Why Choose Cheaper Infant Care Over Safer, More Expensive Options?
Analysis reveals 7 key thematic connections.
Key Findings
Financial Tradeoff Norm
Parents choose lower-cost care because immediate household budgets constrain choices more than abstract safety assurances. This selection reflects a survival-level prioritization where paying rent or buying food reliably outweighs probabilistic benefits tied to accreditation, especially when risks like infant neglect are invisible until they occur. The mechanism operates through localized decision environments—households, neighborhoods, city voucher programs—where underfunded public support systems make cost the dominant filter. What’s underappreciated is how consistently this tradeoff is framed not as neglect but as responsible pragmatism, reinforcing a shared social script that equates financial sacrifice with parental duty.
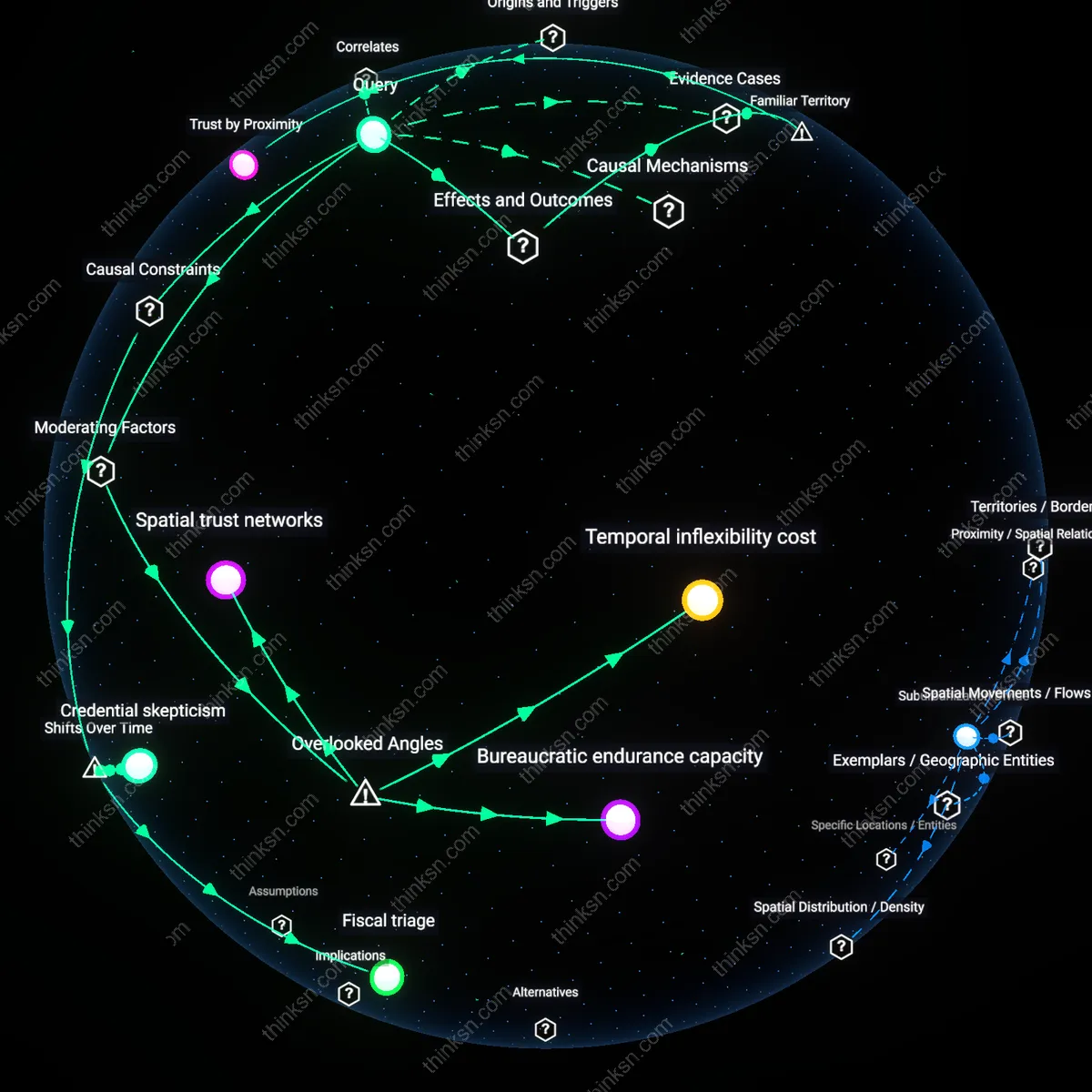
Trust by Proximity
Parents favor familiar caregivers in homes nearby because visible, everyday presence builds perceived reliability more than institutional credentials. This preference leverages community-embedded networks—such as relatives, church members, or longtime neighbors—where trust accumulates through repeated social exposure rather than auditing or regulation. The dynamic functions through neighborhood-scale information circuits where reputation spreads orally and slowly, often bypassing formal quality indicators. What often goes unremarked is how accreditation can seem alien or bureaucratic in these settings, making low-cost home-based care feel more accountable precisely because it is socially visible and culturally legible.
Spatial trust networks
Proximity to kin or culturally affiliated institutions increases reliance on informal evaluations of care quality, bypassing formal accreditation metrics. When infant care programs are embedded within trusted community geographies—such as places of worship, ethnic enclaves, or family-coordinated arrangements—parents weight lived familiarity and social continuity over institutional credentials, especially when those programs are vouched for through intergenerational or neighbor-based validation. This dynamic diminishes the perceived necessity of accreditation not because parents disregard safety, but because safety is redefined through relational continuity rather than external audits—an overlooked mechanism where geographic and social closeness become proxies for institutional legitimacy.
Temporal inflexibility cost
Accredited infant care programs often enforce rigid enrollment cycles, attendance schedules, and fee structures that conflict with the episodic income patterns of gig, shift, or seasonal workers. For parents whose earnings fluctuate weekly or monthly, the financial penalties for absenteeism or late payment in standardized programs create greater perceived risk than variable care quality in lower-cost alternatives. This overlooked dimension reframes cost not as a static price differential but as a dynamic mismatch between care infrastructure and irregular temporal economies, shifting 'affordability' from a fixed calculation to a resilience-of-fit issue.
Bureaucratic endurance capacity
Parents navigating multiple systemic interfaces—such as immigration services, public housing, or court-mandated programs—often lack the surplus cognitive and administrative bandwidth to manage additional documentation-heavy enrollments, even when benefits like subsidized accredited care are technically available. The hidden burden of bureaucratic endurance—collecting notarized forms, maintaining digital access, or attending fixed appointment windows—acts as a silent exclusion filter, making minimally documented, walk-in infant care centers more viable despite lower accreditation. This reveals that program accessibility is less about financial cost and more about procedural survivability in overtaxed decision ecologies.
Fiscal triage
Parents began selecting lower-cost, unaccredited infant care in the 1980s as state defunding of social services shifted care burdens entirely onto households, forcing working mothers to weigh co-pays against closure gaps; this fiscal triage emerged not from ignorance of safety standards but from the systemic elimination of subsidized alternatives that once made accredited care accessible in industrial cities like Detroit or Cleveland. The mechanism—household budget ceilings overriding risk calculus—reflects a post-New Deal erosion of public childcare infrastructure, revealing how cost became a mandatory filter before quality could be assessed.
Credential skepticism
Beginning in the mid-2000s, some immigrant and rural parents increasingly distrusted accreditation as a proxy for quality, shaped by generational care practices and negative encounters with institutionally regulated spaces like child protection systems; their preference for low-cost, kin-embedded care is not inertia but a reactive redefinition of safety as relational continuity, not compliance. This shift grew as accreditation became bureaucratized through federal block-grant reforms post-2002, making it a symbol of surveillance rather than safeguard, particularly in communities with historical marginalization by state agencies.