, those who maintained unified emergency pools could redirect funds fluidly between rent, insurance premiums, and urgent care, while those with segregated medical savings often couldn't access them for basic survival despite mounting health costs. This shows that liquidity survival during systemic shocks depends on fungibility, not categorization—a dynamic overlooked when policies assume stable income envelopes.
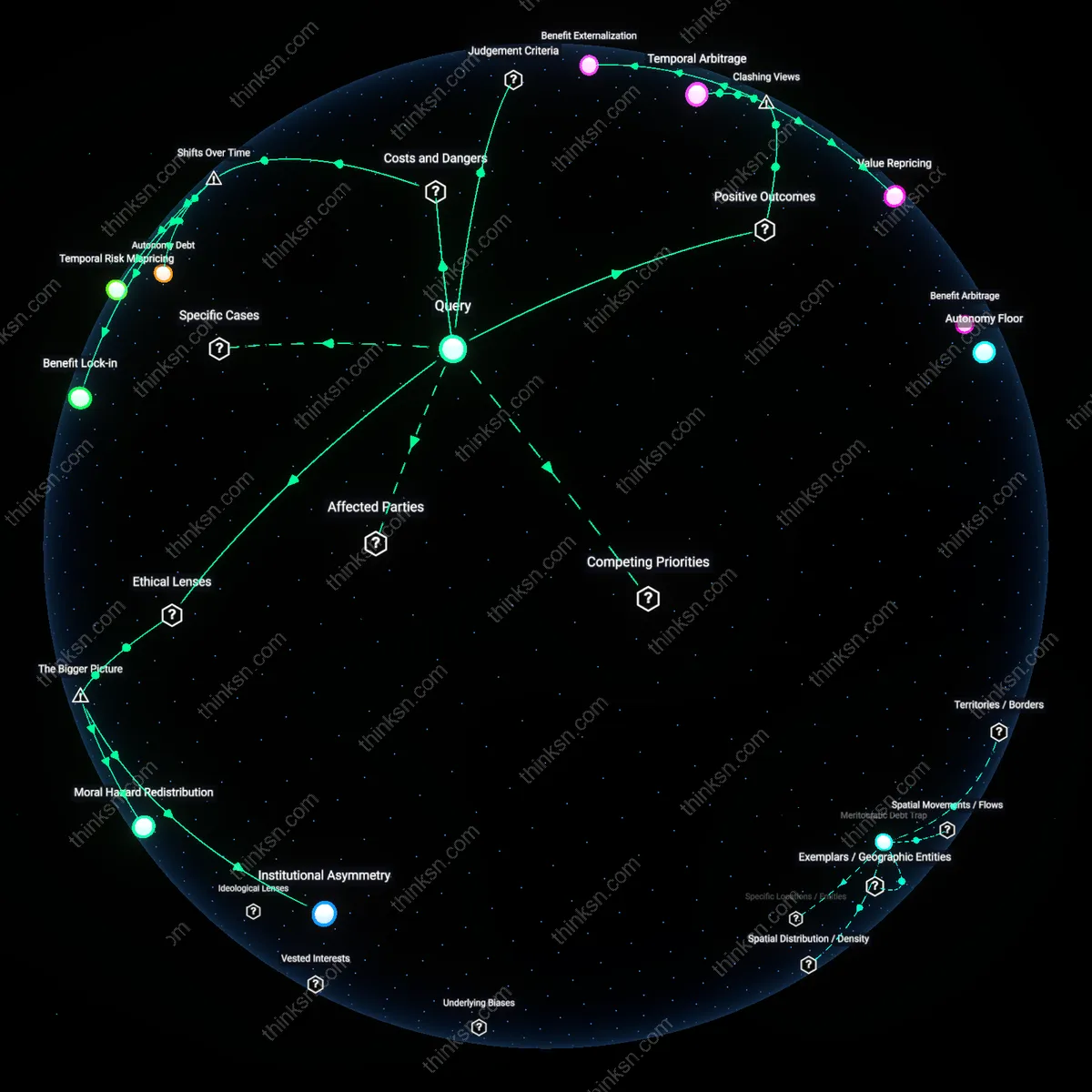
Market Fragmentation Cost
Self-employed professionals in high-deductible insurance plans must isolate healthcare savings because U.S. market fragmentation—exemplified by New York State’s Freelancers Insurance Company collapse in 2017—forces individuals to anticipate sudden coverage gaps and provider-specific cost spikes without systemic backstops. After the FIC dissolved, many freelancers lost access to pooled risk mechanisms and faced full out-of-network charges, meaning those with dedicated medical reserves could immediately cover MRIs or ER visits without draining retirement or business capital. This instance reveals that in the absence of universal safety nets, medical cost exposure operates on a different risk surface than general emergencies, making integration a latent threat to long-term solvency.
Decoupling effect
Self-employed professionals should maintain a separate emergency fund for health-care costs because the post-2010 shift toward high-deductible health plans and individual market enrollment has severed health cost predictability from income stability, forcing practitioners to absorb variable medical outlays as business risk. This structural break—triggered by the Affordable Care Act’s indirect incentivization of consumer-driven health insurance—transformed episodic care into a financial exposure akin to equipment failure or client churn, requiring isolated capital reserves to prevent liquidity crises. The non-obvious insight is that health expenses are no longer household liabilities but operational contingencies, governed not by personal budgeting but by risk-mitigation logic used in small-firm cash flow management.
Actuarial invisibility
Integrating health-care costs into a general savings pool is preferable because the pre-1980 era of employer-sponsored, pooled-risk insurance created a cultural expectation of medical cost insulation that persists even as self-employment rises, leaving today’s freelancers without actuarial scaffolding to forecast liabilities. Modern platforms like Health Savings Accounts and freelance unions (e.g., Freelancers Union pre-2020) attempted to replicate group underwriting, but failed to gain scale due to fragmented labor markets and regulatory gaps, rendering individual savings the de facto risk pool. The key insight is that the disappearance of institutional actuarial assessment means individuals now perform implicit underwriting on themselves—using generalized savings as a proxy for risk pooling, revealing a silent privatization of statistical labor.
Temporal mispricing
Self-employed professionals should segregate health-care savings because the post-2008 financialization of medical debt altered the time horizon of risk, shifting consequences from immediate payment shocks to long-term credit degradation, which general emergency funds are structurally blind to. Credit scoring systems now weigh unpaid medical bills over time, linking episodic health events to future borrowing capacity, yet conventional emergency savings are designed for short-term income gaps, not decade-spanning liability accruals. The overlooked mechanism is that health-specific reserves function as time arbitrage tools—prepaying against the delayed penalty structure of financialized medicine, exposing how emergency preparedness has morphed from liquidity assurance to intertemporal credit positioning.
Temporal Skew
Self-employed professionals should maintain a separate emergency fund for healthcare because the timing mismatch between income volatility and medical billing cycles creates unpredictable cash-flow hazards. Most analyses focus on total cost or savings targets, but overlook how the irregular arrival of freelance earnings interacts with the inflexible, immediate demands of healthcare providers — who typically expect payment within 30–60 days regardless of a patient’s revenue cycle. This temporal misalignment means a practitioner might be flush with funds one month and unable to cover an urgent deductible the next, even if their annual income is sufficient. The non-obvious insight is that liquidity timing, not just savings volume, determines healthcare resilience, making compartmentalized reserves a form of temporal insurance.
Diagnostic Liability
Self-employed professionals should integrate healthcare costs into a general emergency fund because maintaining clinical secrecy becomes a financial liability when medical accounts are segregated. If a distinct healthcare fund is tracked through specialized accounts or withdrawal patterns, it inadvertently flags health status to third parties such as accountants, payment processors, or tax auditors who infer diagnoses from transaction categories like 'oncology' or 'mental health.' Unlike employees whose health data is shielded within employer-sponsored plans, solo practitioners expose sensitive information through financial operational transparency, increasing reputational and insurability risks. The overlooked dynamic is that fund segregation can leak private health data through financial metadata, turning fiscal discipline into a privacy vulnerability.
Frictional Optionality
Self-employed professionals should integrate healthcare costs into a general emergency fund because pooled reserves increase strategic flexibility during systemic disruptions like regulatory reform or insurance shifts. When healthcare is siloed, individuals are more likely to rigidly retain suboptimal insurance plans to justify fund existence, even if switching would save money — a psychological commitment device that reduces adaptability. A unified fund, however, allows rapid re-deployment of capital toward new care delivery models, such as direct primary care subscriptions or cross-border telemedicine, without re-allocating between accounts. The overlooked mechanism is that account structure shapes response latency to institutional innovation, making integration a stealth enabler of option value during policy inflection points.
Temporal Mismatch
Self-employed professionals should not pre-fund healthcare emergencies separately because doing so creates a temporal mismatch between premium payments and cost exposure, making dedicated savings redundant in context of existing insurance cycles. Most self-employed individuals already pay monthly premiums for high-deductible health plans (HDHPs) and are simultaneously building Health Savings Accounts (HSAs), where funds are tax-advantaged and accumulate over time—pre-allocating additional income to a parallel emergency fund effectively double-stacks reserves for the same risk. This redundancy distracts from optimizing HSA utilization and investing those balances for compound growth, revealing that perceived preparedness through duplication often masks a failure to align savings mechanisms with the actual temporal structure of risk and reimbursement in real-world healthcare finance.