Accepting Subsidies While Lobbying to Cut Them?
Analysis reveals 6 key thematic connections.
Key Findings
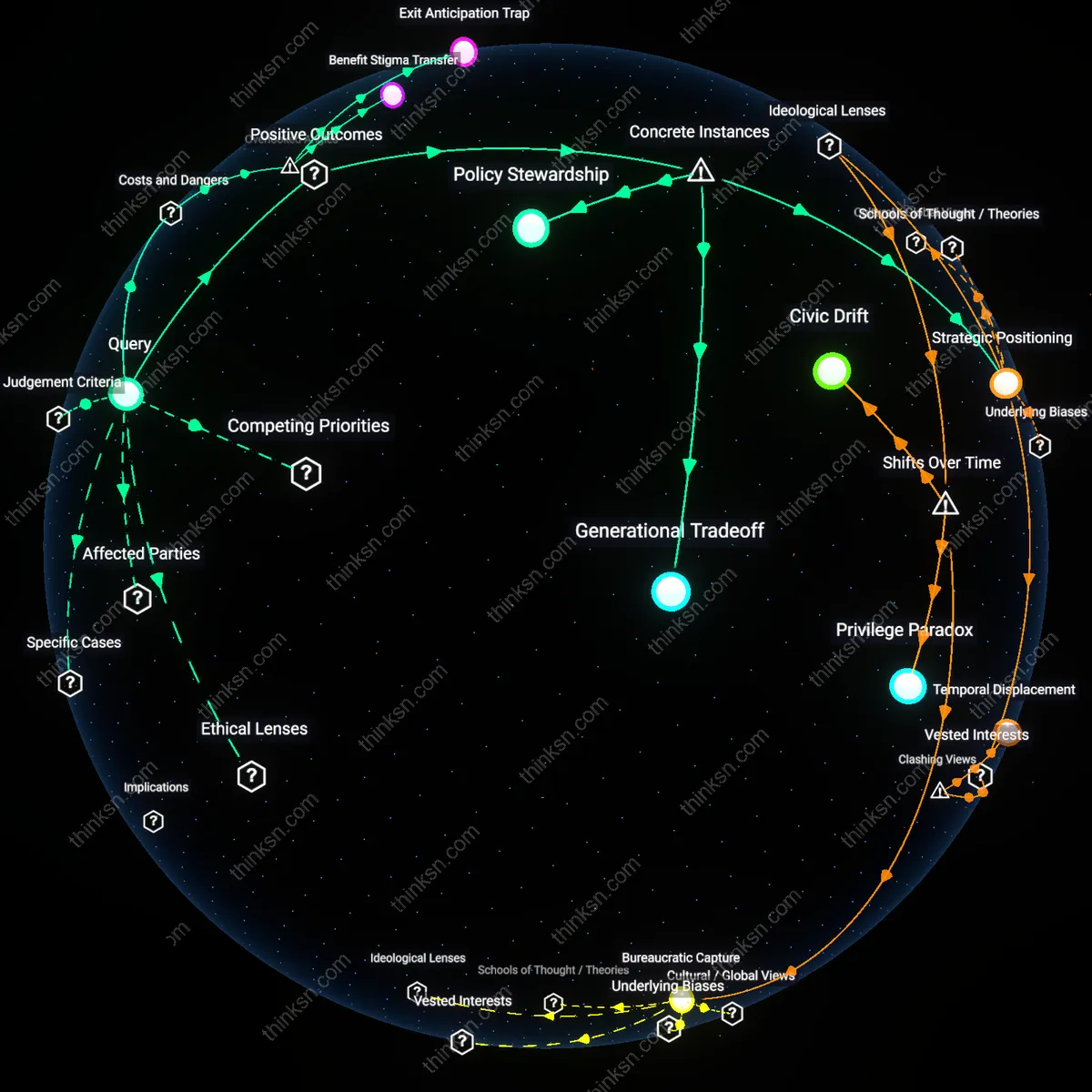
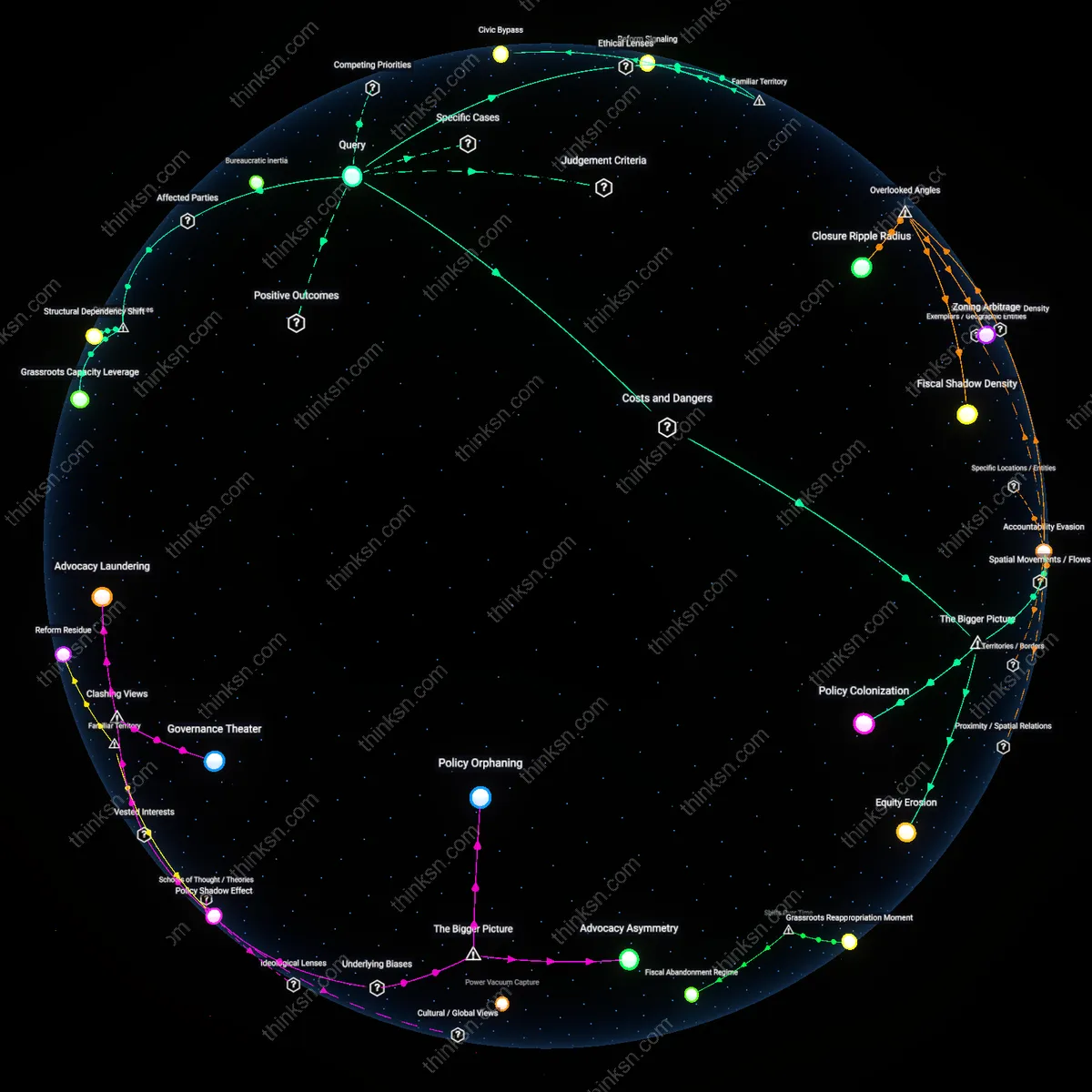
Strategic Positioning
California's Coastal Commission staff members routinely support housing affordability mandates while living in exclusionary coastal communities, leveraging subsidies for below-market public employee housing in Santa Cruz; their acceptance of personal benefit from supply-expanding policies while advocating for fiscal constraints signals not hypocrisy but tactical alignment with long-term institutional credibility, because their dual role as beneficiaries and regulators sustains policy coherence under political pressure, revealing how embedded actors preserve reform capacity through calibrated self-interest.
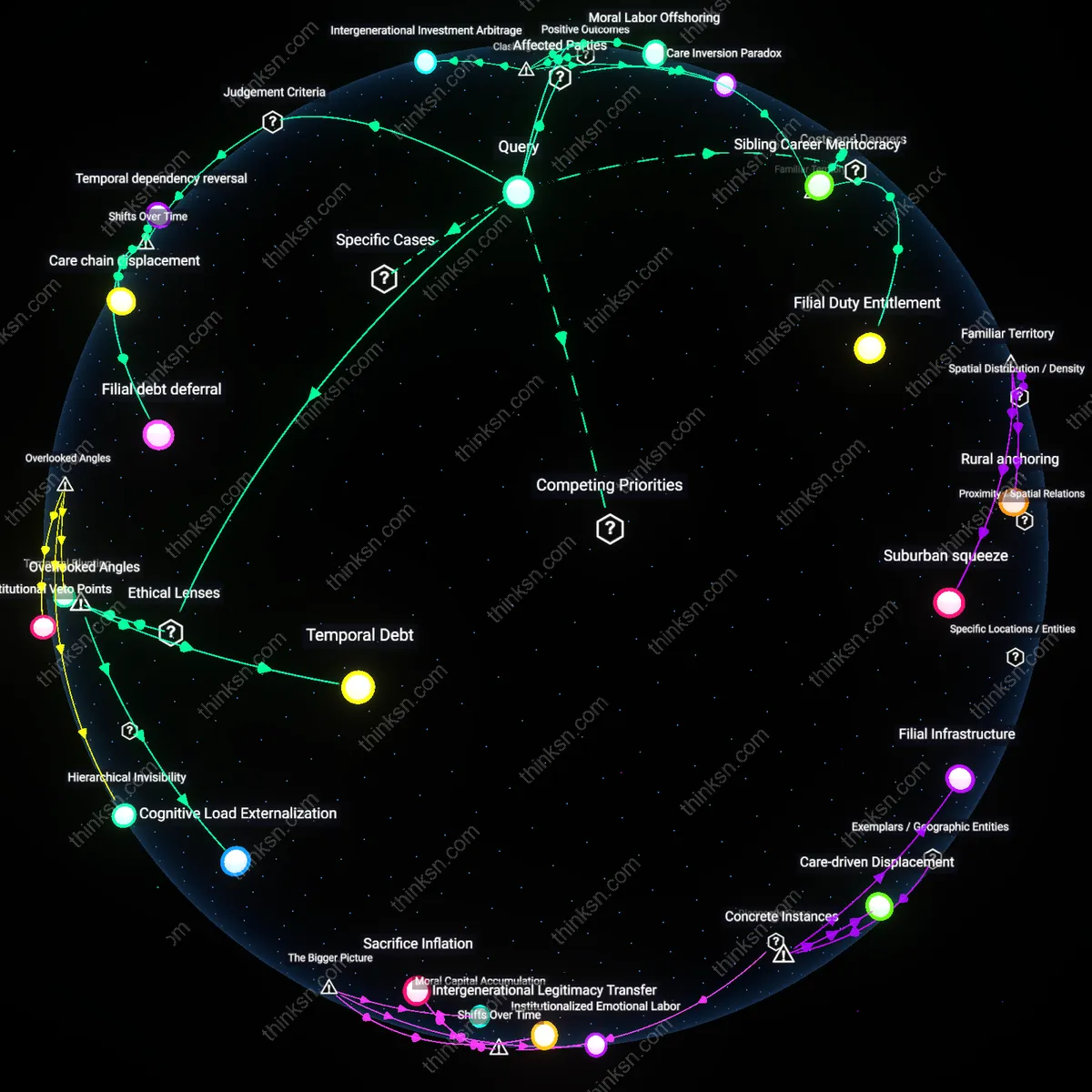
Generational Tradeoff
In Sweden’s 1992 pension reform, civil servants who retained access to transitional benefits under the outgoing defined-benefit system became key advocates for the new privatized framework that limited future subsidies; their concurrent receipt of legacy support and promotion of austerity enabled intergenerational equity by stabilizing public trust in retrenchment, as their personal exposure to phase-out conditions lent authenticity to structural reform, demonstrating how temporary privilege can be instrumentalized to legitimize systemic efficiency gains.
Policy Stewardship
Officials in Germany’s Social Democratic Party (SPD) during the 2003–2005 Hartz reforms accessed public healthcare and pension benefits while pushing for stricter eligibility rules in social assistance programs; their material reliance on the welfare state did not undermine reform credibility but instead anchored reformist legitimacy, because their firsthand experience with bureaucratic inefficiencies positioned them as pragmatic modernizers rather than ideologues, exposing how insider beneficiaries can drive sustainable cost containment without eroding public solidarity.
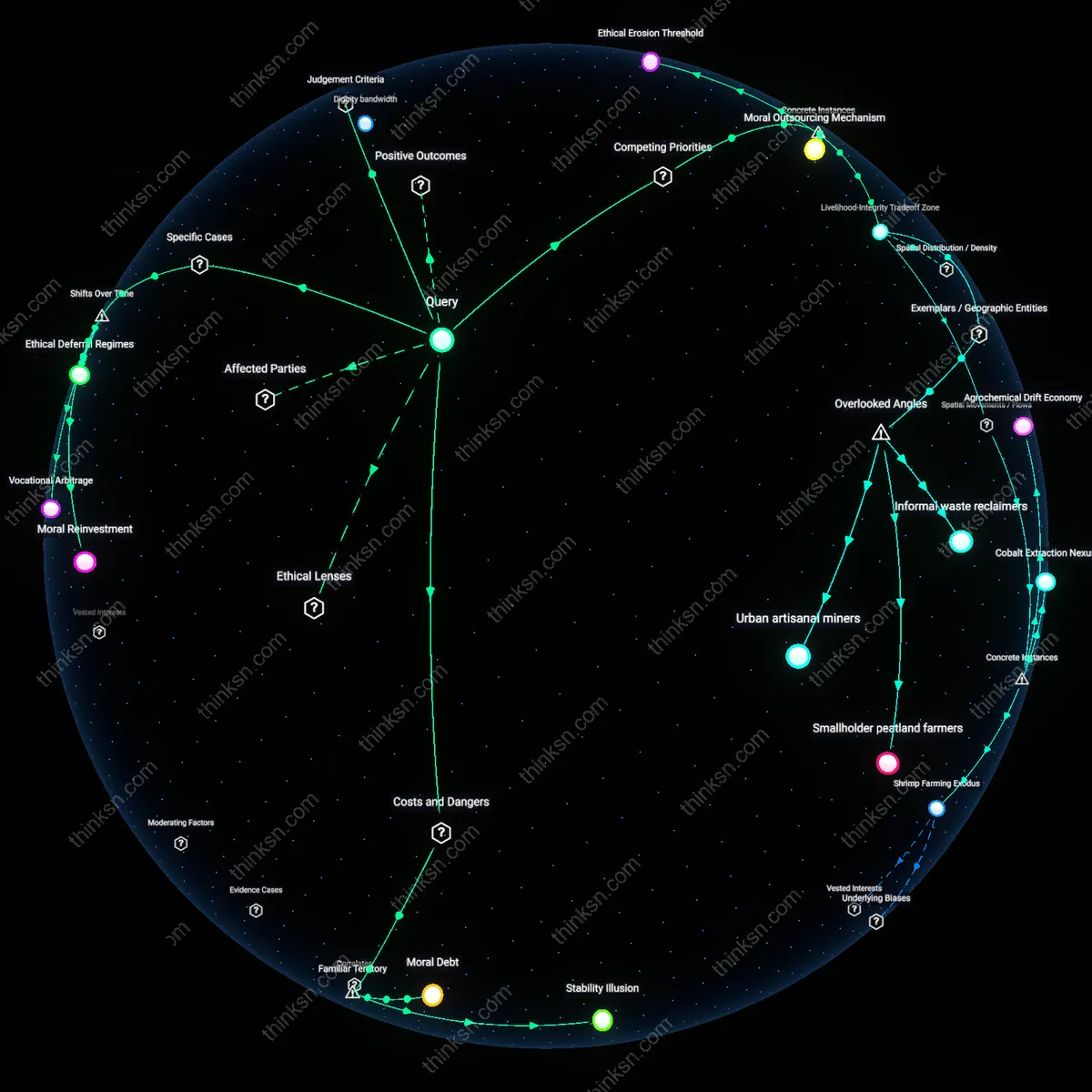
Subsidy Resentment
Accepting assisted living subsidies while campaigning to cut them corrodes trust in recipient communities by signaling conditional solidarity, where beneficiaries leverage access not to improve care standards but to distance themselves from others reliant on the same support, thereby fragmenting advocacy coalitions. This dynamic plays out in suburban county councils across Oregon, where middle-class seniors have successfully lobbied for reduced eligibility thresholds—knowing they will retain grandfathered benefits—thus insulating themselves while imposing greater hardship on future applicants. The non-obvious consequence is not hypocrisy but the strategic erosion of collective claim-making, which undermines long-term systemic resilience by converting subsidy access into a tool of social sorting.
Benefit Stigma Transfer
When families actively use subsidies while advocating their rollback, they unintentionally reinforce the perception that such aid is inherently degrading, because their dual stance implies that while the benefit was necessary for them, it is culturally undesirable for others. This occurs particularly in rural Midwest nursing cooperatives, where recipients frame their own enrollment as a temporary lapse rather than structural reliance, promoting policies that increase administrative barriers—like invasive asset checks—that they themselves evaded during smoother enrollment periods. What is overlooked is how individual moral alibis reproduce systemic stigma, converting personal justifications into policy architecture that punishes future users who lack similar social capital.
Exit Anticipation Trap
Families who accept assisted living subsidies while pushing for their reduction often do so with the unspoken assumption that they will soon exit the system—through recovery, death, or private funding—making their support for cuts seem costless, yet this collective anticipation destabilizes funding models that rely on steady cross-cohort risk pooling. In Florida’s Medicaid waiver programs, actuaries have observed that advocacy by temporary beneficiaries leads to volatile political support, where subsidy reforms gain traction not due to fiscal rigor but because current users expect short tenure and thus underestimate systemic fragility. The hidden risk is not moral inconsistency but the erasure of interdependence from policy timelines, transforming care infrastructure into a churn-based system vulnerable to collapse when exit assumptions prove wrong.