Is Universal Healthcare Worth Higher Taxes?
Analysis reveals 10 key thematic connections.
Key Findings
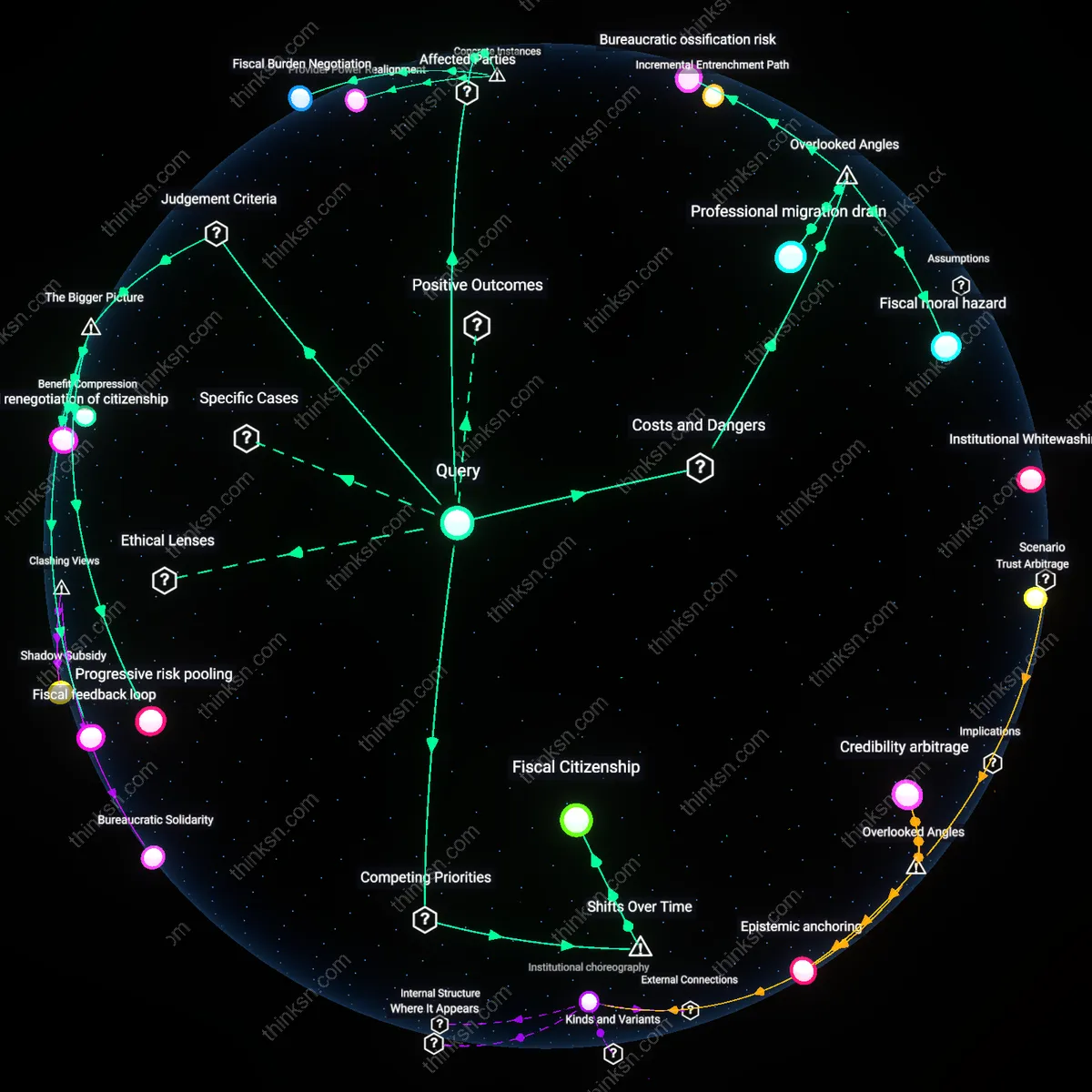
Fiscal Burden Negotiation
In Germany, working-class voters have consistently accepted higher payroll taxes to sustain the statutory health insurance system because employer and employee contributions are pooled across risk groups, shielding low-income individuals from catastrophic costs—this tradeoff reveals that when cost-sharing is institutionalized through collective bargaining between unions, employers, and the state, tax resistance diminishes even under substantial fiscal burdens. The mechanism operates through Germany’s corporatist welfare model, where social partnership structures transform tax obligations into negotiated social rights, making regressive impacts less salient. This underscores how distributional conflict over taxation can be depoliticized through institutionalized stakeholder representation, a dynamic rarely visible in majoritarian systems like the U.S.
Rural Access Dividend
When Thailand implemented the 30 Baht Program in 2001, rural villagers—many previously forgoing care—gained access to hospitals and clinics for a nominal co-pay, funded by reallocated national taxes, resulting in measurable declines in infant mortality and out-of-pocket spending, particularly in Isaan provinces. This shift illustrates that in geographically marginalized populations, the immediate health security gains from universal coverage outweigh tax increases because informal sector workers, who pay indirectly via consumption taxes, experience asymmetric gains in service access. The case reveals that tax tolerance increases when the marginal utility of healthcare access surges for historically excluded populations—a phenomenon obscured in wealthier nations where baseline access is higher.
Provider Power Realignment
In Canada’s 1960s adoption of Medicare, physicians’ incomes were effectively capped through global budgeting and fee schedules negotiated between provincial governments and medical associations, transferring financial risk from individuals to the state while containing costs through centralized leverage. This dynamic shows that higher taxation becomes politically sustainable when it simultaneously redistributes economic power away from private insurers and fee-for-service practitioners toward public administrators and patients. The Saskatchewan Doctors’ Strike of 1962 exposed how provider resistance, not public reluctance, posed the main obstacle—highlighting that tax-based financing reform often functions less as a fiscal bargain with citizens than as a political settlement with entrenched professional elites.
Progressive risk pooling
Individuals should evaluate universal healthcare not as a tax burden but as a mechanism of progressive risk pooling, where broader enrollment dilutes per-capita financial exposure to unpredictable medical shocks. This works through actuarial principles embedded in public insurance systems—such as cross-subsidies from healthier to sicker enrollees and from higher- to lower-income taxpayers—operating at scale through state-administered risk pools like those in Germany or Canada. The non-obvious insight is that higher taxes are not merely a cost but a prepayment that transforms volatile, catastrophic out-of-pocket expenses into predictable, income-adjusted contributions, thereby increasing financial resilience for the middle class.
Fiscal feedback loop
Support for higher taxes becomes more sustainable when individuals perceive universal healthcare as generating a fiscal feedback loop, wherein health gains enhance labor productivity and tax compliance, which in turn bolster public revenues and service capacity. In countries like Sweden, this cycle is institutionalized through coordinated health-labor policies and centralized wage bargaining, which link population health to macroeconomic stability. The underappreciated dynamic is that healthcare financing does not only extract revenue—it can expand the taxable base over time by reducing disability-related labor exit and enabling longer workforce participation.
Moral renegotiation of citizenship
The trade-off between taxes and healthcare access reflects a moral renegotiation of citizenship, where individuals assess whether tax payments affirm or erode their recognition as full members of a national political community. In post-Katrina New Orleans or post-Thatcher Britain, public services became litmus tests of belonging, with universal healthcare signaling inclusion versus stigma. The key insight is that tax tolerance is not purely economic—it rises when healthcare is experienced as a right that confirms dignity, not a benefit contingent on worthiness checks, thus altering the psychology of contribution in stratified societies.
Bureaucratic ossification risk
Adopting a single-payer healthcare system increases the danger of bureaucratic ossification risk, where centralized control entrenches inflexible administrative structures that resist adaptation to medical innovation. Once established, federal healthcare agencies develop path-dependent protocols that stifle incremental improvements—such as AI diagnostics or value-based reimbursement pilots—because regulatory inertia outweighs innovation incentives, especially when oversight bodies prioritize cost containment over clinical agility. This risk is rarely weighted in cost-benefit analyses, which assume administrative efficiency rather than the reality of mission creep and procedural calcification in large public institutions like CMS or the VA.
Fiscal moral hazard
Expanding universal healthcare coverage creates a fiscal moral hazard in which voters and policymakers externalize the long-term financial consequences of expanded services because the tax burden is diffused and delayed. With healthcare costs hidden within broad tax structures rather than direct out-of-pocket expenses, electorates systematically demand more services without perceiving their full cost, leading to unsustainable spending trajectories—evident in countries like Sweden, where public satisfaction with services coexists with structural deficits in elderly care funding. This dynamic subverts democratic fiscal responsibility by decoupling consumption from accountability, a mechanism typically absent from equity-focused healthcare debates.
Professional migration drain
Universal single-payer systems risk triggering a professional migration drain, where high-skilled medical specialists relocate to jurisdictions with higher compensation and autonomy, reducing domestic capacity for complex care. Unlike general workforce mobility, this effect selectively hollows out advanced fields like neurosurgery and oncology, as seen in Quebec’s recurring exodus of specialists to the U.S. private sector, undermining system resilience despite broader access gains. This asymmetry—improved equity for routine care at the expense of cutting-edge availability—is structurally hidden in aggregate health metrics like life expectancy, which fail to capture declining access to rare or intensive interventions.
Fiscal Citizenship
Individuals began weighing healthcare benefits against tax costs only after World War II, when the expansion of the federal income tax transformed ordinary wage earners into direct contributors to centralized social spending. This shift turned healthcare access from a moral or charitable question into a transactional calculation of fiscal reciprocity, binding individual benefit claims to visible tax liabilities. Before broad-based income taxation, healthcare was largely privatized and episodic, financed through out-of-pocket payments or mutual aid societies, so systemic trade-offs between taxes and coverage were politically inert. The postwar tax state rendered these trade-offs legible and personal, producing a new fiscal subject who evaluates solidarity not through need but through return on contribution, fundamentally altering democratic deliberation around equity.