Who Benefits When Dental and Vision Join Health Plans?
Analysis reveals 6 key thematic connections.
Key Findings
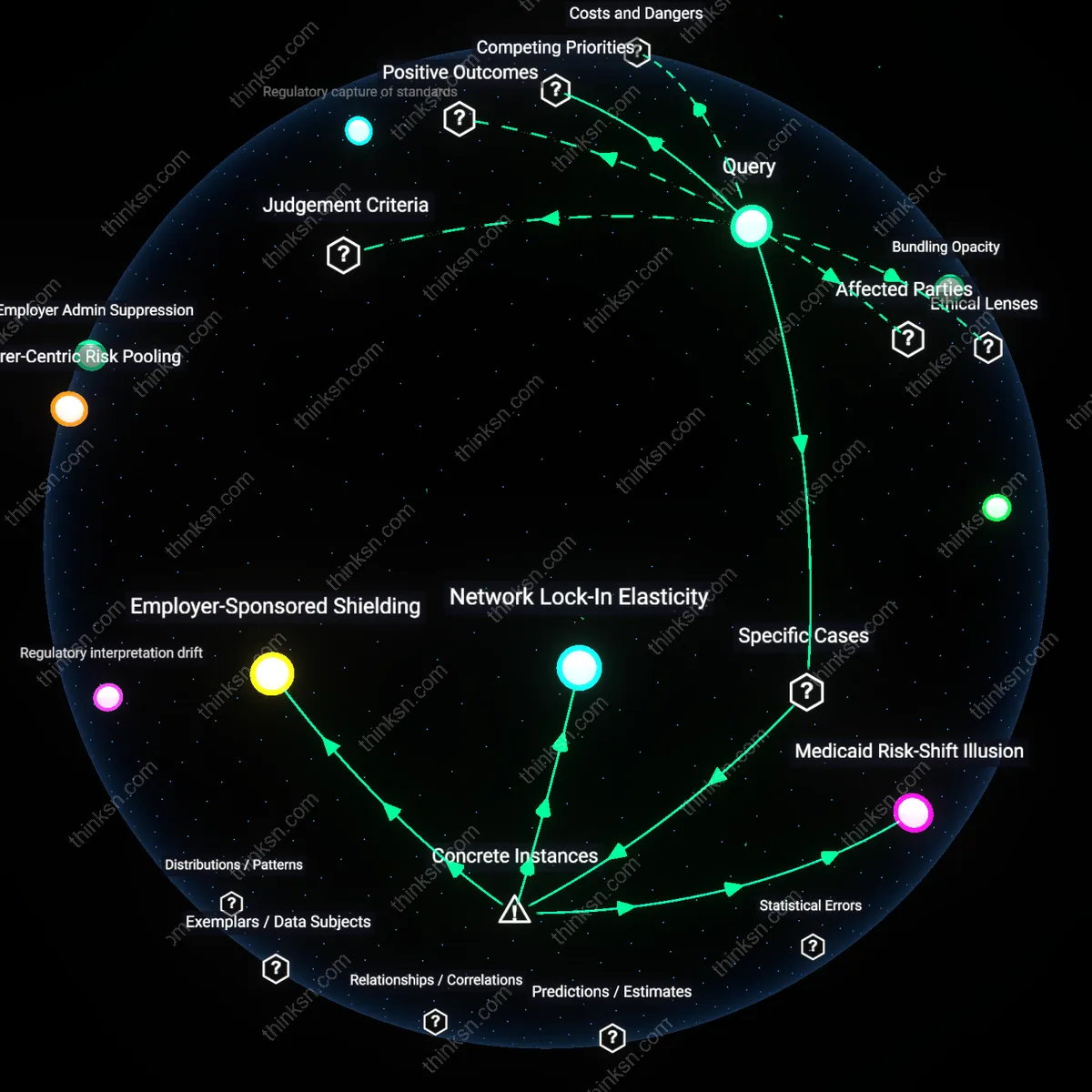
Insurer-Centric Risk Pooling
Bundling dental and vision with primary health insurance primarily benefits large multi-line insurers by enabling cross-subsidization that obscures cost structures, not consumers. Insurers leverage administrative integration to merge risk pools across clinically distinct services, allowing margins from high-utilization dental plans to offset losses in loss-leading vision offerings—while marketing the bundle as holistic care. This integration reduces price comparability between stand-alone and bundled plans, particularly in employer-sponsored markets where opaque actuarial models limit employee understanding. The non-obvious mechanism is not expanded access but the deliberate destabilization of cost transparency as a competitive variable, favoring scale over consumer choice.
Employer Admin Suppression
The main beneficiaries of bundling are HR administrators in mid-to-large private firms, who gain reduced contract management complexity at the cost of employee pricing awareness. By consolidating vendor contracts into single-provider health bundles, employers suppress procurement workload and audit frequency, effectively trading granular cost visibility for operational efficiency. This shift transfers pricing authority from finance and benefits teams to centralized insurance brokers who negotiate opaque bundled rates, making it harder for employers to benchmark individual component costs. The counterintuitive outcome is that administrative convenience is structurally privileged over consumer cost transparency in ERISA-regulated plans, where fiduciary standards do not require itemized valuation of ancillary benefits.
Actuarial Obfuscation Regime
Actuaries, not patients or providers, are the primary functional beneficiaries of bundled dental-vision-primary insurance, as the integration expands their discretionary authority to set non-competitive reference prices across service silos. By modeling utilization covariance between vision exams and chronic disease screenings—despite weak clinical correlation—they justify bundled premiums that resist external price auditing. This creates a regulatory arbitrage where NAIC filing rules permit blended loss ratios, preventing state-level transparency tools from isolating overpricing in low-acute services like routine dentistry. The underappreciated conflict is that actuarial legitimacy, upheld as a technical necessity, systematically undermines consumer capacity to detect cross-service rent extraction.
Employer-Sponsored Shielding
Large employers like Walmart benefit by bundling dental and vision with primary health insurance to suppress visible payroll costs while shifting wellness accountability onto insurers through pre-emptive care mandates. By contracting UnitedHealthcare for integrated benefit administration across 1.5 million employees, Walmart externalizes cost-complexity, making out-of-pocket exposure less transparent to workers despite increased overall premium growth. This reveals how cost bundling in multi-billion-dollar private employer plans obscures true expense allocation under the guise of convenience, enabling employers to appear fiscally responsible without reducing total healthcare spending.
Network Lock-In Elasticity
Kaiser Permanente’s vertically integrated model in California demonstrates how bundling dental and vision into primary coverage increases patient retention through reduced switching incentives, not savings. By co-locating optometry and dental clinics within medical centers and enforcing single-network access, Kaiser limits price visibility at point of service, leading members to undervalue standalone cost comparisons. This case uncovers how integration distorts consumer cost perception not through inflated charges but through the implicit devaluation of alternative providers, tightening network dependency beyond actuarial necessity.
Medicaid Risk-Shift Illusion
In Mississippi’s Medicaid managed care rollout under Centene Corporation’s Molina Healthcare, the bundling of children’s dental and vision screenings with primary care created a false appearance of cost containment by consolidating billing—yet led to underutilization due to opaque referral thresholds. Providers reported difficulty navigating bundled reimbursement codes, delaying preventive services and ultimately increasing long-term morbidity costs hidden from enrollees. This illustrates how administrative simplification in state-federal partnerships can mask deteriorating access, reframing transparency loss as systemic inefficiency rather than pricing obscurity.