Is Low-Carb Best for Diabetes When Moderate Carbs Boost Microbiome?
Analysis reveals 6 key thematic connections.
Key Findings
Dietary Guidelines Entrenchment
Public health institutions should maintain low-carb diet recommendations for diabetes management because these guidelines are tied to long-standing clinical outcomes and entrenched policy frameworks. Major bodies like the American Diabetes Association have standardized low-carb approaches based on glycemic control metrics, which directly inform physician behavior, insurance coverage, and federal nutrition programs. The non-obvious aspect is that even when emerging microbiome research challenges metabolic assumptions, institutional inertia and liability concerns suppress rapid guideline shifts, preserving the authority of established protocols over novel physiological insights.
Patient Agency Trade-off
Individuals with type 2 diabetes face reduced dietary autonomy when low-carb regimens are prioritized over microbiome-optimized eating patterns, because strict carb restriction simplifies daily decision-making at the cost of long-term gut health. Most patients associate diabetes control with immediate blood sugar feedback from glucometers, making moderate carbohydrate intake feel counterintuitive despite its potential microbiota benefits. The underappreciated reality is that patient empowerment is currently defined by glucose mastery, not ecological resilience, which sidelines emerging science in favor of familiar self-monitoring routines.
Pharmaceutical Co-alignment
Pharmaceutical companies benefit from sustaining low-carb dietary norms in diabetes care because persistent metabolic instability increases reliance on glucose-lowering drugs and injectables. When diets emphasize carb restriction over microbiome support, the burden of disease management leans more heavily on pharmacotherapy, reinforcing a treatment paradigm aligned with drug development pipelines and reimbursement models. What’s rarely acknowledged in public discourse is that dietary conservatism indirectly protects drug market stability by discouraging dietary patterns that could reduce medication dependence through enhanced microbial metabolism.
Metabolic Trade-off
Low-carb diets should not be universally prioritized for diabetes management because enhancing gut microbiome diversity through moderate carbohydrate intake can compromise glycemic control, creating a zero-sum trade-off between metabolic stability and microbial ecosystem health. Healthcare providers must weigh immediate blood glucose metrics against long-term dysbiosis risks, a tension amplified by clinical guidelines that privilege short-term biomarkers over gut-mediated metabolic resilience. This conflict is systemically enabled by fragmented medical incentives that reward glucose normalization but not microbiome monitoring, making invisible the delayed consequences of microbial impoverishment. The non-obvious insight is that dietary recommendations are constrained not by scientific uncertainty alone, but by how medical outcomes are temporally weighted in practice.
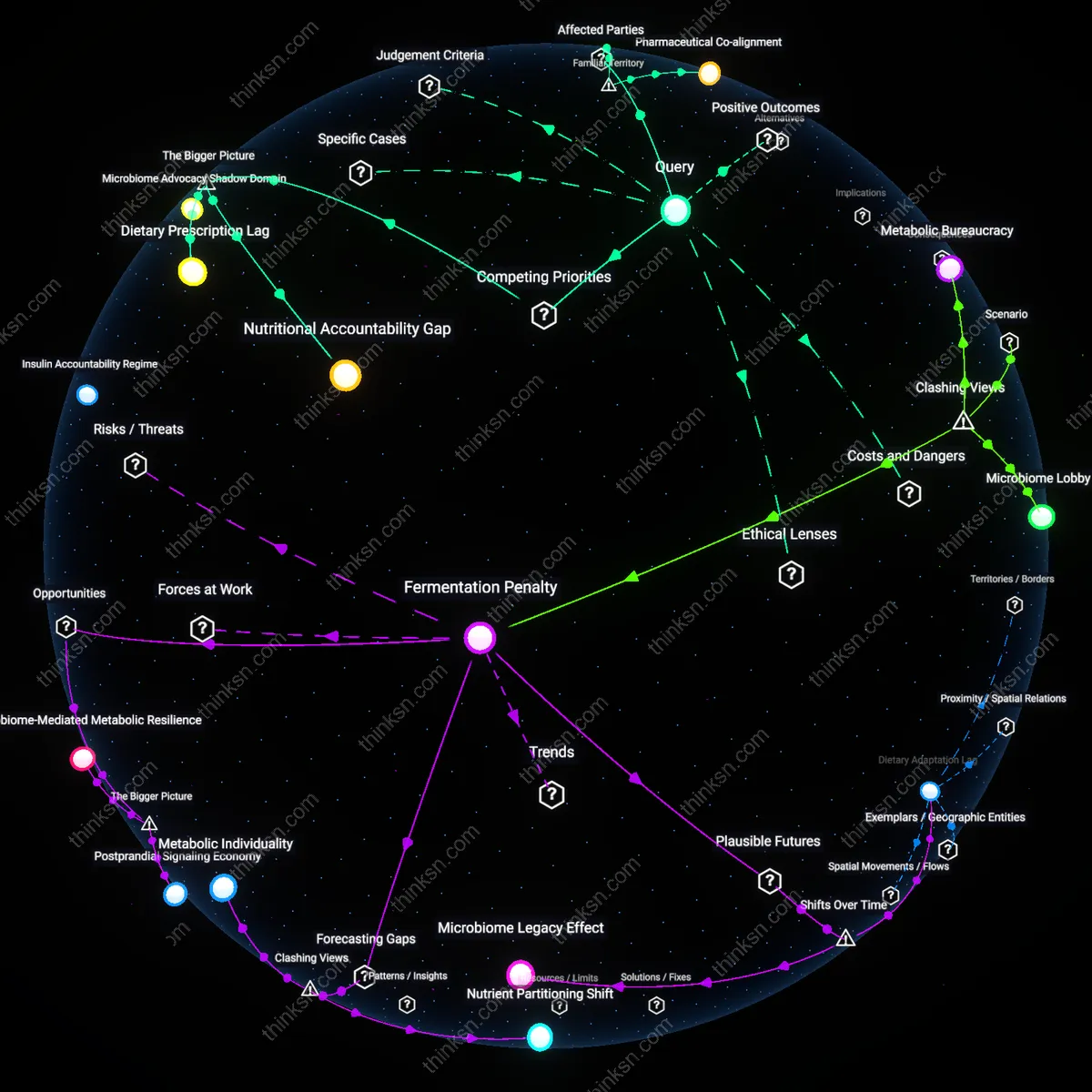
Nutritional Accountability Gap
Low-carb diets should be reconsidered because the clinical focus on carbohydrate restriction sidelines non-dietitian health actors—like gastroenterologists and microbiologists—who lack institutional leverage to influence diabetes protocols despite evidence linking moderate carbs to microbiome benefits. This power asymmetry arises from endocrinology’s dominance in diabetes governance, which structurally excludes gut health expertise from nutritional guideline committees, especially in settings like the American Diabetes Association’s consensus panels. As a result, microbial outcomes remain unaccounted for in dietary recommendations, not due to absence of evidence, but because of entrenched disciplinary hierarchies in metabolic medicine. The overlooked mechanism is how professional jurisdiction shapes what counts as relevant evidence.
Dietary Prescription Lag
Low-carb diets remain entrenched in diabetes care because realigning recommendations around moderate carbohydrate intake would disrupt established food-industrial alliances that profit from low-carb product lines, creating systemic resistance to dietary shifts even when microbial research challenges their efficacy. Pharmaceutical and supplement companies, which fund much of diabetes education through organizations like disease-awareness nonprofits, benefit from the status quo and indirectly shape clinical perceptions by sponsoring continuing medical education that emphasizes glycemic control over gut ecology. This results in a delayed update cycle for dietary guidelines, where scientific innovation is filtered through commercial stakeholders with misaligned incentives. The underappreciated dynamic is that evidence integration is not just epistemic but economically path-dependent.