Why No Universal Palliative Care in the US?
Analysis reveals 5 key thematic connections.
Key Findings
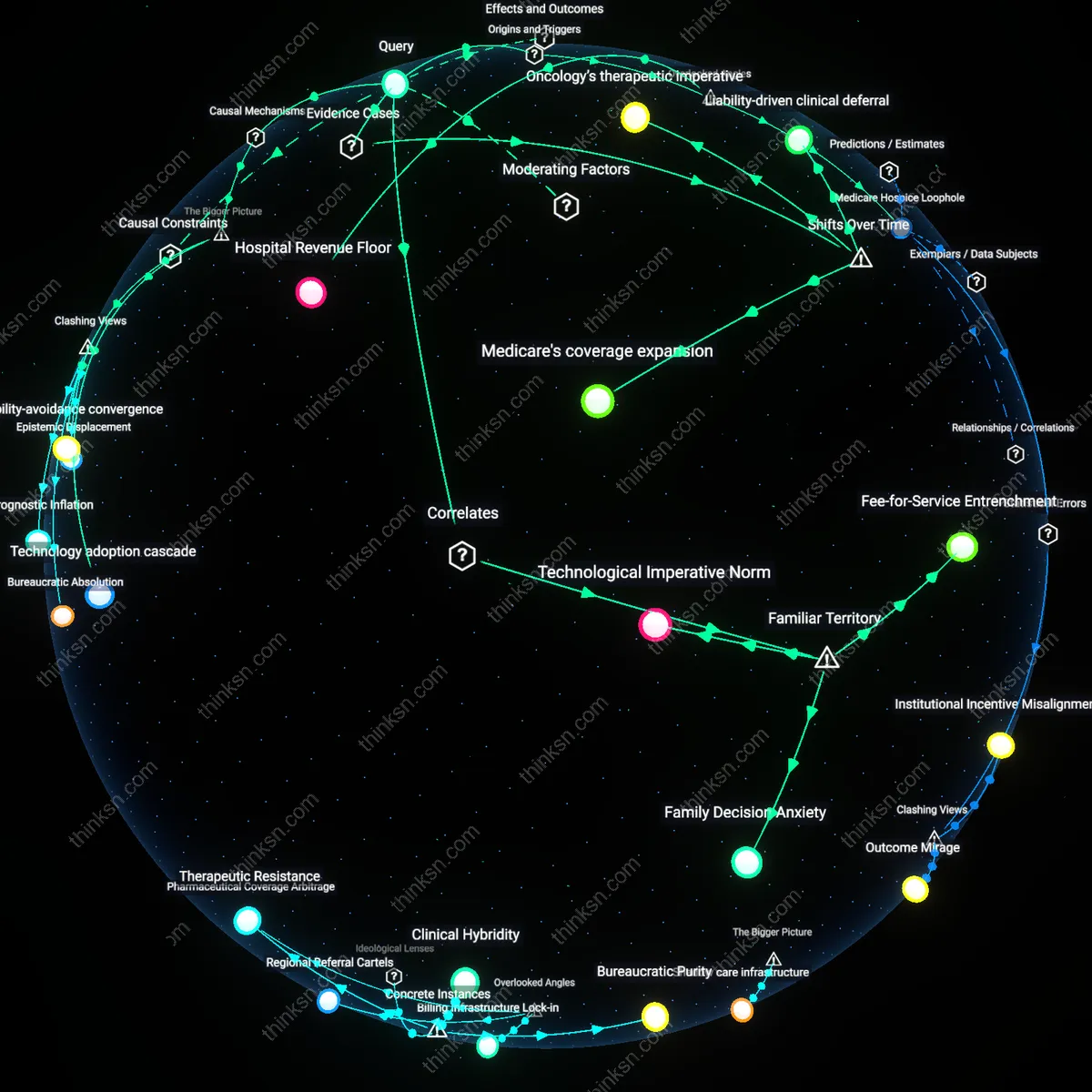
Reimbursement Asymmetry
Shifting Medicare's payment model to bundle palliative care services within chronic disease management for Medicare Advantage plans directly enables broader access for low-income enrollees who disproportionately rely on these plans. This lever works because private insurers follow Medicare's lead in care delivery standards, and tying reimbursement to integrated symptom management rather than curative interventions creates financial incentives for health systems to scale outpatient palliative services in safety-net clinics. The non-obvious dynamic is that Medicare Advantage—a privatized public program—acts as a regulatory Trojan horse, allowing federal policy to indirectly reshape care norms across both public and private markets through aligned incentives.
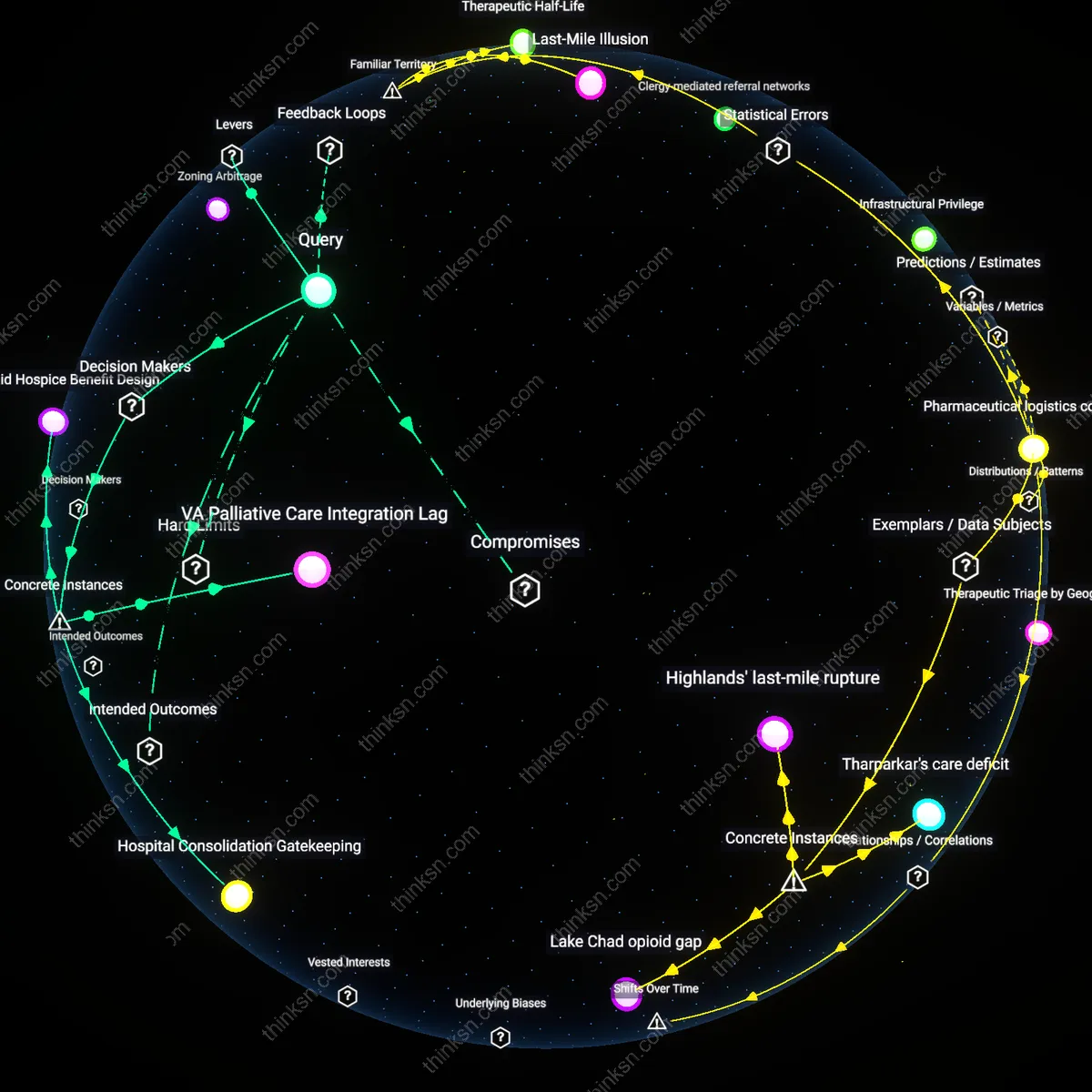
Zoning Arbitrage
Revising statewide certificate-of-need (CON) laws to exclude hospice inpatient facilities from approval requirements enables community-based organizations to establish culturally attuned hospice centers in medically underserved zip codes. In Southern states like North Carolina, CON laws originally intended to control costs have been co-opted by established hospital systems to block competing end-of-life facilities in affluent areas, indirectly restricting spillover access to adjacent low-income counties. Removing this barrier allows grassroots groups to exploit geographic and regulatory fissures, exposing how spatialized health policy tools can entrench care deserts under the guise of fiscal oversight.
Medicaid Hospice Benefit Design
The structure of the Medicaid Hospice Benefit in Louisiana forces terminally ill patients to forgo curative treatments to access palliative care, creating a false choice that disproportionately impacts low-income rural populations who lack access to alternative providers. Because Medicaid is administered at the state level with federal guidelines that mandate hospice election replace rather than supplement ongoing treatment, patients in geographically isolated parishes like Tensas County cannot afford to travel for dual care, effectively excluding them from concurrent care models proven in oncology settings. This reveals how a federal-state financing split, codified in the 1982 Medicare hospice benefit and adopted by Medicaid, institutionalizes treatment discontinuity as a cost-control mechanism, obscuring its role in producing geographic and class-based exclusion under the guise of patient choice.
VA Palliative Care Integration Lag
Despite the Department of Veterans Affairs’ national palliative care rollout after the 2010 Care Coordination for High-Risk Patients initiative, rural veterans in New Mexico’s Zuni Pueblo remain underserved due to the delayed integration of telepalliative services in Indian Health Service (IHS)-VA shared jurisdictions. Because the VA relies on interagency memoranda of understanding with IHS for care delivery, and these agreements lack binding timelines for technology transfer or staffing, palliative care access depends on tribal health infrastructure capacity rather than federal entitlements. This demonstrates how intergovernmental service delivery models, even within fully funded federal systems, reproduce inequity when implementation mechanisms are left to negotiation rather than mandated standards, particularly where overlapping sovereignties become administrative loopholes.
Hospital Consolidation Gatekeeping
After the 2017 merger of Ascension Health and Providence St. Joseph in California, palliative care staffing in former safety-net hospitals in Fresno declined by 40% as centralized administration redirected resources to higher-reimbursement sites in wealthier counties. Because nonprofit health systems classify palliative services as non-revenue-generating and subject to internal capital allocation, care access becomes contingent on facility profitability rather than patient need, especially in regions like the Central Valley with high uninsured rates. This exposes how tax-exempt hospital networks, though bound by community benefit obligations, exploit ambiguity in IRS Form 990 reporting to concentrate specialized services in lucrative markets, transforming ostensibly public-serving institutions into de facto gatekeepers of end-of-life dignity.